Abstract
Purpose
To explore the effect of chemotherapy-induced amenorrhea (CIA) on female osteosarcoma patients’ fertility function, we investigated and analyzed their marital status, fertility, and menstrual status in a retrospective cohort study.
Methods
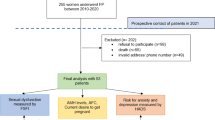
We selected female osteosarcoma patients from database from January 2004 to December 2013. Patients’ characteristics such as age, tumor location, marital status, menstrual status, and fertility status were collected. The data were analyzed using the Statistical Package for the Social Sciences (SPSS), version 22.
Results
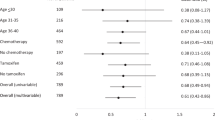
A total of 122 female patients met these criteria and finally responded by questionnaire and telephone follow-up. The marriage rate of female osteosarcoma survivors was 50.8% (62/122), which was significantly lower than the control group (p = 0.000). The average marriage age of female osteosarcoma survivors was 25.5, which was obviously higher than the control group (p = 0.000). CIA occurred in 46 (36.1%) patients. We then found that the incidence of CIA was higher in older patients. (p = 0.011). All of the married patients wanted to have children, and 67.8% (42/62) of them had given birth after chemotherapy. The fertility of married patients with CIA was significantly reduced compared to that of married patients without CIA. (p = 0.001).
Conclusions
The patients with CIA have higher risk of impaired reproductive function than those who did not. Fertility preservation option before the start of the chemotherapy is important. And it is much value to record menstrual pattern and detect sex steroid levels after 6 months of therapy in order to be able to evaluate the fertility status.
Similar content being viewed by others
Data availability
Not applicable.
References
Xiaohui N (2019) Status and prospect of the combined therapy for osteosarcoma in China. Chin J Anat Clin 24(1):1–5. https://doi.org/10.3760/cma.j.issn.2095.7041.2019.01.001
Lee SJ, Schover LR, Partridge AH, Patrizio P, Wallace WH, Hagerty K, Beck LN, Brennan LV, Oktay K (2006) American Society of Clinical Oncology recommendations on fertility preservation in cancer patients. J Clin Oncol 24:2917–2931. https://doi.org/10.1200/JCO.2006.06.5888
Loren AW, Mangu PB, Beck LN, Brennan L, Magdalinski AJ, Partridge AH, Quinn G, Wallace WH, Oktay K, American Society of Clinical Oncology (2013) Fertility preservation for patients with cancer: American Society of Clinical Oncology clinical practice guideline update. J Clin Oncol 31:2500–2510. https://doi.org/10.1200/JCO.2013.49.2678
Yonemoto T, Takahashi M, Maru M, Tomioka A, Saito M, Araki Y, Tazaki M, Tsuchiya M, Iwata S, Kamoda H, Ishii T (2016 Aug) Marriage and fertility in long-term survivors of childhood, adolescent and young adult (AYA) high-grade sarcoma. Int J Clin Oncol 21(4):801–807. https://doi.org/10.1007/s10147-016-0948-2 Epub 2016 Jan 20
HOSHI M, TAKAMI M, IEGUCHI M et al (2014) Fertility following treatment of high-grade malignant bone and soft tissue tumors in young adults. Mol Clin Oncol 3(2):367–374
Ginsberg JP, Goodman P, Leisenring W, Ness KK, Meyers PA, Wolden SL, Smith SM, Stovall M, Hammond S, Robison LL, Oeffinger KC (2010) Long-term survivors of childhood Ewing sarcoma: report from the childhood cancer survivor study. J Natl Cancer Inst 102(16):1272–1283
Greve T, Wielenga VT, Grauslund M, Sørensen N, Christiansen DB, Rosendahl M, Yding Andersen C (2013) Ovarian tissue cryopreserved for fertility preservation from patients with Ewing or other sarcomas appear to have no tumour cell contamination. Eur J Cancer 49(8):1932–1938
The Sixth National Population Census of China (2010). Http://http://www.stats.gov.cn/ztjc/zdtjgz/zgrkpc/dlcrkpc/
Qiu S, Lin T, Zhu Y (2019) Marital status and survival in osteosarcoma patients: an analysis of the Surveillance, Epidemiology, and End Results (SEER) database. Medical science monitor: international medical journal of experimental and clinical research 25:8190–8203. https://doi.org/10.12659/MSM.918048
Walshe JM, Denduluri N, Swain SM (2006) Amenorrhea in premenopausal women after adjuvant chemotherapy for breast cancer. J Clin Oncol 24:5769–5779
Yuksel A, Bildik G, Senbabaoglu F, Akin N, Arvas M, Unal F, Kilic Y, Karanfil I, Eryılmaz B, Yilmaz P, Ozkanbaş C, Taskiran C, Aksoy S, Guzel Y, Balaban B, Ince U, Iwase A, Urman B, Oktem O (2015) The magnitude of gonadotoxicity of chemotherapy drugs on ovarian follicles and granulosa cells varies depending upon the category of the drugs and the type of granulosa cells. Hum Reprod:dev256. https://doi.org/10.1093/humrep/dev256
Walshe JM, Denduluri N, Swain SM (2006) Amenorrhea in premenopausal women after adjuvant chemotherapy for breast cancer. J Clin Oncol 24:5769–5779
Ben-Aharon I, Meizner I, Granot T, Uri S, Hasky N, Rizel S, Yerushalmi R, Sulkes A, Stemmer SM (2012) Chemotherapy-induced ovarian failure as a prototype for acute vascular toxicity. Oncologist. 17:1386–1393
Swain SM, Land SR, Ritter MW, Costantino JP, Cecchini RS, Mamounas EP, Wolmark N, Ganz PA (2009) Amenorrhea in premenopausal women on the doxorubicin-and-cyclophosphamide-followed-by-docetaxel arm of NSABP B-30 trial. Breast Cancer Res Treat 113:315–320
Kim Z, Min SY, Yoon CS, Lee HJ, Lee JS, Youn HJ, Park HK, Noh DY, Hur MH, Korean Breast Cancer Society (2014) The basic facts of Korean breast cancer in 2011: results of a nationwide survey and breast cancer registry database. J Breast Cancer 17:99–106
Elgindy E, Sibai H, Abdelghani A, Mostafa M (2015) Protecting ovaries during chemotherapy through gonad suppression: a systematic review and meta-analysis. Obstet Gynecol 126:187–195. https://doi.org/10.1097/AOG.0000000000000905
Munster PN (2016) Effect of temporary ovarian suppression on chemotherapy-induced amenorrhea, pregnancy, and outcome. JAMA Oncol 2:1089–1090. https://doi.org/10.1001/jamaoncol.2016.0614
Donnez J, Dolmans MM (2018 Jan 25) Fertility preservation in women. N Engl J Med 378(4):400–401. https://doi.org/10.1056/NEJMc1715731
Lambertini M, Cinquini M, Moschetti I et al (2017) Temporary ovarian suppression during chemotherapy to preserve ovarian function and fertility in breast cancer patients: A GRADE approach for evidence evaluation and recommendations by the Italian Association of Medical Oncology. Eur J Cancer. https://doi.org/10.1016/j.ejca.2016.10.034
Jadoul P, Dolmans MM, Donnez J (2010) Fertility preservation in girls during childhood: is it feasible, efficient and safe and to whom should it be proposed? Hum Reprod Update 16:617–630
Code availability
Not applicable.
Funding
This study was funded by “Beijing Hospitals Authority Youth Programme” (grant number QML20170406).
Author information
Authors and Affiliations
Contributions
All authors contributed to the study conception and design. Material preparation, data collection, and analysis were performed by Jiang Yang, Huang Zhen, and Xu Hairong. The first draft of the manuscript was written by Jiang Yang and all authors commented on previous versions of the manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Ethics approval and consent to participate
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards. Informed consent was obtained from all individual participants included in the study.
Consent for publication
All authors are in agreement with the publication of the manuscript.
Conflict of interest
The authors declare no conflict of interest.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Yang, J., Zhen, H., Hairong, X. et al. Chemotherapy-induced amenorrhea and its effects on fertility in long-term female survivors of classic osteosarcoma. Support Care Cancer 29, 5999–6004 (2021). https://doi.org/10.1007/s00520-021-06069-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00520-021-06069-0