Abstract
Purpose
Depressive symptoms of patients with intracranial tumors need to be assessed adequately. The Patient Health Questionnaire for Depression and Anxiety (PHQ-4) is an ultra-short screening tool consisting of four items, a cutoff of six indicates depressive symptoms. The aim was to assess patients’ psychological burden by the PHQ-4 compared with the results of well-established screening instruments.
Methods
Patients were screened three times after primary diagnosis postoperatively (t1), after 3 (t2) and 6 (t3) months using the PHQ-4, the Hornheide Screening Instrument (HSI), the NCCN Distress Thermometer (DT), and the European Organization for Research and Treatment of Cancer Quality of Life Core Questionnaire with its brain module (EORTC QLQ-C30 + BN20). Demographic, tumor-related data, and Karnofsky Performance Scale (KPS) were analyzed. A cutoff value for PHQ-4 indicating a need for support or increased distress was determined by applying receiver operating characteristic (ROC).
Results
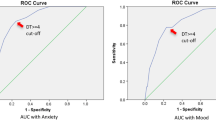
The proportion of patients reaching a total score ≥ 6 was n = 32 out of 139 (23%) at t1; at t2, n = 12 out of 117 (10%) scored ≥ 6. At t3, n = 8 out of 96 (8%) scored ≥ 6. At t1, PHQ-4 scores did not differ significantly between gender, age groups, and tumor laterality. A cutoff value of 2.5 was identified to moderately discriminate between patients in or not in distress (sensitivity 76.8%) and between patients wishing further, specific support or not (sensitivity 82.5%).
Conclusion
The PHQ4 can be applied in this patient cohort to detect those with relevant psychological comorbidities. The cutoff value should be re-evaluated in a larger cohort as we observed that a cutoff of 6, as recommended previously, may be too high in order to detect affected patients adequately.


Similar content being viewed by others
References
Pranckeviciene A, Bunevicius A (2015) Depression screening in patients with brain tumors: a review. CNS Oncol 4(2):71–78
Bunevicius A, Tamasauskas S, Deltuva V, Tamasauskas A, Bunevicius R (2013) Psychological distress symptoms’ clusters in brain tumor patients: factor analysis of depression and anxiety scales. Psycho-oncology. 22(12):2860–2863
Kvale EA, Murthy R, Taylor R, Lee JY, Nabors LB (2009) Distress and quality of life in primary high-grade brain tumor patients. Support Care Cancer 17(7):793–799
Randazzo D, Peters KB (2016) Psychosocial distress and its effects on the health-related quality of life of primary brain tumor patients. CNS Oncol 5(4):241–249
Huang J, Zeng C, Xiao J, Zhao D, Tang H, Wu H, Chen J (2017) Association between depression and brain tumor: a systematic review and meta-analysis. Oncotarget. 8(55):94932–94943
Chan CM, Wan Ahmad WA, Yusof MM, Ho GF, Krupat E (2015) Effects of depression and anxiety on mortality in a mixed cancer group: a longitudinal approach using standardised diagnostic interviews. Psycho-Oncology. 24(6):718–725
Hartung TJ, Friedrich M, Johansen C, Wittchen HU, Faller H, Koch U, Brähler E, Härter M, Keller M, Schulz H, Wegscheider K, Weis J, Mehnert A (2017) The Hospital Anxiety and Depression Scale (HADS) and the 9-item Patient Health Questionnaire (PHQ-9) as screening instruments for depression in patients with cancer. Cancer. 123(21):4236–4243
Mitchell AJ, Lord K, Slattery J, Grainger L, Symonds P (2012) How feasible is implementation of distress screening by cancer clinicians in routine clinical care? Cancer. 118(24):6260–6269
Renovanz M, Hickmann AK, Coburger J, Kohlmann K, Janko M, Reuter AK, Keric N, Nadji-Ohl M, König J, Singer S, Giese A, Hechtner M (2018) Assessing psychological and supportive care needs in glioma patients - feasibility study on the use of the supportive care needs survey short form (SCNS-SF34-G) and the supportive care needs survey screening tool (SCNS-ST9) in clinical practice. Eur J Cancer Care (Engl) 27(1). https://doi.org/10.1111/ecc.12598
Snyder CF, Dy SM, Hendricks DE, Brahmer JR, Carducci MA, Wolff AC, Wu AW (2007) Asking the right questions: investigating needs assessments and health-related quality-of-life questionnaires for use in oncology clinical practice. Support Care Cancer 15(9):1075–1085
Mitchell AJ, Coyne JC (2007) Do ultra-short screening instruments accurately detect depression in primary care? A pooled analysis and meta-analysis of 22 studies. Br J Gen Pract 57(535):144–151
Mitchell AJ (2010) Short screening tools for cancer-related distress: a review and diagnostic validity meta-analysis. J Natl Compr Cancer Netw 8(4):487–494
Goebel S, Mehdorn HM (2011) Measurement of psychological distress in patients with intracranial tumours: the NCCN distress thermometer. J Neuro-Oncol 104(1):357–364
Kawada T (2014) Patient Health Questionnaire-2 as a screening tool for psychological distress in brain tumor patients. Psycho-oncology. 23(3):353
Kroenke K, Spitzer RL, Williams JB, Lowe B (2009) An ultra-brief screening scale for anxiety and depression: the PHQ-4. Psychosomatics. 50(6):613–621
Renovanz M, Tsakmaklis H, Soebianto S, Neppel I, Nadji-Ohl M, Beutel M, Werner A, Ringel F, Hickmann AK (2018) Screening for distress in patients with intracranial tumors during the first 6 months after diagnosis using self-reporting instruments and an expert rating scale (the basic documentation for psycho-oncology short form - PO-Bado SF). Oncotarget. 9(57):31133–31145
Herschbach P, Keller M, Knight L, Brandl T, Huber B, Henrich G, Marten-Mittag B (2004) Psychological problems of cancer patients: a cancer distress screening with a cancer-specific questionnaire. Br J Cancer 91(3):504–511
Rumpold G, Augustin M, Zschocke I, Strittmatter G, Sollner W (2001) The validity of the Hornheide questionnaire for psychosocial support in skin tumor patients: a survey in an Austrian and German outpatient population with melanoma. Psychother Psychosom Med Psychol 51(1):25–33 Die Validitat des Hornheider Fragebogens zur psychosozialen Unterstutzung bei Tumorpatienten. Eine Untersuchung an zwei reprasentativen ambulanten Stichproben von Melanompatienten
Aaronson NK, Ahmedzai S, Bergman B, Bullinger M, Cull A, Duez NJ, Filiberti A, Flechtner H, Fleishman SB, JCJM H, Kaasa S, Klee M, Osoba D, Razavi D, Rofe PB, Schraub S, Sneeuw K, Sullivan M, Takeda F (1993) The European Organization for Research and Treatment of Cancer QLQ-C30: a quality-of-life instrument for use in international clinical trials in oncology. J Natl Cancer Inst 85(5):365–376
Taphoorn MJ, Claassens L, Aaronson NK, Coens C, Mauer M, Osoba D, Stupp R, Mirimanoff RO, van den Bent M, Bottomley A, EORTC Quality of Life Group, and Brain Cancer, NCIC and Radiotherapy Groups (2010) An international validation study of the EORTC brain cancer module (EORTC QLQ-BN20) for assessing health-related quality of life and symptoms in brain cancer patients. Eur J Cancer 46(6):1033–1040
Lowe B, Wahl I, Rose M, Spitzer C, Glaesmer H, Wingenfeld K et al (2010) A 4-item measure of depression and anxiety: validation and standardization of the Patient Health Questionnaire-4 (PHQ-4) in the general population. J Affect Disord 122(1–2):86–95
Strittmatter G, Tilkorn M, Mawick R (2002) How to identify patients in need of psychological intervention. Recent Results Cancer Res 160:353–361
Strittmatter G (2006) Screening-Instrumente zur Ermittlung der Betreuungsbedürftigkeit von Tumorpatienten. In: Herschbach P, Heußner P, Sellschopp A (eds) Psycho-Onkologie Perspektiven heute. Papst Science Publishers, Lengerich, pp 122–142
Goebel S, Stark AM, Kaup L, von Harscher M, Mehdorn HM (2011) Distress in patients with newly diagnosed brain tumours. Psycho-oncology. 20(6):623–630
Cohen J (1988) Statistical power analysis for the behavioral sciences, 2nd edn. Lawrence Erlenbaum Associates, New Jersey
Viera AJ, Garrett JM (2005) Understanding interobserver agreement: the kappa statistic. Fam Med 37(5):360–363
Hickmann AK, Hechtner M, Nadji-Ohl M, Janko M, Reuter AK, Kohlmann K, Haug M, Grüninger S, Deininger M, Ganslandt O, König J, Wirtz CR, Coburger J, Renovanz M (2017) Evaluating patients for psychosocial distress and supportive care needs based on health-related quality of life in primary brain tumors: a prospective multicenter analysis of patients with gliomas in an outpatient setting. J Neurooncol 131(1):135–151. https://doi.org/10.1007/s11060-016-2280-0
Akobeng AK (2007) Understanding diagnostic tests 3: receiver operating characteristic curves. Acta Paediatr 96(5):644–647
Marten-Mittag B, Book K, Buchhold B, Dinkel A, Grundobler B, Henrich G et al (2015) The basic documentation for psycho-oncology short form (PO-Bado SF)–an expert rating scale for distress screening: development and psychometric properties. Psycho-oncology. 24(6):653–660
Boele FW, Zant M, Heine EC, Aaronson NK, Taphoorn MJ, Reijneveld JC et al (2014) The association between cognitive functioning and health-related quality of life in low-grade glioma patients. Neuro Oncol Practice 1(2):40–46
Bosma I, Vos MJ, Heimans JJ, Taphoorn MJ, Aaronson NK, Postma TJ et al (2007) The course of neurocognitive functioning in high-grade glioma patients. Neuro-Oncology. 9(1):53–62
Spiers S, Oral E, Fontham ETH, Peters ES, Mohler JL, Bensen JT, Brennan CS (2018) Modelling attrition and nonparticipation in a longitudinal study of prostate cancer. BMC Med Res Methodol 18(1):60
Newberry A, Sherwood P, Hricik A, Bradley S, Kuo J, Crago E, Hoffman LA, Given BA (2010) Understanding recruitment and retention in neurological research. J Neurosci Nurs 42(1):47–57
Taphoorn MJ, Klein M (2004) Cognitive deficits in adult patients with brain tumours. Lancet Neurol 3(3):159–168
Halkett GK, Lobb EA, Rogers MM, Shaw T, Long AP, Wheeler HR et al (2015) Predictors of distress and poorer quality of life in high grade glioma patients. Patient Educ Couns 98(4):525–532
Weihs KL, Wiley JF, Crespi CM, Krull JL, Stanton AL (2018) Predicting future major depression and persistent depressive symptoms: development of a prognostic screener and PHQ-4 cutoffs in breast cancer patients. Psycho-oncology. 27(2):420–426
Mainio A, Hakko H, Niemela A, Koivukangas J, Rasanen P (2006) Gender difference in relation to depression and quality of life among patients with a primary brain tumor. Eur Psychiatry 21(3):194–199
Low J, Gessler S, Williams R, Daniells E, Brough V, Tookman A, Jones L (2009) Screening for distress and depression in cancer patients: is ultrashort depression screening a valid measure in the UK? A prospective validation study. J Pain Symptom Manag 38(2):234–243
Boele FW, van Uden-Kraan CF, Hilverda K, Weimer J, Donovan HS, Drappatz J, Lieberman FS, Verdonck-de Leeuw I, Sherwood PR (2017) Neuro-oncology family caregivers’ view on keeping track of care issues using eHealth systems: it’s a question of time. J Neuro-Oncol 134(1):157–167
Goebel S, von Harscher M, Mehdorn HM (2011) Comorbid mental disorders and psychosocial distress in patients with brain tumours and their spouses in the early treatment phase. Support Care Cancer 19(11):1797–1805
Acknowledgements
We thank all patients who participated in the study. We acknowledge all further members of our study group—Markus Haug, Susanne Janz, Güler Savas and Stefan Kindel—for the tremendous support. This work contains parts of the dissertation of Isabell Neppel, Sari Soebianto and Helena Tsakmaklis. This study was funded by the Friedhelm Frees Stiftung, Mainz, Germany.
Funding
The study was supported by the Friedhelm Frees Stiftung, Mainz, Germany. The authors have no financial relationship with the organization that sponsored the research.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest. The first author has full control of all primary data and agrees the journal to review the data if requested.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Renovanz, M., Soebianto, S., Tsakmaklis, H. et al. Evaluation of the psychological burden during the early disease trajectory in patients with intracranial tumors by the ultra-brief Patient Health Questionnaire for Depression and Anxiety (PHQ-4). Support Care Cancer 27, 4469–4477 (2019). https://doi.org/10.1007/s00520-019-04718-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00520-019-04718-z