Abstract
Purpose
The purpose of this systematic review is to synthesize the evidence on the types of interventions that have been utilized by Indigenous Peoples living with cancer, and report on their relevance to Indigenous communities and how they align with holistic wellness.
Methods
A systematic review with narrative synthesis was conducted.
Results
The search yielded 7995 unique records; 27 studies evaluating 20 interventions were included. The majority of studies were conducted in USA, with five in Australia and one in Peru. Study designs were cross-sectional (n=13); qualitative (n=5); mixed methods (n=4); experimental (n=3); and quasi-experimental (n=2). Relevance to participating Indigenous communities was rated moderate to low. Interventions were diverse in aims, ingredients, and outcomes. Aims involved (1) supporting the healthcare journey, (2) increasing knowledge, (3) providing psychosocial support, and (4) promoting dialogue about cancer. The main ingredients of the interventions were community meetings, patient navigation, arts, and printed/online/audio materials. Participants were predominately female. Eighty-nine percent of studies showed positive influences on the outcomes evaluated. No studies addressed all four dimensions of holistic wellness (physical, mental, social, and spiritual) that are central to Indigenous health in many communities.
Conclusion
Studies we found represented a small number of Indigenous Nations and Peoples and did not meet relevance standards in their reporting of engagement with Indigenous communities. To improve the cancer survivorship journey, we need interventions that are relevant, culturally safe and effective, and honoring the diverse conceptualizations of health and wellness among Indigenous Peoples around the world.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Worldwide, Indigenous PeoplesFootnote 1 have a higher cancer burden than non-Indigenous counterparts [1,2,3,4,5,6,7,8]. One report indicated that cancer incidence and mortality rates were higher in First Nations people in Canada for lung, colorectal, and kidney cancers as compared to non-First Nations people [2], while a comparison of 5-year survival and mortality rates for 15 cancers in a cohort population across Canada found that First Nations adults had poorer survival from all cancers except multiple myeloma, reaching over 20% lower for cervical and ovarian cancers and 10–15% lower for colorectal, breast, non-Hodgkin lymphoma, and leukemia [9]. In the province of Manitoba, First Nations people diagnosed with cancer were significantly younger with significantly higher mortality rates, despite similar incidence rates after adjusting for age, sex, income, and area of residence [8]. The underlying causes of these disparities are wide ranging and complex, and include lower rates of screening and late-stage diagnoses [10, 11]. However, more pervasive reasons stem from colonial legacies that have created poverty, social exclusion, and systemic racism in mainstream healthcare [1, 2, 11,12,13,14].
The unique cancer burdens faced by Indigenous Peoples have largely been attributed to the impacts of colonization and the subsequent lack of culturally safe healthcare services and supports [1, 2, 12, 13]. Historical trauma has profoundly impacted Indigenous peoples’ trust and engagement in Western healthcare systems [1, 15, 16]. Approaches to survivorship that are tailored to specific needs of survivors have been shown to decrease cancer burden, increase survival rates, and enhance well-being [1, 17]. Despite potential benefits, Indigenous Peoples do not typically seek survivorship supports and Indigenous values, practices, and distinct needs are not typically reflected in mainstream health care or cancer survivorship interventions [1, 15, 17,19,20]. While the term “cancer survivorship” can vary, we recognize it as living with, through, and beyond a diagnosis of cancer [21]. Many Indigenous people have described feeling unsafe and fearing stigmatization with cancer survivorship interventions [17]. In voicing their survivorship experiences, Indigenous people have described a failure of healthcare services to accommodate their distinct ethnic, cultural, and socio-historical needs [17, 18].
What might culturally safe cancer survivorship programs and supports look like for Indigenous Peoples? The Health Council of Canada recommends the provision of culturally safe care that respects traditional, holistic approaches to wellness and healing [18]. The incorporation of traditional, holistic approaches that include spirituality, traditions, and family has been found to be important to Indigenous cancer survivors [17, 22, 23]. Indigenous people are in the best position to guide their path to health and wellness [24], and strengths-based, community engaged, decolonizing approaches that recognize and honor Indigenous knowledge are needed [25].
Grounding cancer survivorship interventions within an understanding of Indigenous wellness is also important [2]. Indigenous health and wellness are often understood to be a balance of one’s physical, spiritual, emotional, and mental being. While this may be expressed differently in different Indigenous nations, it is closely tied to the four dimensions of the Medicine Wheel for First Nations Peoples in North America [26, 27].
Setting a course to move cancer survivorship programs forward calls for a comprehensive exploration of past initiatives. Cancer survivorship interventions that have been used by Indigenous Peoples have not been systematically described, particularly their relevance to Indigenous communities and Indigenous wellness. As part of a larger study to improve healthcare deliver with Indigenous Peoples in Canada [28], the purpose of this systematic review was to synthesize the research evidence on cancer survivorship strategies that have been used by Indigenous Peoples. The research objectives are to:
-
1)
Identify methodological approaches that have been used in cancer survivorship research,
-
2)
Describe components of cancer survivorship interventions and the reported evidence on their relevance to Indigenous communities,
-
3)
Examine outcomes of the interventions and their positioning to holistic wellness.
Methods
We considered quantitative and qualitative evidence following a multi-stage methodological approach that involved searching the literature, screening articles for inclusion and exclusion criteria, extracting data, assessing articles for methodological quality and relevance to Indigenous communities, and synthesizing study findings to produce a narrative summary of results [29].
Search strategy
We created the search strategy with a health sciences librarian. Seven electronic databases were searched from their date of inception to March 6, 2018, and then were updated on August 20, 2020: Medline (Ovid), Embase (Ovid), Cochrane’s Central Registry for Randomized Controlled Trials - CENTRAL (Ovid), PsycINFO (Ovid), CINAHL (EBSCOHost), and PubMed. No modifications were made to the search strategy during the update. We included keywords and subject heading applicable to each database for concepts related to Indigenous Populations, cancer survivorship, and interventions (See Additional files 1 and 2). Supplemental searching involved examining reference list of eligible articles and systematic reviews identified in the search.
Types of studies
We included articles with quantitative, qualitative; and mixed-methods designs. To be included, studies had to (1) involve Indigenous cancer survivors or caregivers, (2) execute a psychosocial cancer survivorship intervention, (3) report on patient outcomes qualitatively and/or quantitatively, and (4) collect primary data. There were no language exclusion criteria, and no restrictions on publication date.
Systematic reviews, commentaries, editorials, and theses were excluded. Studies were also excluded if the interventions involved treatments such as pharmacological, surgical, radiation, biological, or stem cells as this review was concerned with survivorship supports and not treatments. Interventions that focused on pre-diagnosis screening were also excluded.
Selection of studies
All titles and abstracts identified in the database search were independently screened for eligibility in Covidence systematic review software [30] by four reviewers. Full copies of articles identified as potentially eligible, or with insufficient information to decide, were retrieved and independently assessed for inclusion criteria by two reviewers. Disagreements were resolved through discussions and adjudication with the lead author (WG).
Data extraction
We designed a data extraction form based on the review objectives and iteratively refined it after pilot testing with two articles from each study design (n=6) to ensure the data extracted reflected the aims of the review. One reviewer extracted data from all included articles into an Excel spreadsheet and two reviewers verified it for accuracy. Data were extracted on study characteristics, including outcomes and impacts, and any information about collaborating with Indigenous communities to conduct the study. Details about each intervention were extracted into categories of the AIMD framework that describe (1) Aims (what the intervention is intended to achieve and for whom); (2) Ingredients (what comprises the intervention); (3) Mechanisms (how the intervention is proposed to work); and (4) Delivery (how the intervention was delivered) [31]. The AIMD framework was developed to enhance understandings of how interventions work to inform healthcare practices and policies [31].
Assessment of relevance to Indigenous communities
Two reviewers (SM, LW) independently assessed each study’s relevance to Indigenous communities and methodological quality. Discrepancies were resolved and assessments confirmed through discussions and adjudication with two authors (WG, MR) who provided the final assessment ratings. We used a tool inspired by Smylie et al. to assess the evidence of the interventions’ relevancy to participating Indigenous communities and members [32, 33]. The assessment examined whether there was evidence in the published papers of Indigenous participants’ engagement in the research through four categories of relevance: (1) alignment of study designs and measures to the community/participants’ values, beliefs, and knowledge systems; (2) alignment to local priorities; (3) relevance of underlying intervention to participating communities/participants; and (4) whether the study protocol was vetted by local community members [32, 33]. We measured evidence of relevance on a zero-to-eight scale by summing scores of community participation in any stage of the study, including development and implementation. Each of the four categories was scored as follows: 0=not reported, 1=partial evidence; 2=explicit evidence. A composite score was created for each intervention by totalling the four subcomponent scores where 0=none, 1–3=weak, 4–6=moderate, and 7–8=strong evidence of the interventions relevance to participating communities.
Assessment of methodological quality
We used three tools to assess methodological quality of included studies according to study design: (1) McMaster Critical Review tools for quantitative research [34]; (2) McMaster Critical Review tools for qualitative research [35]; and (3) Mixed Methods Appraisal tool (MMAT) for mixed-methods studies [36, 37]. We adapted a scoring system based on previously published systematic reviews [38, 39]. We divided the number obtained in the quality rating for each study by the total number of possible points, to obtain a total quality rating between 0 and 1. Studies were then categorized as weak (0–.25), weak-moderate (.26–.50), moderate (.51–.75), or strong (.76–1.0).
We conducted methodological quality and relevance assessments for each study that evaluated an intervention and aggregated data (when required) for all studies that evaluated the same intervention. For example, if one intervention was evaluated in three studies, we assessed the methodological quality and relevence to Indigenous communities or participants from the pooled data of all the studies that evaluated the same intervention. (See Table 1 for a summary of tools).
Data synthesis
We conducted a narrative synthesis [40] to produce a summary of studies. We tabulated characteristics of included studies in Excel and descriptively synthesized data on interventions and outcomes. To synthesize components of the interventions, we systematically coded data into the following categories based on the AIMD framework: Aims, Target Group, Ingredients, and Delivery. We then developed themes for each of the categories as they emerged from the studies. Themes were based on the primary author’s descriptions whenever possible. For example, when an author reported that the purpose of the intervention was to “better support Indigenous Australians through their cancer journey,” we identified the theme as “support and improve the healthcare journey.”
As methodologies, interventions, and outcomes were vastly heterogeneous, we categorized outcomes into descriptive themes as they related to the outcomes that were evaluated. Indigenous team members (ND, MB) brought an Indigenous perspective to the thematic analysis of outcomes. We first categorized outcomes as follows: (1) holistic wellness outcomes and (2) responses towards the intervention. Holistic wellness outcomes corresponded to conceptualizations of Indigenous wellness and encompassed findings related to physical, mental, emotional, or spiritual health. The physical domain involves taking care of one’s body; the mental involves rational thought; the emotional encompasses relationships and being connected to family and community; and the spiritual involves beliefs, values, and identity [26, 27, 41]. Responses towards the intervention encompassed aspects of the interventions that could influence wellness, such as perceptions of cultural safety, cultural appropriateness, acceptability, or satisfaction. We then inductively created subcategories for each outcome category as they emerged from the data, using an iterative and consultative process among the research team that involved data display, re-categorization, and confirmation.
Results
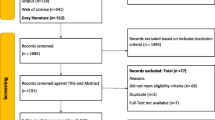
The search yielded 7995 unique records after duplicate removal, with 257 identified as potentially relevant. Twenty-seven studies evaluating 20 interventions met the inclusion criteria and were included in this review. Of the potentially relevant articles that were not included, the top reasons were not empirical involving primary data (n=76, 33%), no intervention (n=66, 28%), or not about cancer (n=24, 10%) (Fig. 1 PRISMA diagram).
Characteristics of included studies
Twenty interventions were evaluated in 27 studies. Characteristics of included studies are described in Table 2. Four interventions were evaluated in multiple studies, i.e., (1) Native Navigators and Cancer Continuum (NNACC) program [42,43,44]; (2) Walking Forward program [45,46,47,48]; (3) Family ‘ohana intervention [23, 49], and (4) Aboriginal women’s cancer support network [50, 51]. The remainder of the interventions were evaluated in a single study. Sixty-seven percent of the studies were quantitative (n=18) [23, 42,43,44,45,46,47,48,49, 52,53,54,55,56,57,58], 19% qualitative (n=5) [50, 51, 59, 60], and 15% mixed methods (n=4) [61,62,63,64].
Of the 18 quantitative studies, three (n=17%) used an experimental design (RCTs) [23, 49, 56] and the remainder used quasi-experimental or non-experimental designs. All quantitative studies used surveys for data collection except for two [45, 53], which used medical records and/or electronic databases. Data in the mixed-methods studies (n=4) involved surveys, interviews, or discussion groups, while the qualitative studies (n=5) employed interviews, focus groups, and journaling.
Twenty-one (77%) of the included studies were conducted in the USA, with five from Australia (18%), and one from Peru (4%). Studies had diverse healthcare settings, the majority set in the community (n=21, 77%), four in hospitals, and two in medical clinics.
The total number of participants in each study ranged from 8 to 900. Participants’ Indigenous ethnicity included Native American (n=13; 50%), Alaskan Native (n=3; 12%), a combination of Native American and Alaskan Native (n=2; 8%), Native Hawaiian (n=2; 8%), Australian Aboriginal (n=5; 19%), Peruvian (n=1; 4%), and not specified (n=1, 4%). Twenty-six percent of studies (n=7) included family members or caregivers. Only one study reported the majority of participants as male [46], and four studies (15%) did not report the sex of participants [44, 47, 48, 63]. The earliest study was published in 1999 [63] with 81% published over the last 10 years (n=22).
Relevance to communities
Ratings of relevance to participating Indigenous communities were as follows: eight studies rated as weak [51, 52, 57, 58, 62, 64,65,66], 18 studies as moderate [23, 42,43,44,45,46,47,48,49, 54,55,56, 59,60,61, 63, 67, 68], and one study provided no evidence of relevance [53]. Overall, ratings were highest for studies keeping with local community beliefs, values, and local priorities as evident by community members’ participation in designing, tailoring, or delivering the interventions and collecting study data. Having study protocols vetted by community members was the least reported relevance criterion.
Methodological quality assessment
Quality assessments for the three experimental studies were moderate [23, 49] and weak-moderate [69]; quasi-experimental studies were weak-moderate [55, 58]; and non-experimental studies were moderate (n=5) [45,46,47,48, 57], weak-moderate (n=6) [42, 43, 54, 65, 68, 70], and weak (n=2) [52, 53]. For qualitative studies (n=5), three rated strong [51, 60, 66], one moderate [67], and one weak-moderate [59]. Of the mixed-methods studies (n=4), two rated moderate [61, 63] and two rated weak-moderate [62, 64]. Discrepancies in methodological quality assessment varied according to study design, with issues in quantitative studies predominately related to the validity and reliability of data collection tools, intervention integrity, numbers and reasons for dropouts or withdrawals, and confounding differences between groups. In the qualitative studies, quality assessment concerns involved inadequate reporting of theoretical perspectives, role of researchers, and relationship with participants. Clarity on how qualitative and quantitative aspects were integrated in mixed-methods studies had the weakest ratings (see Table 2).
Interventions
The interventions were diverse in aims, ingredients, and outcomes studies. The overarching aims of the interventions were (1) to support and improve the healthcare journey (n=19 studies); (2) increase knowledge (n=8 studies); (3) provide psychosocial support (n=6 studies); and (4) promote dialogue about cancer (n=2 studies). All interventions targeted Indigenous cancer survivors and/or community members, with 10 studies (37%) also targeting healthcare providers (see Table 3).
Ingredients of the interventions
We identified seven different ingredients of the interventions: community meetings (n=8 studies) [23, 42,43,44, 47, 49, 54, 66]; patient navigation (n=8 studies) [45,46,47,48, 52, 56, 65, 67]; visual and performing arts (n=7 studies) [55, 58,59,60,61,62, 64]; printed, online, or audio materials (n=7 studies) [23, 49, 55, 56, 60, 63, 68]; healthcare provider education (n=4 studies) [42, 44, 63, 68]; support groups (n=4 studies) [50, 51, 57, 67]; and telehealth (n=3 studies) [52, 53, 57]. Studies used one or two of the ingredients with just over half (n=14) using two ingredients. For example, Burhansstipanov et al. held community meetings and healthcare provider education [42], whereas Hodge et al. used visual art and printed materials [55, 60]. Visual arts included videos [55, 58, 60] and performing arts involved Readers Theatre where cancer survivors read out loud plays that were scripted with cancer stories [59, 62]. Healthcare provider education involved didactic and interactive face-to-face seminars, practice, and online webinars [42, 44, 63, 68].
Study outcomes
Overall, 89% (n=24) of studies showed positive influences of the interventions on outcomes. For example Dignan et al. reported that the proportion of Indigenous women that had a mammogram for breast cancer screening was significantly higher in the intervention group of a randomized control trial in the USA [56]. Results of the pre/post-survey studies that evaluated the Native Navigators and the Cancer Continuum (NNACC) [42,43,44] intervention reported increases in cancer screening, appointments, referrals rates, and knowledge about cancer and cancer care. Two studies reported no impact from the intervention [61, 65], and one study reported negative findings in the form of unresolved tensions between Western and Indigenous people in delivering of the intervention [50].
Twenty-two (81%) studies evaluated outcomes that aligned holistic wellness (physical, mental, emotional, and spiritual), and 12 studies (44%) evaluated outcomes related to responses towards the intervention. Both holistic wellness and responses towards the intervention were evaluated in seven studies [42, 44, 49, 60, 63, 64, 67], but only five studies evaluated responses towards the intervention [50, 52, 57, 61, 68]. (See Table 4 for the intervention ingredients with study outcomes and Table 5 for descriptions of outcomes).
Holistic wellness outcomes
The majority of holistic wellness outcomes that were evaluated related to physical aspects of wellness (n=14; 64%) [23, 42, 43, 45,46,47,48, 51, 53, 55, 64, 65, 67, 69], such as access to healthcare services, self-management of pain, or breast self-exams. Nine studies evaluated outcomes aligned with emotional wellness, such as self-efficacy and coping [23, 49], emotional and social support [23, 49, 67], calmness [58], anxiety [64], stress [61], and comfort speaking about cancer [59, 62]. Eight studies (38%) evaluated mental wellness that involved knowledge [42, 44, 47, 54, 59, 62,63,64] or intention [54, 62]. Two studies evaluated spiritual wellness and showed a positive impact [23, 49].
No studies evaluated all four dimensions of holistic wellness, though three studies [23, 49, 64] evaluated three dimensions of wellness. For example, Mokuau et al. evaluated physical, emotional, and spiritual outcomes with Native Hawaiian women [23, 49] and Sanderson et al. evaluated physical, mental, and emotional outcomes with Navajo women [64]. Half the studies (n=12) assessed only one dimension of wellness [43,44,45,46, 48, 53,54,55,56, 58, 63,64,65], whereas six studies [42, 47, 51, 59, 62, 67] measured two aspects of wellness.
Responses towards the intervention that influence wellness
Of the 12 studies that evaluated a response towards the intervention, only one reported a negative response [50]. Participants in Cuesta-Briand et al.’s qualitative study in Australia identified unresolved tensions between Indigenous and non-Indigenous people around the structure and delivery of the intervention, which threatened the intervention’s success and sustainability [50]. Positive responses towards the interventions included patient satisfaction, perceptions of cultural safety, appropriateness, usefulness, and acceptability of the interventions [42, 44, 52, 57, 60]. For example, Burhansstipanov [42] reported workshop content was perceived as useful by 90% of participants and Pruthi [52] identified patient satisfaction as good or excellent by 98% of participants.
Aspects of cultural relevance or safety were explicitly reported in six studies [49, 61, 63, 64, 66, 68]. Participants in the study by Bierbaum et al. [68] considered intervention resources to be culturally appropriate and acceptable and Mokuau et al.’s [49] participants appreciated cultural tailoring of materials. Although participants in the pilot study by Warson et al. [61] described the intervention positively, the survey used for data collection was considered culturally biased and therefore inconclusive.
Discussion
The purpose of this systematic review was to synthesize the published research evidence on cancer survivorship interventions that have been conducted with Indigenous Peoples. In total, we found 20 different interventions that were evaluated in 27 published studies. The majority of studies (89%) showed a positive impact on the outcomes evaluated. Most (81%) were published in the last 10 years with the majority (77%) in the USA. Participants represented a diversity of Indigenous Peoples and were predominately female. Doorenbos et al. [57] suggest that the lack of male participation in cancer survivorship interventions may be related to cultural differences in self-expression or discomfort in mixed-gender groups. Given that males may experience survivorship differently, and that sex and gender have historically been foundational to roles, traditions, and ceremonies for many Indigenous Peoples, further understandings of sex and gender conceptualizations and expressions is warranted in designing and delivering cancer survivorship interventions. We recommend further research to understand sex and gender conceptualizations and expressions in designing and delivering cancer survivorship interventions for Indigenous Peoples.
Relevance of the interventions to Indigenous communities
Studies in this review did not provide strong evidence that the interventions had relevance to the Indigenous communities that participated in them, with just over half (60%) rating as moderately relevant, and one study [53] proving no evidence of community relevance. Ratings of relevance were based on the published papers providing sufficient details that the study was developed collaboratively with Indigenous communities. However, it is unclear whether authors had been engaged but failed to report their engagement in sufficient details to warrant high ratings. Smylie et al. 2016 [33] noted similar limitations on the role of Indigenous community’s participation in prenatal and infant-toddler programs, noting that community investment, cultural integrity, and relevance were unclear because of inadequate reporting of details and context. From a social justice standpoint, Indigenous research requires methodologies that engage with communities and give back in ways that community members decide what is “useful” and relevant [71]. We support recommendations from Indigenous scholars that reporting how Indigenous communities and/or participants are involved in a study and the relevance to communities be a priority in publishing [32, 33]. As of December 2020, the Canadian Journal of Public Health requires authors to clearly describe how Indigenous Peoples were engaged in a study to be considered for publication, becoming the first scientific journal known in Canada to adopt such a policy [72].
The studies that evaluated the Walking Forward - To’katakiya zanniyan omani pi ye/yo intervention [45,46,47,48] offered ways of achieving community relevance by describing their engagement methods with participating Hawaiian communities. These included participation in the planning process, implementation, consultations, and shared responsibilities for data analyses, writing, and dissemination of findings. Similar methods and strategies were described in a “Two-Eyed Seeing” approach by Rowan et al. [41] of cultural interventions to treat addictions with Indigenous populations. Developing Indigenous health research requires Western researchers to create shared spaces that legitimize Indigenous knowledge, acknowledge the tainted history of research with Indigenous Peoples, and recognize the inherent rights of Indigenous Peoples to self-determine knowledge for understanding the world [71].
Researchers wanting to be engaged in ethical research with Indigenous communities can look for guidance in policies and principles that have been established. For example, in Canada, the Tri-Council policy statement Research Involving the First Nations, Inuit, and Metis People of Canada emphasizes traditional cultural values, community engagement, and mutually respectful relationships. The Public Health Agency of Canada further suggests the following for developing interventions with Indigenous communities: (1) be based in community, (2) use a holistic approach, (3) integrate Indigenous cultural knowledge, (4) build on community strengths and needs, (5) develop partnerships/collaboration, and (6) demonstrate effectiveness [73]. These strategies are consistent with the community relevance assessments we used in this review and in studies by Minichiello et al. [32] and Smylie et al. [33]. Establishing an equitable research environment is necessary to guide meaningful cancer survivorship research with Indigenous communities.
Methodological approaches
Studies in this review commonly used quasi-experimental designs and many involved data collection methods, such as surveys, that do not typically represent Indigenous epistemologies or approaches to knowledge development [71]. Warson reported that American Indian and Alaska Native participants of an art intervention responded positively to the intervention but were not receptive to completing the validated survey as it was culturally biased [61]. Valuable insights can be gleaned from understanding the inherent tensions between Western science and Indigenous approaches to knowledge development [71]. Many Western approaches uphold neutrality, objectivity, and universal laws of generalizability, concepts that may philosophically conflict with Indigenous research paradigms. These conflicts were underscored in the study by Cuesta-Briand et al., who reported opposing perspectives on the structure and delivery of the intervention as central to the tensions between Indigenous and Western researchers and participants [66].
Studies in this review used a variety of data collection methods that are consistent with Indigenous approaches to knowledge sharing, such as interviews [51, 59, 63, 64, 66, 67], discussion groups [60, 62, 63], and art [61]. However, theoretical perspectives that give ownership to Indigenous communities and do not separate the research from their ways of knowing were not explicit. Instead, studies predominately described Western research methodologies. Kovach explains that researchers wishing to use Indigenous methodologies alongside Western approaches should transparently indicate this, highlight differences, and not assume that Indigenous methodologies can be subsumed under Western ways of knowing [71].
Outcomes and positioning to holistic wellness
While the inclusion of body, mind, emotions, and spirit is widely recognized as integral to wellness among Indigenous Peoples [24, 74], studies in this review were predominately focused on the physical aspect of wellness, which is more consistent with Western biomedical healthcare perspectives. Frameworks such as the First Nations Mental Wellness Continuum [26] and Wellbeing Framework for Australian Aboriginal and Torres Strait Islander Peoples [75] offer conceptualizations of Indigenous wellness that can guide meaningful measurement approaches and outcomes. Indigenous-led research and decolonizing approaches that include Elders, healers, Knowledge Keepers, and community members will help to regain access to knowledge for holistic health and healing [71, 74].
Responses about the intervention
Despite relatively low ratings for relevance to Indigenous communities, participants predominately described the interventions as acceptable and culturally sensitive. These findings indicate that the interventions themselves were well-received, with many participants stating they would recommend the interventions to other community members. We summarized responses to the interventions as impacting wellness through participants’ engagement with the interventions. For example, although the survey in Warson’s study was determined to be culturally biased, the art intervention focused on a native concept of wellness and was positively received [61], while Sanderson et al. reported Navajo women found the video intervention to be culturally specific and positive [64]. These findings illustrate the importance of engaging with Indigenous communities to develop, deliver, and evaluate cancer survivorship interventions. Figure 2 graphically summarizes the holistic wellness outcomes and response to the intervention identified in the literature.
Strengths and limitations of the review
As a team of Western researchers and Indigenous community members, we followed a systematic and rigorous process with regular community meetings to conduct this review and we privileged Indigenous knowledge in the analysis and interpretations of findings. Limitations, however, must be acknowledged. While reference lists of included studies were examined for further studies, we did not search gray literature, so findings were restricted to scholarly journals. We did not contact primary authors to clarify study relevance to Indigenous communities, and therefore our ratings may be low due to underreporting in the published articles. Lastly, we did not exclude studies based on methodological weaknesses or ratings of indigenous relevance, nor did we analyze data for different Indigenous groups. Rather, we synthesized all studies together to provide a summary of the research to date.
Conclusions
Indigenous Peoples have shown resilience in their adaptations to the traumas of colonization that have contributed to lack of culturally safe cancer survivorship care. We found few studies, and the studies we found only represented a small number of Indigenous Peoples. Methodological quality in these studies was generally low, based on Western standards, and more importantly, they did not meet relevancy standards in reporting of engagement with communities. To improve the cancer survivorship journey for Indigenous people, we need research that is relevant to Indigenous communities, culturally safe and effective, and honoring the diverse conceptualizations of health and wellness among Indigenous Peoples.
Data Availability
Additional File 1: Search strategy; Additional File 2: Search Filters
Notes
Consistent with international health research environments, the term “Indigenous” is used throughout this paper to denote the original habitant of a country regardless of its borders. We refer to specific Indigenous Peoples when identifiable, and use the term Indigenous when a group is not identifiable or when referring to literature about the original inhabitants of a country.
References
Canadian Partnership Against Cancer (2013) First Nations cancer control in Canada baseline report. Canadian Partnership Against Cancer, Toronto, p 62
Chiefs of Ontario, Cancer care Ontario, and Institute for Clinical Evaluative Sciences (2017) Cancer in First Nations People in Ontario: incidence, mortality, survival and prevalence. Toronto, ON. https://www.cancercareontario.ca/sites/ccocancercare/files/assets/CancerInFirstNationsPeopleInOntario.pdf
White MC, Espey DK, Swan J, Wiggins CL, Eheman C, Kaur JS (2014) Disparities in cancer mortality and incidence among American Indians and Alaska natives in the United States. Am J Public Health 104(Suppl 3):S377–S387
Australian Institute of Health and Welfare (2018) Cancer in Aboriginal & Torres Strait Islander people of Australia Canberra. https://www.aihw.gov.au/reports/cancer/cancer-in-indigenous-australians/contents/table-of-contents
Gurney JK, Campbell S, Turner S, Scott N (2020) Addressing cancer inequities for indigenous populations: The New Zealand story. J Cancer Policy 23:100209
McGahan CE, Linn K, Guno P, Johnson H, Coldman AJ, Spinelli JJ, Caron NR (2017) Cancer in First Nations people living in British Columbia, Canada: an analysis of incidence and survival from 1993 to 2010. Cancer Causes Control 28(10):1105–1116
Decker KM, Kliewer EV, Demers AA, Fradette K, Biswanger N, Musto G, Elias B, Turner D (2016) Cancer incidence, mortality, and stage at diagnosis in First Nations living in Manitoba. Curr Oncol 23(4):225–232
Horrill TC, Dahl L, Sanderson E, Munro G, Garson C, Taylor C, Fransoo R, Thompson G, Cook C, Linton J, Schultz ASH (2019) Comparing cancer incidence, stage at diagnosis and outcomes of First Nations and all other Manitobans: a retrospective analysis. BMC Cancer 19(1):1055
Withrow DR, Pole JD, Nishri ED, Tjepkema M, Marrett LD (2017) Cancer survival disparities between First Nation and non-Aboriginal adults in Canada: follow-up of the 1991 Census Mortality Cohort. Cancer Epidemiol Biomark Prev 26(1):145–151
Kewayosh A et al (2015) Improving health equity for First Nations, Inuit and Metis people: Ontario's Aboriginal Cancer Strategy II. Healthcare Quarterly 17 Spec No:33–40
Marrett LD, Chaudhry M (2003) Cancer incidence and mortality in Ontario First Nations, 1968-1991 (Canada). Cancer Causes Control 14(3):259–268
Anderson I, Robson B, Connolly M, al-Yaman F, Bjertness E, King A, Tynan M, Madden R, Bang A, Coimbra CEA Jr, Pesantes MA, Amigo H, Andronov S, Armien B, Obando DA, Axelsson P, Bhatti ZS, Bhutta ZA, Bjerregaard P, Bjertness MB, Briceno-Leon R, Broderstad AR, Bustos P, Chongsuvivatwong V, Chu J, Deji, Gouda J, Harikumar R, Htay TT, Htet AS, Izugbara C, Kamaka M, King M, Kodavanti MR, Lara M, Laxmaiah A, Lema C, Taborda AML, Liabsuetrakul T, Lobanov A, Melhus M, Meshram I, Miranda JJ, Mu TT, Nagalla B, Nimmathota A, Popov AI, Poveda AMP, Ram F, Reich H, Santos RV, Sein AA, Shekhar C, Sherpa LY, Skold P, Tano S, Tanywe A, Ugwu C, Ugwu F, Vapattanawong P, Wan X, Welch JR, Yang G, Yang Z, Yap L (2016) Indigenous and tribal peoples' health (The Lancet-Lowitja Institute Global Collaboration): a population study. Lancet 388(10040):131–157
Tjepkema M, Wilkins R (2011) Remaining life expectancy at age 25 and probability of survival to age 75, by socio-economic status and Aboriginal ancestry. Health Rep 22(4):31–36
Inuit T, Cancer Care Ontario (2017) Cancer risk factors and screening among Inuit in Ontario and other Canadian regions. Toronto, ON. http://tungasuvvingatinuit.ca/wp-content/uploads/2019/06/Inuit-Cancer-Risk-Factors-Report.pdf
Hammond C, Thomas R, Gifford W, Poudrier J, Hamilton R, Brooks C, Morrison T, Scott T, Warner D (2017) Cycles of silence: First Nations women overcoming social and historical barriers in supportive cancer care. Psycho-Oncology 26(2):191–198
Poudrier J, Thomas-MacLean R (2009) "We’ve fallen into the cracks": a photovoice project with Aboriginal breast cancer survivors. Nurs Inq 16(4):11
Cavanagh BM, Wakefield CE, McLoone JK, Garvey G, Cohn RJ (2016) Cancer survivorship services for indigenous peoples: where we stand, where to improve? A systematic review. J Cancer Survivorship: Res Pract 10(2):330–341
Health Council of Canada (2012) Empathy, dignity and respect. Creating cultural safety for Aboriginal people in urban health care. Toronto, ON. https://healthcouncilcanada.ca/files/Aboriginal_Report_EN_web_final.pdf
Poudrier J, Mac-Lean RT (2009) ‘We've fallen into the cracks’: Aboriginal women's experiences with breast cancer through photovoice. Nurs Inq 16(4):306–317
Thomas R, Gifford W, Poudrier J, Hamilton R, Brooks C, Scott T, Morrison T, Warner D, Hammond C (2015) First Nations, Inuit, and Métis women's experiences of cancer survivorship: protocol for the National Picture Project. Int J Qual Methods 14(1):97–120
Clark EJ et al (1996) Imperatives for quality cancer care: access, advocacy, action, and accountability. National Coalition for Cancer Survivorship (NCCS), Silver Spring
Cheifetz O, Park Dorsay J, Hladysh G, MacDermid J, Serediuk F, Woodhouse LJ (2014) CanWell: meeting the psychosocial and exercise needs of cancer survivors by translating evidence into practice. Psycho-Oncology 23(2):204–215
Mokuau N, Braun KL, Daniggelis E (2012) Building family capacity for Native Hawaiian women with breast cancer. Health Soc Work 37(4):216–224
King M (2011) Scaling up the knowledge to achieve Aboriginal wellness. Can J Psychiatry 56(2):73–74
Hyett S, Marjerrison S, Gabel C (2018) Improving health research among Indigenous Peoples in Canada. CMAJ: Canadian Medical Association Journal 190(20):E616–E621
Health Canada (2015) First Nations mental wellness continuum framework. Ottawa, ON
Fiedeldey-Van Dijk C et al (2017) Honoring Indigenous culture-as-intervention: development and validity of the Native Wellness Assessment. J Ethn Subst Abus 16(2):181–218
Gifford W, Thomas R, Barton G, Graham ID (2019) Providing culturally safe cancer survivorship care with Indigenous communities: study protocol for an integrated knowledge translation study. Pilot Feasib Stud 5(1):33
Grimshaw J (2010) A guide to knowledge synthesis: a knowledge synthesis chapter., in Knowledge Translation. Canadian Institutes of Health Research: Ottawa, ON
Veritas Health Innovation (2020) Covidence systematic review software. Melbourne, Australia. www.covidence.org
Bragge P et al (2017) AIMD - a validated, simplified framework of interventions to promote and integrate evidence into health practices, systems, and policies. BMC Med Res Methodol 17(1):38
Minichiello A et al (2016) Effective strategies to reduce commercial tobacco use in Indigenous communities globally: a systematic review. BMC Public Health 16:21
Smylie J, Kirst M, McShane K, Firestone M, Wolfe S, O'Campo P (2016) Understanding the role of Indigenous community participation in Indigenous prenatal and infant-toddler health promotion programs in Canada: a realist review. Soc Sci Med 150:128–143
Westmorland M, et al. (1998) Critical review form quantitative studies. McMaster University
Letts L, et al. (2007) Critical Review Form Qualitative Studies (Version 2.0). McMaster University
Pace R, Pluye P, Bartlett G, Macaulay AC, Salsberg J, Jagosh J, Seller R (2012) Testing the reliability and efficiency of the pilot Mixed Methods Appraisal Tool (MMAT) for systematic mixed studies review. Int J Nurs Stud 49(1):47–53
Hong Qp P, et al. Mixed Methods Appraisal Tool (MMAT), Version 2018. 2018. McGill University
Gifford WA, Squires JE, Angus DE, Ashley LA, Brosseau L, Craik JM, Domecq MC, Egan M, Holyoke P, Juergensen L, Wallin L, Wazni L, Graham ID (2018) Managerial leadership for research use in nursing and allied health care professions: a systematic review. Implement Sci 13(1):127
Squires JE, Estabrooks CA, Gustavsson P, Wallin L (2011) Individual determinants of research utilization by nurses: a systematic review update. Implement Sci 6:1
Popay J et al (2005) Guidance on the conduct of narrative synthesis in systematic reviews: a product from the ESRC Methods Programme. Lancaster University, Lancaster
Rowan M et al (2014) Cultural interventions to treat addictions in Indigenous populations: findings from a scoping study. Substance Abuse Treatment Prevent Pol 9(1):34
Burhansstipanov L, Krebs LU, Dignan MB, Jones K, Harjo LD, Watanabe-Galloway S, Petereit DG, Pingatore NL, Isham D (2014) Findings from the Native Navigators and the Cancer Continuum (NNACC) Study. J Cancer Educ 29(3):420–427
Burhansstipanov L et al (2012) Preliminary lessons learned from the “Native Navigators and the Cancer Continuum” (NNACC). J Cancer Educ 27(Suppl 1):S57–S65
Krebs LU, Burhansstipanov L, Watanabe-Galloway S, Pingatore NL, Petereit DG, Isham D (2013) Navigation as an intervention to eliminate disparities in American Indian communities. Semin Oncol Nurs 29(2):118–127
Guadagnolo BA, Boylan A, Sargent M, Koop D, Brunette D, Kanekar S, Shortbull V, Molloy K, Petereit DG (2011) Patient navigation for American Indians undergoing cancer treatment: utilization and impact on care delivery in a regional health care center. Cancer 117(12):2754–2761
Guadagnolo BA, Cina K, Koop D, Brunette D, Petereit DG (2011) A pre-post survey analysis of satisfaction with health care and medical mistrust after patient navigation for American Indian cancer patients. J Health Care Poor Underserved 22(4):1331–1343
Petereit DG et al (2011) Addressing cancer disparities among American Indians through innovative technologies and patient navigation: the walking forward experience. Front Oncol 1:11
Petereit DG, Molloy K, Reiner ML, Helbig P, Cina K, Miner R, Tail CS, Rost C, Conroy P, Roberts CR (2008) Establishing a patient navigator program to reduce cancer disparities in the American Indian communities of Western South Dakota: initial observations and results. Cancer Control 15(3):254–259
Mokuau N, Braun KL, Wong LK, Higuchi P, Gotay CC (2008) Development of a family intervention for Native Hawaiian women with cancer: a pilot study. Soc Work 53(1):9–19
Cuesta-Briand B, Bessarab D, Shahid S, Thompson SC (2015) Addressing unresolved tensions to build effective partnerships: lessons from an Aboriginal cancer support network. Int J Equity Health 14(1):122
Cuesta-Briand B, Bessarab D, Shahid S, Thompson SC (2016) 'Connecting tracks': exploring the roles of an Aboriginal women's cancer support network. Health Soc Care Commun 24(6):779–788
Pruthi S, Stange KJ, Malagrino GD Jr, Chawla KS, LaRusso NF, Kaur JS (2013) Successful implementation of a telemedicine-based counseling program for high-risk patients with breast cancer. Mayo Clin Proc 88(1):68–73
Sabesan S, Larkins S, Evans R, Varma S, Andrews A, Beuttner P, Brennan S, Young M (2012) Telemedicine for rural cancer care in North Queensland: bringing cancer care home. Aust J Rural Health 20(5):259–264
Hill TG, Briant KJ, Bowen D, Boerner V, Vu T, Lopez K, Vinson E (2010) Evaluation of Cancer 101: an educational program for native settings. J Cancer Educ 25(3):329–336
Hodge F, Nandy K, Cadogan M, Itty T, Warda U, Martinez F, Quan A (2016) Predictors of pain management among American Indian cancer survivors. J Health Care Poor Underserved 27(2):636–643
Dignan MB, Burhansstipanov L, Hariton J, Harj L, Rattler T, Lee R, Mason M (2005) A comparison of two Native American Navigator formats: face-to-face and telephone. Cancer Control 12(Suppl 2):28–33
Doorenbos AZ, Eaton LH, Haozous E, Towle C, Revels L, Buchwald D (2010) Satisfaction with telehealth for cancer support groups in rural American Indian and Alaska Native communities. Clin J Oncol Nurs 14(6):765–770
Ferris DG, Condorhuaman WSG, Waller J, Lilienthal A (2015) Impact of a video intervention for rural Peruvian women with cervical neoplasia before loop excisional procedures. J Lower Genit Tract Dis 19(3):224–228
Cueva M (2010) Readers' theatre as cancer education: an organic inquiry in Alaska awakening possibilities in a living spiral of understanding. J Cancer Educ 25(1):3–8
Hodge FS, Itty TL, Cadogan MP, Martinez F (2012) “Weaving balance into life”: development and cultural adaptation of a cancer symptom management toolkit for Southwest American Indians. J Cancer Surviv 6(2):182–188
Warson E (2012) Healing pathways: art therapy for American Indian cancer survivors. J Cancer Educ 27(1):S47–S56
Cueva M, Kuhnley R, Lanier A, Dignan M (2005) Using theater to promote cancer education in Alaska. J Cancer Educ 20(1):45–48
Elliott BA, Johnson KM, Elliott TE, Day JJ (1999) Enhancing cancer pain control among American Indians (ECPCAI): a study of the Ojibwe of Minnesota. J Cancer Educ 14(1):28–33
Sanderson PR, Teufel-Shone NI, Baldwin JA, Sandoval N, Robinson F (2010) Breast cancer education for Navajo women: a pilot study evaluating a culturally relevant video. J Cancer Educ 25(2):217–223
Dockery LE, Motwani A, Ding K, Doescher M, Dvorak JD, Moore KN, Holman LL (2018) Improving cancer care for American Indians with cervical cancer in the Indian Health Service (IHS) system — navigation may not be enough. Gynecol Oncol 149:89–92
Cuesta-Briand B et al (2015) Addressing unresolved tensions to build effective partnerships: lessons from an Aboriginal cancer support network. Int J Equity Health 14(122):1–10
Ivers R, Jackson B, Levett T, Wallace K, Winch S (2019) Home to health care to hospital: evaluation of a cancer care team based in Australian Aboriginal primary care. Aust J Rural Health 27(1):88–92
Bierbaum M et al (2017) Challenges to uptake of cancer education resources by rural Aboriginal Health Workers: the Cancer Healing Messages flipchart experience. Rural Remote Health 17:4199
Dignan MB, Burhansstipanov L, Bemis L (2005) Successful implementation of genetic Education for Native Americans workshops at national conferences. Genetics 169(2):517–521
Krebs LU, et al. (2013) Navigation as an intervention to eliminate disparities in American Indian communities. Semin Oncol Nurs 29(2):118–127
Kovach M (2009) Indigenous methodologies: characteristics, conversations and contexts. University of Toronto Press, Toronto
Canadian Public Health Association. In the News: Canadian Journal of Public Health adopts requirement for meaningful engagement of First Nations, Inuit, Métis, and Indigenous Peoples 2020 December 8 2020 [cited 2020 December 8 2020]; Available from: https://www.cpha.ca/canadian-journal-public-health-adopts-requirement-meaningful-engagement-first-nations-inuit-metis?utm_source=CPHA+Weekly+Update&utm_campaign=83235be584-EMAIL_CAMPAIGN_2019_12_12_04_17_COPY_01&utm_medium=email&utm_term=0_5a537eba78-83235be584-164511607. Accessed 8 Dec 2020
Public Health Agency of Canada. Aboriginal ways tried and true. 2020 [cited 2020; Available from: https://cbpp-pcpe.phac-aspc.gc.ca/aboriginalwtt/.
Allen L, Hatala A, Ijaz S, Courchene ED, Bushie EB (2020) Indigenous-led health care partnerships in Canada. Can Med Assoc J 192(9):E208–E216
Davy C, Kite E, Sivak L, Brown A, Ahmat T, Brahim G, Dowling A, Jacobson S, Kelly T, Kemp K, Mitchell F, Newman T, O’Brien M, Pitt J, Roesch K, Saddler C, Stewart M, Thomas T (2017) Towards the development of a wellbeing model for Aboriginal and Torres Strait Islander peoples living with chronic disease. BMC Health Serv Res 17(1):659
Acknowledgements
We would like to thank Dr. Linda Juergensen, Mr. Wenjun (Jason) Chen, and Ms. Tara Abdul-Fatah for their help with screening studies and data extraction.
Code availability
Not applicable
Funding
This work was supported by grants from the Ontario Ministry of Health and Long-term Care Health System Research Fund Call for Targeted Research in Nursing (#417) and Canadian Institute of Health Research (CIHR) (#163079)
Author information
Authors and Affiliations
Contributions
WG conceptualized and secured funding for the study. She designed and led the study and drafted the manuscript. PD and MB are citizens of Algonquins of Pikwàkanagàn First Nation and healthcare providers with Algonquins of Pikwàkanagàn Health Services and Family Health Team; they incorporated Indigenous knowledge into the data analysis and interpretation of findings. MR and SM assisted with data analysis, interpretation of findings, and drafting the manuscript. MR additionally assisted with supervising trainees. SM, ZA, and LW contributed to data collection and quality appraisal. LS developed and executed the search strategy. All authors contributed to interpretation of findings and editing the manuscript. All authors approved the final manuscript.
Corresponding author
Ethics declarations
Ethics approval
Not applicable
Consent to participate
Not applicable
Consent for publication
Not applicable
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Gifford, W., Rowan, M., Dick, P. et al. Interventions to improve cancer survivorship among Indigenous Peoples and communities: a systematic review with a narrative synthesis. Support Care Cancer 29, 7029–7048 (2021). https://doi.org/10.1007/s00520-021-06216-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00520-021-06216-7