Abstract
Background
For the treatment of delirium, antipsychotics such as haloperidol are used as standard treatments. However, haloperidol has a little sedative effect and may not be sufficiently effective in controlling overactive delirium. Hydroxyzine, an antihistamine, may be used in combination with haloperidol to supplement its sedative effect. The aim of this study was to investigate the effect of haloperidol alone or in combination with hydroxyzine on the improvement of overactive delirium retrospectively.
Method
Delirium was assessed from medical records using the Intensive Care Delirium Screening Checklist (ICDSC). The number of patients and days with an ICDSC score of < 4, indicating an absence of delirium after haloperidol alone or haloperidol and hydroxyzine was surveyed for 6 days.
Results
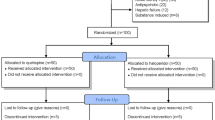
A total of 157 patients were diagnosed with delirium from April 2019 to July 2021, of which 18 patients received haloperidol alone, and 21 patients received the combination of haloperidol and hydroxyzine for overactive delirium. The number of patients with a mean ICDSC score of < 4 on days 1–6 was two patients (11%) in the haloperidol groups and two patients (10%) in the combination of haloperidol and hydroxyzine group (P = 0.999). The days within < 4 of the ICDSC score on days 1–6 were 0.8 (1.3) and 0.8 (1.5), respectively (P = 0.848).
Conclusion
Haloperidol alone and haloperidol plus hydroxyzine are both effective in the treatment of overactive delirium. However, the concomitant use of hydroxyzine with haloperidol may not improve the efficacy of treatment of overactive delirium compared to haloperidol alone.


Similar content being viewed by others
Data availability
All data generated or analyzed during this study are included in this published article.
Code availability
Not applicable.
References
American Psychiatric Association, DSM-5 Task Force (2013) Diagnostic and statistical manual of mental disorders: DSM-5™ (5th ed.). American Psychiatric Publishing, Inc. Washington, DC
Folstein MF, Bassett SS, Romanoski AJ, Nestadt G (1991) The epidemiology of delirium in the community: the Eastern Baltimore Mental Health Survey. Int Psychogeriatr 3:169–176
Dyer CB, Ashton CM, Teasdale TA (1995) Postoperative delirium. A review of 80 primary data-collection studies. Arch Intern Med 155:461–5
Lawlor PG, Gagnon B, Mancini IL, Pereira JL, Hanson J, Suarez-Almazor ME, Bruera ED (2000) Occurrence, causes, and outcome of delirium in patients with advanced cancer: a prospective study. Arch Intern Med 160:786–794
Huybrechts KF, Gerhard T, Crystal S, Olfson M, Avorn J, Levin R, Lucas JA, Schneeweiss S (2012) Differential risk of death in older residents in nursing homes prescribed specific antipsychotic drugs: population based cohort study. BMJ 344:e977. https://doi.org/10.1136/bmj.e977
Tahir TA, Eeles E, Karapareddy V, Muthuvelu P, Chapple S, Phillips B, Adyemo T, Farewell D, Bisson JI (2010) A randomized controlled trial of quetiapine versus placebo in the treatment of delirium. J Psychosom Res 69:485–490
Breitbart W, Tremblay A, Gibson C (2002) An open trial of olanzapine for the treatment of delirium in hospitalized cancer patients. Psychosomatics 43:175–182
Kishi Y, Kato M, Okuyama T, Thurber S (2012) Treatment of delirium with risperidone in cancer patients. Psychiatry Clin Neurosci 66:411–417
Burry L, Hutton B, Williamson DR, Mehta S, Adhikari NK, Cheng W, Ely EW, Egerod I, Fergusson DA, Rose L (2019) Pharmacological interventions for the treatment of delirium in critically ill adults. Cochrane Database Syst Rev 9(9):CD011749. https://doi.org/10.1002/14651858.CD011749.pub2
Bergeron N, Dubois MJ, Dumont M, Dial S, Skrobik Y (2001) Intensive Care Delirium Screening Checklist: evaluation of a new screening tool. Intensive Care Med 27:859–864
Hui D, Frisbee-Hume S, Wilson A, Dibaj SS, Nguyen T, De La Cruz M, Walker P, Zhukovsky DS, Delgado-Guay M, Vidal M, Epner D, Reddy A, Tanco K, Williams J, Hall S, Liu D, Hess K, Amin S, Breitbart W, Bruera E (2017) Effect of lorazepam with haloperidol vs haloperidol alone on agitated delirium in patients with advanced cancer receiving palliative care: A randomized clinical trial. JAMA 318:1047–1056
Matsuo N, Morita T (2007) Efficacy, safety, and cost effectiveness of intravenous midazolam and flunitrazepam for primary insomnia in terminally ill patients with cancer: a retrospective multicenter audit study. J Palliat Med 10:1054–1062
Baillargeon J, Singh G, Kuo YF, Raji MA, Westra J, Sharma G (2019) Association of opioid and benzodiazepine use with adverse respiratory events in older adults with chronic obstructive pulmonary disease. Ann Am Thorac Soc 16:1245–1251
Hui D, De La Rosa A, Wilson A, Nguyen T, Wu J, Delgado-Guay M, Azhar A, Arthur J, Epner D, Haider A, De La Cruz M, Heung Y, Tanco K, Dalal S, Reddy A, Williams J, Amin S, Armstrong TS, Breitbart W, Bruera E (2020) Neuroleptic strategies for terminal agitation in patients with cancer and delirium at an acute palliative care unit: a single-centre, double-blind, parallel-group, randomised trial. Lancet Oncol 21:989–998
Tuma R, DeAngelis LM (2000) Altered mental status in patients with cancer. Arch Neurol 57:1727–1731
Marcantonio ER, Juarez G, Goldman L, Mangione CM, Ludwig LE, Lind L, Katz N, Cook EF, Orav EJ, Lee TH (1994) The relationship of postoperative delirium with psychoactive medications. JAMA 272:1518–1522
Agostini JV, Leo-Summers LS, Inouye SK (2001) Cognitive and other adverse effects of diphenhydramine use in hospitalized older patients. Arch Intern Med 161:2091–2097
Beach SR, Gross AF, Hartney KE, Taylor JB, Rundell JR (2020) Intravenous haloperidol: a systematic review of side effects and recommendations for clinical use. Gen Hosp Psychiatry 67:42–50
Acknowledgements
We thank Yu Yamada, MD, Ph.D., Mayumi Tsukagoshi, CNS, Daiki Hasegawa, Momoka Suda, and Ayumi Ozawa for their help with data collection and expert advice on this study.
Author information
Authors and Affiliations
Contributions
Junya Sato and Rei Tanaka contributed to the conception and design of the study. Junya Sato conducted the data collection and initial analysis. Rei Tanaka participated in the additional analysis of the data and logical discussion of the results. The first draft of the manuscript was written by Junya Sato and read by Rei Tanaka, which was revised and agreed upon by both authors.
Corresponding author
Ethics declarations
Ethics approval
This study was conducted in accordance with the principles of the Declaration of Helsinki. It was approved by the Ethics Committee of the International University of Health and Welfare (Date: April 21, 2021/No. 21-B-457).
Consent to participate
Not applicable.
Consent to publish
Not applicable.
Competing interests
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Sato, J., Tanaka, R. A retrospective comparison of haloperidol and hydroxyzine combination therapy with haloperidol alone in the treatment of overactive delirium. Support Care Cancer 30, 4889–4896 (2022). https://doi.org/10.1007/s00520-022-06903-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00520-022-06903-z