Abstract
Chronic pancreatitis is considered to be an irreversible progressive chronic inflammatory disease. The etiology and pathology of chronic pancreatitis are complex; therefore, it is important to correctly understand the stage and pathology and provide appropriate treatment accordingly. The newly revised Clinical Practice Guidelines of Chronic Pancreatitis 2015 consist of four chapters, i.e., diagnosis, staging, treatment, and prognosis, and includes a total of 65 clinical questions. These guidelines have aimed at providing certain directions and clinically practical contents for the management of chronic pancreatitis, preferentially adopting clinically useful articles. These revised guidelines also refer to early chronic pancreatitis based on the Criteria for the Diagnosis of Chronic Pancreatitis 2009. They include such items as health insurance coverage of high-titer lipase preparations and extracorporeal shock wave lithotripsy, new antidiabetic drugs, and the definition of and treatment approach to pancreatic pseudocyst. The accuracy of these guidelines has been improved by examining and adopting new evidence obtained after the publication of the first edition.
Similar content being viewed by others
Introduction
In Japan, the first edition of the Clinical Practice Guidelines for Chronic Pancreatitis was compiled in 2009, based on the clinical diagnostic criteria for chronic pancreatitis prepared by the Japan Pancreas Society in 2001. However, the 2001 criteria for the diagnosis of chronic pancreatitis were revised to contain the category of early chronic pancreatitis in 2009 [1]. Therefore, in the Clinical Practice Guidelines newly revised in 2015, we have referred to the diagnosis of early phase lesions of chronic pancreatitis based on the Criteria for the Diagnosis of Chronic Pancreatitis 2009; in addition, we have described the advent of high-titer lipase formulations, which have been available in Japan since 2009, and the utility of low-fat elemental diets (ED) for patients with pain. In addition, we have included in these Clinical Practice Guidelines items such as health insurance coverage of extracorporeal shock wave lithotripsy (ESWL), new antidiabetic agents such as incretin-related drugs, and the definition of and treatment approach to pancreatic pseudocyst following the revision of the Atlanta Classification in 2013. We have also added the effects of pancreatic duct stenting on internal pancreatic fistulas with pancreatic ascites and pleural effusions, and biliary stenting on bile duct stenosis complicated by chronic pancreatitis. We aimed at improving the accuracy of these Clinical Practice Guidelines by examining and adopting new evidence obtained after the publication of the first edition of the guidelines. In addition, we have adopted the idea of the GRADE (Grades of Recommendation Assessment, Development, and Evaluation) system in the descriptive content of the statements and determined the degrees of recommendation [2–4]. The revised content of the Clinical Practice Guidelines for Chronic Pancreatitis 2015 consists of four chapters: diagnosis, staging, treatment, and prognosis, and includes a total of 65 clinical questions (CQ). In this article, we will primarily explain the newly revised points described above in the order of the four chapters.
Diagnosis
The definitive diagnosis of chronic pancreatitis is sometimes difficult, especially if the disease is not considered by the physicians treating the patient. This chapter describes how chronic pancreatitis is suspected, based on signs, symptoms, and laboratory results, and how the diagnosis is developed. The CQ are very detailed and consist of 12 items, including history taking, physical examination, determination methods for pancreatic enzymes in the blood and urine [5, 6], significance of various imaging methods [chest and abdominal radiography, abdominal ultrasonography, computed tomography (CT), magnetic resonance imaging (MRI), endoscopic ultrasound, and pancreatography] in the diagnosis of chronic pancreatitis [7–15], exocrine pancreatic function testing, pathological diagnosis, differential diagnosis from pancreatic cancer and intraductal papillary mucinous neoplasm (IPMN), and genetic testing [16–20].
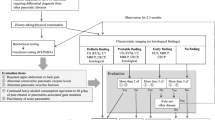
In order to facilitate understanding the path to diagnosis, flow diagram 1 (Fig. 1) was prepared. When chronic pancreatitis is suspected, a diagnosis should be made according to the criteria for the diagnosis of chronic pancreatitis revised in 2009 [1]. Definitive and probable diagnosis of chronic pancreatitis can be made by imaging alone. Of the cases in which findings for probable diagnosis are present, those that satisfy two or more items among repeated attacks of upper abdominal pain, abnormalities in blood/urine pancreatic enzymes, and exocrine pancreatic dysfunction are definitively diagnosed as chronic pancreatitis. However, the concept of early chronic pancreatitis has been adopted. Cases that do not qualify for definitive or probable diagnosis but which satisfy two or more items from the above three findings in addition to persistent drinking history (80 g/day), and show appropriate imaging findings as well (Table 1), are diagnosed as early chronic pancreatitis.
Staging
Chronic pancreatitis generally first presents with repeated upper abdominal and back pain, and endocrine and exocrine pancreatic function gradually deteriorates [21, 22]. In Japan, the disease is classified into three phases: compensated, transitional, and uncompensated, depending on the stage; however, an early chronic pancreatitis category has been added before the compensated phase in this revision [1]. Exocrine pancreatic disorder (that includes digestive and absorptive disorders) and abnormal glucose tolerance (pancreatic diabetes) occur as chronic pancreatitis progresses; therefore, to improve prognosis, pharmacological and nutritional therapies should be given in accordance with the stage of the disease. In this regard, staging of chronic pancreatitis is important. The CQ in this chapter comprise eight items, and clinical signs, blood and urine pancreatic enzyme levels, imaging, exocrine pancreatic function tests, and abnormal glucose tolerance tests, as well as the significance of scoring of these factors, are all important in determining the severity, staging, and treatment of chronic pancreatitis [23–32].
Treatment
There are numerous CQ in the Clinical Practice Guidelines for Chronic Pancreatitis. This chapter comprises six items (treatment strategy, lifestyle guidance, pain management, treatment of exocrine pancreatic insufficiency, treatment of diabetes mellitus, and treatment of complications), and there are CQ for each of these items. The treatment strategies and contents differ depending on the severity and the stage of chronic pancreatitis; in addition, surgical treatment sometimes becomes necessary. Flow diagram 2 (Fig. 2) shows the outline of the treatment path, flow diagram 3 (Fig. 3) shows the path of conservative medical treatment, and flow diagram 4 (Fig. 4) shows the path of surgical treatment.
Conservative medical treatment path for chronic pancreatitis. The figure shows a schematic flow diagram for the conservative medical treatment of chronic pancreatitis (CP). Single asterisk with regard to cases of acute exacerbation of chronic pancreatitis, severity diagnosis for acute pancreatitis should be made promptly and treatment strategy in accordance with that for acute pancreatitis should be determined. Double asterisks therapy with an elemental diet may be considered. Triple asterisks in pharmacotherapy, choice of drug and selection of dose should be decided according to this figure
Surgical treatment path for chronic pancreatitis. The figure shows a schematic flow diagram for the surgical treatment of chronic pancreatitis (CP). Single asterisk efficacy may be expected only for pain involving sympathomimetic nerves. Treatment strategy should be decided after explaining the possible use of narcotics and associated risks. Double asterisks this applies only in cases in which strict postoperative lifestyle guidance, including abstinence from alcohol drinking, is possible
Treatment strategy
Treatment strategies are individually explained according to causes, presence or absence of activity, severity, and stage; in addition, items such as whether the treatment strategies for chronic pancreatitis differ depending on lifestyle, especially alcohol drinking habits, are also discussed.
-
The etiology and pathology of chronic pancreatitis are complex, and the treatment differs depending on individual stages. In Japan, chronic pancreatitis is classified into compensated, transitional, and uncompensated phases. Exocrine pancreatic disorder (that includes digestive and absorptive disorders) and abnormal glucose tolerance (pancreatic diabetes) occur as chronic pancreatitis progresses; therefore, to improve prognosis, pharmacological and nutritional therapies should be given in accordance with the stage of the disease [33–35].
-
In the compensated phase, the prevention of repeated relapses and pain has priority; therefore, diet therapy to avoid excessive pancreatic stimulation and pharmacotherapy with mainly protease inhibitors are important. However, in the uncompensated phase, marked digestive and absorptive disorders appear. Pancreatitis symptoms such as upper abdominal and back pain often remit or disappear; therefore, the loss of fat in stool should be considered, and physicians should not uniformly direct patients to take low-fat meals. Steatorrhea is gauged by making patients take a sufficient amount of fat (50–70 g/day), followed by administration of a sufficient amount of digestive enzyme preparations. With the availability of pancrelipase, a high-titer digestive enzyme preparation, oral administration of small numbers or amounts of capsules or granules has become possible [36–39]. In addition, in the uncompensated phase, the secretion of bicarbonate, which maintains an alkaline pancreatic juice, is dramatically reduced; therefore, the pH of the upper small intestine is decreased. When postprandial pH in the small intestine becomes 4 or lower, the bile acids precipitate and digestive enzymes (lipases in particular) lose their activities; therefore, poor digestion and absorption of fat ensue. For patients with steatorrhea due to exocrine pancreatic dysfunction, in order to increase the pH in the upper small intestine, concomitant administration of antacids such as H2 receptor antagonists and proton pump inhibitors with digestive enzyme preparations becomes necessary [40–43].
-
In the uncompensated phase, which involves digestive and absorptive disorders (exocrine pancreatic insufficiency) due to pancreatic dysfunction-induced insufficient pancreatic secretion, it is important to control digestive and absorptive disorders and pancreatic diabetes. Therefore, in order to avoid poor nutritional conditions, an appropriate amount of fat should be given to patients, followed by administration of a sufficient amount of digestive enzyme preparations. For diabetes mellitus, it is necessary to control blood glucose and to determine the amount of insulin to be administered [44, 45].
-
Incretins [glucagon-like peptide-1 (GLP-1) and glucose-dependent insulinotropic peptide (GIP)], which are hormones secreted by the digestive tract, dependently promote insulin secretion and glucose-concentration; in addition, they are known to have protective and proliferative effects on pancreatic beta cells. Recently, drugs targeting these incretins, i.e., GLP-1 agonists and inhibitors of the incretin-degrading enzyme, dipeptidyl peptidase-4 (DPP-4), have been developed and have drawn attention as new treatments for type 2 diabetes mellitus [46]. On the other hand, the utility of incretin-related drugs for pancreatic diabetes mellitus has not yet been established. In these guidelines, we have proposed the use of these drugs only when the benefits of treatment are considered to surpass the risks. In addition, sodium/glucose cotransporter 2 (SGLT2) inhibitors have been newly developed; however, as in the case of incretin-related drugs, no evidence showing efficacy against diabetes mellitus complicated by chronic pancreatitis has been observed [47–50].
-
In chronic pancreatitis, various complications occur. These include pancreatic pseudocyst, pancreatic abscess, internal pancreatic fistulas with pancreatic ascites and pleural effusions, biliary stenosis, and hemosuccus pancreaticus. These guidelines discuss pharmacotherapy, endoscopic treatment, and surgical treatment for the above complications. In addition, ESWL has become covered by health insurance and reimbursable in Japan. Endoscopic treatment including ESWL is effective against abdominal pain due to chronic pancreatitis and thus is recommended in these guidelines. In addition, pancreatic stenting, which was shown to be effective for abdominal pain, has also become reimbursable by insurance. However, the criterion for the duration of pancreatic stent treatment has been set at approximately 1 year. In ineffective or relapsing cases, a proposal to consider surgical treatment has been made [51–62].
Lifestyle guidance
If the cause of chronic pancreatitis is alcoholic, abstinence from alcohol is necessary. These guidelines explain how to guide patients to abstinence using a flow diagram [63–65]. In addition, smoking increases the risks of developing chronic pancreatitis and pancreatic calcification. Abstinence from smoking may prevent the progression of chronic pancreatitis; therefore, giving smoking cessation guidance is recommended [66–68].
Pain management
Abdominal and back pain are major contributors to deterioration of the quality of life of patients with chronic pancreatitis. Inability to lead a social life, worsening nutritional conditions because of inability to ingest food, etc., are grave concerns that often confront practicing physicians. These guidelines refer to various pharmacotherapies and also describe the application of endoscopic and surgical treatments [69–71]. The utility of an elemental diet (ED) in patients with chronic pancreatitis with pain has been demonstrated; therefore, ED is recommended in these guidelines. Among various enteral nutrients, Elental, an ED, is characterized by its extremely low fat content and is reimbursable by health insurance for use for pancreatic diseases [72]. In these guidelines, fat-restricted diet therapy is considered basic for patients with chronic pancreatitis who present with attacks of abdominal pain; therefore, restriction of dietary fat is proposed for the management of abdominal pain.
Prognosis
Generally, chronic pancreatitis is a progressive inflammatory disease. Therefore, staging and determination of severity are necessary during follow-up observation; in other words, observation and evaluation of clinical symptoms, such as abdominal pain, changes of pancreatic enzyme levels over time, morphology of the pancreas, and endocrine and exocrine pancreatic functions, are useful. In addition, patients with chronic pancreatitis constitute a high-risk group for ordinary-type pancreatic cancer [73–75]. Although clear evidence for testing is lacking, many patients with chronic pancreatitis lead a lifestyle associated with carcinogenic risks (alcohol drinking and/or smoking), and it is useful to perform cancer screening [65, 76–81].
Conclusions
The Clinical Practice Guidelines for Chronic Pancreatitis 2015 describe general principles regarding the diagnosis, treatment, and prognosis of chronic pancreatitis and thus support decision-making by practicing physicians. These guidelines may be used by general clinicians, but in the following cases, referral to a pancreatologist is recommended: (1) chronic pancreatitis with repeated attacks of acute pancreatitis; (2) chronic pancreatitis in which pain and nutritional management is difficult; (3) chronic pancreatitis with pancreatic diabetes mellitus in which glucose control is difficult; (4) familial/hereditary and juvenile-onset chronic pancreatitis; and (5) chronic pancreatitis with advanced complications/comorbidities.
Chronic pancreatitis has a prolonged course; therefore, even if the drugs or treatments remain the same, their method of use may need to be changed, depending on the stage of the disease. In these guidelines, efforts have been made to promote visual understanding of the overall flow: we have prepared flow diagrams for general diagnosis and treatment, conservative medical treatment, and surgical treatment; we have also created CQ that correspond to the individual items above to enhance understanding.
References
Shimosegawa T, Kataoka K, Kamisawa T, et al. The revised Japanese clinical diagnostic criteria for chronic pancreatitis. J Gastroenterol. 2010;45:584–91.
Schünemann HJ, Oxman AD, Brozek J, et al. GRADE: assessing the quality of evidence for diagnostic recommendations. Evid Based Med. 2008;13:162–3.
Schünemann HJ, Oxman AD, Brozek J, et al. Grading quality of evidence and strength of recommendations for diagnostic tests and strategies. BMJ. 2008;336:1106–10.
Guyatt GH, Oxman AD, Vist GE, et al. GRADE: an emerging consensus on rating quality of evidence and strength of recommendations. BMJ. 2008;336:924–6.
Pezzilli R, Talamini G, Gullo L. Behavior of serum pancreatic enzymes in chronic pancreatitis. Dig Liver Dis. 2000;32:233–7.
Ventrucci M, Gullo L, Daniele C, et al. Comparative study of serum pancreatic isoamylase, lipase, and trypsin-like immunoreactivity in pancreatic disease. Digestion. 1983;28:114–21.
Ammann RW, Muench R, Otto R, et al. Evolution and regression of pancreatic calcification in chronic pancreatitis: a prospective long-term study of 107 patients. Gastroenterology. 1988;95:1018–28.
Buscail L, Escourrou J, Moreau J, et al. Endoscopic ultrasonography in chronic pancreatitis: a comparative prospective study with 8 conventional ultrasonography, computed tomography, and ERCP. Pancreas. 1995;10:251–7.
Rosch T, Schusdziarra V, Born P, et al. Modern imaging methods versus clinical assessment in the evaluation of hospital in-patients with suspected pancreatic disease. Am J Gastroenterol. 2000;95:2261–70.
Bozkurt T, Braun U, Leferink S, et al. Comparison of pancreatic morphology and exocrine functional impairment in patients with chronic pancreatitis. Gut. 1994;35:1132–6.
Sanyal R, Stevens T, Novak E, et al. Secretin-enhanced MRCP: review of technique and application with proposal for quantification of exocrine function. AJR Am J Roentgenol. 2012;198:124–32.
Catalano MF, Lahoti S, Geenen JE, et al. Prospective evaluation of endoscopic ultrasonography, endoscopic retrograde pancreatography, and secretin test in the diagnosis of chronic pancreatitis. Gastrointest Endosc. 1998;48:11–7.
Wiersema MJ, Hawes RH, Lehman GA, et al. Prospective evaluation of endoscopic ultrasonography and endoscopic retrograde cholangiopancreatography in patients with chronic abdominal pain of suspected pancreatic origin. Endoscopy. 1993;25:555–64.
Buscail L, Escourrou J, Moreau J, et al. Endoscopic ultrasonography in chronic pancreatitis: a comparative prospective study with conventional ultrasonography, computed tomography, and ERCP. Pancreas. 1995;10:251–7.
Mikata R, Ishihara T, Tada M, et al. Clinical usefulness of repeated pancreatic juice cytology via endoscopic naso-pancreatic drainage tube in patients with pancreatic cancer. J Gastroenterol. 2013;48:866–73.
Kataoka K, Yamane Y, Kato M, et al. Diagnosis of chronic pancreatitis using noninvasive tests of exocrine pancreatic function: comparison to duodenal intubation tests. Pancreas. 1997;15:409–15.
Stasi MD, Lencioni R, Solmi L, et al. Ultrasound-guided fine needle biopsy of pancreatic masses: results of a multicenter study. Am J Gastroenterol. 1998;93:1329–33.
Tanno S, Nakano Y, Koizumi K, et al. Pancreatic ductal adenocarcinomas in long-term follow-up patients with branch duct intraductal papillary mucinous neoplasms. Pancreas. 2010;39:36–40.
Ellis I, Lerch MM, Whitcomb DC. Genetic testing for hereditary pancreatitis: guideline for indication, counseling, consent and privacy issues. Pancreatology. 2001;1:405–15.
Teich N, Mossner J. Hereditary chronic pancreatitis. Best Pract Res Clin Gastroenterol. 2008;22:115–30.
Ammann RW. A clinically based classification system for alcoholic chronic pancreatitis: summary of an international workshop on chronic pancreatitis. Pancreas. 1997;14:215–21.
Ramesh H. Proposal for a new grading system for chronic pancreatitis. J Clin Gastroenterol. 2002;35:67–70.
Ventrucci M, Gullo L, Daniele C, et al. Comparative study of serum pancreatic isoamylase, lipase, and trypsin-like immunoreactivity in pancreatic disease. Digestion. 1983;28:114–21.
Kamisawa T, Matsukawa M, Yoshiike M, et al. Chronic pancreatitis progressing from segmental lesions. Hepatogastroenterology. 2005;52:1255–8.
Otsuki M. Chronic pancreatitis: the problems of diagnostic criteria. Pancreatology. 2004;4:28–41.
Catalano MF, Sahai A, Levy M, et al. EUS-based criteria for the diagnosis of chronic pancreatitis: the Rosemont classification. Gastrointest Endosc. 2009;69:1251–61.
Kitagawa M, Naruse S, Ishiguro H, et al. Evaluating exocrine function tests for diagnosing chronic pancreatitis. Pancreas. 1997;15:402–8.
Kataoka K, Yamane Y, Kato M, et al. Diagnosis of chronic pancreatitis using noninvasive tests of exocrine pancreatic function: comparison to duodenal intubation tests. Pancreas. 1997;15:409–15.
Hayakawa T, Kondo T, Shibata T. Relationship between pancreatic exocrine function and histological changes in chronic pancreatitis. Am J Gastroenterol. 1992;87:1170–4.
Koizumi M, Yoshida Y, Abe N, et al. Pancreatic diabetes in Japan. Pancreas. 1998;16:385–91.
Chari ST, Singer MV. The problem of classification and staging of chronic pancreatitis. Scand J Gastroenterol. 1994;29:949–60.
Schneider A, Löhr JM, Singer MV. The M-ANNHEIM classification of chronic pancreatitis: introduction of a unifying classification system based on a review of previous classifications of the disease. J Gastroenterol. 2007;42:101–19.
Etemad B, Whitcomb DC. Chronic pancreatitis: diagnosis, classification, and new genetic developments. Gastroenterology. 2001;120:682–707.
Axon AT, Classen M, Cotton PB, et al. Pancreatography in chronic pancreatitis: international definitions. Gut. 1984;25:1107–12.
Ammann RW. Diagnosis and management of chronic pancreatitis: current knowledge. Swiss Med Wkly. 2006;136:166–74.
Nakamura T, Takeuchi T, Tando Y. Pancreatic dysfunction and treatment options. Pancreas. 1998;16:329–36.
Marotta F, O’Keefe SJ, Marks IN, et al. Pancreatic enzyme replacement therapy: importance of gastric acid secretion, H2-antagonists, and enteric coating. Dig Dis Sci. 1989;34:456–61.
Lankisch PG. Enzyme treatment of exocrine pancreatic insufficiency in chronic pancreatitis. Digestion. 1993;54(Suppl 2):21–9.
Layer P, Keller J, Lankisch PG. Pancreatic enzyme replacement therapy. Curr Gastroenterol Rep. 2001;3:101–8.
Nakamura T, Arai Y, Tando Y, et al. Effect of omeprazole on changes in gastric and upper small intestine pH levels in patients with chronic pancreatitis. Clin Ther. 1995;17:448–59.
Lankisch PG. Acute and chronic pancreatitis: an update on management. Drugs. 1984;28:554–64.
Scolapio JS, Malhi-Chowla N, Ukleja A. Nutrition supplementation in patients with acute and chronic pancreatitis. Gastroenterol Clin North Am. 1999;28:695–707.
Perry RS, Gallagher J. Management of maldigestion associated with pancreatic insufficiency. Clin Pharm. 1985;4:161–9.
Kawabe K, Ito T, Igarashi H, et al. The current managements of pancreatic diabetes in Japan. Clin J Gastroenterol. 2009;2:1–8.
Ito T, Otsuki M, Igarashi H, et al. Epidemiological study of pancreatic diabetes in Japan in 2005: a nationwide study. Pancreas. 2010;39:829–35.
Daniel JD, Michael AN. The incretin system: glucagon-like peptide-1 receptor agonists and dipeptidyl peptidase-4 inhibitors in type 2 diabetes. Lancet. 2006;368:1969–75.
Elashoff M, Matveyenko AV, Gier B, et al. Pancreatitis, pancreatic, and thyroid cancer with glucagon-like peptide-1-based therapies. Gastroenterology. 2011;141:150–6.
Butler PC, Elashoff M, Elahoff R, et al. A critical analysis of the clinical use of incretin-based therapies: are the GLP-1 therapies safe? Diabetes Care. 2013;36:2118–25.
Dore DD, Hussein M, Hoffman C, et al. A pooled analysis of exenatide use and risk of acute pancreatitis. Curr Med Res Opin. 2013;29:1577–86.
Nauck MA. A critical analysis of the clinical use of incretin-based therapies: the benefits by far outweigh the potential risks. Diabetes Care. 2013;36:2126–32.
Banks PA, Bollen TL, Dervenis C, et al. Classification of acute pancreatitis–2012: revision of the Atlanta classification and definitions by international consensus. Gut. 2013;62:102–11.
Varadarajulu S, Bang JY, Sutton BS, et al. Equal efficacy of endoscopic and surgical cystogastrostomy for pancreatic pseudocyst drainage in a randomized trial. Gastroenterology. 2013;145:583–90.
Nealon WH, Walser E. Duct drainage alone is sufficient in the operative management of pancreatic pseudocyst in patients with chronic pancreatitis. Ann Surg. 2003;237:614–20.
Schlosser W, Siech M, Beger HG. Pseudocyst treatment in chronic pancreatitis: surgical treatment of the underlying disease increases the long-term success. Dig Surg. 2005;22:340–5.
Olakowski M, Mieczkowska-Palacz H, Olakowska E, et al. Surgical management of pancreaticopleural fistulas. Acta Chir Belg. 2009;109:735–40.
Tajima Y, Tsutsumi R, Kuroki T, et al. Evaluation and management of thoracopancreatic fistula. Surgery. 2006;140:773–8.
Ohge H, Yokoyama T, Kodama T, et al. Surgical approaches for pancreatic ascites: report of three cases. Surg Today. 1999;29:458–61.
Dumonceau JM, Tringali A, Blero D, et al. Biliary stenting: indications, choice of stents and results: European Society of Gastrointestinal Endoscopy (ESGE) clinical guideline. Endoscopy. 2012;44:277–89.
Lermite E, Regenet N, Tuech JJ, et al. Diagnosis and treatment of hemosuccus pancreaticus: development of endovascular management. Pancreas. 2007;34:229–32.
Inui K, Tazuma S, Yamaguchi T, et al. Treatment of pancreatic stones with extracorporeal shock wave lithotripsy. Pancreas. 2005;30:26–30.
Ohara H, Hoshino M, Hayakawa T, et al. Single application extracorporeal shock wave lithotripsy is the first choice for patients with pancreatic duct stones. Am J Gastroenterol. 1996;91:1388–94.
Sauerbruch T, Holl J, Paumgartner G. Extracorporeal lithotripsy of pancreatic stones in patients with chronic pancreatitis and pain: a prospective follow up study. Gut. 1992;33:969–72.
Hayakawa T, Kondo T, Shibata T, et al. Chronic alcoholism and evolution of pain and prognosis in chronic pancreatitis. Digestion. 1993;54:148–55.
Lankisch PG, Lohr-Happe A, Otto J, et al. Natural course in chronic pancreatitis. Digestion. 1993;54:148–55.
Miyake H, Harada H, Kunichika K, et al. Clinical course and prognosis of chronic pancreatitis. Pancreas. 1987;2:378–85.
Andriulli A, Botteri E, Almasio PL, et al. Smoking as a cofactor for causation of chronic pancreatitis: a meta-analysis. Pancreas. 2010;39:1205–10.
Cavallini G, Talamini G, Vaona B, et al. Effect of alcohol and smoking on pancreatic lithogenesis in the course of chronic pancreatitis. Pancreas. 1994;9:42–6.
Imoto M, DiMagno EP. Cigarette smoking increases the risk of pancreatic calcification in late-onset but not early-onset idiopathic chronic pancreatitis. Pancreas. 2000;21:115–9.
Kanoh M, Ibata H, Miyagawa M, et al. Clinical effects of camostat in chronic pancreatitis. Biomed Res. 1989;10(Suppl 1):145–50.
Cahen DL, Gouma DJ, Laramée P, et al. Long-term outcomes of endoscopic vs surgical drainage of the pancreatic duct in patients with chronic pancreatitis. Gastroenterology. 2011;141:1690–5.
Dumonceau JM, Delhaye M, Tringali A, et al. Endoscopic treatment of chronic pancreatitis: European Society of Gastrointestinal Endoscopy (ESGE) Clinical Guideline. Endoscopy. 2012;44:784–800.
Kataoka K, Sakagami J, Hirota M, et al. Effects of oral ingestion of the elemental diet in patients with painful chronic pancreatitis in the real-life setting in Japan. Pancreas. 2014;43:451–7.
Lowenfels AB, Maisonneuve P, Cavallini G, et al. Pancreatitis and the risk of pancreatic cancer: international Pancreatitis Study Group. N Engl J Med. 1993;328:1433–7.
Kamisawa T, Tu Y, Egawa N, et al. The incidence of pancreatic and extrapancreatic cancers in Japanese patients with chronic pancreatitis. Hepatogastroenterology. 2007;54:1579–81.
Capurso G, Falconi M, Panzuto F, et al. Risk factors for sporadic pancreatic endocrine tumors: a case-control study of prospectively evaluated patients. Am J Gastroenterol. 2009;104:3034–304.
Lankisch MR, Imoto M, Layer P, et al. The effect of small amounts of alcohol on the clinical course of chronic pancreatitis. Mayo Clin Proc. 2001;76:242–51.
Arvanitakis M, Van Laethem JL, Parma J, et al. Predictive factors for pancreatic cancer in patients with chronic pancreatitis in association with K-ras gene mutation. Endoscopy. 2004;36:535–42.
Löhr M, Müller P, Mora J, et al. p53 and K-ras mutations in pancreatic juice samples from patients with chronic pancreatitis. Gastrointest Endosc. 2001;53:734–43.
Nojgaard C, Bendtsen F, Becker U, et al. Danish patients with chronic pancreatitis have a four-fold higher mortality rate than the Danish population. Clin Gastroenterol Hepatol. 2010;8:384–90.
Lankisch PG, Löhr-Happe A, Otto J, et al. Natural course in chronic pancreatitis: pain, exocrine and endocrine pancreatic insufficiency and prognosis of the disease. Digestion. 1993;54:148–55.
Knop FK, Vilsboll T, Larsen S, et al. No hypoglycemia after subcutaneous administration of glucagon-like peptide-1 in lean type 2 diabetic patients and in patients with diabetes secondary to chronic pancreatitis. Diabetes Care. 2003;26:2581–7.
Acknowledgments
This article was supported by a Grant-in-Aid from the JSGE.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
Any financial relationship with enterprises, businesses, or academic institutions in the subject matter or materials discussed in the manuscript are listed as follows; (1) those from which the authors, the spouse, partner or immediate relatives of the authors, have received individually any income, honoraria or any other types of remuneration; no conflict of interest; and (2) those from which the academic institutions of the authors received support (commercial/academic cooperation); Astellas Pharma Inc., AstraZeneca K.K., Asubio Pharma Co., Ltd., Eisai Co., Ltd., MSD K.K., Otsuka Pharmaceutical Co., Ltd., Daiichi Sankyo Co., Daiichi Sankyo Co., Ltd., Takeda Pharmaceutical Company Limited., Mitsubishi Tanabe Pharma Corporation, Chugai Pharmaceutical Co., Ltd.
Additional information
The original version of this article appeared in Japanese as “Manseisuien Sinryo Guideline 2015” from the Japanese Society of Gastroenterology (JSGE), published by Nankodo, Tokyo, 2015. Please see the article on the standards, methods, and process of developing the guidelines (doi:10.1007/s00535-014-1016-1).
The members of the Guidelines Committee are listed in the Appendix in the text.
Appendix
Appendix
Members of the Guidelines Committee who created and evaluated the JSGE “Evidence-based clinical guidelines for chronic pancreatitis” are listed below.
Executive Committee
Chair: Tooru Shimosegawa (Division of Gastroenterology, Tohoku University Graduate School of Medicine)
Vice-Chair: Tetsuhide Ito (Department of Medicine and Bioregulatory Science, Graduate School of Medical Sciences, Kyushu University)
Members: Hiroshi Ishiguro (Department of Human Nutrition, Nagoya University Graduate School of Medicine), Hirotaka Ohara (Department of Community-based Medical Education, Nagoya City University Graduate School of Medical Sciences), Terumi Kamisawa (Department of Internal Medicine, Tokyo Metropolitan Komagome Hospital), Junichi Sakagami (Department of Molecular Gastroenterology and Hepatology, Graduate School of Medical Science, Kyoto Prefectural University of Medicine), Naohiro Sata (Department of Surgery, Jichi Medical University), Yoshifumi Takeyama (Department of Surgery, Kinki University Faculty of Medicine), Morihisa Hirota (Division of Gastroenterology, Tohoku University Graduate School of Medicine), Hiroyuki MIyakawa (Division of Biliopancreatology, Sapporo Kosei General Hospital)
Evaluation Committee
Chair: Keiko Shiratori (Department of Gastroenterology, Tokyo Women’s Medical University)
Vice-Chair: Masanori Sugiyama (Department of Surgery, Kyorin University School of Medicine)
Members: Kazuichi Okazaki (Division of Gastroenterology and Hepatology, Kansai Medical University), Shigeyuki Kawa (Center for Health, Safety, and Environmental Management, Shinshu University), Yusuke Tando (Department of Endocrinology and Metabolism, Hirosaki University School of Medicine)
Main Collaborators
Hisato Igarashi, Lingaku Lee, Takashi Fujiyama, Masayuki Hijioka, Keijiro Ueda, Yuichi Tachibana (Department of Medicine and Bioregulatory Science, Graduate School of Medical Sciences, Kyushu University), Yoshio Togame, Hieoaki Yasuda, Ryusuke Kato (Department of Molecular Gastroenterology and Hepatology, Graduate School of Medical Science, Kyoto Prefectural University of Medicine)
Observer
Keisho Kataoka (Otsu Municipal Hospital)
The Japanese Society of Gastroenterology
President, Tooru Shimosegawa (Division of Gastroenterology, Tohoku University Graduate School of Medicine)
Rights and permissions
About this article
Cite this article
Ito, T., Ishiguro, H., Ohara, H. et al. Evidence-based clinical practice guidelines for chronic pancreatitis 2015. J Gastroenterol 51, 85–92 (2016). https://doi.org/10.1007/s00535-015-1149-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00535-015-1149-x