Abstract
Purpose
This study aimed to identify the heterogeneity of dyadic quality of life (QoL) profiles, determine whether these profiles differ in terms of demographic and medical factors, neuroticism, resilience, and family functioning, and explore the combined effect of patient and caregiver neuroticism, resilience, and family functioning on dyadic QoL profiles.
Methods
A cross-sectional study was conducted with 304 advanced lung cancer patient-caregiver dyads. Self-report questionnaires were administered to patient-caregiver dyads to assess demographic and medical characteristics, neuroticism, resilience, family functioning, and QoL.
Results
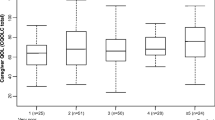
The latent profile analysis identified four subgroups of dyadic QoL: patient-low-caregiver-high profile (38.82%), patient-high-caregiver-high profile (22.37%), patient-high-caregiver-low profile (19.74%), and patient-low-caregiver-low profile (19.08%). Additionally, when both patients and their caregivers had a high level of neuroticism or low level of resilience and low family functioning, compared with only member having them, there was a higher risk of poorer dyadic QoL.
Conclusions
Our study identified the four heterogeneities of dyadic QoL profiles among advanced lung cancer patient-caregiver dyads. Future dyadic interventions should consider the heterogeneity of dyadic QoL in this population and prioritize patient-caregiver dyads at risk of poor dyadic QoL. Furthermore, when high neuroticism, low resilience, or family functioning coexist between patients and their caregivers, both parties exhibit much lower dyadic QoL.

Similar content being viewed by others
Data availability
The data of this study can be available from the corresponding author.
Code availability
N/A.
References
World Health Organization (2021) China - The global cancer observatory. https://gco.iarc.fr/today/data/factsheets/populations/160-china-fact-sheets.pdf. Accessed Mar 2021
Reale ML, Di Maio M (2020) Quality of life in patients with lung cancer: the way forward. Lancet Oncol 21(5):617–619. https://doi.org/10.1016/S1470-2045(20)30151-0
Cancer Statistics Review (2020) Previous version: SEER cancer statistics review, pp. 1975–2012. https://seer.cancer.gov/archive/csr/1975_2012/. Accessed 22 Aug 2020
Lopez-Class M, Gomez-Duarte J, Graves K, Ashing-Giwa K (2012) A contextual approach to understanding breast cancer survivorship among Latinas. Psychooncology 21(2):115–124. https://doi.org/10.1002/pon.1998
Luo X, Gao L, Li J, Lin Y, Zhao J, Li Q (2019) A critical literature review of dyadic web-based interventions to support cancer patients and their caregivers, and directions for future research. Psychooncology 29(1):38–48. https://doi.org/10.1002/pon.5278
Kelley HH, Thibaut JW (1978) Interpersonal relations: a theory of interdependence. New York: Wiley
Streck BP, Wardell DW, LoBiondo-Wood G, Beauchamp JES (2020) Interdependence of physical and psychological morbidity among patients with cancer and family caregivers: review of the literature. Psychooncology 29(6):974–989. https://doi.org/10.1002/pon.5382
Lyons KS, Lee CS (2020) The association of dyadic symptom appraisal with physical and mental health over time in care dyads living with lung cancer. J Fam Nurs 26(1):15–25. https://doi.org/10.1177/1074840719889967
Bauer D, Shanahan M (2007) Modeling complex interactions: person-centered and variable-centered approaches. In: Little T, Bovaird J, Card NA (eds) Modeling contextual effects in longitudinal studies. Erlbaum, pp 255–284
Li Q, Chiang VCL, Xu X, Xu Y, Loke AY (2015) The experiences of Chinese couples living with cancer: a Focus Group Study. Cancer Nurs 38(5):383–394. https://doi.org/10.1097/NCC.0000000000000196
Yu DSF, Cheng ST, Wang J (2018) Unravelling positive aspects of caregiving in dementia: an integrative review of research literature. Int J Nurs Stud 79:1–26. https://doi.org/10.1016/j.ijnurstu.2017.10.008
Galvin M, Gavin T, Mays I, Heverin M, Hardiman O (2020) Individual quality of life in spousal ALS patient–caregiver dyads. Health Qual Life Outcomes 18(1):371. https://doi.org/10.1186/s12955-020-01551-5
Lee CS, Lyons KS (2019) Patterns, relevance, and predictors of dyadic mental health over time in lung cancer. Psychooncology 28(8):1721–1727. https://doi.org/10.1002/pon.5153
Lyons KS, Lee CS (2018) The theory of dyadic illness management. J Fam Nurs 24(1):8–28. https://doi.org/10.1177/1074840717745669
Lazarus RS, Folkman S (1984) Stress, appraisal, and coping. Springer, Berlin
Macía P, Gorbeña S, Gómez A, Barranco M, Iraurgi I (2020) Role of neuroticism and extraversion in the emotional health of people with cancer. Heliyon 6(7):e04281. https://doi.org/10.1016/j.heliyon.2020.e04281
Dunne S, Mooney O, Coffey L, Sharp L, Desmond D, Timon C et al (2017) Psychological variables associated with quality of life following primary treatment for head and neck cancer: a systematic review of the literature from 2004 to 2015. Psychooncology 26(2):149–160. https://doi.org/10.1002/pon.4109
Kim SK, Park M, Lee Y, Choi SH, Moon SY, Seo SW et al (2017) Influence of personality on depression, burden, and health-related quality of life in family caregivers of persons with dementia. Int Psychogeriatr 29(2):227–237. https://doi.org/10.1017/S1041610216001770
Carver CS (1998) Resilience and thriving: Issues, models, and linkages. J Soc Issues 54(2):245–266. https://doi.org/10.1111/0022-4537.641998064
Tian J, Hong JS (2014) Assessment of the relationship between resilience and quality of life in patients with digestive cancer. World J Gastroenterol 20(48):18439–18444. https://doi.org/10.3748/wjg.v20.i48.18439
Üzar-Özçeti NYS, Dursun Sİ (2020) Quality of life, caregiver burden, and resilience among the family caregivers of cancer survivors. Eur J Oncol Nurs 48:101832. https://doi.org/10.1016/j.ejon.2020.101832
Li C, Lu H, Qin W, Li X, Yu J, Fang F (2019) Resilience and its predictors among Chinese liver cancer patients undergoing transarterial chemoembolization. Cancer Nurs 42(5):E1–E9. https://doi.org/10.1097/NCC.0000000000000640
Kołtuniuk A, Rozensztrauch A, Budzińska P, Rosińczuk J (2019) The quality of life of Polish children with cerebral palsy and the impact of the disease on the family functioning. J Pediatr Nurs 47:e75–e82. https://doi.org/10.1016/j.pedn.2019.05.011
Lim JW, Ashing-Giwa KT (2013) Is family functioning and communication associated with health-related quality of life for Chinese- and Korean-American breast cancer survivors? Qual Life Res Int J Qual Life Asp Treat Care Rehab 22(6):1319–1329. https://doi.org/10.1007/s11136-012-0247-y
Carciofo R, Yang J, Song N, Du F, Zhang K (2016) Psychometric evaluation of Chinese-language 44-item and 10-item big five personality inventories, including correlations with chronotype, mindfulness and mind wandering. PLoS ONE 11(2):e0149963. https://doi.org/10.1371/journal.pone.0149963
Wang L, Shi Z, Zhang Y, Zhang Z (2010) Psychometric properties of the 10-item Connor-Davidson Resilience Scale in Chinese earthquake victims. Psychiatry Clin Neurosci 64(5):499–504. https://doi.org/10.1111/j.1440-1819.2010.02130.x
Liu P, He M (1999) Family assessment device, FAD. In Wang X, Wang X & Ma H. (Eds.), Handbook of Mental Health Rating Scales (Supplement, pp. 149–152). Chinese Mental Health Journal. (Chinese)
Wang S, Luan R, Lei Y, Kuang C, He C, Chen Y (2007) Development and evaluation of Chinese version of short form 8. Modern Prev Med 34(6):1022–1023. https://doi.org/10.3969/j.issn.1003-8507.2007.06.009
Schnettler B, Grunert KG, Orellana L, Miranda H, Lobos G, Miranda-Zapata E et al (2021) The diverging patterns of life satisfaction between families: A latent profile analysis in dual-earner parents with adolescents. Current Psychology (Advance online publication). https://doi.org/10.1007/s12144-020-01316-9
Carragher N, Adamson G, Bunting B, McCann S (2009) Subtypes of depression in a nationally representative sample. J Affect Disord 113(1–2):88–99. https://doi.org/10.1016/j.jad.2008.05.015
Li Q, Xu Y, Zhou H, Loke AY (2016) Factors influencing the health-related quality of life of Chinese advanced cancer patients and their spousal caregivers: a cross-sectional study. BMC Palliat Care 15(1):72. https://doi.org/10.1186/s12904-016-0142-3
Abdullah NN, Idris IB, Shamsuddin K, Abdullah NMA (2020) Health-related quality of life in Malaysian gastrointestinal cancer patients and their family caregivers—a comparison study. Support Care Cancer 28(4):1891–1899. https://doi.org/10.1007/s00520-019-05007-5
Lin Y, Hu C, Xu Y, Zhao J, Li Q (2020) The mutual impact and moderating factors of quality of life between advanced cancer patients and their family caregivers. Support Care Cancer 28(11):5251–5262. https://doi.org/10.1007/s00520-020-05351-x
Chen JE, Lou VW, Jian H, Zhou Z, Yan M, Zhu J et al (2018) Objective and subjective financial burden and its associations with health-related quality of life among lung cancer patients. Support Care Cancer 26(4):1265–1272. https://doi.org/10.1007/s00520-017-3949-4
Lathan CS, Cronin A, Tucker-Seeley R, Zafar SY, Ayanian JZ, Schrag D (2016) Association of financial strain with symptom burden and quality of life for patients with lung or colorectal cancer. J Clin Oncol 34(15):1732–1740. https://doi.org/10.1200/JCO.2015.63.2232
Laird BJA, Fallon M, Hjermstad MJ, Tuck S, Kaasa S, Klepstad P et al (2016) Quality of life in patients with advanced cancer: differential association with performance status and systemic inflammatory response. J Clin Oncol 34(23):2769–2775. https://doi.org/10.1200/JCO.2015.65.7742
Hsu T, Nathwani N, Loscalzo M, Chung V, Chao J, Karanes C et al (2019) Understanding caregiver quality of life in caregivers of hospitalized older adults with cancer. J Am Geriatr Soc 67(5):978–986. https://doi.org/10.1111/jgs.15841
Ma Y, He B, Jiang M, Yang Y, Wang C, Huang C et al (2020) Prevalence and risk factors of cancer-related fatigue: a systematic review and meta-analysis. Int J Nurs Stud 111:103707. https://doi.org/10.1016/j.ijnurstu.2020.103707
Lahey BB (2009) Public health significance of neuroticism. Am Psychol 64(4):241–256. https://doi.org/10.1037/a0015309
Zhang J, Yu NX, Zhou M, Zhang J (2017) Dyadic effects of resilience on well-being in Chinese older couples: mediating role of spousal support. J Fam Psychol: JFP: J Div Fam Psychol Am Psychol Assoc 31(3):273–281. https://doi.org/10.1037/fam0000250
Connor KM, Davidson JRT (2003) Development of a new resilience scale: the Connor-Davidson Resilience Scale (CD-RISC). Depress Anxiety 18(2):76–82. https://doi.org/10.1002/da.10113
Lim JW, Shon EJ (2018) The dyadic effects of family cohesion and communication on health-related quality of life: the moderating role of sex. Cancer Nurs 41(2):156–165. https://doi.org/10.1097/NCC.0000000000000468
Wang H, Yue H, Ren M, Feng D (2021) Dyadic effects of family-functioning and resilience on quality of life in advanced lung cancer patients and caregivers: an actor-partner interdependence mediation model. Eur J Oncol Nurs 52:101963. https://doi.org/10.1016/j.ejon.2021.101963
Shin DW, Shin J, Kim SY, Yang HK, Cho J, Youm JH et al (2016) Family avoidance of communication about cancer: a dyadic examination. Cancer Res Treat 48(1):384–392. https://doi.org/10.4143/crt.2014.280
Li Y, Wang K, Yin Y, Li Y, Li S (2018) Relationships between family resilience, breast cancer survivors’ individual resilience, and caregiver burden: a cross-sectional study. Int J Nurs Stud 88:79–84. https://doi.org/10.1016/j.ijnurstu.2018.08.011
Acknowledgements
This study was funded by the Young Scholars Program of Shandong University (grant number: 2017WLJH42). The authors would like to thank all the participants in this study. This study could not have been completed without their support.
Author information
Authors and Affiliations
Contributions
Hui Wang: conceptualization, investigation, methodology, writing original draft; Tiantian Deng: conceptualization, investigation, methodology, writing-review; Cong Cao: conceptualization, methodology, writing-review; Danjun Feng: funding acquisition, conceptualization, methodology, supervision. All the authors have read and approved the final version of the manuscript.
Corresponding author
Ethics declarations
Ethical approval
This study was approved by the ethics review board of the School of Nursing and Rehabilitation at Shandong University and was conducted following tenets of the Declaration of Helsinki.
Consent to participate
Informed consent was obtained from all participants in this study.
Consent for publication
All authors approved the final paper for publication.
Conflicts of interest
The authors have no relevant financial or non-financial interests to disclose.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Posted history
This manuscript was previously posted to bioRxiv: https://www.researchsquare.com/article/rs-1199351/v1.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Wang, H., Deng, T., Cao, C. et al. Distinct dyadic quality of life profiles among patient-caregiver dyads with advanced lung cancer: a latent profile analysis. Support Care Cancer 31, 704 (2023). https://doi.org/10.1007/s00520-023-08182-8
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s00520-023-08182-8