Abstract
Purpose
To investigate the effectiveness of art-making interventions on physical and psychological outcomes, as well as quality of life (QOL), in adult patients with cancer.
Methods
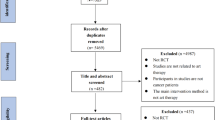
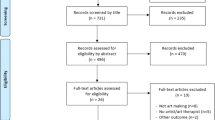
Seven English-language databases (PubMed, Academic Search Premier, EMBASE, CINAHL, PsycINFO, The Cochrane Library, and Web of Science) and three Chinese-language databases (CNKI, WanFang, and VIP) were searched up to and including May 1, 2023. We used the Cochrane Risk of Bias tool 2.0 and the Risk of Bias in Non-Randomized Studies-of Interventions to evaluate the certainty of evidence. The data were analyzed using Review Manager software 5.4. The study protocol was registered with PROSPERO (CRD42022321471).
Results
The studies predominantly focused on visual art (n = 21), two specifically used performing art (n = 2), and five integrated both forms of art-making (n = 5). The pooled results showed that art-making significantly improved anxiety (SMD = − 1.12, 95% CI [− 1.43, − 0.81], p < 0.01), depression (SMD = − 0.91, 95% CI [− 1.16, − 0.65], p < 0.01), distress (SMD = − 1.19, 95% CI [− 1.43, − 0.95], p < 0.01), psychological well-being (SMD = 0.41, 95% CI [0.02, 0.80], p = 0.04), societal well-being (SMD = 0.29, 95% CI [0.04, 0.54], p = 0.03), nausea (SMD = − 1.81, 95% CI [− 2.84, − 0.78], p < 0.01), physical well-being (SMD = 0.11, 95% CI [0.02, 0.20], p = 0.02), and QOL (SMD = 0.81, 95% CI [0.29, 1.33], p < 0.01). However, it did not significantly improve fatigue (SMD = − 0.28, 95% CI [− 0.75, 0.19], p = 0.24) and pain (SMD = − 0.18, 95% CI [− 1.97, 1.60], p = 0.84) in patients with cancer.
Conclusions
Art-making interventions may boost psychological well-being, physical symptoms, and QOL among patients with cancer. More robust studies are necessary to overcome methodological limitations and promote wider adoption of these interventions.
Trial registration
Prospero registration number: CRD42022321471.











Similar content being viewed by others
Data availability
The data that support the findings of this systematic review are all presented in tables, appendixes, and figures.
References
Sung H, Ferlay J, Siegel RL, Laversanne M, Soerjomataram I, Jemal A, Bray F (2021) Global cancer statistics 2020: GLOBOCAN estimates of incidence and mortality worldwide for 36 cancers in 185 countries. CA: Cancer J Clinic 71(3):209–249. https://doi.org/10.3322/caac.21660
Hong HC, Min A, Kim YM (2023) A systematic review and pooled prevalence of symptoms among childhood and adolescent and young adult cancer survivors. J Clin Nurs 32(9–10):1768–1794. https://doi.org/10.1111/jocn.16201
Hong HC, Kim YM, Min A (2022) Factors influencing quality of life among childhood cancer survivors in Korea: a quantile regression approach. Res Nurs Health 45(1):108–122. https://doi.org/10.1002/nur.22170
Paley CA, Boland JW, Santarelli M, Murtagh FEM, Ziegler L, Chapman EJ (2023) Non-pharmacological interventions to manage psychological distress in patients living with cancer: a systematic review. BMC Palliat Care 22(1):88. https://doi.org/10.1186/s12904-023-01202-8
Kim KS, Lor M (2022) Art making as a health intervention: concept analysis and implications for nursing interventions. Adv Nurs Sci 45(2):155–169. https://doi.org/10.1097/ANS.0000000000000412
Puetz TW, Morley CA, Herring MP (2013) Effects of creative arts therapies on psychological symptoms and quality of life in patients with cancer. JAMA Intern Med 173(11):960–969. https://doi.org/10.1001/jamainternmed.2013.836
Zhang Y (2021) Effects of art therapy group assisted hospice care on cancer-related fatigue and stress response in patients with advanced esophageal cancer. Nursing Practice and Research 18(2):271–274. https://doi.org/10.3969/j.issn.1672-9676.2021.02.032
Collette N, Gueell E, Farinas O, Pascual A (2021) Art therapy in a palliative care unit: symptom relief and perceived helpfulness in patients and their relatives. J Pain Symptom Manage 61(1):103–111. https://doi.org/10.1016/j.jpainsymman.2020.07.027
De Feudis L, Graziano G, Lanciano T, Garofoli M, Lisi A, Marzano N (2021) An art therapy group intervention for cancer patients to counter distress before chemotherapy. Arts & Health 13(1):35–48. https://doi.org/10.1080/17533015.2019.1608566
Kaimal G, Carroll-Haskins K, Mensinger JL, Dieterich-Hartwell R, Biondo J, Levin WP (2020) Outcomes of therapeutic artmaking in patients undergoing radiation oncology treatment: a mixed-methods pilot study. Integr Cancer Ther 19:1–14. https://doi.org/10.1177/1534735420912835
Akbulak F, Can G (2023) Effectiveness of mandala coloring in reducing anxiety in women with early-stage breast cancer receiving chemotherapy for the first time. Explore (New York, N.Y.) 19(1):42–47. https://doi.org/10.1016/j.explore. 2022.04.007
Cai J, Wang CL (2022) Effect of painting therapy on chemotherapy ⁃ induced nausea, vomiting and anxiety in patients with breast cancer. Chinese Nursing Res 36(21):3890–3896. https://doi.org/10.12102/j.issn.1009-6493.2022.21.023
Yang LL, Su L (2021) Effect of painting therapy on emotion and quality of life in breast cancer patients undergoing chemotherapy. Modern Clinical Nursing 21(9):55–61. https://doi.org/10.3969/j.issn.1671-8283.2022.09.009
Joly F, Pasquier D, Levy C, Mousseau M, D’Almeida MC, Noal S, Le Tinier F, Geffrelot J, Ciais C, Szymczak V, Leon C, Rousselot MP, Darbas S, Hanzen C, Heutte N (2022) Impact of creative art therapy on fatigue and quality of life in patients treated for localized breast cancer: a randomized study. Psychooncology 31(8):1412–1419. https://doi.org/10.1002/pon.5940
Xie R, Luo RJ, Chen WL, Wan H (2022) Effects of dance movement therapy on cancer related fatigue and nutritional status of young and middle-aged female breast cancer patients with chemotherapy. Chinese Journal of Practical Nursing 38(14):1074–1079. https://doi.org/10.3760/cma.j.cn211501-20210609-01636
Li C, Ma DY, Li FL, He M, Yang N, Mai XR, Yang CM (2020) Innovation and practice of care model in female cancer ward based on expressive art therapy. J Kunming Med Univ 41(9):167–170
Czamanski-Cohen J, Wiley JF, Sela N, Caspi O, Weihs K (2019) The role of emotional processing in art therapy (REPAT) for breast cancer patients. J Psychosoc Oncol 37(5):586–598. https://doi.org/10.1080/07347332.2019.1590491
Puig A, Lee SM, Goodwin L, Sherrard PA (2006) The efficacy of creative arts therapies to enhance emotional expression, spirituality, and psychological well-being of newly diagnosed stage I and stage II breast cancer patients: a preliminary study. Arts Psychother 33(3):218–228. https://doi.org/10.1016/j.aip.2006.02.004
Wiswell S, Bell JG, McHale J, Elliott JO, Rath K, Clements A (2019) The effect of art therapy on the quality of life in patients with a gynecologic cancer receiving chemotherapy. Gynecol Oncol 152(2):334–338. https://doi.org/10.1016/j.ygyno.2018.11.026
Hanser SB, Bauer-Wu S, Kubicek L, Healey M, Manola J, Hernandez M, Bunnell C (2006) Effects of a music therapy intervention on quality of life and distress in women with metastatic breast cancer. J Soc Integr Oncol 4(3):116–124. https://doi.org/10.2310/7200.2006.014
Mische Lawson L, Glennon C, Fiscus V, Harrell V, Krause K, Moore AB, Smith K (2016) Effects of making art and listening to music on symptoms related to blood and marrow transplantation. Oncol Nurs Forum 43(2):E56–E63. https://doi.org/10.1188/16.ONF.E56-E63
Ando M, Imamura Y, Kira H, Nagasaka T (2013) Feasibility and efficacy of art therapy for Japanese cancer patients: a pilot study. Arts Psychother 40(1):130–133. https://doi.org/10.1016/j.aip.2012.12.007
Pamelia EM (2015) Therapeutic art-making and art therapy: similarities and differences and a resulting framework (Master’s thesis). Retrieved from https://scholarworks.iupui.edu/handle/1805/6900
Elkis-Abuhoff DL, Goldblatt RB, Gaydos M, Convery C (2013) A pilot study to determine the psychological effects of manipulation of therapeutic art forms among patients with Parkinson’s disease. International Journal of Art Therapy 18(3):113–121. https://doi.org/10.1080/17454832.2013.797481
Archer S, Buxton S, Sheffield D (2015) The effect of creative psychological interventions on psychological outcomes for adult cancer patients: a systematic review of randomised controlled trials. Psychooncology 24(1):1–10. https://doi.org/10.1002/pon.3607
Kim KS, Loring S, Kwekkeboom K (2018) Use of art-making intervention for pain and quality of life among cancer patients: a systematic review. J Holist Nurs 36(4):341–353. https://doi.org/10.1177/0898010117726633
Ennis G, Kirshbaum M, Waheed N (2018) The beneficial attributes of visual art-making in cancer care: an integrative review. Eur J Cancer Care 27(1). https://doi.org/10.1111/ecc.12663
Deng X, An S, Cheng C (2019) Cultural differences in the implicit and explicit attitudes toward emotion regulation. Personality Individ Differ 149:220–222. https://doi.org/10.1016/j.paid.2019.05.057
Xiao JN, Chow KM, Chan CW, Li M, Deng Y (2020) Qualitative study on perceived dignity of cancer patients undergoing chemotherapy in China. Support Care Cancer 28:2921–2929. https://doi.org/10.1007/s00520-019-05123-2
Higgins JP, Savović J, Page MJ, Elbers RG, Sterne JA (2022) Cochrane handbook for systematic reviews of interventions, version 6.1. https://training.cochrane.org/handbook/current/chapter-08/
Sterne JA, Hernan MA, Reeves BC, Savovic J, Berkman ND, Viswanathan M, Henry D, Altman DG, Ansari MT, Boutron I, Carpenter JR, Chan AW, Churchill R, Deeks JJ, Hrobjartsson A, Kirkham J, Juni P, Loke YK, Pigott TD, Ramsay CR, Regidor D, Rothstein HR, Sandhu L, Santaguida PL, Schunemann HJ, Shea B, Shrier I, Tugwell P, Turner L, Valentine JC, Waddington H, Waters E, Wells GA, Whiting PF, Higgins JP (2016) ROBINS-I: a tool for assessing risk of bias in non-randomised studies of interventions. BMJ 355:i4919. https://doi.org/10.1136/bmj.i4919
Higgins JP, Thompson SG, Deeks JJ, Altman DG (2003) Measuring inconsistency in meta-analyses. BMJ 327(7414):557–560. https://doi.org/10.1136/bmj.327.7414.557
Fu WJ, Huang Y, Liu X, Ren JH, Zhang MQ (2020) The effect of art therapy in women with gynecologic cancer: a systematic review. Evidence-based Complementary and Alternative Medicine 2020:8063172. https://doi.org/10.1155/2020/8063172
Qian JL, Zhou XL, Sun XS, Wu MW, Sun SW, Yu XY (2020) Effects of expressive writing intervention for women’s PTSD, depression, anxiety and stress related to pregnancy: a meta-analysis of randomized controlled trials. Psychiatry Res 288:112933. https://doi.org/10.1016/j.psychres.2020.112933
Klagsbrun J, Rappaport L, Speiser VM, Post P, Byers J, Stepakoff S, Karman S (2005) Focusing and expressive arts therapy as a complementary treatment for women with breast cancer. J Creat Ment Health 1(1):107–137. https://doi.org/10.1300/J456v01n01_08
Sun YQ, Du KY, Li QM, Zhang X (2017) Application of painting art therapy in the postoperative rehabilitation of breast cancer patients. Hebei Medical Journal 39(11):1743–1745. https://doi.org/10.3969/j.issn.1002-7386.2017.11.042
Glinzak L (2016) Effects of art therapy on distress levels of adults with cancer: a proxy pretest study. Art Ther 33(1):27–34. https://doi.org/10.1080/07421656.2016.1127687
Liou KT, Lynch KA, Nwodim O, Popkin K, Greene JS, Atkinson TM, Bradt J, Mao JJ (2022) Comparison of depressive symptom outcomes in hospitalized adult cancer patients receiving music therapy or massage therapy. J Pain Symptom Manage 63(2):e155–e159. https://doi.org/10.1016/j.jpainsymman.2021.09.007
Radl D, Vita M, Gerber N, Gracely EJ, Bradt J (2018) The effects of Self-Book© art therapy on cancer-related distress in female cancer patients during active treatment: a randomized controlled trial. Psychooncology 27(9):2087–2095. https://doi.org/10.1002/pon.4758
Nainis N, Paice JA, Ratner J, Wirth JH, Lai J, Shott S (2006) Relieving symptoms in cancer: innovative use of art therapy. J Pain Symptom Manage 31(2):162–169. https://doi.org/10.1016/j.jpainsymman.2005.07.006
Shen LF, Zhu H, Sun MR, Jin AX (2022) Application of virtual interaction painting therapy on emotional disorders of postoperative oral cancer patients. Rehabilitation and Nursing 21(4):10–19. https://doi.org/10.3969/j.issn.167-9875,2022.04.003
Bell JG, McHale J, Elliott JO, Heaton W (2022) The impact of art therapy on anxiety and hope in patients with gynecologic cancer undergoing chemotherapy. Arts Psychother 80:101947. 10.10 16/j.aip.2022.101947
Liu X, Zhang MQ, Jiang SS, Tan Y, Hou XN, Li LL, Xu TJ (2022) Application of painting therapy in perioperative nursing of gynecological cancer patients. Chinese General Practice Nursing 20(25):3527–3530. https://doi.org/10.1204/j.issn.1674-4748.2022.25.019
Song WZ (2021) Construction and application of group painting therapy in perioperative neuropsychological symptom group with primary liver cancer (Master’s thesis). Retrieved from https://kns.cnki.net/KCMS/detail/detail.aspx?dbname=CMFD202201&filename=1021699237.nh.
Zhou CC, Wang CL, Ren QL, Wu, Y (2022) Effects of painting therapy on chemotherapy⁃induced nausea and vomiting and quality of life in female patients with lung cancer. Chinese Nursing Res 34(15):2788–2792. https://doi.org/10.12102/j.issn.1009-6493.2020.15.039
Su LY, Xing YR, Li HZ (2022) Application of mandala painting therapy in patients with primary liver cancer undergoing radiofrequency ablation. Henan Medical Research 31(17):3227–3231. https://doi.org/10.3969/j.issn.1004-437X.2022.17.047
Lewandowska A, Rudzki G, Lewandowski T, Próchnicki M, Rudzki S, Laskowska B, Brudniak J (2020) Quality of life of cancer patients treated with chemotherapy. Int J Environ Res Public Health 17(19):6938. https://doi.org/10.3390/ijerph17196938
Xu L, Cheng PF, Wu Y, Zhang JX, Zhu JY, Cui JW, Yu RX (2022) The effects of art therapy on anxiety and depression in breast cancer patients: an updated meta-analysis. Eur J Cancer Care 29(5):e13266. https://doi.org/10.1111/ecc.13266
Jiang XH, Chen XJ, Xie QQ, Feng YS, Chen S, Peng JS (2022) Effects of art therapy in cancer care: a systematic review and meta-analysis. Eur J Cancer Care 29(5):e13277. https://doi.org/10.1111/ecc.13277
Czamanski-Cohen J, Weihs KL (2016) The bodymind model: a platform for studying the mechanisms of change induced by art therapy. Arts Psychother 51:63–71. https://doi.org/10.1016/j.aip.2016.08.006
Tang Y, Fu F, Gao H, Shen L, Chi I, Bai Z (2019) Art therapy for anxiety, depression, and fatigue in females with breast cancer: a systematic review. J Psychosoc Oncol 37(1):79–95. https://doi.org/10.1080/07347332.2018.1506855
Wahbeh H, Svalina MN, Oken BS (2014) Group, one-on-one, or internet? Preferences for mindfulness meditation delivery format and their predictors. Open Medicine Journal 1:66–74. https://doi.org/10.2174/1874220301401010066
Riba MB, Donovan KA, Ahmed K, Andersen B, Braun I, Breitbart WS, Brewer BW, Corbett C, Fann J, Fleishman S, Garcia S, Greenberg DB, Handzo GF, Hoofring LH, Huang CH, Hutchinson S, Johns S, Keller J, Kumar P, Lahijani S, Martin S, Niazi SK, Pailler M, Parnes F, Rao V, Salman J, Scher E, Schuster J, Teply M, Usher A, Valentine AD, Vanderlan J, Lyons MS., McMillian NR, Darlow SD (2023) NCCN Guidelines(R) Insights: Distress Management, Version 2.2023. J Natl Compr Canc Net 21(5):450–457. https://doi.org/10.6004/jnccn.2023.0026
Abrahams H, Gielissen M, Schmits IC, Verhagen C, Rovers MM, Knoop H (2016) Risk factors, prevalence, and course of severe fatigue after breast cancer treatment: a meta-analysis involving 12327 breast cancer survivors. Ann Oncol 27(6):965–974. https://doi.org/10.1093/annonc/mdw099
Hagan R, Manktelow R, Taylor BJ, Mallett J (2014) Reducing loneliness amongst older people: a systematic search and narrative review. Aging Ment Health 18(6):683–693. https://doi.org/10.1080/13607863.2013.875122
Boehm K, Cramer H, Staroszynski T, Ostermann T (2014) Arts therapies for anxiety, depression, and quality of life in breast cancer patients: a systematic review and meta-analysis. Evidence-Based Complement Altern Med 103297. https://doi.org/10.1155/2014/103297
Acknowledgements
We are grateful for the English editing services from Rachel Arbing and the assistance in literature search from the library staff of Fujian Medical University.
Funding
This work was supported by the General Project of Fujian Provincial Nature Science Foundation (grant no. 2021J01246) and NIH/NIMH P30MH058107 (PI: Steven Shoptaw).
Author information
Authors and Affiliations
Contributions
Feifei Huang and Wei-Ti Chen made substantial contributions to design this systematic review and data conversion, as well as agreed to be accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved. Qiuhong Chen and Yonglin Li conducted database searches. Jialing Lin and Xiujing Lin selected the studies, extracted the data from the original articles, and assessed the quality of the studies. Jialing Lin was involved in drafting the manuscript. All authors gave final approval of the version to be published.
Corresponding authors
Ethics declarations
Conflict of interest
The authors declare no competing interests.
Statistics
a. The authors have checked to make sure that our submission conforms as applicable to the Journal’s statistical guidelines described here.
b. The statistics were checked prior to submission by an expert statistician Jianqing Zheng (Email: 18060108268@189.cn).
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Lin, J., Lin, X., Chen, Q. et al. The effects of art-making intervention on mind–body and quality of life in adults with cancer: a systematic review and meta-analysis. Support Care Cancer 32, 186 (2024). https://doi.org/10.1007/s00520-024-08364-y
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s00520-024-08364-y