Abstract
Background
The aim of this study was to evaluate short- and long-term outcomes in relatively young patients (≤60 years old) who underwent endoscopic papillary balloon dilation (EPBD) for bile duct stone removal.
Methods
Immediate and long-term outcomes were evaluated in 311 patients who were 60 years old or younger at the time of EPBD. The stone recurrence rate was compared among four groups stratified according to gallbladder (GB) status before and after EPBD (cholecystectomy after EPBD, GB left in situ with stones, GB left in situ without stones, and cholecystectomy before EPBD).
Results
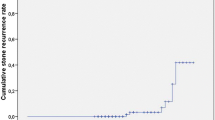
Bile duct stones were completely removed via EPBD alone in 304 patients (97.7%). Post-EPBD pancreatitis occurred in 24 patients (7.7%), and was mild in 18 patients, moderate in 5 patients, and severe in 1 patient. The rate of pancreatitis was significantly higher in these patients than in patients aged more than 60 years who underwent EPBD during the same study period (4.7%). Long-term outcomes were evaluated in 217 patients who were followed for at least 1 year after complete stone removal via EPBD. During a mean follow-up period of 5.6 years (range, 1.0–13.4 years), stone recurrence was observed in 13 patients (6.0%). The cumulative stone recurrence rates at 5 and 10 years after EPBD were 5.9 and 7.1%, respectively. Patients in the cholecystectomy after EPBD group had the lowest risk of stone recurrence among the four groups (2.0%).
Conclusion
EPBD removes bile duct stones in the majority of younger patients without increasing the risk of severe pancreatitis. Post-EPBD pancreatitis is more likely to occur in younger patients as compared to older patients. The long-term outcomes of EPBD appear favorable, especially in patients who have undergone cholecystectomy after EPBD.

Similar content being viewed by others
References
Hawes RH, Cotton PB, Vallon AG. Follow-up 6 to 11 years after duodenoscopic sphincterotomy for stones in patients with prior cholecystectomy. Gastroenterology. 1990;98:1008–12.
Bergman JJ, van der Mey S, Rauws EA, Tijssen JG, Gouma DJ, Tytgat GN, et al. Long-term follow-up after endoscopic sphincterotomy for bile duct stones in patients younger than 60 years of age. Gastrointest Endosc. 1996;44:643–9.
Prat F, Malak NA, Pelletier G, Buffet C, Fritsch J, Choury AD, et al. Biliary symptoms and complications more than 8 years after endoscopic sphincterotomy for choledocholithiasis. Gastroenterology. 1996;110:894–9.
Sugiyama M, Atomi Y. Follow-up of more than 10 years after endoscopic sphincterotomy for choledocholithiasis in young patients. Br J Surg. 1998;85:917–21.
Sugiyama M, Atomi Y. Risk factors predictive of late complications after endoscopic sphincterotomy for bile duct stones: long-term (more than 10 years) follow-up study. Am J Gastroenterol. 2002;97:2763–7.
Tanaka M, Takahata S, Konomi H, Matsunaga H, Yokohata K, Takeda T, et al. Long-term consequence of endoscopic sphincterotomy for bile duct stones. Gastrointest Endosc. 1998;48:465–9.
Yasuda I, Tomita E, Enya M, Kato T, Moriwaki H. Can endoscopic papillary balloon dilation really preserve sphincter of Oddi function? Gut. 2001;49:686–91.
Bergman JJ, van Berkel AM, Groen AK, Schoeman MN, Offerhaus J, Tytgat GN, et al. Biliary manometry, bacterial characteristics, bile composition, and histologic changes fifteen to seventeen years after endoscopic sphincterotomy. Gastrointest Endosc. 1997;45:400–5.
Hakamada K, Sasaki M, Endoh M, Itoh T, Morita T, Konn M. Late development of bile duct cancer after sphincteroplasty: a ten- to twenty-two-year follow-up study. Surgery. 1997;121:488–92.
May GR, Cotton PB, Edmunds SE, Chong W. Removal of stones from the bile duct at ERCP without sphincterotomy. Gastrointest Endosc. 1993;39:749–54.
Mathuna PM, White P, Clarke E, Merriman R, Lennon JR, Crowe J. Endoscopic balloon sphincteroplasty (papillary dilation) for bile duct stones: efficacy, safety, and follow-up in 100 patients. Gastrointest Endosc. 1995;42:468–74.
Isayama H, Komatsu Y, Inoue Y, Toda N, Shiratori Y, Tsujino T, et al. Preserved function of the Oddi sphincter after endoscopic papillary balloon dilation. Hepatogastroenterology. 2003;50:1787–91.
Kawabe T, Komatsu Y, Isayama H, Takemura T, Toda N, Tada M, et al. Histological analysis of the papilla after endoscopic papillary balloon dilation. Hepatogastroenterology. 2003;50:919–23.
Bergman JJ, Rauws EA, Fockens P, van Berkel AM, Bossuyt PM, Tijssen JG, et al. Randomised trial of endoscopic balloon dilation versus endoscopic sphincterotomy for removal of bile duct stones. Lancet. 1997;349:1124–9.
Fujita N, Maguchi H, Komatsu Y, Yasuda I, Hasebe O, Igarashi Y, et al. Endoscopic sphincterotomy and endoscopic papillary balloon dilatation for bile duct stones: a prospective randomized controlled multicenter trial. Gastrointest Endosc. 2003;57:151–5.
Disario JA, Freeman ML, Bjorkman DJ, Macmathuna P, Petersen BT, Jaffe PE, et al. Endoscopic balloon dilation compared with sphincterotomy for extraction of bile duct stones. Gastroenterology. 2004;127:1291–9.
Tsujino T, Kawabe T, Komatsu Y, Yoshida H, Isayama H, Sasaki T, et al. Endoscopic papillary balloon dilation for bile duct stone: immediate and long-term outcomes in 1000 patients. Clin Gastroenterol Hepatol. 2007;5:130–7.
Tsujino T, Kawabe T, Isayama H, Sasaki T, Kogure H, Togawa O, et al. Efficacy and safety of low-pressured and short-time dilation in endoscopic papillary balloon dilation for bile duct stone removal. J Gastroenterol Hepatol. 2008;23:867–71.
Cotton PB, Lehman G, Vennes J, Geenen JE, Russell RC, Meyers WC, et al. Endoscopic sphincterotomy complications and their management: an attempt at consensus. Gastrointest Endosc. 1991;37:383–93.
Ito Y, Tsujino T, Togawa O, Yamamoto N, Isayama H, Nakata R, et al. Endoscopic papillary balloon dilation for the management of bile duct stones in patients 85 years of age and older. Gastrointest Endosc. 2008;68:477–82.
Baron TH, Harewood GC. Endoscopic balloon dilation of the biliary sphincter compared to endoscopic biliary sphincterotomy for removal of common bile duct stones during ERCP: a metaanalysis of randomized, controlled trials. Am J Gastroenterol. 2004;99:1455–60.
Heo JH, Kang DH, Jung HJ, Kwon DS, An JK, Kim BS, et al. Endoscopic sphincterotomy plus large-balloon dilation versus endoscopic sphincterotomy for removal of bile duct stones. Gastrointest Endosc. 2007;66:720–6.
Attasaranya S, Cheon YK, Vittal H, Howell DA, Wakelin DE, Cunningham JT, et al. Large-diameter biliary orifice balloon dilation to aid in endoscopic bile duct stone removal: a multicenter series. Gastrointest Endosc. 2008;67:1046–52.
Bergman JJ, Huibregtse K. What is the current status of endoscopic balloon dilation for stone removal? Endoscopy. 1998;30:43–5.
Sugiyama M, Abe N, Atomi Y. Should endoscopic balloon dilation be used for the extraction of bile duct stones? Nat Clin Pract Gastroenterol Hepatol. 2005;2:74–5.
Freeman ML, Nelson DB, Sherman S, Haber GB, Herman ME, Dorsher PJ, et al. Complications of endoscopic biliary sphincterotomy. N Engl J Med. 1996;335:909–18.
Mehta SN, Pavone E, Barkun JS, Bouchard S, Barkun AN. Predictors of post-ERCP complications in patients with suspected choledocholithiasis. Endoscopy. 1998;30:457–63.
Cheng CL, Sherman S, Watkins JL, Barnett J, Freeman M, Geenen J, et al. Risk factors for post-ERCP pancreatitis: a prospective multicenter study. Am J Gastroenterol. 2006;101:139–47.
Kozarek RA. Balloon dilation of the sphincter of Oddi. Endoscopy. 1988;20(Suppl 1):207–10.
Bergman JJ, van Berkel AM, Groen AK, Schoeman MN, Offerhaus J, Tytgat GN, et al. Biliary manometry, bacterial characteristics, bile composition, and histologic changes fifteen to seventeen years after endoscopic sphincterotomy. Gastrointest Endosc. 1997;45:400–5.
Kaufman HS, Magnuson TH, Lillemoe KD, Frasca P, Pitt HA. The role of bacteria in gallbladder and common duct stone formation. Ann Surg. 1989;209:584–91 (Discussion pp. 591–592).
Sugiyama M, Atomi Y. Endoscopic papillary balloon dilation causes transient pancreatobiliary and duodenobiliary reflux. Gastrointest Endosc. 2004;60:186–90.
Paganini AM, Guerrieri M, Sarnari J, De Sanctis A, D’Ambrosio G, Lezoche G, et al. Thirteen years’ experience with laparoscopic transcystic common bile duct exploration for stones. Effectiveness and long-term results. Surg Endosc. 2007;21:34–40.
Ochi Y, Mukawa K, Kiyosawa K, Akamatsu T. Comparing the treatment outcomes of endoscopic papillary dilation and endoscopic sphincterotomy for removal of bile duct stones. J Gastroenterol Hepatol. 1999;14:90–6.
Strömberg C, Luo J, Enochsson L, Arnelo U, Nilsson M. Endoscopic sphincterotomy and risk of malignancy in the bile ducts, liver, and pancreas. Clin Gastroenterol Hepatol. 2008;6:1049–53.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Tsujino, T., Yoshida, H., Isayama, H. et al. Endoscopic papillary balloon dilation for bile duct stone removal in patients 60 years old or younger. J Gastroenterol 45, 1072–1079 (2010). https://doi.org/10.1007/s00535-010-0254-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00535-010-0254-0