Abstract
Purpose
Malignant pleural effusion (MPE) affects 1 million people worldwide annually and can significantly impair physical activity. Accelerometry is a validated method of objectively assessing physical activity. The purpose of this study was to determine the compliance in patients with MPE to accelerometry and describe their activity.
Methods
Patients with MPE wore an Actigraph GT3X accelerometer over a 7-day continuous wear protocol. Compliance was measured as the percent of patients who had ≥4 valid days (i.e., 8-h/day of waking wear-time). Eastern Cooperative Oncology Group performance status was documented the day of actigraphy initialization.
Results
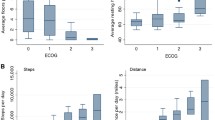
Forty-six patients with MPE received accelerometers; 44 (95.7%) returned their device. No complications were reported on their use. Forty subjects (90.9%) had ≥4 valid days of wear-time. Patients spent most of their waking hours sedentary [mean 11.0 h (SD 1.95)], with limited participation in moderate and vigorous physical activity [mean 9.5 min (SD 14.16)]. Compared to patients with better performance status (n = 32), patients with poorer performance status (n = 11) spent significantly more hours/day sedentary [mean difference 2.1 (CI 0.86–3.32); p = 0.001], as did those who survived <3 months (n = 5) compared to >12 months (n = 27) [mean difference 2.6 (CI 0.49–4.77); p = 0.013).
Conclusion
Accelerometry was applied successfully in patients with MPE with high compliance and no adverse events. This is the first reported objectively measured physical activity in patients with MPE and revealed high sedentary behavior and low physical activity. The data reflected patient performance status and discriminated between survival groups. Accelerometry can provide a useful measure for future interventional studies in patients with MPE.



Similar content being viewed by others
References
Light RW (2011) Pleural effusions. Med Clin North Am 95(6):1055–1070. doi:10.1016/j.mcna.2011.08.005
Clive AO, Kahan BC, Hooper CE, Bhatnagar R, Morley AJ, Zahan-Evans N et al (2014) Predicting survival in malignant pleural effusion: development and validation of the LENT prognostic score. Thorax 69(12):1098–1104. doi:10.1136/thoraxjnl-2014-205285
Thomas R, Francis R, Davies HE, Lee YC (2014) Interventional therapies for malignant pleural effusions: the present and the future. Respirology 19(6):809–822. doi:10.1111/resp.12328
Cheville AL, Novotny PJ, Sloan JA, Basford JR, Wampfler JA, Garces YI et al (2011) The value of a symptom cluster of fatigue, dyspnea, and cough in predicting clinical outcomes in lung cancer survivors. J Pain Symptom Manag 42(2):213–221. doi:10.1016/j.jpainsymman.2010.11.005
O’Driscoll M, Corner J, Bailey C (1999) The experience of breathlessness in lung cancer. Eur J Cancer Care (Engl) 8(1):37–43
Lowe SS, Danielson B, Beaumont C, Watanabe SM, Baracos VE, Courneya KS (2014) Associations between objectively measured physical activity and quality of life in cancer patients with brain metastases. J Pain Symptom Manag 48(3):322–332. doi:10.1016/j.jpainsymman.2013.10.012
Vallance JK, Boyle T, Courneya KS, Lynch BM (2014) Associations of objectively assessed physical activity and sedentary time with health-related quality of life among colon cancer survivors. Cancer 120(18):2919–2926. doi:10.1002/cncr.28779
Solberg Nes L, Liu H, Patten CA, Rausch SM, Sloan JA, Garces YI et al (2012) Physical activity level and quality of life in long term lung cancer survivors. Lung Cancer 77(3):611–616. doi:10.1016/j.lungcan.2012.05.096
Sloan JA, Cheville AL, Liu H, Novotny PJ, Wampfler JA, Garces YI et al (2016) Impact of self-reported physical activity and health promotion behaviors on lung cancer survivorship. Health Qual Life Outcomes 14:66. doi:10.1186/s12955-016-0461-3
Lynch BM, Cerin E, Owen N, Hawkes AL, Aitken JF (2008) Prospective relationships of physical activity with quality of life among colorectal cancer survivors. J Clin Oncol 26(27):4480–4487. doi:10.1200/jco.2007.15.7917
Canario AC, Cabral PU, de Paiva LC, Florencio GL, Spyrides MH, Goncalves AK (2016) Physical activity, fatigue and quality of life in breast cancer patients. Rev Assoc Med Bras 62(1):38–44. doi:10.1590/1806-9282.62.01.38
Beesley VL, Price MA, Butow PN, Green AC, Olsen CM, Webb PM (2011) Physical activity in women with ovarian cancer and its association with decreased distress and improved quality of life. Psychooncology 20(11):1161–1169. doi:10.1002/pon.1834
Kelly CM, Shahrokni A (2016) Moving beyond Karnofsky and ECOG performance status assessments with new technologies. J Oncol 2016:6186543. doi:10.1155/2016/6186543
Oken MM, Creech RH, Tormey DC, Horton J, Davis TE, McFadden ET et al (1982) Toxicity and response criteria of the Eastern Cooperative Oncology group. Am J Clin Oncol 5(6):649–655
Schag CC, Heinrich RL, Ganz PA (1984) Karnofsky performance status revisited: reliability, validity, and guidelines. J Clin Oncol 2(3):187–193
Light RW, Rogers JT, Cheng D, Rodriguez RM (1999) Large pleural effusions occurring after coronary artery bypass grafting. Cardiovascular surgery associates, PC. Ann Intern Med 130(11):891–896
Courneya KS, McNeely ML, Culos-Reed SN, Vallance JK, Bell GJ, Mackey JR et al (2016) The Alberta moving beyond breast cancer (AMBER) cohort study: recruitment, baseline assessment, and description of the first 500 participants. BMC Cancer 16:481. doi:10.1186/s12885-016-2534-4
McVeigh JA, Winkler EA, Healy GN, Slater J, Eastwood PR, Straker LM (2016) Validity of an automated algorithm to identify waking and in-bed wear time in hip-worn accelerometer data collected with a 24 h wear protocol in young adults. Physiol Meas 37(10):1636–1652. doi:10.1088/0967-3334/37/10/1636
Evenson KR, Wen F, Metzger JS, Herring AH (2015) Physical activity and sedentary behavior patterns using accelerometry from a national sample of United States adults. Int J Behav Nutr Phys Act 12:20. doi:10.1186/s12966-015-0183-7
Freedson PS, Melanson E, Sirard J (1998) Calibration of the computer science and applications, Inc. accelerometer. Med Sci Sports Exerc 30(5):777–781
Matthews CE, Chen KY, Freedson PS, Buchowski MS, Beech BM, Pate RR et al (2008) Amount of time spent in sedentary behaviors in the United States, 2003-2004. Am J Epidemiol 167(7):875–881. doi:10.1093/aje/kwm390
Feito Y, Garner HR, Bassett DR (2015) Evaluation of ActiGraph’s low-frequency filter in laboratory and free-living environments. Med Sci Sports Exerc 47(1):211–217. doi:10.1249/mss.0000000000000395
Tudor-Locke C, Leonardi C, Johnson WD, Katzmarzyk PT, Church TS (2011) Accelerometer steps/day translation of moderate-to-vigorous activity. Prev Med 53(1–2):31–33. doi:10.1016/j.ypmed.2011.01.014
Tudor-Locke C, Schuna JM Jr, Barreira TV, Mire EF, Broyles ST, Katzmarzyk PT et al (2013) Normative steps/day values for older adults: NHANES 2005-2006. J Gerontol A Biol Sci Med Sci 68(11):1426–1432. doi:10.1093/gerona/glt116
van Roekel EH, Winkler EA, Bours MJ, Lynch BM, Willems PJ, Meijer K et al (2016) Associations of sedentary time and patterns of sedentary time accumulation with health-related quality of life in colorectal cancer survivors. Prev Med Rep 4:262–269. doi:10.1016/j.pmedr.2016.06.022
Cavalheri V, Jenkins S, Cecins N, Phillips M, Sanders LH, Hill K (2016) Patterns of sedentary behaviour and physical activity in people following curative intent treatment for non-small cell lung cancer. Chron Respir Dis 13(1):82–85. doi:10.1177/1479972315616931
Granger CL, McDonald CF, Irving L, Clark RA, Gough K, Murnane A et al (2014) Low physical activity levels and functional decline in individuals with lung cancer. Lung Cancer 83(2):292–299. doi:10.1016/j.lungcan.2013.11.014
Campbell PT, Patel AV, Newton CC, Jacobs EJ, Gapstur SM (2013) Associations of recreational physical activity and leisure time spent sitting with colorectal cancer survival. J Clin Oncol 31(7):876–885. doi:10.1200/jco.2012.45.9735
Matthews CE, Moore SC, Sampson J, Blair A, Xiao Q, Keadle SK et al (2015) Mortality benefits for replacing sitting time with different physical activities. Med Sci Sports Exerc 47(9):1833–1840. doi:10.1249/mss.0000000000000621
Tudor-Locke C, Barreira TV, Schuna JM Jr, Mire EF, Chaput JP, Fogelholm M et al (2015) Improving wear time compliance with a 24-hour waist-worn accelerometer protocol in the international study of childhood obesity, lifestyle and the environment (ISCOLE). Int J Behav Nutr Phys Act 12:–11. doi:10.1186/s12966-015-0172-x
Matthews CE, Ainsworth BE, Thompson RW, Bassett DR Jr (2002) Sources of variance in daily physical activity levels as measured by an accelerometer. Med Sci Sports Exerc 34(8):1376–1381
Cormie P, Newton RU, Spry N, Joseph D, Taaffe DR, Galvao DA (2013) Safety and efficacy of resistance exercise in prostate cancer patients with bone metastases. Prostate Cancer Prostatic Dis 16(4):328–335. doi:10.1038/pcan.2013.22
Cormie P, Galvao DA, Spry N, Joseph D, Taaffe DR, Newton RU (2014) Functional benefits are sustained after a program of supervised resistance exercise in cancer patients with bone mestastases: longitudinal results of a pilot study. Support Care Cancer 22:1537–1548. doi:10.1007/s00520-013-2103-1
Acknowledgements
EJ receives an Australian Lung Foundation and Edith Cowan University PhD scholarship. YCGL is a National Health and Medical Research Council (NHMRC) of Australia Career Development Fellow and receives project grant funding from the NHMRC, New South Wales Dust Disease Board, Sir Charles Gairdner Research Advisory Committee, Lung Institute of Western Australia Westcare Alan King Grants, and the Cancer Council Western Australia. LS receives an NHMRC of Australia Senior Research Fellowship. CJM is supported by a Cancer Council Western Australia Postdoctoral Research Fellowship. The authors have full control of all primary data, which can be reviewed by the journal upon request
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflicts of interest.
Rights and permissions
About this article
Cite this article
Jeffery, E., Lee, Y., McVeigh, J. et al. Feasibility of objectively measured physical activity and sedentary behavior in patients with malignant pleural effusion. Support Care Cancer 25, 3133–3141 (2017). https://doi.org/10.1007/s00520-017-3721-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00520-017-3721-9