Abstract
Purpose
In addition to cancer-related distress, people with head and neck cancer (HNC) endure facial disfigurement and difficulties with eating and communication. High rates of alcohol use and socio-economic disadvantage raise concerns that patients with HNC may be less likely than others to participate in and adhere to psychological interventions. This article aims to inform future practice and research by reviewing the evidence in support of psychological interventions for this patient group.
Methods
We searched CENTRAL, Medline, Embase, PsycINFO and CINAHL in December 2009. Relevant studies were rated for internal and external validity against the criteria of the Agency for Healthcare Research and Quality (AHRQ) US Preventive Services Task Force. Wherever possible, outcomes were evaluated using effect sizes to confirm statistically significant results and enable comparison between studies. Meta-analysis was planned according to criteria in the Cochrane Handbook for Systematic Reviews. Levels of evidence for each intervention type were evaluated using AHRQ criteria.
Results
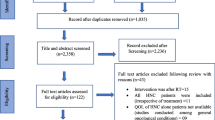
Nine studies met inclusion criteria. One study was rated ‘good’ for internal validity and four for external validity. Psycho-education and/or cognitive–behavioural therapy were evaluated by seven studies, and communication skills training and a support group by one study each. Significant heterogeneity precluded meta-analysis. Based on a study-by-study review, there was most support for psycho-education, with three out of five studies finding at least some effect.
Conclusions
Research to date suggests it is feasible to recruit people with HNC to psychological interventions and to evaluate their progress through repeated-outcome measures. Evidence for interventions is limited by the small number of studies, methodological problems, and poor comparability. Future interventions should target HNC patients who screen positive for clinical distress and be integrated into standard care.
Similar content being viewed by others
References
National Cancer Institute (2010) Head and neck cancer. http://www.cancer.gov/cancertopics/types/head-and-neck. Accessed 19th Sept 2010.
Bofetta P, Hashibe M, La Vecchia C, Zatonski W, Rehm J (2006) The burden of cancer attributable to alcohol drinking. Int J Cancer 119:884–887
Deleyiannis FW, Thomas DB, Vaughan TL et al (1996) Alcoholism: independent predictor of survival in patients with head and neck cancer. J Natl Cancer Inst 88:542–549
IOM (Institute of Medicine) (2009) State of the USA health indicators: letter report. The National Academies Press, Washington
Conway DI, McKinney PA, McMahon AD et al (2010) Socioeconomic factors associated with risk of upper aerodigestive tract cancer in Europe. Eur J Cancer 46:588–598
Zabora J, BrintzenhofeSzoc K, Curbow B, Hooker C, Piantadosi S (2001) The prevalence of psychological distress by cancer site. Psycho Oncol 10(1):19–28
Ledeboer QCP, Velden LA, Boer MF, Feenstra L, Pruyn JFA (2005) Physical and psychosocial correlates of head and neck cancer: an update of the literature and challenges for the future (1996–2003). Clin Otolaryngol 30(4):303–319
Llewellyn CD, McGurk M, Weinman J (2005) Are psycho-social and behavioural factors related to health related-quality of life in patients with head and neck cancer? A systematic review. Oral Oncol 41(5):440–454
Rogers SN, Ahad SA, Murphy AP (2007) A structured review and theme analysis of papers published on ‘quality of life’ in head and neck cancer: 2000–2005. Oral Oncol 43(9):843–868
Murphy BA, Ridner S, Wells N, Dietrich M (2007) Quality of life research in head and neck cancer: a review of the current state of the science. Crit Rev Oncol Hematol 62(3):251–267
Callahan C (2004) Facial disfigurement and sense of self in head and neck cancer. Soc Work Health Care 40(2):73–87
Frampton M (2001) Psychological distress in patients with head and neck cancer: review. Br J Oral Maxillofac Surg 39(1):67–70
Haman KL (2008) Psychologic distress and head and neck cancer: part 1–review of the literature.[see comment]. J Support Oncol 6(4):155–163
Ziegler L, Newell R, Stafford N, Lewin R (2004) A literature review of head and neck cancer patients information needs, experiences and views regarding decision-making. Eur J Cancer Care 13(2):119–126
Humphris GM, Ozakinci G (2006) Psychological responses and support needs of patients following head and neck cancer. Int J Surg 4:37–44
Chen AM, Jennelle RLS, Grady V et al (2009) Prospective study of psychosocial distress among patients undergoing radiotherapy for head and neck cancer. Int J Radiat Oncol Biol Phys 73(1):187–193
Neilson KA, Pollard AC, Boonzaier AM et al (2010) Psychological distress (depression and anxiety) in people with head and neck cancers. Med J Aust 193:S48–S51
Uitterhoeve RJ, Vernooy M, Litjens M et al (2004) Psychosocial interventions for patients with advanced cancer - a systematic review of the literature. Br J Cancer 91(6):1050–1062
Osborn RL, Demoncada AC, Feuerstein M (2006) Psychosocial interventions for depression, anxiety, and quality of life in cancer survivors: meta-analyses. Int J Psychiatry Med 36(1):13–34
Rodin G, Lloyd N, Katz M et al (2007) The treatment of depression in cancer patients: a systematic review. Support Care Cancer 15(2):123–136
Jacobsen PB, Jim HS (2008) Psychosocial interventions for anxiety and depression in adult cancer patients: achievements and challenges. CA Cancer J Clin 58(4):214–230
Semple CJ, Sullivan K, Dunwoody L, Kernohan WG (2004) Psychosocial interventions for patients with head and neck cancer: past, present, and future. Cancer Nurs 27(6):434–441
National Comprehensive Cancer Network (NCCN) (1999) NCCN practice guidelines for the management of psychosocial distress. Oncology 13:113–147
De Boer MF, McCormick LK, Pruyn JF, Ryckman RM, van den Borne BW (1999) Physical and psychosocial correlates of head and neck cancer: a review of the literature. Otolaryngol Head Neck Surg 120(3):427–436
Owen C, Watkinson JC, Pracy P, Glaholm J (2001) The psychosocial impact of head and neck cancer. Clin Otolaryngol Allied Sci 26(5):351–356
Newell SA, Sanson-Fisher RW, Savolainen NJ (2002) Systematic review of psychological therapies for cancer patients: overview and recommendations for future research. J Natl Cancer Inst 94(8):558–584
Williams S, Dale J (2006) The effectiveness of treatment for depression/depressive symptoms in adults with cancer: a systematic review. Br J Cancer 94(3):372–390
Agency for Healthcare Research and Quality (2009) Current methods of the US Preventive Services Task Force: a review of the procedures. http://www.ahrq.gov/Clinic/ajpmsuppl/harris2.htm. Accessed August 11 2009
National Breast Cancer Centre & National Cancer Control Initiative (NBCC & NCCI) (2003) Clinical practice guidelines for the psychosocial care of adults with cancer. National Breast Cancer Centre, Sydney
Higgins JPT, Green S (2008) The Cochrane Collaboration. Cochrane Handbook for Systematic Reviews of Interventions Version 5.0.1: Available from www.cochrane-handbook.org.
Cohen J (1988) Statistical power analysis for the behavioural sciences, 2nd edn. Lawrence Erlbaum, Hillsdale
Bailey JJ (2001) Development of a multi-modal psychological intervention as adjunctive therapy for smoking-related cancers. Dissertation, University of Memphis, US
Feldman JE, Baker KH (1988) The psychodynamics of prolonged treatment in a patient with cancer of the hypopharynx. Cancer Nurs 11(6):362–367
Clarke A (2001) Resourcing and training head and neck cancer nurse specialists to deliver a social rehabilitation programme to patients. Dissertation, City University
Petruson KM, Silander EM, Hammerlid EB (2003) Effects of psychosocial intervention on quality of life in patients with head and neck cancer. Head Neck 25(7):576–584
Hammerlid E, Persson LO, Sullivan M, Westin T (1999) Quality-of-life effects of psychosocial intervention in patients with head and neck cancer. Otolaryngol Head Neck Surg 120(4):507–516
Katz MR, Irish JC, Devins GM (2004) Development and pilot testing of a psychoeducational intervention for oral cancer patients. Psycho Oncol 13(9):642–653
Semple CJ, Dunwoody L, Kernohan WG, McCaughan E (2009) Development and evaluation of a problem-focused psychosocial intervention for patients with head and neck cancer. Support Care Cancer 17(4):379–388
Allison PJ, Edgar L, Nicolau B, Archer J, Black M, Hier M (2004) Results of a feasibility study for a psycho-educational intervention in head and neck cancer. Psycho Oncol 13(7):482–485
Vilela LD, Nicolau B, Mahmud S et al (2006) Comparison of psychosocial outcomes in head and neck cancer patients receiving a coping strategies intervention and control subjects receiving no intervention. J Otolaryngol 35(2):88–96
Allison PJ, Nicolau B, Edgar L, Archer J, Black M, Hier M (2004) Teaching head and neck cancer patients coping strategies: results of a feasibility study. Oral Oncol 40(5):538–544
Fiegenbaum W (1981) A social training program for clients with facial disfigurations: a contribution to the rehabilitation of cancer patients. Int J Rehabil Res 4(4):501–509
Duffy SA, Ronis DL, Valenstein M et al (2006) A tailored smoking, alcohol, and depression intervention for head and neck cancer patients. Cancer Epidemiol Biomark Prev 15(11):2203–2208
Vakharia KT, Ali MJ, Wang SJ (2007) Quality-of-life impact of participation in a head and neck cancer support group. Otolaryngol Head Neck Surg 136(3):405–410
Zimmermann T, Heinrichs N, Baucom DH (2007) “Does one size fit all?” Moderators in psychosocial interventions for breast cancer patients: a meta-analysis. Ann Behav Med 34(3):225–239
Berglund G, Petersson LM, Eriksson KC et al (2007) “Between Men”: a psychosocial rehabilitation programme for men with prostate cancer. Acta Oncol 46(1):83–89
Penedo FJ, Molton I, Dahn JR et al (2006) A randomized clinical trial of group-based cognitive-behavioral stress management in localized prostate cancer: development of stress management skills improves quality of life and benefit finding. Ann Behav Med 31(3):261–270
Parker PA, Pettaway CA, Babaian RJ et al (2009) The effects of a presurgical stress management intervention for men with prostate cancer undergoing radical prostatectomy. J Clin Oncol 27(19):3169–3176
Holland J, Weiss T (2008) The new standard of quality cancer care: integrating the psychosocial aspects in routine cancer from diagnosis through survivorship. Cancer J 14(6):425–428
Katz MR, Kopek N, Waldron J, Devins GM, Tomlinson G (2004) Screening for depression in head and neck cancer. Psycho Oncol 13(4):269–280
Center for Epidemiologic Studies (1971) Center for Epidemiologic Studies Depression Scale (CES-D). National Institute of Mental Health, Rockville
Ullrich de Muynck R, Ullrich R (1977) Der Unsicherheitsfragebogen. Testmanual und Anleitung fur den Therapeuten (Section III). Pfeiffer, Munich
Aaronson NK, Ahmedzai S, Bergman B et al (1993) The European Organization for Research and Treatment of Cancer QLQ-C30: a quality-of-life instrument for use in international clinical trials in oncology. J Natl Cancer Inst 85:365–376
Zigmond AS, Snaith RP (1983) The Hospital Anxiety and Depression Scale. Acta Psychiatr Scand 67(6):361–370
Telch CF, Telch MJ (1986) Group coping skills instruction and supportive group therapy for cancer patients: a comparison of strategies. J Consult Clin Psychol 54(6):802–808
Spielberger CD, Gorsuch RL, Lushene R, Vagg PR, Jacobs GA (1983) Manual for the State-Trait Anxiety Inventory. Consulting Psychologists, Palo Alto
Bradburn N (1969) The Structure of Psychological Well-Being. Aldine, Chicago
Atkinson T (1977) Is Satisfaction a good measure of the perceived quality of life? Annual Meeting of the American Statistical Association, Chicago, Illinois
Rogers SN, Gwanne S, Lowe D, Humphris G, Yueh B, Weymuller EAJ (2002) The addition of mood and anxiety domains to the University of Washington quality of life scale. Head Neck 24(6):521–529
Acknowledgements
We wish to acknowledge the support of the Psycho-oncology Co-operative Research Group (PoCoG), which provided the opportunity for the authors to collaborate on this review.
Conflict of interest
No organisation sponsored this research. No primary data were collected. The authors agree to allow the journal to review data subjected to secondary analysis in this article if requested.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Luckett, T., Britton, B., Clover, K. et al. Evidence for interventions to improve psychological outcomes in people with head and neck cancer: a systematic review of the literature. Support Care Cancer 19, 871–881 (2011). https://doi.org/10.1007/s00520-011-1119-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00520-011-1119-7