Abstract
Purpose
Cannabis use among patients with cancer is common, yet data are limited regarding use patterns, reasons for use, and degree of benefit, which represents an unmet need in cancer care delivery. This need is salient in states without legal cannabis programs, where perceptions and behavior among providers and patients may be affected.
Methods
A cross-sectional survey of patients with cancer and survivors at the Hollings Cancer Center at the Medical University of South Carolina (no legal cannabis marketplace in SC) was completed as part of the NCI Cannabis Supplement. Patients (ages 18 +) were recruited using probability sampling from patient lists (N = 7749 sampled; N = 1036 completers). Weight-adjusted Chi-square tests compared demographics and cancer details among patients using cannabis since diagnosis versus those not using cannabis, while weighted descriptives are presented for cannabis use prevalence, consumption, symptom management, and legalization beliefs.
Results
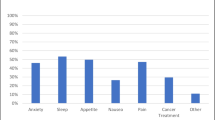
Weighted prevalence of cannabis use since diagnosis was 26%, while current cannabis use was 15%. The most common reasons for cannabis use after diagnosis were difficulty sleeping (50%), pain (46%), and mood changes and stress, anxiety, or depression (45%). Symptom improvement was endorsed for pain (57%), stress/anxiety/depression (64%), difficulty sleeping (64%), and loss of appetite (40%).
Conclusions
Among patients with cancer and survivors at a NCI-designated cancer center within SC, a state without legal access to medical cannabis, prevalence rates, and reasons for cannabis use are consistent with emerging literature in oncology populations. These findings have implications for care delivery, and work is needed to inform recommendations for providers and patients.





Similar content being viewed by others
Data Availability
The final dataset will be made available to qualified requestors in accordance with NIH Data Sharing Policies and with an executed data use agreeement between MUSC and the requestor. Requests for de-identified data access should be made directly to the corresponding author (Dr. Erin McClure).
References
Pergam SA et al (2017) Cannabis use among patients at a comprehensive cancer center in a state with legalized medicinal and recreational use. Cancer 123(22):4488–4497
Martell K et al (2018) Rates of cannabis use in patients with cancer. Curr Oncol 25(3):219–225
Do EK et al (2021) Cannabis use among cancer survivors in the United States: analysis of a nationally representative sample. Cancer 127(21):4040–4049
Lee M et al (2023) Marijuana use among US adults with cancer: findings from the 2018–2019 Behavioral Risk Factor Surveillance System. J Cancer Surviv 17(4):1161–1170
Cousins MM et al (2021) Prevalence of cannabis use among individuals with a history of cancer in the United States. Cancer 127(18):3437–3444
Tringale KR et al (2019) The role of cancer in marijuana and prescription opioid use in the United States: a population-based analysis from 2005 to 2014. Cancer 125(13):2242–2251
Cousins MM et al (2023) Cannabis use in patients seen in an academic radiation oncology department. Pract Radiat Oncol 13(2):112–121
Anderson SP et al (2019) Impact of medical cannabis on patient-reported symptoms for patients with cancer enrolled in Minnesota’s medical cannabis program. J Oncol Pract 15(4):e338–e345
Blake EA et al (2019) Non-prescription cannabis use for symptom management amongst women with gynecologic malignancies. Gynecol Oncol Rep 30:100497
Poghosyan H et al (2021) Association between daily and non-daily cannabis use and depression among United States adult cancer survivors. Nurs Outlook 69(4):672–685
Vinette B et al (2022) Routes of administration, reasons for use, and approved indications of medical cannabis in oncology: a scoping review. BMC Cancer 22(1):319
Rosa WE et al (2020) Patient trade-offs related to analgesic use for cancer pain: a MaxDiff analysis study. Pain Manag Nurs 21(3):245–254
Wegier P et al (2020) “No thanks, I don’t want to see snakes again”: a qualitative study of pain management versus preservation of cognition in palliative care patients. BMC Palliat Care 19(1):182
Aviram J et al (2022) The effectiveness and safety of medical cannabis for treating cancer related symptoms in oncology patients. Front Pain Res (Lausanne) 3:861037
Bar-Lev Schleider L et al (2018) Prospective analysis of safety and efficacy of medical cannabis in large unselected population of patients with cancer. Eur J Intern Med 49:37–43
Swarm RA et al (2019) Adult cancer pain, Version 3.2019, NCCN Clinical Practice Guidelines in Oncology. J Natl Compr Canc Netw 17(8):977–1007
Aviram J et al (2020) Short-term medical cannabis treatment regimens produced beneficial effects among palliative cancer patients. Pharmaceuticals (Basel) 13(12)
National Conference of State Legislatures. State medical cannabis laws (2022). Available from: http://www.ncsl.org/research/health/state-medical-marijuana-laws.aspx. Accessed 25 Jan 2023
Compton WM et al (2017) Use of marijuana for medical purposes among adults in the United States. JAMA 317(2):209–211
Leung J et al (2022) Prevalence and self-reported reasons of cannabis use for medical purposes in USA and Canada. Psychopharmacology 239(5):1509–1519
Dai H, Richter KP (2019) A National Survey of Marijuana Use Among US Adults With Medical Conditions, 2016–2017. JAMA Netw Open 2(9):e1911936
Park JY, Wu LT (2017) Prevalence, reasons, perceived effects, and correlates of medical marijuana use: A review. Drug Alcohol Depend 177:1–13
Harris PA et al (2009) Research electronic data capture (REDCap)–a metadata-driven methodology and workflow process for providing translational research informatics support. J Biomed Inform 42(2):377–381
StataCorp (2017) Stata Statistical Software: Release 15. College Station, TX: StataCorp LLC
Boehnke KF et al (2022) U.S. trends in registration for medical cannabis and reasons for use from 2016 to 2020: an observational study. Ann Intern Med 175(7):945–951
Kosiba JD, Maisto SA, Ditre JW (2019) Patient-reported use of medical cannabis for pain, anxiety, and depression symptoms: systematic review and meta-analysis. Soc Sci Med 233:181–192
Walsh Z et al (2013) Cannabis for therapeutic purposes: patient characteristics, access, and reasons for use. International Journal of Drug Policy 24(6):511–516
Worster B, Hajjar ER, Handley N (2022) Cannabis use in patients with cancer: a clinical review. JCO Oncology Pract 18(11):743–749
Braun IM et al (2018) Medical oncologists’ beliefs, practices, and knowledge regarding marijuana used therapeutically: a nationally representative survey study. J Clin Oncol 36(19):1957–1962
McLennan A et al (2020) Health care provider preferences for, and barriers to, cannabis use in cancer care. Curr Oncol 27(2):e199–e205
Lapham GT et al (2022) Comparison of medical cannabis use reported on a confidential survey vs documented in the electronic health record among primary care patients. JAMA Netw Open 5(5):e2211677
National Academies of Sciences, E., and Medicine, , The health effects of cannabis and cannabinoids: current state of evidence and recommendations for research. 2017, National Academies Press (US): Washington (DC).
Abrams DI (2022) Cannabis, cannabinoids and cannabis-based medicines in cancer care. Integr Cancer Ther 21:15347354221081772
Hill KP (2020) Medical Cannabis. JAMA 323(6):580–580
Hasin DS et al (2016) Prevalence and correlates of DSM-5 cannabis use disorder, 2012–2013: findings from the national epidemiologic survey on alcohol and related conditions–III. Am J Psychiatry 173(6):588–599
Ribeiro L, Ind PW (2018) Marijuana and the lung: hysteria or cause for concern? Breathe (Sheff) 14(3):196–205
Ribeiro LI, Ind PW (2016) Effect of cannabis smoking on lung function and respiratory symptoms: a structured literature review. NPJ Prim Care Respir Med 26:16071
Velayudhan L, McGoohan KL, Bhattacharyya S (2021) Evaluation of THC-related neuropsychiatric symptoms among adults aged 50 years and older: a systematic review and metaregression analysis. JAMA Netw Open 4(2):e2035913
Hudson A, Hudson P (2021) Risk factors for cannabis-related mental health harms in older adults: a review. Clin Gerontol 44(1):3–15
Choi NG, Dinitto DM, Arndt S (2019) Potential harms of marijuana use among older adults. Public Policy & Aging Report 29(3):88–94
National Academies of Sciences Engineering and Medicine. The health effects of cannabis and cannabinoids: the current state of evidence and recommendations for research. 2017, National Academies Press: Washington (DC)
Guo Y et al (2016) Population survey features and response rates: a randomized experiment. Am J Public Health 106(8):1422–1426
Babalonis S et al (2021) Δ(8)-THC: legal status, widespread availability, and safety concerns. Cannabis Cannabinoid Res 6(5):362–365
Acknowledgements
The authors would like to thank the research staff at the Medical University of South Carolina, Addiction Sciences Division, including Benjamin Laprise, Isabeau Burnett, Kemi Chukwuka-White, Emma Mandel, Patrick Cato, and Elizabeth Bradley. We thank ICF for providing technical support to the supplement grantees, including advising on sampling plans and computing survey weights, and in collaboration with NCI, developing a core set of survey questions. Finally, we would like to thank the patients at the Hollings Cancer Center at MUSC for their participation in this survey and sharing their experiences with the research team.
Funding
This research was funded by an administrative supplement to the Hollings Cancer Center at the Medical University of South Carolina (P30 CA138313, PI Dubois, Supplement PI, McClure) from the National Cancer Institute (NCI), NIH, DHHS. Additional funding and support came from the National Center for Advancing Translational Sciences (NCATS UL1TR001450, PI Brady), NIDA K24DA038240 (McRae-Clark), K23 DA045766 (Dahne), the National Institute on Alcohol Abuse and Alcoholism (T32AA007474; PI: Woodward), and in part by the Biostatistics Shared Resource, Hollings Cancer Center, Medical University of South Carolina (P30 CA138313).
Author information
Authors and Affiliations
Contributions
EM, RT, JD, and AMC were involved in the conception and design of this study. EM and KW drafted the original manuscript. KW, RT, and EH provided statistical guidance and conducted data analyses. All authors were involved in the interpretation of results, as well as writing and editing the manuscript and all approve the final version of this manuscript.
Corresponding author
Ethics declarations
Ethical approval
All study procedures were approved by the Institutional Review Board (IRB) at the Medical University of South Carolina (MUSC). All procedures were conducted in accordance with the Declaration of Helsinki.
Competing interests
Rachel Tomko provided consultation to the American Society of Addiction Medicine. No other authors have conflicts of interest to disclose.
Conflict of interest
Rachel Tomko provided consultation to the American Society of Addiction Medicine. Other authors declare no competing interests.
Disclosures
The contents of this manuscript are the sole responsibility of the authors and do not necessarily represent the official views of the NCI.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
McClure, E.A., Walters, K.J., Tomko, R.L. et al. Cannabis use prevalence, patterns, and reasons for use among patients with cancer and survivors in a state without legal cannabis access. Support Care Cancer 31, 429 (2023). https://doi.org/10.1007/s00520-023-07881-6
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s00520-023-07881-6