Abstract
Purpose
Breast cancer-related lymphedema (BCRL) is an incurable complication occurring after breast cancer treatment. The influence of obesity/overweight on the development of BCRL at different points after surgery was seldom verified. We aimed to determine the cut-off BMI/weight value associated with an increased risk of BCRL at different postoperative time in Chinese breast cancer survivors.
Methods
Patients who underwent breast surgery plus axillary lymph node dissection (ALND) were retrospectively evaluated. Disease and treatment characteristics of participants were collected. BCRL was diagnosed by circumference measurements. Univariate and multivariable logistic regression was used to assess the relationship of lymphedema risk with BMI/weight and other disease- and treatment-related factors.
Results
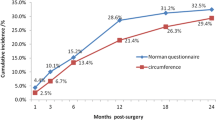
518 patients were included. Lymphedema occurred more frequently among breast cancer patients with preoperative BMI ≥ 25 kg/m2 (37.88%) than among those with preoperative BMI < 25 kg/m2(23.32%), with significant differences at 6–12 and 12–18 months after surgery (χ2 = 23.183, P = 0.000; χ2 = 5.279, P = 0.022). By multivariable logistics analysis, preoperative BMI ≥ 30 kg/m2 presented a significantly greater risk of lymphedema than a preoperative BMI < 25 kg/m2 (OR [95% CI] = 2.928 [1.565, 5.480]). Other factors, including radiation (breast/chest wall + axilla vs. none: OR [95% CI] = 3.723[2.271–6.104]), was an independent risk factor for lymphedema.
Conclusions
Preoperative obesity was an independent risk factor for BCRL in Chinese breast cancer survivors, and a preoperative BMI ≥ 25 kg/m2 indicated greater likelihood of lymphedema development within 6–18 months postoperatively.

Similar content being viewed by others
Data availability
Data are not available.
Abbreviations
- BMI:
-
Body mass index
- CI:
-
Confidence interval
- BCRL:
-
Breast cancer-related lymphedema
- ALND:
-
Axillary lymph-node dissection
- SD:
-
Standard deviation
- WHO:
-
World Health Organization
- RLND:
-
Regional lymph node irradiation
References
Taghian NR, Miller CL, Jammallo LS, Toole J, Skolny MN (2014) Lymphedema following breast cancer treatment and impact on quality of life: a review. Crit Rev Oncol Hemato 192:227–234
Dayan JH, Ly CL, Kataru RP, Mehrara BJ (2018) Lymphedema: pathogenesis and novel therapies. Annu Rev Med 69:263–276
DiSipio T, Rye S, Newman B, Hayes S (2013) Incidence of unilateral arm lymphoedema after breast cancer: a systematic review and meta-analysis. Lancet Oncol 14:500–515
Chachaj A, Małyszczak K, Pyszel K, Lukas J, Tarkowski R, Pudełko M et al (2010) Physical and psychological impairments of women with upper limb lymphedema following breast cancer treatment. Psychooncology 19:299–305
Hayes SC, Janda M, Cornish B, Battistutta D, Newman B (2008) Lymphedema after breast cancer: incidence, risk factors, and effect on upper body function. J Clin Oncol 26:3536–3542
Stolldorf DP, Dietrich MS, Ridner SH (2016) Symptom frequency, intensity, and distress in patients with lower limb lymphedema. Lymphat Res Biol 14:78–87
Vassard D, Olsen MH, Zinckernagel L, Vibe-Petersen J, Dalton SO, Johansen C (2010) Psychological consequences of lymphoedema associated with breast cancer: a prospective cohort study. Eur J Cancer 46:3211–3218
Khan F, Amatya B, Pallant JF, Rajapaksa I (2012) Factors associated with long-term functional outcomes and psychological sequelae in women after breast cancer. Breast 21:314–320
Zou L, Liu FH, Shen PP, Hu Y, Liu XQ, Xu YY et al (2018) The incidence and risk factors of related lymphedema for breast cancer survivors post-operation: a 2-year follow-up prospective cohort study. Breast Cancer 25:309–314
Shaitelman SF, Chiang YJ, Griffin KD, DeSnyder SM, Smith BD, Schaverien MV et al (2017) Radiation therapy targets and the risk of breast cancer-related lymphedema: a systematic review and network meta-analysis. Breast Cancer Res Treat 162:201–215
Ridner SH, Dietrich MS, Stewart BR, Armer JM (2011) Body mass index and breast cancer treatment-related lymphedema. Support Care Cancer 19:853–857
Helyer LK, Varnic M, Le LW, Leong W, McCready D (2010) Obesity is a risk factor for developing postoperative lymphedema in breast cancer patients. Breast J 16:48–54
Jammallo LS, Miller CL, Singer M, Horick NK, Skolny MN, Specht MC et al (2013) Impact of body mass index and weight fluctuation on lymphedema risk in patients treated for breast cancer. Breast Cancer Res Treat 142:59–67
Leray H, Malloizel-Delaunay J, Lusque A, Chantalat E, Bouglon L, Chollet C et al (2020) Body mass index as a major risk factor for severe breast cancer-related lymphedema. Lymphat Res Biol 18:510–516
Flegal KM, Kruszon-Moran D, Carroll MD, Fryar CD, Ogden CL (2016) Trends in obesity among adults in the United States, 2005 to 2014. JAMA 315:2284–2291
Ma S, Xi B, Yang L, Sun J, Zhao M, Bovet P (2021) Trends in the prevalence of overweight, obesity, and abdominal obesity among Chinese adults between 1993 and 2015. Int J Obes (Lond) 45:427–437
Ancukiewicz M, Miller CL, Skolny MN, O’Toole J, Warren LE, Jammallo LS et al (2012) Comparison of relative versus absolute arm size change as criteria for quantifying breast cancer-related lymphedema: the flaws in current studies and need for universal methodology. Breast Cancer Res Treat 135:145–152
Greene AK, Grant FD, Slavin SA (2012) Lower-extremity lymphedema and elevated body-mass index. N Engl J Med 366:2136–2137
Weitman ES, Aschen SZ, Farias-Eisner G, Albano N, Cuzzone DA, Ghanta S et al (2013) Obesity impairs lymphatic fluid transport and dendritic cell migration to lymph nodes. PLoS ONE 8:e70703
Savetsky IL, Torrisi JS, Cuzzone DA, Ghanta S, Albano NJ, Gardenier JC et al (2014) Obesity increases inflammation and impairs lymphatic function in a mouse model of lymphedema. Am J Physiol Heart Circ Physiol 307:H165–H172
Aschen S, Zampell JC, Elhadad S, Weitman E, De Brot AM, Mehrara BJ (2012) Regulation of adipogenesis by lymphatic fluid stasis: part II. Expression of adipose differentiation genes. Plast Reconstr Surg 129:838–847
Ghanta S, Cuzzone DA, Torrisi JS, Albano NJ, Joseph WJ, Savetsky IL et al (2015) Regulation of inflammation and fibrosis by macrophages in lymphedema. Am J Physiol Heart Circ Physiol 308:H1065–H1077
McLaughlin SA, Brunelle CL, Taghian A (2020) Breast cancer-related lymphedema: risk factors, screening, management, and the impact of locoregional treatment. J Clin Oncol 38:2341–2350
Ee C, Cave AE, Naidoo D, Bilinski K, Boyages J (2020) Weight before and after a diagnosis of breast cancer or ductal carcinoma in situ: a national Australian survey. BMC Cancer 20:113
Ridner SH, Dietrich MS, Cowher MS, Taback B, McLaughlin S, Ajkay N et al (2019) A randomized trial evaluating bioimpedance spectroscopy versus tape measurement for the prevention of lymphedema following treatment for breast cancer: interim analysis. Ann Surg Oncol 26:3250–3259
Roberts SA, Gillespie TC, Shui AM, Brunelle CL, Daniell KM, Locascio JJ et al (2021) Weight loss does not decrease risk of breast cancer-related arm lymphedema. Cancer 127:3939–3945
Tsai CL, Hsu C-Y, Chang WW, Lin Y-N (2020) Effects of weight reduction on the breast cancer-related lymphedema: a systematic review and meta-analysis. Breast 52:116–121
Provan D (2019) Body weight and the management of lymphoedema. Br J Community Nurs 24:576–579
Author information
Authors and Affiliations
Contributions
Shaomei Shang and Ling Wang were responsible for the study design. Ning Liu and Miao Yu performed data collection. Hongbo Chen and Yuanzhen Li performed data analysis. Ling Wang, Hongbo Chen, Yuanzhen Li, and Huixue Wang were responsible for the drafting of the manuscript. Shaomei Shang made critical revision of the manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Ethics approval
This study had appropriate ethical approval (the Peking University Research Ethics Committee, IRB00001052-21051).
Consent to participate
Written informed consent was obtained from the parents.
Consent for publication
No participants are identifiable.
Competing interests
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Wang, L., Chen, H., Li, Y. et al. Body mass index increases the risk of breast cancer-related lymphedema at 6–18 months after surgery: a retrospective study. Support Care Cancer 31, 278 (2023). https://doi.org/10.1007/s00520-023-07721-7
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s00520-023-07721-7