Abstract
Background
Celiac disease is a chronic autoimmune enteropathy caused by gluten ingestion. While its prevalence in Western countries is reported to be as high as 1%, the prevalence has not been evaluated in a large-scale study of a Japanese population. The aim of our study was to clarify the possible presence of celiac disease in a Japanese non-clinical population as well as in patients showing symptoms suggestive of the disease.
Methods
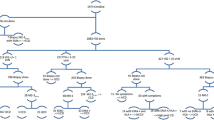
Serum samples were collected from 2008 non-clinical adults and 47 patients with chronic unexplained abdominal symptoms between April 2014 and June 2016. The anti-tissue transglutaminase (TTG) immunoglobulin A antibody titer was determined as a screening test for celiac disease in all subjects, and individuals with a value of >2 U/mL subsequently underwent testing for the presence of serum endomysial IgA antibody (EMA) as confirmation. Those testing positive for EMA or with a high concentration (>10 U/mL) of TTG were further investigated by histopathological examinations of duodenal mucosal biopsy specimens and HLA typing tests.
Results
Of the 2008 non-clinical adults from whom serum samples were collected, 161 tested positive for TTG, and all tested negative for EMA. Four subjects who had a high TTG titer were invited to undergo confirmatory testing, and the histopathological results confirmed the presence of celiac disease in only a single case (0.05%). Of the 47 symptomatic patients, one (2.1%) was found to have a high TTG titer and was diagnosed with celiac disease based on duodenal histopathological findings.
Conclusion
The presence of celiac disease in a non-clinical Japanese population was low at 0.05% and was rarely found in patients with unexplained chronic abdominal symptoms.


Similar content being viewed by others
References
Ludvigsson JF, Bai JC, Biagi F, et al. Diagnosis and management of adult coeliac disease: guidelines from the British Society of Gastroenterology. Gut. 2014;63:1210–28.
Rubio-Tapia A, Hill ID, Kelly CP, et al. ACG clinical guidelines: diagnosis and management of celiac disease. Am J Gastroenterol. 2013;108:656–76.
Fasano A, Catassi C. Clinical practice. Celiac disease. N Engl J Med. 2012;367:2419–26.
Ford AC, Chey WD, Talley NJ, et al. Yield of diagnostic tests for celiac disease in individuals with symptoms suggestive of irritable bowel syndrome: systematic review and meta-analysis. Arch Intern Med. 2009;169:651–8.
Reilly NR, Green PH. Epidemiology and clinical presentations of celiac disease. Semin Immunopathol. 2012;34:473–8.
van der Windt DA, Jellema P, Mulder CJ, et al. Diagnostic testing for celiac disease among patients with abdominal symptoms: a systematic review. JAMA. 2010;303:1738–46.
Oxentenko AS, Murray JA. Celiac disease: ten things that every gastroenterologist should know. Clin Gastroenterol Hepatol. 2015;13:1396–404.
Gujral N, Freeman HJ, Thomson AB. Celiac disease: prevalence, diagnosis, pathogenesis and treatment. World J Gastroenterol. 2012;18:6036–59.
Vives-Pi M, Takasawa S, Pujol-Autonell I, et al. Biomarkers for diagnosis and monitoring of celiac disease. J Clin Gastroenterol. 2013;47:308–13.
Fernandez E, Riestra S, Rodrigo L, et al. Comparison of six human anti-transglutaminase ELISA-tests in the diagnosis of celiac disease in the Saharawi population. World J Gastroenterol. 2005;11:3762–6.
Srinivas M, Basumani P, Podmore G, et al. Utility of testing patients, on presentation, for serologic features of celiac disease. Clin Gastroenterol Hepatol. 2014;12:946–52.
Liu E, Rewers M, Eisenbarth GS. Genetic testing: who should do the testing and what is the role of genetic testing in the setting of celiac disease? Gastroenterology. 2005;128:S33–7.
Kang JY, Kang AH, Green A, et al. Systematic review: worldwide variation in the frequency of coeliac disease and changes over time. Aliment Pharmacol Ther. 2013;38:226–45.
Rewers M. Epidemiology of celiac disease: what are the prevalence, incidence, and progression of celiac disease? Gastroenterology. 2005;128:S47–51.
West J, Fleming KM, Tata LJ, et al. Incidence and prevalence of celiac disease and dermatitis herpetiformis in the UK over two decades: population-based study. Am J Gastroenterol. 2014;109:757–68.
Hall EH, Crowe SE. Environmental and lifestyle influences on disorders of the large and small intestine: implications for treatment. Dig Dis. 2011;29:249–54.
Ihara M, Makino F, Sawada H, et al. Gluten sensitivity in Japanese patients with adult-onset cerebellar ataxia. Intern Med. 2006;45:135–40.
Ohata C, Ishii N, Hamada T, et al. Distinct characteristics in Japanese dermatitis herpetiformis: a review of all 91 Japanese patients over the last 35 years. Clin Dev Immunol. 2012;2012:562168.
Watanabe C, Komoto S, Hokari R, et al. Prevalence of serum celiac antibody in patients with IBD in Japan. J Gastroenterol. 2014;49:825–34.
Katanoda K, Matsumura Y. National nutrition survey in Japan–its methodological transition and current findings. J Nutr Sci Vitaminol (Tokyo). 2002;48:423–32.
Ministry of Health, Labour and Welfare. National health and nutrition survey. www.mhlw.go.jp/seisakunitsuite/bunya/kenkou_iryou/kenkou/kenkounippon21/en/eiyouchousa/koumoku_syokuhin_chousa.html. Accessed 25 Mar 2017.
Liu E, Lee HS, Aronsson CA, et al. Risk of pediatric celiac disease according to HLA haplotype and country. N Engl J Med. 2014;371:42–9.
Bonatto MW, Kotze L, Orlandoski M, et al. Endoscopic evaluation of celiac disease severity and its correlation with histopathological aspects of the duodenal mucosa. Endosc Int Open. 2016;4:E767–77.
Marsh MN. Gluten, major histocompatibility complex, and the small intestine. A molecular and immunobiologic approach to the spectrum of gluten sensitivity (‘celiac sprue’). Gastroenterology. 1992;102:330–54.
Villanacci V, Ceppa P, Tavani E, et al. Coeliac disease: the histology report. Dig Liver Dis. 2011;43[Suppl 4]:S385–95.
Muniz JG, Sdepanian VL, Fagundes UN. Prevalence of genetic susceptibility for celiac disease in blood donors in Sao Paulo. Brazil Arq Gastroenterol. 2016;53:267–72.
Rostom A, Murray JA, Kagnoff MF. American Gastroenterological Association (AGA) Institute technical review on the diagnosis and management of celiac disease. Gastroenterology. 2006;131:1981–2002.
Saito S, Ota S, Yamada E, et al. Allele frequencies and haplotypic associations defined by allelic DNA typing at HLA class I and class II loci in the Japanese population. Tissue Antigens. 2000;56:522–9.
Irvine AJ, Chey WD, Ford AC. Screening for celiac disease in irritable bowel syndrome: an updated systematic review and meta-analysis. Am J Gastroenterol. 2017;112:65–76.
Petrarca L, Nenna R, Mastrogiorgio G, et al. Dyspepsia and celiac disease: prevalence, diagnostic tools and therapy. World J Methodol. 2014;4:189–96.
Sanchez-Vargas LA, Thomas-Dupont P, Torres-Aguilera M, et al. Prevalence of celiac disease and related antibodies in patients diagnosed with irritable bowel syndrome according to the Rome III criteria. A case–control study. Neurogastroenterol Motil. 2016;28:994–1000.
Di Tola M, Marino M, Goetze S, et al. Identification of a serum transglutaminase threshold value for the noninvasive diagnosis of symptomatic adult celiac disease patients: a retrospective study. J Gastroenterol. 2016;51:1031–9.
Korponay-Szabo IR, Szabados K, Pusztai J, et al. Population screening for coeliac disease in primary care by district nurses using a rapid antibody test: diagnostic accuracy and feasibility study. BMJ. 2007;335:1244–7.
Hill P, Austin A, Forsyth J, et al. British Society of Gastroenterology guidelines on the diagnosis and management of coeliac disease. Gut. 2015;64:691–2.
Hadithi M, von Blomberg BM, Crusius JB, et al. Accuracy of serologic tests and HLA-DQ typing for diagnosing celiac disease. Ann Intern Med. 2007;147:294–302.
Kim CY, Quarsten H, Bergseng E, et al. Structural basis for HLA-DQ2-mediated presentation of gluten epitopes in celiac disease. Proc Natl Acad Sci USA. 2004;101:4175–9.
Lundin KE, Gjertsen HA, Scott H, et al. Function of DQ2 and DQ8 as HLA susceptibility molecules in celiac disease. Hum Immunol. 1994;41:24–7.
Paulsen G, Lundin KE, Gjertsen HA, et al. HLA-DQ2-restricted T-cell recognition of gluten-derived peptides in celiac disease. Influence of amino acid substitutions in the membrane distal domain of DQ beta 1*0201. Hum Immunol. 1995;42:145–53.
Megiorni F, Mora B, Bonamico M, et al. HLA-DQ and susceptibility to celiac disease: evidence for gender differences and parent-of-origin effects. Am J Gastroenterol. 2008;103:997–1003.
Acknowledgments
The authors thank Takashi Toda, and Atsuko Konishi (Shimane Environment and Health Public Corporation) for blood sample preparation. We also thank Keiko Masuzaki (Shimane University School of Medicine) for excellent technical assistance.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Fukunaga, M., Ishimura, N., Fukuyama, C. et al. Celiac disease in non-clinical populations of Japan. J Gastroenterol 53, 208–214 (2018). https://doi.org/10.1007/s00535-017-1339-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00535-017-1339-9