Abstract
Purpose
This study retrospectively investigated relationships among risk factors and post-hepatectomy surgical site infection (SSI) and other complications in patients who underwent hepatectomy for hepatocellular carcinoma (HCC).
Methods
We included 334 patients who underwent hepatectomies for liver cancers between January 2011 and December 2015 in this study. We evaluated risk factors for SSI and other post-hepatectomy complication, including demographic factors, preoperative factors, and preoperative intervention including oral management, perioperative factors, and length of hospital stay, with univariate and multivariate analyses. The oral management intervention included self-care instructions, extraction of infected teeth, removal of dental plaques and calculus (scaling), professional mechanical teeth cleaning, removal of tongue coating, and cleaning of dentures. SSI was defined in accordance with the guideline issued by the Centers for Disease Control and Prevention; it included purulent discharge from any incision or organ space within 30 days postoperatively, with or without microbiological evidence. Complications of grade II or greater, according to the Clavien-Dindo classification, were regarded as postoperative complications.
Results
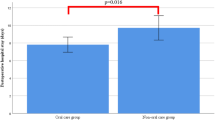
We found bacterial infection of ascites (Odds ratio (OR) = 13.72), lack of preoperative oral management intervention (OR = 10.17), and severe liver fibrosis (OR = 2.76) to be associated with SSI and severe liver fibrosis (OR = 2.28), hypoalbuminemia (OR = 2.02), blood transfusion (OR = 1.86), and longer operation time (OR = 1.80) to be associated with postoperative complications.
Conclusions
Preoperative oral management may reduce the risk of SSI in patients with HCC who undergo hepatectomy.
Similar content being viewed by others
References
Torre LA, Bray F, Siegel RL, Ferlay J, Lortet-Tieulent J, Jemal A (2015) Global cancer statistics, 2012. CA Cancer J Clin 65:87–108
Wei AC, Tung-Ping Poon R, Fan ST, Wong J (2003) Risk factors for perioperative morbidity and mortality after extended hepatectomy for hepatocellular carcinoma. Br J Surg 90:33–41
Yang T, Zhang J, Lu JH, Yang GS, Wu MC, Yu WF (2011) Risk factors influencing postoperative outcomes of major hepatic resection of hepatocellular carcinoma for patients with underlying liver diseases. World J Surg 35:2073–2082
Imamura H, Seyama Y, Kokudo N, Maema A, Sugawara Y, Sano K et al (2003) One thousand fifty-six hepatectomies without mortality in 8 years. Arch Surg 138:1198–1206
Togo S, Matsuo K, Tanaka K, Matsumoto C, Shimizu T, Ueda M, Morioka D, Nagano Y, Endo I, Shimada H (2007) Perioperative infection control and its effectiveness in hepatectomy patients. J Gastroenterol Hepatol 22:1942–1948
Mangram AJ, Horan TC, Pearson ML, Silver LC, Jarvis WR (1999) Guideline for prevention of surgical site infection, 1999. Centers for Disease Control and Prevention (CDC) Hospital Infection Control Practices Advisory Committee. Am J Infect Control 27:97–132 quiz 133-4
Kokudo T, Uldry E, Demartines N, Halkic N (2015) Risk factors for incisional and organ space surgical site infections after liver resection are different. World J Surg 39:1185–1192
Uchiyama K, Ueno M, Ozawa S, Kiriyama S, Kawai M, Hirono S, Tani M, Yamaue H (2011) Risk factors for postoperative infectious complications after hepatectomy. J Hepatobiliary Pancreat Sci 18:67–73
Soutome S, Yanamoto S, Funahara M, Hasegawa T, Komori T, Yamada SI et al (2017) Effect of perioperative oral care on prevention of postoperative pneumonia associated with esophageal cancer surgery: a multicenter case-control study with propensity score matching analysis. Medicine (Baltimore) 96:e7436
Pedersen PU, Larsen P, Håkonsen SJ (2016) The effectiveness of systematic perioperative oral hygiene in reduction of postoperative respiratory tract infections after elective thoracic surgery in adults: a systematic review. JBI Database System Rev Implement Rep 14:140–173
Nobuhara H, Yanamoto S, Funahara M, Matsugu Y, Hayashida S, Soutome S et al (2018) Effect of perioperative oral management on the prevention of surgical site infection after colorectal cancer surgery: a multicenter retrospective analysis of 698 patients via analysis of covariance using propensity score. Medicine (Baltimore) 97:e12545
Sato J, Goto J, Harahashi A, Murata T, Hata H, Yamazaki Y, Satoh A, Notani KI, Kitagawa Y (2011) Oral health care reduces the risk of postoperative surgical site infection in inpatients with oral squamous cell carcinoma. Support Care Cancer 19:409–416
Ichida F, Tsuji T, Omata M, Inoue K, Kamimura T, Yamada G et al (1996) New Inuyama classification; new criteria for histological assessment of chronic hepatitis. Int Hepatol Commun 6:112–119
Clavien PA, Barkun J, de Oliveira ML, Vauthey JN, Dindo D, Schulick RD, de Santibañes E, Pekolj J, Slankamenac K, Bassi C, Graf R, Vonlanthen R, Padbury R, Cameron JL, Makuuchi M (2009) The Clavien-Dindo classification of surgical complications: five-year experience. Ann Surg 250:187–196
Benzoni E, Molaro R, Cedolini C, Favero A, Cojutti A, Lorenzin D, Intini S, Adani GL, Baccarani U, Bresadola F, Uzzacu A (2007) Liver resection for HCC: analysis of causes and risk factors linked to postoperative complications. Hepatogastroenterology. 54:186–189
Lee CW, Tsai HI, Sung CM, Chen CW, Huang SW, Jeng WJ et al (2016) Risk factors for early mortality after hepatectomy for hepatocellular carcinoma. Medicine (Baltimore) 95:e5028
Taketomi A, Kitagawa D, Itoh S, Harimoto N, Yamashita Y, Gion T, Shirabe K, Shimada M, Maehara Y (2007) Trends in morbidity and mortality after hepatic resection for hepatocellular carcinoma: an institute’s experience with 625 patients. J Am Coll Surg 204:580–587
Sato N, Kenjo A, Kimura T, Okada R, Ishigame T, Kofunato Y, Shimura T, Abe K, Ohira H, Marubashi S (2018) Prediction of major complications after hepatectomy using liver stiffness values determined by magnetic resonance elastography. Br J Surg 105:1192–1199
Tang H, Lu W, Yang Z, Jiang K, Chen Y, Lu S et al (2017) Risk factors and long-term outcome for postoperative intra-abdominal infection after hepatectomy for hepatocellular carcinoma. Medicine (Baltimore) 96:e6795
Schindl MJ, Redhead DN, Fearon KC, Garden OJ, Wigmore SJ, Edinburgh Liver Surgery and Transplantation Experimental Research Group (eLISTER) (2005) The value of residual liver volume as a predictor of hepatic dysfunction and infection after major liver resection. Gut. 54:289–296
Fernández J, Gustot T (2012) Management of bacterial infections in cirrhosis. J Hepatol 56(Suppl 1):S1–S12
Gascón P, Zoumbos NC, Young NS (1984) Immunologic abnormalities in patients receiving multiple blood transfusions. Ann Intern Med 100:173–177
Tranchart H, Gaillard M, Chirica M, Ferretti S, Perlemuter G, Naveau S, Dagher I (2015) Multivariate analysis of risk factors for postoperative complications after laparoscopic liver resection. Surg Endosc 29:2538–2544
Nitta H, Beppu T, Itoyama A, Higashi T, Sakamoto K, Nakagawa S, Mima K, Okabe H, Imai K, Hayashi H, Hashimoto D, Chikamoto A, Ishiko T, Baba H (2015) Poor outcomes after hepatectomy in patients with ascites infected by methicillin-resistant staphylococci. J Hepatobiliary Pancreat Sci. 22:166–176
Yoshikawa T, Nomi T, Hokuto D, Yasuda S, Kawaguchi C, Yamada T, Kanehiro H, Nakajima Y (2017) Risk factors for postoperative ascites in patients undergoing liver resection for hepatocellular carcinoma. World J Surg 41:2095–2100
Wade WG (2013) The oral microbiome in health and disease. Pharmacol Res 69:137–143
Han YW, Wang X (2013) Mobile microbiome: oral bacteria in extra-oral infections and inflammation. J Dent Res 92:485–491
Humphrey LL, Fu R, Buckley DI, Freeman M, Helfand M (2008) Periodontal disease and coronary heart disease incidence: a systematic review and meta-analysis. J Gen Intern Med 23:2079–2086
Sfyroeras GS, Roussas N, Saleptsis VG, Argyriou C, Giannoukas AD (2012) Association between periodontal disease and stroke. J Vasc Surg 55:1178–1184
Acknowledgments
We thank the Edanz Group (https://en-author-services.edanzgroup.com) for editing the draft of this manuscript.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Hasegawa, T., Takeda, D., Tanaka, M. et al. Effects of preoperative dental examination and oral hygiene instruction on surgical site infection after hepatectomy: a retrospective study. Support Care Cancer 29, 653–659 (2021). https://doi.org/10.1007/s00520-020-05525-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00520-020-05525-7