Abstract
Background
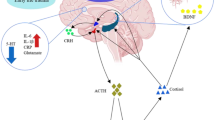
Cancer-related depression is a well-documented condition that significantly impacts long-term quality of life. Brain-derived neurotrophic factor (BDNF), a neurotrophin essential for neurogenesis and neuronal plasticity, has been implicated in various neuropsychological disorders including depression associated with cancer. Cytokines, on the other hand, play a crucial role in regulating depression, potentially by influencing BDNF expression. Transforming growth factor-β (TGF-β), a key immune regulator within the tumor microenvironment, has been found to elevate BDNF levels, establishing a link between peripheral immune responses and depression. The study aims to investigate the correlation of TGF-β and BDNF in cancer-related depression.
Methods
This study involved a cohort of 153 gynecological patients, including 61 patients with gynecological cancer and 92 patients without cancer. Depression levels were assessed using the subscale of Hospital Anxiety and Depression Scale (HADS-D), and TGF-β and BDNF plasma levels were measured using enzyme-linked immunosorbent assay (ELISA).
Results
The study revealed elevated plasma TGF-β levels in patients with cancer (32.24 ± 22.93 ng/ml) compared to those without cancer (25.24 ± 19.72 ng/ml) (P = 0.046). Additionally, reduced levels of BDNF were observed in patients presenting depression symptoms (44.96 ± 41.06 pg/ml) compared to those without depression (133.5 ± 176.7 pg/ml) (P = 0.036). Importantly, a significant correlation between TGF-β and BDNF was found in patients without cancer but with depression (correlation coefficient = 0.893, **P < 0.01). Interestingly, cancer appeared to influence the association between TGF-β and BDNF in patients with depression, as evidenced by a significant difference in the correlation of TGF-β and BDNF between cancer and non-cancer groups (P = 0.041).
Conclusions
These findings underscore the active involvement of TGF-β and BDNF crosstalk in the context of cancer-related depression.


Similar content being viewed by others
Data availability
The data that support the findings of this study are available from the Southern Medical University but restrictions apply to the availability of these data, which were used under license for the current study, and so are not publicly available.
Abbreviations
- BDNF:
-
Brain-derived neurotrophic factor
- TGF-β:
-
Transforming growth factor-β
- HADS:
-
Hospital Anxiety and Depression Scale
- HADS-D:
-
Subscale of Hospital Anxiety and Depression Scale
- ELISA:
-
Enzyme-linked immunosorbent assay
References
Honda K, Goodwin RD (2004) Cancer and mental disorders in a national community sample: findings from the National Comorbidity Survey. Psychother Psychosom 73(4):235–242
Harter M, Baumeister H, Reuter K, Jacobi F, Hofler M, Bengel J, Wittchen HU (2007) increased 12-month prevalence rates of mental disorders in patients with chronic somatic diseases. Psychother Psychosom 76(6):354–360
Dalton SO, Laursen TM, Ross L, Mortensen PB, Johansen C (2009) Risk for hospitalization with depression after a cancer diagnosis: a nationwide, population-based study of cancer patients in Denmark from 1973 to 2003. J Clin Oncol 27(9):1440–1445
Wang JL, Reimer MA, Metz LM, Patten SB (2000) Major depression and quality of life in individuals with multiple sclerosis. Int J Psychiat Med 30(4):309–317
Eaton WW (2002) Epidemiologic evidence on the comorbidity of depression and diabetes. J Psychosom Res 53(4):903–906
Gagnon LM, Patten SB (2002) Major depression and its association with long-term medical conditions. Can J Psychiat 47(2):149–152
Smith EM, Gomm SA, Dickens CM (2003) Assessing the independent contribution to quality of life from anxiety and depression in patients with advanced cancer. Palliative Med 17(6):509–513
Mitchell AJ, Chan M, Bhatti H, Halton M, Grassi L, Johansen C, Meader N (2011) Prevalence of depression, anxiety, and adjustment disorder in oncological, haematological, and palliative-care settings: a meta-analysis of 94 interview-based studies. Lancet Oncol 12(2):160–174
Gabryelska A, Turkiewicz S, Ditmer M, Karuga FF, Strzelecki D, Bialasiewicz P (2022) Sochal M: BDNF and proBDNF serum protein levels in obstructive sleep apnea patients and their involvement in insomnia and depression symptoms. J Clin Med 11(23):7135
Jehn CF, Becker B, Flath B, Nogai H, Vuong L, Schmid P, Lüftner D (2015) Neurocognitive function, brain-derived neurotrophic factor (BDNF) and IL-6 levels in cancer patients with depression. J Neuroimmunol 287:88–92
Marshe V, Maciukiewicz M, Tiwari AK, Freeman N, Kennedy JL, Rotzinger S, Kennedy S, Muller D (2017) Investigating associations between Il-1beta, Il-2, Il-6, Tspo and Bdnf variants and response to duloxetine or placebo treatment in patients with major depression. Eur Neuropsychopharm 27:S187–S188
Hennings JM, Kohli MA, Uhr M, Holsboer F, Ising M, Lucae S (2019) Polymorphisms in the BDNF and BDNFOS genes are associated with hypothalamus-pituitary axis regulation in major depression. Prog Neuro-Psychoph 95:109686
Ochi T, Vyalova NM, Losenkov IS, Levchuk LA, Loonen AJM, Bosker FJ, Simutkin GG, Bokhan NA, Wilffert B, Ivanova SA (2019) Investigating the potential role of BDNF and PRL genotypes on antidepressant response in depression patients: a prospective inception cohort study. Pharmacoepidem Dr S 28:132–132
Meshkat S, Alnefeesi Y, Jawad MY, Di Vincenzo JD, Rodrigues NB, Ceban F, Lui LMW, McIntyre RS, Rosenblat JD (2022) Brain-derived neurotrophic factor (BDNF) as a biomarker of treatment response in patients with treatment resistant depression (TRD): a systematic review & meta-analysis. Psychiat Res 317:114857
Stielow C, Heinen D, Heinzel S, Schwefel M, Teran C, Kallies G, Fydrich T, Rapp M, Heissel A, Strohle A (2022) BDNF at rest and after acute aerobic exercise in women with depression. Med Sci Sport Exer 54(9):89–89
Wang Y, Bai LP, Liu W, Zhu XD, Zhang XY (2022) Altered BDNF levels are associated with cognitive impairment in Parkinson?s disease patients with depression. Parkinsonism Relat D 103:122–128
Shimizu E, Hashimoto K, Okamura N, Koike K, Komatsu N, Kumakiri C, Nakazato M, Watanabe H, Shinoda N, Okada S et al (2003) Alterations of serum levels of brain-derived neurotrophic factor (BDNF) in depressed patients with or without antidepressants. Biol Psychiat 54(1):70–75
Sen S, Duman R, Sanacora G (2008) Serum brain-derived neurotrophic factor, depression, and antidepressant medications: meta-analyses and implications. Biol Psychiat 64(6):527–532
Holubec L, Fiala O, Matejka VM, Podlipny J, Dreslerova J, Vrzalova J, Topolcan O, Finek J, Svoboda T (2012) The difference in the serum levels of Bdnf, Il-6, Il-8, Il-10 and Egf in oncology patients divided according to the presence of symptoms of depression. Ann Oncol 23:474–474
Klein AB, Williamson R, Santini MA, Clemmensen C, Ettrup A, Rios M, Knudsen GM, Aznar S (2011) Blood BDNF concentrations reflect brain-tissue BDNF levels across species. Int J Neuropsychoph 14(3):347–353
Dandekar MP, Saxena A, Scaini G, Shin JH, Migut A, Giridharan VV, Zhou YZ, Barichello T, Soares JC, Quevedo J et al (2019) Medial forebrain bundle deep brain stimulation reverses anhedonic-like behavior in a chronic model of depression: importance of BDNF and inflammatory cytokines. Mol Neurobiol 56(6):4364–4380
Liu BP, Zhang C, Zhang YP, Li KW, Song C (2022) The combination of chronic stress and smoke exacerbated depression-like changes and lung cancer factor expression in A/J mice: involve inflammation and BDNF dysfunction. Plos One 17(11):e0277945
Arosio B, Guerini FR, Voshaar RCO, Aprahamian I (2021) Blood brain-derived neurotrophic factor (BDNF) and major depression: do we have a translational perspective? Front Behav Neurosci 15:626906
Mosiolek A, Mosiolek J, Jakima S, Pieta A, Szulc A (2021) Effects of antidepressant treatment on neurotrophic factors (BDNF and IGF-1) in patients with major depressive disorder (MDD). J Clin Med 10(15):3377
Felger JC, Lotrich FE (2013) Inflammatory cytokines in depression: neurobiological mechanisms and therapeutic implications. Neuroscience 246:199–229
Ayoub S, Berberi A, Fayyad-Kazan M (2020) Cytokines, masticatory muscle inflammation, and pain: an update. J Mol Neurosci 70(5):790–795
Muller HHO, Czwalinna K, Wang RH, Lucke C, Lam AP, Philipsen A, Gschossmann JM, Moeller S (2021) Occurence of post-traumatic stress symptoms, anxiety and depression in the acute phase of transient ischemic attack and stroke. Psychiat Quart 92(3):905–915
Himmerich H, Fulda S, Linseisen J, Seiler H, Wolfram G, Himmerich S, Gedrich K, Kloiber S, Lucae S, Ising M et al (2008) Depression, comorbidities and the TNF-alpha system. Eur Psychiat 23(6):421–429
Enzerink A, Vaheri A (2011) Fibroblast activation in vascular inflammation. J Thromb Haemost 9(4):619–626
Barbierato M, Facci L, Argentini C, Marinelli C, Skaper SD, Giusti P (2013) Astrocyte-microglia cooperation in the expression of a pro-inflammatory phenotype. Cns Neurol Disord-Dr 12(5):608–618
Yirmiya R, Goshen I (2011) Immune modulation of learning, memory, neural plasticity and neurogenesis. Brain Behav Immun 25(2):181–213
Himmerich H, Patsalos O, Lichtblau N, Ibrahim MAA, Dalton B (2019) Cytokine research in depression: principles, challenges, and open questions. Front Psychiatry 10:30
Miller AH, Maletic V, Raison CL (2009) Inflammation and its discontents: the role of cytokines in the pathophysiology of major depression. Biol Psychiat 65(9):732–741
Haroon E, Raison CL, Miller AH (2012) Psychoneuroimmunology meets neuropsychopharmacology: translational implications of the impact of inflammation on behavior. Neuropsychopharmacol 37(1):137–162
Schmidt FM, Lichtblau N, Minkwitz J, Chittka T, Thormann J, Kirkby KC, Sander C, Mergl R, Fasshauer M, Stumvoll M et al (2014) Cytokine levels in depressed and non-depressed subjects, and masking effects of obesity. J Psychiatr Res 55:29–34
Huang W, Gan W, Huang A, Fu YL, Shang YZ, Chen Y, Tian Z, Zhang Y, Fang G (2019) Efficacy of electroacupuncture combined with probiotics for depression and chronic diarrhea in patients and effect on serum inflammatory cytokines. NE and BDNF Exp Ther Med 18(5):3470–3474
Yap NY, Toh YL, Tan CJ, Acharya MM, Chan A (2021) Relationship between cytokines and brain-derived neurotrophic factor (BDNF) in trajectories of cancer-related cognitive impairment. Cytokine 144:155556
Li HY, Shi XH, Yang F, Zhang XR, Li F (2022) Blood inflammatory cytokines as predictors of depression in patients with glioma. Front Psychiatry 13:930985
Binnewies M, Roberts EW, Kersten K, Chan V, Fearon DF, Merad M, Coussens LM, Gabrilovich DI, Ostrand-Rosenberg S, Hedrick CC et al (2018) Understanding the tumor immune microenvironment (TIME) for effective therapy. Nat Med 24(5):541–550
Kartikasari AER, Huertas CS, Mitchell A, Plebanski M (2021) Tumor-induced inflammatory cytokines and the emerging diagnostic devices for cancer detection and prognosis. Front Oncol 11:692142
David CJ, Massague J (2018) Contextual determinants of TGF beta action in development, immunity and cancer. Nat Rev Mol Cell Bio 19(7):419–435
Kumari A, Shonibare Z, Monavarian M, Arend RC, Lee NY, Inman GJ, Mythreye K (2021) TGF beta signaling networks in ovarian cancer progression and plasticity. Clin Exp Metastas 38(2):139–161
Luo FY, Huang Y, Li YL, Zhao XL, Xie Y, Zhang QW, Mei J, Liu XH (2021) A narrative review of the relationship between TGF-β signaling and gynecological malignant tumor. Ann Transl Med 9(20):1601
Dobolyi A, Vincze C, Pál G, Lovas G (2012) The neuroprotective functions of transforming growth factor beta proteins. Int J Mol Sci 13(7):8219–8258
Kim YK, Lee SW, Kim SH, Shim SH, Han SW, Choi SH, Lee BH (2008) Differences in cytokines between non-suicidal patients and suicidal patients in major depression. Prog Neuro-Psychoph 32(2):356–361
Musil R, Schwarz MJ, Riedel M, Dehning S, Cerovecki A, Spellmann I, Arolt V, Muller N (2011) Elevated macrophage migration inhibitory factor and decreased transforming growth factor-beta levels in major depression - no influence of celecoxib treatment. J Affect Disorders 134(1–3):217–225
Caraci F, Spampinato SF, Morgese MG, Tascedda F, Salluzzo MG, Giambirtone MC, Caruso G, Munafò A, Torrisi SA, Leggio GM et al (2018) Neurobiological links between depression and AD: the role of TGF-β1 signaling as a new pharmacological target. Pharmacol Res 130:374–384
Sometani A, Kataoka H, Nitta AI, Fukumitsu H, Nomoto H, Furukawa S (2001) Transforming growth factor-beta 1 enhances expression of brain-derived neurotrophic factor and its receptor, TrkB, in neurons cultured from rat cerebral cortex. J Neurosci Res 66(3):369–376
Zigmond AS, Snaith RP (1983) The Hospital Anxiety and Depression Scale. Acta Psychiat Scand 67(6):361–370
Yang Y, Ding RJ, Hu D, Zhang F, Sheng L (2014) Reliability and validity of a Chinese version of the HADS for screening depression and anxiety in psycho-cardiological outpatients. Compr Psychiat 55(1):215–220
Duman RS, Heninger GR, Nestler EJ (1997) A molecular and cellular theory of depression. Arch Gen Psychiat 54(7):597–606
Murawska-Cialowicz E, Wiatr M, Cialowicz M, de Assis GG, Borowicz W, Rocha-Rodrigues S, Paprocka-Borowicz M, Marques A (2021) BDNF impact on biological markers of depression-role of physical exercise and training. Int J Env Res Pub He 18(14):7553
Park H, Poo MM (2013) Neurotrophin regulation of neural circuit development and function. Nat Rev Neurosci 14(1):7–23
Shen J, Yang L, Wei WS (2022) Dl-3-n-butylphthalide prevents chronic restraint stress-induced depression-like behaviors and cognitive impairment via regulating CaMKII/CREB/BDNF signaling pathway in hippocampus. NeuroReport 33(14):597–603
Wang Z, Wang S, Liu Y, Gao S, Yu YQ, Hu ZL (2021) Serum levels of BDNF in patients with adenoma and colorectal cancer. Dis Markers 2021:8867368
Brierley GV, Priebe IK, Purins L, Fung KYC, Tabor B, Lockett T, Nice E, Gibbs P, Tie J, McMurrick P et al (2013) Serum concentrations of brain-derived neurotrophic factor (BDNF) are decreased in colorectal cancer patients. Cancer Biomark 13(2):67–73
Guzel T, Mech K, Iwanowska M, Wronski M, Slodkowski M (2021) Brain derived neurotrophic factor declines after complete curative resection in gastrointestinal cancer. Peerj 9:e11718
Massague J (2008) TGF beta in cancer. Cell 134(2):215–230
Khanehsar MA, Hoseinbeyki M, Taha MF, Javeri A (2020) Repression of TGF-beta signaling in breast cancer cells by miR-302/367 cluster. Cell J 21(4):444–450
Colak S, ten Dijke P (2017) Targeting TGF-β signaling in cancer. Trends Cancer 3(1):56–71
Sulaiman A, Chambers J, Chilumula SC, Vinod V, Kandunuri R, McGarry S, Kim S (2022) At the intersection of cardiology and oncology: TGFβ as a clinically translatable therapy for TNBC treatment and as a major regulator of post-chemotherapy cardiomyopathy. Cancers 14(6):1577
Yi M, Li TY, Niu MK, Wu YZ, Zhao ZY, Wu KM (2022) TGF-β: a novel predictor and target for anti-PD-1/PD-L1 therapy. Front Immunol 13:1061394
Acknowledgements
The authors would like to express their gratitude to the participants for their willingness to complete the questionnaires, which made this study possible.
Funding
The study was supported by the National Natural Science Foundation of China (grant number: 72004088).
Author information
Authors and Affiliations
Contributions
JJL: performing experiments, data collection, and data analysis, and contributing to writing. LX: methodology, supervision, funding acquisition. XCN: methodology, data analysis, and contributing to writing. ZJW: data collection. YYL: data collection. LLZ: conceptualization, supervision, funding acquisition. YWL: conceptualization, writing the manuscript, supervision, funding acquisition. All authors agree to be accountable for the content of the work.
Corresponding authors
Ethics declarations
Ethics approval and consent to participate
The study was approved by the Medical Ethics Committee of X Hospital of Southern Medical University (NFEC-2020–281). All methods were carried out in accordance with relevant guidelines and regulations. All patients had been provided informed consent before participating this study.
Consent for publication
Not applicable.
Competing interests
The authors declare no competing interests.
Disclaimer
The funding source had no role in the design of this study and did not have any role during its execution, analyses, interpretation of the data, or decision to submit results.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Lin, J., Xiao, L., Nie, X. et al. Investigating the role of TGF-β and BDNF in cancer-related depression: a primary cross-sectional study. Support Care Cancer 32, 365 (2024). https://doi.org/10.1007/s00520-024-08542-y
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s00520-024-08542-y