Abstract
Purpose
Fifty percent of patients develop chronic gastrointestinal (GI) symptoms following pelvic radiotherapy that adversely affect quality of life. Fewer than 20 % are referred to a gastroenterologist. We aimed to determine if structured gastroenterological evaluation is of benefit to this patient group.
Methods
Sixty patients with GI symptoms at ≥6 months after radical pelvic radiotherapy were identified prospectively from oncology clinics in this service evaluation. Those requiring urgent investigation were excluded. Patients were assessed at baseline using patient-reported questionnaires: inflammatory bowel disease questionnaire (IBDQ), Vaizey incontinence questionnaire, and the Common Terminology Criteria for Adverse Events (CTCAE) pelvis questionnaire. Participants were referred for gastroenterological evaluation using an algorithmic approach. Further assessments were made at 3 and 6 months.
Results
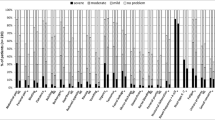
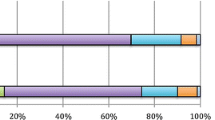
Twenty men and 36 women with primary gynecological (31), urological (17), or lower GI (8) tumors were included (mean age, 58.5 years). Median time from radiotherapy to baseline assessment was 3.0 years. Multiple GI symptoms were reported (median, 8; range, 4–16) including frequency, urgency, loose stool, fecal incontinence, flatulence, bloating/distension, and rectal bleeding. Common diagnoses included radiation proctopathy, bile acid malabsorption, diverticulosis, and colonic polyps. Statistically significant improvements in all questionnaire scores between baseline and 6 months were found: IBDQ (p = 0.014), Vaizey (p < 0.0005), and CTCAE rectum-bowel subset (p = 0.001).
Conclusions
Gastroenterological evaluation identifies significant, potentially treatable diagnoses in patients who develop chronic GI symptoms following pelvic radiotherapy. Some findings are incidental and unrelated to previous cancer treatment. Radiation-induced GI symptoms have historically been considered “untreatable.” We report the first data to show that structured gastroenterological assessment has the potential to improve outcome by identifying diagnoses and facilitating focused treatment.






Similar content being viewed by others
References
West CML, Davidson SE (2009) Measurement tools for gastrointestinal symptoms in radiation oncology. Curr Opin Support Palliat Care 3(1):36–40
Green JA et al (2001) Survival and recurrence after concomitant chemotherapy and radiotherapy for cancer of the uterine cervix: a systematic review and meta-analysis. Lancet 358(9284):781–786
Ryu H-S et al (2005) Postoperative adjuvant concurrent chemoradiotherapy improves survival rates for high-risk, early stage cervical cancer patients. Gynecol Oncol 96(2):490–495
Vale CL et al (2010) Substantial improvement in UK Cervical Cancer Survival with chemoradiotherapy: results of a Royal College of Radiologists' audit. Clin Oncol 22(7):590–601
Bentzen SM, Baumann M (2002) Clinical manifestations of normal-tissue damage. In: Steel G (ed) Basic clinical radiobiology. Hodder Arnold, London
van der Laan HP et al (2008) Grading-system-dependent volume effects for late radiation-induced rectal toxicity after curative radiotherapy for prostate cancer. Int J Radiat Oncol Biol Phys 70(4):1138–1145
Davidson SE et al (2007) Improving the capture of adverse event data in clinical trials: the role of the International Atomic Energy Agency. Int J Radiat Oncol Biol Phys 69(4):1218–1221
Denham JW et al (1999) Is there more than one late radiation proctitis syndrome? Radiother Oncol 51(1):43–53
DeCosse JJ et al (1969) The natural history and management of radiation induced injury of the gastrointestinal tract. Ann Surg 170(3):369–34
Schofield PF, Holden D, Carr ND (1983) Bowel disease after radiotherapy. J R Soc Med 76(6):463–466
Olopade FA et al (2005) A modified inflammatory bowel disease questionnaire and the Vaizey Incontinence questionnaire are simple ways to identify patients with significant gastrointestinal symptoms after pelvic radiotherapy. Br J Cancer 92:1663–1670
Barker CL et al (2009) The impact of radiotherapy late effects on quality of life in gynaecological cancer patients. Br J Cancer 100(10):1558–1565
Andreyev HJN et al (2010) Defining pelvic-radiation disease for the survivorship era. Lancet Oncol 11(4):310–312
Andreyev HJN et al (2003) GI symptoms developing after pelvic radiotherapy require gastroenterological review but is this happening in the UK? Clin Oncol 15(2):S12
Henson C et al (2011) Late onset bowel dysfunction post-pelvic radiotherapy: a national survey of current practice and opinions of clinical oncologists. Clin Oncol 23(8):552–7
Andreyev HJN et al (2005) Gastrointestinal symptoms after pelvic radiotherapy: role for the gastroenterologist? Int J Radiat Oncol Biol Phys 62(5):1464–1471
Theis VS et al (2010) Chronic radiation enteritis. Clin Oncol 22(1):70–83
Benton B et al (2011) Can nurses manage gastrointestinal symptoms arising from pelvic radiation disease? Clin Oncol 23(8):538–551
Andreyev HJ et al (2012) Practice guidance on the management of acute and chronic gastrointestinal problems arising as a result of treatment for cancer. Gut 61(2):179–192
Khalid U et al (2006) A modified inflammatory bowel disease questionnaire and the Vaizey Incontinence questionnaire are more sensitive measures of acute gastrointestinal toxicity during pelvic radiotherapy than R.T.O.G. grading. Int J Radiat Oncol Biol Phys 64(5):1432–1441
Vaizey CJ et al (1999) Prospective comparison of faecal incontinence grading systems. Gut 44(1):77–80
Farnell DJJ et al (2010) Efficacy of data capture for patient-reported toxicity following radiotherapy for prostate or cervical cancer. Eur J Cancer 46(3):534–540
Bjelland I et al (2002) The validity of the hospital anxiety and depression scale. An updated literature review. J Psychosom Res 52(2):p. 69–77
Irvine EJ (1999) Development and subsequent refinement of the inflammatory bowel disease questionnaire: a quality-of-life instrument for adult patients with inflammatory bowel disease. J Pediatr Gastroenterol Nutr 28(4):S23–7
Hlavaty T et al (2006) Evaluation of short-term responsiveness and cutoff values of inflammatory bowel disease questionnaire in Crohn's disease. Inflamm Bowel Dis 12(3):199–204
Andreyev HJN et al (2011) "Pelvic radiation disease": new understanding and new solutions for a new disease in the era of cancer survivorship. Scand J Gastroenterol 46(4):389–397
Guyatt G et al (1989) A new measure of health status for clinical trials in inflammatory bowel disease. Gastroenterology 96(3):804–810
Wedlake L et al (2008) Small bowel bacterial overgrowth and lactose intolerance during radical pelvic radiotherapy: an observational study. Eur J Cancer 44(15):2212–2217
Rusu RI et al (2012) Is the glucose hydrogen methane breath test an accurate diagnostic tool for small intestinal bacterial overgrowth? Gut 61:A248–A249
Conflict of interest
Dr. Caroline Henson received grant support from Macmillan Cancer Support and a small award from the Shire SpR Project Innovation Fund. Otherwise, none of the authors have a financial relationship with the organization that sponsored the research. The authors have full control of all primary data and agree to allow the journal to review their data if requested.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Henson, C.C., Davidson, S.E., Ang, Y. et al. Structured gastroenterological intervention and improved outcome for patients with chronic gastrointestinal symptoms following pelvic radiotherapy. Support Care Cancer 21, 2255–2265 (2013). https://doi.org/10.1007/s00520-013-1782-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00520-013-1782-y