Abstract
Purpose
Taste and smell changes (TSCs) are common in head and neck (H&N) cancer and during and after chemotherapy (CT) and radiotherapy (RT). It is an area that has been under-investigated, particularly in the treatment-naive, but can negatively impact nutritional status. This study examined the prevalence, severity and characteristics of TSCs in people with non-H&N solid tumours, before CT and RT, and their relationship with co-occurring symptoms.
Methods
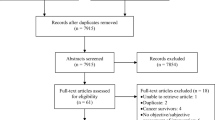
A prospective, observational study was conducted. Forty consecutive pre-treatment cancer patients, referred to radiation oncology outpatients over 6 weeks, were recruited. Data on TSCs, symptoms and nutritional status were obtained using the ‘Taste and Smell Survey’ and the ‘abridged Patient-Generated Subjective Global Assessment’ (abPG-SGA). BMI was measured. SPSS® was used for statistical analysis. Two-sided P values <0.05 were considered statistically significant.
Results
Most patients were newly diagnosed (n = 28; 70 %). Nineteen (48 %) reported TSCs; nine noted a stronger sweet and seven a stronger salt taste. Of these, four reported a stronger and four a weaker smell sensation. Those at nutritional risk reported more TSCs (n = 13/20). TSCs were significantly associated with dry mouth (P < 0.01), early satiety (P < 0.05) and fatigue (P < 0.05).
Conclusions
TSCs preceded CT or RT in almost half of treatment-naive patients with solid tumours, notably stronger sweet and salt tastes. Half of the study group were at nutritional risk; the majority of these reported TSCs. TSCs were significantly associated with other symptoms. Future research and clinical guidelines, with a common terminology for assessment, diagnosis and management of cancer TSCs, are needed.


Similar content being viewed by others
References
Brisbois TD, Hutton JL, Baracos VE, Wismer WV (2006) Taste and smell abnormalities as an independent cause of failure of food intake in patients with advanced cancer-an argument for the application of sensory science. J Palliat Care 22:111–114
Hutton JL, Baracos VE, Wismer WV (2007) Chemosensory dysfunction is a primary factor in the evolution of declining nutritional status and quality of life in patients with advanced cancer. J Pain Symptom Manag 33:156–165
Hoffman HJ, Cruickshanks KJ, Davis B (2009) Perspectives on population-based epidemiological studies of olfactory and taste impairment. Ann N Y Acad Sci 1170:514–530
Henkin RI, Levy LM, Fordyce A (2013) Taste and smell function in chronic disease: a review of clinical and biochemical evaluations of taste and smell dysfunction in over 5000 patients at The Taste and Smell Clinic in Washington. DC Am J Otolaryngol 34:477–489
Landis BN, Beutner D, Frasnelli J, Hüttenbrink KB, Hummel T (2005) Gustatory function in chronic inflammatory middle ear diseases. Laryngoscope 115:1124–1127
Zabernigg A, Gamper EM, Giesinger JM, Rumpold G, Kemmler G, Gattringer K, Sperner-Unterweger B, Holzner B (2010) Taste alterations in cancer patients receiving chemotherapy: a neglected side effect? Oncologist 15:913–920
Ovesen L, Hannibal J, Sørensen M, Allingstrup L (1991) Food intake, eating-related complaints, and smell and taste sensations in patients with cancer of the lung, ovary and breast undergoing chemotherapy. Clin Nutr 10:336–341
Baharvand M, Shoaleh Saadi N, Barakian R, Moghaddam EJ (2013) Taste alteration and impact on quality of life after head and neck radiotherapy. J Oral Pathol Med 42:106–112
Leyrer CM, Chan MD, Peiffer AM, Horne E, Harmon M, Carter AF, Hinson WH, Mirlohi S, Duncan SE, Dietrich AM, GJ L (2014) Taste and smell disturbances after brain irradiation: a dose-volume histogram analysis of a prospective observational study. Pract Radiat Oncol 4:130–135
McGreevy J, Orrevall Y, Belqaid K, Wismer W, Tishelman C, BM B (2014) Characteristics of taste and smell alterations reported by patients after starting treatment for lung cancer. Support Care Cancer 22:2635–2644
Belqaid K, Orrevall Y, McGreevy J, Månsson-Brahme E, Wismer W, Tishelman C, BM B (2014) Self-reported taste and smell alterations in patients under investigation for lung cancer. Acta Oncol 53:1405–1412
Bernhardson BM, Tishelman C, LE R (2008) Self-reported taste and smell changes during cancer chemotherapy. Support Care Cancer 16:275–283
Gamper EM, Zabernigg A, Wintner LM, Giesinger JM, Oberguggenberger A, Kemmler G, Sperner-Unterweger B, Holzner B (2012) Coming to your senses: detecting taste and smell alterations in chemotherapy patients. A systematic review. J Pain Symptom Manage 44:880–895
Johnson FM (2001) Alterations in taste sensation: a case presentation of a patient with end-stage pancreatic cancer. Cancer Nurs 24:149–155
Lehrer S, Levine E, Bloomer WD (1985) Abnormally diminished sense of smell in women with oestrogen receptor positive breast cancer. Lancet 2:333
Comeau TB, Epstein JB, Migas C (2001) Taste and smell dysfunction in patients receiving chemotherapy: a review of current knowledge. Support Care Cancer 9:575–580
Mattes R, Arnold C, Boraas M (1987) Learned food aversion among cancer chemotherapy patients. Cancer 60:2576–2580
Ottery FD (1994) Cancer cachexia: prevention, early diagnosis, and management. Cancer Pract 2:123–131
Walsh D, Rybicki L (2006) Symptom clustering in advanced cancer. Support Care Cancer 14:831–836
Komurcu S, Nelson KA, Walsh D, Ford RB, LA R (2002) Gastrointestinal symptoms among inpatients with advanced cancer. Am J Hosp Palliat Care 19:351–355
Heald AE, Pieper CF, Schiffman SS (1998) Taste and smell complaints in HIV-infected patients AIDS 12: 1667–1674
Gabrielson DK, Scaffidi D, Leung E, Stoyanoff L, Robinson J, Nisenbaum R, Brezden-Masley C, PB D (2013) Use of an abridged scored Patient-Generated Subjective Global Assessment (abPG-SGA) as a nutritional screening tool for cancer patients in an outpatient setting. Nutr Cancer 65:234–239
World Health Organisation. BMI Classification 2000. (Internet: http://www.who.int/bmi/index.jsp?introPage=intro_3.html) (accessed 13 April 2015)
Oken MM, Creech RH, Tormey DC, Horton J, Davis TE, McFadden ET, PP C (1982) Toxicity and response criteria of the Eastern Cooperative Oncology Group. Am J Clin Oncol 5:649–655
Steinbach S, Hundt W, Zahnert T, Berktold S, Böhner C, Gottschalk N, Hamann M, Kriner M, Heinrich P, Schmalfeldt B, Harbeck N (2010) Gustatory and olfactory function in breast cancer patients. Support Care Cancer 18:707–713
Harris AM, Griffin SM (2003) Postoperative taste and smell deficit after upper gastrointestinal cancer surgery-an unreported complication. J Surg Oncol 82:147–150 discussion 150-152
Bernhardson BM, Tishelman C, Rutqvist LE (2009) Taste and smell changes in patients receiving cancer chemotherapy: distress, impact on daily life, and self-care strategies. Cancer Nurs 32:45–54
Hummel T, Kobal G, Gudziol H, Mackay-Sim A (2007) Normative data for the “Sniffin’ Sticks” including tests of odor identification, odor discrimination, and olfactory thresholds: an upgrade based on a group of more than 3,000 subjects. Eur Arch Otorhinolaryngol 264:237–243
Maes A, Huygh I, Weltens C, Vandevelde G, Delaere P, Evers G, den Bogaert W V (2002) De Gustibus: time scale of loss and recovery of tastes caused by radiotherapy. Radiother Oncol 63:195–201
Schiffman SS (1997) Taste and smell losses in normal aging and disease. JAMA 278:1357–1362
Konstantinidis I, Chatziavramidis A, Printza A, Metaxas S, Constantinidis J (2010) Effects of smoking on taste: assessment with contact endoscopy and taste strips. Laryngoscope 120:1958–1963
Bering T, Mauricio SF, Silva JB, MI C (2014) Nutritional and metabolic status of breast cancer women. Nutr Hosp 31:751–758
Hebuterne X, Lemarie E, Michallet M, de Montreuil CB, Schneider SM, Goldwasser F (2014) Prevalence of malnutrition and current use of nutrition support in patients with cancer. J Parenter Enter Nutr 38:196–204
Brisbois TD, de Kock IH, Watanabe SM, Baracos VE, Wismer WV (2011) Characterization of chemosensory alterations in advanced cancer reveals specific chemosensory phenotypes impacting dietary intake and quality of life. J Pain Symptom Manag 41:673–683
Walsh D, Donnelly S, Rybicki L (2000) The symptoms of advanced cancer: relationship to age, gender, and performance status in 1,000 patients. Support Care Cancer 8:175–179
National Cancer Registry Ireland, Cancer in Ireland 1994–2012: annual report of the National Cancer Registry, Cork, Ireland, 2014
Cancer Research UK. Cancer Incidence Statistics 2011. (Internet: http://www.cancerresearchuk.org/health-professional/cancer-statistics/incidence) (accessed 11 August 2015)
American Cancer Society. Cancer Facts & Figures 2015. (Internet: http://www.cancer.org/acs/groups/content/@editorial/documents/document/acspc-044552.pdf) (accessed 11 August 2015)
Bowling A (2005) Mode of questionnaire administration can have serious effects on data quality. J Public Health (Oxf) 27:281–291
Alt-Epping B, Nejad RK, Jung K, Gross U, Nauck F (2012) Symptoms of the oral cavity and their association with local microbiological and clinical findings-a prospective survey in palliative care. Support Care Cancer 20:531–537
Aapro M, Arends J, Bozzetti F, Fearon K, Grunberg SM, Herrstedt J, Hopkinson J, Jacquelin-Ravel N, Jatoi A, Kaasa S, Strasser F (2014) Early recognition of malnutrition and cachexia in the cancer patient: a position paper of a European School of Oncology Task Force. Ann Oncol 25:1492–1499
Bernhardson BM, Tishelman C, LE R (2009) Olfactory changes among patients receiving chemotherapy. Eur J Oncol Nurs 13:9–15
Thorne T, Olson K, Wismer W (2015) A state-of-the-art review of the management and treatment of taste and smell alterations in adult oncology patients. Support Care Cancer 23:2843–2851
Acknowledgments
The authors acknowledge the patients and staff at St. Luke’s Radiation Oncology Network, St. James’s Hospital and Our Lady’s Hospice and Care Services for their support. Particular thanks to Aine Breen, Mary Cunningham, Aoife Gorham, Anita O’Donovan, Anne O’Hara and Laoise Ryan for their help with the logistical planning of the study.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethical approval was obtained from the Research Ethics Committee at St. Luke’s Radiation Oncology Network and the joint St. James’s Hospital/Adelaide and Meath Hospital, Dublin Research Ethics Committee.
Conflict of interest
None
Disclosures
None
Rights and permissions
About this article
Cite this article
Spotten, L., Corish, C., Lorton, C. et al. Subjective taste and smell changes in treatment-naive people with solid tumours. Support Care Cancer 24, 3201–3208 (2016). https://doi.org/10.1007/s00520-016-3133-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00520-016-3133-2