Abstract
Purpose
Fatigue is a prevalent, distressing side effect of cancer and cancer treatment which commonly coexists with insomnia. Cognitive behavioral therapy for insomnia (CBT-I) has been shown to improve insomnia in cancer patients, but less is known about its ability to impact fatigue. This work is the analysis for a secondary aim of a four-arm randomized controlled trial (RCT) study assessing the combined and comparative effect of CBT-I and a wakefulness-promoting agent, armodafinil (A), to improve sleep and daytime functioning in cancer survivors. Herein, we examine the effect of CBT-I, with and without A, on fatigue in cancer survivors.
Patients and methods
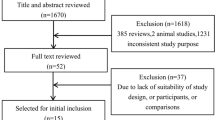
This study was a four-arm factorial study with CBTI-I (yes/no) versus A (yes/no). It consisted of 96 cancer survivors (average age 56 years; 88 % female; 68 % breast cancer). Fatigue was assessed by the brief fatigue inventory (BFI) and the FACIT-Fatigue scale. The analysis assessed the additive effects of CBT-I and A and possible non-additive effects where the effect of CBT-I changes depending on the presence or absence of A.
Results
Analyses adjusting for baseline differences showed that CBT-I improved fatigue as measured by two separate scales (BFI: P = 0.002, Std. error = 0.32, effect size (ES) = 0.46; FACIT-Fatigue: P < 0.001, Std. error = 1.74, ES = 0.64). Armodafinil alone did not show a statistically significant effect on fatigue levels (all Ps > 0.40) nor did the drug influence the efficacy of CBT-I. Structural equation analysis revealed that reductions in insomnia severity were directly responsible for improving cancer-related fatigue.
Conclusions
CBT-I with and without armodafinil resulted in a clinically and statistically significant reduction of subjective daytime fatigue in cancer survivors with chronic insomnia. Armodafinil did not improve cancer-related fatigue (CRF) and did not change the efficacy of CBT-I. Patients reporting CRF should be screened and, if indicated, treated for insomnia as part of a comprehensive fatigue management program.



Similar content being viewed by others
References
Bower JE (2014) Cancer-related fatigue—mechanisms, risk factors, and treatments. Nat Rev Clin Oncol 11(10):597–609. doi:10.1038/nrclinonc.2014.127
Barsevick AM, Irwin MR, Hinds P, Miller A, Berger A, Jacobsen P, Ancoli-Israel S, Reeve BB, Mustian K, O’Mara A, Lai JS, Fisch M, Cella D, National Cancer Institute Clinical Trials Planning M (2013) Recommendations for high-priority research on cancer-related fatigue in children and adults. J Natl Cancer Inst 105(19):1432–1440. doi:10.1093/jnci/djt242
Menning S, de Ruiter MB, Veltman DJ, Koppelmans V, Kirschbaum C, Boogerd W, Reneman L, Schagen SB (2015) Multimodal MRI and cognitive function in patients with breast cancer prior to adjuvant treatment—the role of fatigue. Neuroimage Clin 7:547–554. doi:10.1016/j.nicl.2015.02.005
Sekse RJ, Hufthammer KO, Vika ME (2015) Fatigue and quality of life in women treated for various types of gynaecological cancers: a cross-sectional study. J Clin Nurs 24(3–4):546–555. doi:10.1111/jocn.12647
Gerber LH, Stout N, McGarvey C, Soballe P, Shieh CY, Diao G, Springer BA, Pfalzer LA (2011) Factors predicting clinically significant fatigue in women following treatment for primary breast cancer. Support Care Cancer 19(10):1581–1591. doi:10.1007/s00520-010-0986-7
Scott JA, Lasch KE, Barsevick AM, Piault-Louis E (2011) Patients’ experiences with cancer-related fatigue: a review and synthesis of qualitative research. Oncol Nurs Forum 38(3):E191–203. doi:10.1188/11.ONF.E191-E203
Paiva CE, Paiva BS (2013) Prevalence, predictors, and prognostic impact of fatigue among Brazilian outpatients with advanced cancers. Support Care Cancer 21(4):1053–1060. doi:10.1007/s00520-012-1625-2
Jones JM, Olson K, Catton P, Catton CN, Fleshner NE, Krzyzanowska MK, McCready DR, Wong RK, Jiang H, Howell D (2015) Cancer-related fatigue and associated disability in post-treatment cancer survivors. J Cancer Surviv. doi:10.1007/s11764-015-0450-2
Minton O, Stone PC (2012) A comparison of cognitive function, sleep and activity levels in disease-free breast cancer patients with or without cancer-related fatigue syndrome. BMJ Support Palliat Care 2(3):231–238. doi:10.1136/bmjspcare-2011-000172
Goedendorp MM, Gielissen MF, Verhagen CA, Bleijenberg G (2013) Development of fatigue in cancer survivors: a prospective follow-up study from diagnosis into the year after treatment. J Pain Symptom Manag 45(2):213–222. doi:10.1016/j.jpainsymman.2012.02.009
Pertl MM, Hevey D, Collier S, Lambe K, O’Dwyer AM (2014) Predictors of fatigue in cancer patients before and after chemotherapy. J Health Psychol 19(6):699–710. doi:10.1177/1359105313477675
Berger AM, Abernethy AP, Atkinson A, Barsevick AM, Breitbart WS, Cella D, Cimprich B, Cleeland C, Eisenberger MA, Escalante CP, Jacobsen PB, Kaldor P, Ligibel JA, Murphy BA, O’Connor T, Pirl WF, Rodler E, Rugo HS, Thomas J, Wagner LI (2010) Cancer-related fatigue. J Natl Compr Cancer Netw 8(8):904–931
Barsevick A, Frost M, Zwinderman A, Hall P, Halyard M, Consortium G (2010) I’m so tired: biological and genetic mechanisms of cancer-related fatigue. Qual Life Res 19(10):1419–1427. doi:10.1007/s11136-010-9757-7
Miller AH, Ancoli-Israel S, Bower JE, Capuron L, Irwin MR (2008) Neuroendocrine-immune mechanisms of behavioral comorbidities in patients with cancer. J Clin Oncol 26(6):971–982. doi:10.1200/JCO.2007.10.7805
Savard J, Simard S, Ivers H, Morin CM (2005) Randomized study on the efficacy of cognitive-behavioral therapy for insomnia secondary to breast cancer, part I: sleep and psychological effects. J Clin Oncol 23(25):6083–6096. doi:10.1200/JCO.2005.09.548
Matthews EE, Berger AM, Schmiege SJ, Cook PF, McCarthy MS, Moore CM, Aloia MS (2014) Cognitive behavioral therapy for insomnia outcomes in women after primary breast cancer treatment: a randomized, controlled trial. Oncol Nurs Forum 41(3):241–253. doi:10.1188/14.ONF.41-03AP
Garland SN, Carlson LE, Stephens AJ, Antle MC, Samuels C, Campbell TS (2014) Mindfulness-based stress reduction compared with cognitive behavioral therapy for the treatment of insomnia comorbid with cancer: a randomized, partially blinded, noninferiority trial. J Clin Oncol Off J Am Soc Clin Oncol 32(5):449–457. doi:10.1200/JCO.2012.47.7265
Espie CA, Fleming L, Cassidy J, Samuel L, Taylor LM, White CA, Douglas NJ, Engleman HM, Kelly HL, Paul J (2008) Randomized controlled clinical effectiveness trial of cognitive behavior therapy compared with treatment as usual for persistent insomnia in patients with cancer. J Clin Oncol 26(28):4651–4658. doi:10.1200/JCO.2007.13.9006
Garland SN, Johnson JA, Savard J, Gehrman P, Perlis M, Carlson L, Campbell T (2014) Sleeping well with cancer: a systematic review of cognitive behavioral therapy for insomnia in cancer patients. Neuropsychiatr Dis Treat 10:1113–1124. doi:10.2147/NDT.S47790
Fleming L, Randell K, Harvey CJ, Espie CA (2014) Does cognitive behaviour therapy for insomnia reduce clinical levels of fatigue, anxiety and depression in cancer patients? Psycho-Oncology 23(6):679–684. doi:10.1002/pon.3468
Zee PC, Ancoli-Israel S, Workshop P (2009) Does effective management of sleep disorders reduce cancer-related fatigue? Drugs 69(Suppl 2):29–41. doi:10.2165/11531140-000000000-00000
Dirksen SR, Epstein DR (2008) Efficacy of an insomnia intervention on fatigue, mood and quality of life in breast cancer survivors. J Adv Nurs 61(6):664–675. doi:10.1111/j.1365-2648.2007.04560.x
Savard J, Simard S, Ivers H, Morin CM (2005) Randomized study on the efficacy of cognitive-behavioral therapy for insomnia secondary to breast cancer, part II: immunologic effects. J Clin Oncol 23(25):6097–6106. doi:10.1200/JCO.2005.12.513
Hovey E, de Souza P, Marx G, Parente P, Rapke T, Hill A, Bonaventura A, Michele A, Craft P, Abdi E, Lloyd A, Investigators M (2014) Phase III, randomized, double-blind, placebo-controlled study of modafinil for fatigue in patients treated with docetaxel-based chemotherapy. Support Care Cancer 22(5):1233–1242. doi:10.1007/s00520-013-2076-0
Spathis A, Fife K, Blackhall F, Dutton S, Bahadori R, Wharton R, O’Brien M, Stone P, Benepal T, Bates N, Wee B (2014) Modafinil for the treatment of fatigue in lung cancer: results of a placebo-controlled, double-blind, randomized trial. J Clin Oncol Off J Am Soc Clin Oncol 32(18):1882–1888. doi:10.1200/JCO.2013.54.4346
Boele FW, Douw L, de Groot M, van Thuijl HF, Cleijne W, Heimans JJ, Taphoorn MJ, Reijneveld JC, Klein M (2013) The effect of modafinil on fatigue, cognitive functioning, and mood in primary brain tumor patients: a multicenter randomized controlled trial. Neuro-Oncology 15(10):1420–1428. doi:10.1093/neuonc/not102
Berenson JR, Yellin O, Shamasunder HK, Chen CS, Charu V, Woliver TB, Sanani S, Schlutz M, Nassir Y, Swift RA, Andreu-Vieyra C, Vescio R (2014) A phase 3 trial of armodafinil for the treatment of cancer-related fatigue for patients with multiple myeloma. Support Care Cancer. doi:10.1007/s00520-014-2486-7
Roscoe JA, Garland SN, Heckler CE, Perlis ML, Peoples AR, Shayne M, Savard J, Daniels NP, Morrow GR (2014) Randomized placebo-controlled trial of cognitive behavioral therapy and armodafinil for insomnia after cancer treatment. J Clin Oncol. doi:10.1200/JCO.2014.57.6769
Perlis ML, Jungquist C, Smith MT, Posner D (2005) Cognitive behavioral tretament of insomnia: a session-by-session guide. Springer, New York
Mendoza TR, Wang XS, Cleeland CS, Morrissey M, Johnson BA, Wendt JK, Huber SL (1999) The rapid assessment of fatigue severity in cancer patients: use of the brief fatigue inventory. Cancer 85(5):1186–1196
Norman GR, Sloan JA, Wyrwich KW (2003) Interpretation of changes in health-related quality of life: the remarkable universality of half a standard deviation. Med Care 41(5):582–592. doi:10.1097/01.MLR.0000062554.74615.4C
Cella D, Eton DT, Lai JS, Peterman AH, Merkel DE (2002) Combining anchor and distribution-based methods to derive minimal clinically important differences on the Functional Assessment of Cancer Therapy (FACT) anemia and fatigue scales. J Pain Symptom Manag 24(6):547–561
Savard MH, Savard J, Simard S, Ivers H (2005) Empirical validation of the insomnia severity index in cancer patients. Psychooncology 14(6):429–441. doi:10.1002/pon.860
Little RJA, Rubin DB (2002) Statistical analysis with missing data. Wiley, Hoboken
van Buuren S (2007) Multiple imputation of discrete and continuous data by fully conditional specification. Stat Methods Med Res 16:219–242
van Buuren S, Groothuis-Oudshoorn K (2011) Mice: multivariate imputation by chained equations in R. J Stat Softw 45(3):1548–7660
Enders CK (2010) Applied missing data analysis. Guilford, New York
van Buuren S (2012) Flexible imputation of missing data, Chapman and Hall/CRC interdisciplinary statistics series. CRC, Boca Raton, FL
Byrne BM (2012) Structural equation modeling with Mplus: basic concepts, applications, and programming, Multivariate applications series. Routledge Academic, New York
Brown JN, Howard CA, Kemp DW (2010) Modafinil for the treatment of multiple sclerosis-related fatigue. Ann Pharmacother 44(6):1098–1103. doi:10.1345/aph.1M705
Golicki D, Bala MM, Niewada M, Wierzbicka A (2010) Modafinil for narcolepsy: systematic review and meta-analysis. Med Sci Monit 16(8):RA177–186
Saavedra-Velez C, Yusim A, Anbarasan D, Lindenmayer JP (2009) Modafinil as an adjunctive treatment of sedation, negative symptoms, and cognition in schizophrenia: a critical review. J Clin Psychiatry 70(1):104–112
Jean-Pierre P, Morrow GR, Roscoe JA, Heckler C, Mohile S, Janelsins M, Peppone L, Hemstad A, Esparaz BT, Hopkins JO (2010) A phase 3 randomized, placebo-controlled, double-blind, clinical trial of the effect of modafinil on cancer-related fatigue among 631 patients receiving chemotherapy: a University of Rochester Cancer Center Community Clinical Oncology Program Research base study. Cancer 116(14):3513–3520. doi:10.1002/cncr.25083
Goedendorp MM, Gielissen MF, Verhagen CA, Bleijenberg G (2009) Psychosocial interventions for reducing fatigue during cancer treatment in adults. Cochrane Database Syst Rev 1:CD006953. doi:10.1002/14651858.CD006953.pub2
Acknowledgments
This study is supported by NCI grants 5 R01 CA126968, R25 CA102618 and UG1 CA18961. Study medication was provided by Teva Pharmaceuticals USA.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
Dr. Perlis receives royalties for a CBT-I manual and demonstration DVD and research funding from Teva Pharmaceuticals and served as an advisor to InsomniSolv. He has also provided expert testimony to Cantor Colburn, LLP. None of the remaining authors have disclosures to report.
Drs. Heckler and Roscoe have full control of the primary data and agree to allow the journal to review it on request.
Rights and permissions
About this article
Cite this article
Heckler, C.E., Garland, S.N., Peoples, A.R. et al. Cognitive behavioral therapy for insomnia, but not armodafinil, improves fatigue in cancer survivors with insomnia: a randomized placebo-controlled trial. Support Care Cancer 24, 2059–2066 (2016). https://doi.org/10.1007/s00520-015-2996-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00520-015-2996-y