Abstract
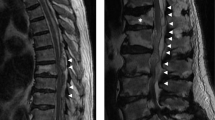
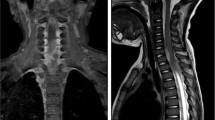
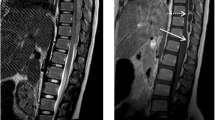
Two cases of spinal epidural abscess are reported whose abscesses became granulated after epidural catheterization. Although emergency surgical intervention was performed almost within 24 h after the diagnosis of epidural abscess in case 1, the patient revealed a poor outcome. After laminoplasty, case 2 received lumbar epidural catheterization, and he had a complete recovery. The abscesses were recognized to spread around the catheter insertion site of the operative procedure in both cases, and MRI in case 2 showed the connection between the epidural abscess and the interspinous space where the catheter had been inserted. Methicillin-sensitive Staphylococcus aureus (MSSA) was identified at the operative field in both cases. Also, MSSA was identified at the subcutaneous abscess around the catheter in case 1 and at the catheter tip in case 2. Those findings suggest the midpoint of the abscess is the puncture site and that MSSA is found in or around the catheter. Infection at epidural catheterization seems to be caused by catheter insertion or skin contamination after catheterization. As those catheterizations were completed in the outpatient theater, we conclude that epidural catheterization should be performed in the operating room or with a restricted aseptic technique.
Similar content being viewed by others
References
D Rigamonti L Liem P Sampath N Knoller Y Numaguchi DL Schreibman MA Sloan A Wolf S Zeidman (1999) ArticleTitleSpinal epidural abscess: contemporary trends in etiology, evaluation, and management Surg Neurol 52 189–197 Occurrence Handle10.1016/S0090-3019(99)00055-5 Occurrence Handle1:STN:280:DyaK1MznsV2mtw%3D%3D Occurrence Handle10447289
GA Tung JWK Yim LA Mermel L Philip JM Rogg (1999) ArticleTitleSpinal epidural abscess correlation between MRI findings and outcome Neuroradiology 41 904–909 Occurrence Handle10.1007/s002340050865 Occurrence Handle1:STN:280:DC%2BD3c7gtlyntQ%3D%3D Occurrence Handle10639666
E Reihsaus H Waldbaur W Seeling (2000) ArticleTitleSpinal epidural abscess: a meta-analysis of 915 patients Neurosurg Rev 232 175–204
LP Wang J Hauerberg JF Schmidt (2001) ArticleTitleLong-term outcome after neurosurgically treated spinal epidural abscess following epidural analgesia Acta Anaesthesiol Scand 45 233–239 Occurrence Handle1:STN:280:DC%2BD3M3isVKrtw%3D%3D Occurrence Handle11167170
LP Wang J Hauerberg JF Schmidt (1999) ArticleTitleIncidence of spinal epidural abscess after epidural analgesia: a national 1-year survey Anesthesiology 91 1928–1936 Occurrence Handle1:STN:280:DC%2BD3c%2FmsFKqtw%3D%3D Occurrence Handle10598636
SM Tay R Lee (2001) ArticleTitleCase report: catheter-related epidural abscess Ann Acad Med Singap 30 62–65 Occurrence Handle1:STN:280:DC%2BD3Mzit1Knug%3D%3D Occurrence Handle11242629
JMG Phillips JC Stedeford E Hartsilver C Roberts (2002) ArticleTitleEpidural abscess complicating insertion of epidural catheters Br J Anaesth 89 778–782 Occurrence Handle10.1093/bja/aef260 Occurrence Handle1:STN:280:DC%2BD38njsVGqtQ%3D%3D Occurrence Handle12393782
Author information
Authors and Affiliations
About this article
Cite this article
Kamiyama, Y. Two cases of spinal epidural abscess with granulation tissue associated with epidural catheterization. J Anesth 20, 102–105 (2006). https://doi.org/10.1007/s00540-005-0370-9
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1007/s00540-005-0370-9