Abstract
Background and aim
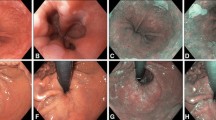
The endoscopic landmark of esophagogastric junction (EGJ) for diagnosis of Barrett’s esophagus (BE) differs between Japan and Western countries. Japanese endoscopists use the distal end of the lower esophageal palisade vessels to localize EGJ. In the West, endoscopists use the proximal gastric folds because of concerns that palisade vessels may be difficult to recognize. We evaluated whether there were differences between American and Japanese endoscopists in the recognition of palisade vessels.
Method
A total of 82 patients were enrolled in this study. Patients were referred for diagnostic esophagogastroduodenoendoscopy (EGD) at the Veterans Affairs Palo Alto Health Care System, from May to July 2008. American and Japanese endoscopists evaluated the EGJ of patients undergoing diagnostic EGD. We analyzed the differences in the recognition of the distal end of palisade vessels. We calculated the kappa statistic to measure interobserver variability.
Results
Based on localization using the distal end of the palisade vessels, American and Japanese endoscopists identified the EGJ in 87.8% (72/82) and 89.0% (73/82) of cases, respectively. The kappa statistic for visualization of EGJ was 0.88 [95% confidence interval (CI): 0.73–1.00].
Conclusion
American and Japanese endoscopists similarly recognized the distal end of palisade vessels as EGJ.

Similar content being viewed by others
References
Blot WJ, Devesa SS, Kneller RW, Fraumeri JF Jr. Rising incidence of adenocarcinoma of the esophagus and gastric cardia. JAMA. 1991;265:1287–9.
Pera M, Cameron AJ, Trastek VF, Carpenter HA, Zinsmeister AR. Increasing incidence of adenocarcinoma of the esophagus and esophagogastric junction. Gastroenterology. 1993;104:510–3.
Shoji T, Hongo M, Fukudo S, Handa M, Inaba H, Kano M, et al. Increasing incident of Barrett’s esophagus and Barrett’s carcinoma in Japan. Gastroenterology. 1999;116:A312. Abstract.
Kusano C, Gotoda T, Christopher JK, Katai H, Kato H, Taniguchi H, et al. Changing trends in the proportion of adenocarcinoma of the esophagogastric junction in a large tertiary referral center in Japan. J Gastroenterol and Hepatol. 2008;23:1662–5.
Hongo M. Review article: Barrett’s oesophagus and carcinoma in Japan. Aliment Pharmacol Ther. 2004;20(suppl 8):50–4.
Ronkainen J, Aro P, Storskrubb T, Johansson SE, Lind T, Bolling-Sternevald E, et al. Prevalence of Barrett’s esophagus in the general population: an endoscopic study. Gastroenterology. 2005;129(6):1825–31.
Kawano T, Kouzu T, Ohara S, Kusano M. The prevalence of Barrett’s mucosa in the Japanese (Japanese with English abstract). Gastroenterol Endosc. 2005;47:951–61.
Spechler SJ, Goyal RK. The columnar-lined esophagus, intestinal metaplasia, and Norman Barrett. Gastroenterology. 1996;110:614–21.
Hoshihara Y, Kosuge T, Yamamoto T, Hashimoto M, Hoteya O. Endoscopic diagnosis of Barrett’s esophagus. Nippon Rinsho. 2005;63:1394–8. (Japanese with English abstract).
Amano K, Adachi K, Katsube T, Watanabe M, Kinoshita Y. Role of hiatus hernia and gastric mucosal atrophy in the development of reflux esophagitis in the elderly. J Gastroenterol Hepatol. 2001;16:132–6.
Sharma P, Dent J, Armstrong D, Bergman JJ, Gossner L, Hoshihara Y, et al. The development and validation of an Endoscopic grading system for Barrett’s esophagus: the Prague C and M criteria. Gastroenteroogy. 2006;131:1392–9.
Sharma P, Mcquaid K, Dent J, Fennerty MB, Sampliner R, Spechler S, et al. A critical review of the diagnosis and management of Barrett’s esophagus: the AGA Chicago Workshop. Gastroenterology. 2004;127:310–30.
Lundell LR, Dent J, Bennett JR, Blum AL, Armstrong D, Galmiche JP, et al. Endoscopic assessment of oesophagitis: clinical and functional correlates and further validation of the Loss Angels classification. Gut. 1999;45:172–80.
de Carvalho CA. Surl’angioarchitecture veineuse de la zone de transition oesophagogastriquw et son interpretation functionnelle. Acta Anat (Basel). 1996;64:125–62.
Noda T. Angioarchitectural study of esophageal varices. With special reference to variceal rupture. Virchows Arch A Pathol Anast Histopathol. 1984;404:381–92.
Amano Y, Ishimura N, Furuta K, Takahashi Y, Chinuki D, Mishima Y, et al. Which landmark results in a more consistent diagnosis of Barrett’s esophagus, the gastric fold or the palisade vessels? Gastrointestinal Endosc. 2006;64:206–11.
Sampliner RE. Practice Parameters Committee of the American College of Gastroenterology. Up dated guidelines for the diagnosis, surveillance, and therapy of Barrett’s esophagus. Am J Gastroenterol. 2002;97:1888–95.
Hirota WK, Loughney TM, Lazas DJ, Maydonovitch CL, Rholl V, Wong RK. Specialized intestinal metaplasia, dysplasia, and cancer of the esophagus and esophagogastric junction: prevalence and clinical data. Gastroenterology. 1999;116:277–85.
Nandurkar S, Talley NJ, Martin CJ, Ng TH, Adams S. Short segment Barrett’s esophagus: prevalence, diagnosis and association. Gut. 1997;40:710–5.
Acknowledgments
The authors thank Dr. Shai Friedland, Tohru Sato, attending fellows, and all of medical staffs who belong to the section of GI endoscopy, Veterans Affairs Palo Alto Health Care System.
Conflict of interest statement
None declared.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Kusano, C., Kaltenbach, T., Shimazu, T. et al. Can Western endoscopists identify the end of the lower esophageal palisade vessels as a landmark of esophagogastric junction?. J Gastroenterol 44, 842–846 (2009). https://doi.org/10.1007/s00535-009-0083-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00535-009-0083-1