Abstract
Introduction
Depression symptoms, frequently diagnosed in older patients with cancer, impacts on oncological treatment feasibility. The Francophone Society of Geriatric Oncology (SOFOG) has initiated a systematic review on depression treatment in older patients with cancer, to advocate guidelines.
Data sources
Medline via PubMed, Embase, CENTRAL.
Methods
We included randomized and non-randomized controlled trials, reviews and meta-analysis, retrospective and prospective cohort studies, qualitative studies, and guidelines published between January 2013 and December 2018 that involved depression with cancer in which the entire sample or a sub-group aged 65 and above. Efficacy and tolerance of depression treatment were examined, as a primary or secondary outcome, among articles published in French or English.
Results
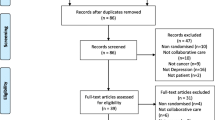
Of 3171 references, only seven studies met our eligibility criteria. This systematic review reveals a lack of evidence-based knowledge in this field, preventing from making any recommendations on drug and non-drug therapies. It has highlighted the need for multidisciplinary collaboration with the French and Francophone Society of Psycho-Oncology.
Conclusion
In clinical practice, we advise health professionals to use the screening process not as a result but rather as an opportunity to engage with the patient and also to question the need for antidepressants and non-drug therapies.

Similar content being viewed by others
References
Nelson CJ, Cho C, Berk AR, Holland J, Roth AJ (2010) Are gold standard depression measures appropriate for use in geriatric cancer patients? A systematic evaluation of self-report depression instruments used with geriatric, cancer, and geriatric cancer samples. J Clin Oncol 28:348–356. https://doi.org/10.1200/JCO.2009.23.0201
Krebber AM, Buffart LM, Kleijn G et al (2014) Prevalence of depression in cancer patients: a meta-analysis of diagnostic interviews and self-report instruments. Psycho-Oncology 23:121–130. https://doi.org/10.1002/pon.3409
Goldzweig G, Baider L, Rottenberg Y, Andritsch E, Jacobs JM (2018) Is age a risk factor for depression among the oldest old with cancer? J Geriatr Oncol 9(5):476–481. https://doi.org/10.1016/j.jgo.2018.03.011
Wildiers H, Heeren P, Puts M, Topinkova E, Janssen-Heijnen ML, Extermann M et al (2014) International Society of Geriatric Oncology consensus on geriatric assessment in older patients with cancer. J Clin Oncol 32:2595–2603. https://doi.org/10.1200/JCO.2013.54.8347
Saracino RM, Weinberger MI, Roth AJ, Hurria A, Nelson CJ (2017) Assessing depression in a geriatric cancer population. Psychooncology 26:1484–1490. https://doi.org/10.1002/pon.4160
Magnuson A, Sattar S, Nightingale G, Saracino R, Skonecki E, Trevino KM (2019) A practical guide to geriatric syndromes in older adults with cancer: a focus on falls, cognition, polypharmacy, and depression. Am Soc Clin Oncol Educ Book 39:e96–e109. https://doi.org/10.1200/EDBK_237641
World Health Organization (2018) International Classification of Diseases-11. [Internet document]. Retrieved from https://www.who.int/classifications/icd/en/. Accessed 23 April 2020
American Psychiatric Association (2013) Diagnostic and Statistical Manuel of Mental Disorders: DSM-5. [Internet document]. Retrieved from https://cdn.website-editor.net/30f11123991548a0af708722d458e476/files/uploaded/DSM%2520V.pdf. Accessed 23 April 2020
Dauchy S, Leger I, des Guetz G, Ellien F, Tidjani L, Zelzl L et al (2012) What kind of psycho-oncological care for elderly cancer patients? Short guidelines from the French Society of Psycho-Oncology. Psycho-Oncol 6:43–49. https://doi.org/10.1007/s11839-012-0359-1
Coelho A, Parola V, Cardoso D, Bravo ME, Apóstolo J (2017) Use of non-pharmacological interventions for comforting patients in palliative care: a scoping review. JBI Database System Rev Implement Rep 15(7):1867–1904. https://doi.org/10.11124/JBISRIR-2016-003204
Haute Autorité de Santé (2017). Épisode dépressif caractérisé de l’adulte : prise en charge en premier recours [Internet document]. Retrieved from https://www.has-sante.fr/jcms/c_1739917/fr/episode-depressif-caracterise-de-l-adulte-prise-en-charge-en-premier-recours. Accessed 23 April 2020
Weinberger MI, Roth AJ, Nelson CJ (2009) Untangling the complexities of depression diagnosis in older cancer patients. Oncologist. 14:60–66. https://doi.org/10.1634/theoncologist.2008-0147
Seppala LJ, Wermelink AMAT, de Vries M, Ploegmakers KJ, van de Glind EMM, Daams JG et al (2018) Fall-risk-increasing drugs: a systematic review and meta-analysis: II. Psychotropics. J Am Med Dir Assoc 19(4):371.e11–371.e17. https://doi.org/10.1016/j.jamda.2017.12.098
Sharma M, Loh KP, Nightingale G, Mohile SG, Holmes HM (2016) Polypharmacy and potentially inappropriate medication use in geriatric oncology. J Geriatr Oncol 7(5):346–353. https://doi.org/10.1016/j.jgo.2016.07.010
Hamilton M (1960) A rating scale for depression. J Neurol Neurosurg Psychiatry 23:56–62
Beck AT, Ward CH, Mendelson M, Mock J, Erbaugh J (1961) An inventory for measuring depression. Arch Gen Psychiatry 4:561–571
Montgomery SA, Asberg M (1979) A new depression scale designed to be sensitive to change. Br J Psychiatry 134:382–389. https://doi.org/10.1192/bjp.134.4.382
Zigmond AS, Snaith RP (1983) The Hospital Anxiety and Depression Scale. Acta Psychiatr Scand 67(6):361–370
Dai J, Liao N, Shi J, Tao JQ (2017) Study of prevalence and influencing factors of depression in tumor patients and the therapeutic effects of fluoxetine. Eur Rev Med Pharmacol Sci 21(21):4966–4974
Haque R, Shi J, Schottinger JE, Ahmed SA, Cheetham TC, Chung J et al (2015) Tamoxifen and antidepressant drug interaction in a cohort of 16,887 breast cancer survivors. J Natl Cancer Inst 108(3). https://doi.org/10.1093/jnci/djv337
Ostuzzi G, Matcham F, Dauchy S, Barbui C, Hotopf M (2018) Antidepressants for the treatment of depression in people with cancer. Cochrane Database Syst Rev 4:CD011006. https://doi.org/10.1002/14651858.CD011006.pub3
Sakaguchi S, Okamura H (2015) Effectiveness of collage activity based on a life review in elderly cancer patients: a preliminary study. Palliat Support Care 13(2):285–293. https://doi.org/10.1017/S1478951514000194
Sharpe M, Walker J, Holm Hansen C, Martin P, Symeonides S, Gourley C et al (2014) SMaRT (Symptom Management Research Trials) Oncology-2 Team Integrated collaborative care for comorbid major depression in patients with cancer (SMaRT Oncology-2): a multicentre randomised controlled effectiveness trial. Lancet 384(9948):1099–1108. https://doi.org/10.1016/S0140-6736(14)61231-9
Vyas A, Babcock Z, Kogut S (2017) Impact of depression treatment on health-related quality of life among adults with cancer and depression: a population-level analysis. J Cancer Surviv 11(5):624–633. https://doi.org/10.1007/s11764-017-0635-y
Yagli NV, Ulger O (2015) The effects of yoga on the quality of life and depression in elderly breast cancer patients. Complement Ther Clin Pract 21(1):7–10. https://doi.org/10.1016/j.ctcp.2015.01.002
Walker J, Sharpe M, Kroenke K, Murray G (2010) The HSCL-20: one questionnaire, two versions. J Psychosom Res 68:313–314. https://doi.org/10.1016/j.jpsychores.2009.11.002
Fisch MJ, Loehrer PJ, Kristeller J, Passik S, Jung S, Shen J, Arquette MA, Brames MJ, Einhorn LH, Hoosier Oncology Group (2003) Fluoxetine versus placebo in advanced cancer outpatients: a double-blinded trial of the Hoosier Oncology Group. J Clin Oncol 21(10):1937–1943. https://doi.org/10.1200/JCO.2003.08.025
Musselman DL, Somerset WI, Guo Y, Manatunga AK, Porter M, Penna S, Lewison B, Goodkin R, Lawson K, Lawson D, Evans DL, Nemeroff CB (2006) A double-blind, multicenter, parallel-group study of paroxetine, desipramine, or placebo in breast cancer patients (stages I, II, III, and IV) with major depression. J Clin Psychiatry 67(2):288–296. https://doi.org/10.4088/jcp.v67n0217
Razavi D, Allilaire JF, Smith M, Salimpour A, Verra M, Desclaux B, Saltel P, Piollet I, Gauvain-Piquard A, Trichard C, Cordier B, Fresco R, Guillibert E, Sechter D, Orth JP, Bouhassira M, Mesters P, Blin P (1996) The effect of fluoxetine on anxiety and depression symptoms in cancer patients. Acta Psychiatr Scand 94:205–210. https://doi.org/10.1111/j.1600-0447.1996.tb09850.x
Elias R, Loh KP, Targia V, Whitehead M, Canin B, Jatoi A et al (2020) Behavioral, psychological, and supportive care interventions in geriatric oncology: the Cancer and Aging Research Group infrastructure core. J Geriatr Oncol 11(2):347–349. https://doi.org/10.1016/j.jgo.2019.07.019
Schroyen S, Adam S, Jerusalem G, Missotten P (2014) Ageism and its clinical impact in oncogeriatry: state of knowledge and therapeutic leads. Clin Interv Aging 10:117–125. https://doi.org/10.2147/CIA.S70942
Choi JW, Park EC (2019) Suicide risk after cancer diagnosis among older adults: a nationwide retrospective cohort study [published online ahead of print, 2019 Nov 28]. J Geriatr Oncol S1879-4068(19):30379–30819. https://doi.org/10.1016/j.jgo.2019.11.006
Hsu T, Loscalzo M, Ramani R, Forman S, Popplewell L, Clark K, Katheria V, Feng T, Strowbridge R, Rinehart R, Smith D, Matthews K, Dillehunt J, Hurria A (2014) Factors associated with high burden in caregivers of older adults with cancer. Cancer 120(18):2927–2935. https://doi.org/10.1002/cncr.28765
Simmons LA (2007) Self-perceived burden in cancer patients: validation of the Self-perceived Burden Scale. Cancer Nurs 30(5):405–411. https://doi.org/10.1097/01.NCC.0000290816.37442.af
Carver CS (1997) You want to measure coping but your protocol’s too long: consider the brief COPE. Int J Behav Med 4(1):92–100. https://doi.org/10.1207/s15327558ijbm0401_6
De Vries M, van Weert JC, Jansen J, Lemmens VE, Maas HA (2007) Step by step development of clinical care pathways for older cancer patients: necessary or desirable? Eur J Cancer 43(15):2170–2178. https://doi.org/10.1016/j.ejca.2007.08.004
Piau A, Bourgade G, Berbon C, Nourhashemi F, Louit C, Balardy L (2019) Access to individualized oncology care for older patients in complex healthcare networks: The skilled nurse option. J Geriatr Oncol S1879-4068(19):30329–30327. https://doi.org/10.1016/j.jgo.2019.10.014
Nelson CJ, Saracino RM, Roth AJ, Harvey E, Martin A, Moore M et al (2019) Cancer and aging: reflections for elders (CARE): a pilot randomized controlled trial of a psychotherapy intervention for older adults with cancer. Psychooncology 28(1):39–47. https://doi.org/10.1002/pon.4907
Scotté F, Bossi P, Carola E, Cudennec T, Dielenseger P, Gomes F et al (2018) Addressing the quality of life needs of older patients with cancer: a SIOG consensus paper and practical guide. Ann Oncol 29(8):1718–1726. https://doi.org/10.1093/annonc/mdy228
Acknowledgments
The authors would like to thank the SOFOG and SFFPO scientific directors for having sustained this project.
Funding
The geriatricians’ research time is funded by the French National Cancer Institute (INCa) via the regional Coordination Units in Geriatric Oncology (UCOG).
Author information
Authors and Affiliations
Contributions
VFD, BB, JYN, CC, and DB have planned and designed the study,
VFD, BB, and JYN have performed the systematic review,
BB, OS, and CC were major contributors in writing the manuscript.
All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no competing interests.
Ethics approval
Not requested.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
ESM 1
(DOCX 33 kb).
Rights and permissions
About this article
Cite this article
Beauplet, B., Soulie, O., Niemier, JY. et al. Dealing with the lack of evidence to treat depression in older patients with cancer: French Societies of Geriatric Oncology (SOFOG) and PsychoOncology (SFFPO) position paper based on a systematic review. Support Care Cancer 29, 563–571 (2021). https://doi.org/10.1007/s00520-020-05682-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00520-020-05682-9