Abstract
Purpose
1) To determine the effect of a home-based walking exercise program on the sleep quality and quality of life of cancer patients, as well as 2) to determine if enhanced sleep quality was associated with improvement in quality of life over time.
Methods
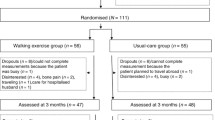
This is a prospective, longitudinal, two-armed, randomized clinical trial. Participants were recruited from oncology outpatient clinics in two university-based medical centers and were allocated to either usual care (n = 35) or a home-based walking exercise intervention for 8 weeks (n = 36). Measurements included the Taiwanese version of the Pittsburgh Sleep Quality Index, the Medical Outcomes Study Short Form-36, the Taiwanese Version Ratings of the Perceived Exertion Scale, and a walking exercise log. This study was analyzed on an intention-to-treat basis. Effects of the walking exercise program on sleep quality and quality of life were analyzed by the generalized estimating equation method.
Results
Patients in the exercise group reported significant improvements in sleep quality (β = −3.54, p < 0.01) and the mental health dimension of quality of life (β = 10.48, p < 0.01). Among patients who exercised, enhanced sleep quality also corresponded with reduced bodily pain (β = 0.98, p = 0.04) and improvements over time in the mental health dimension of quality of life (β = −3.87, p < 0.01).
Conclusions
A home-based walking exercise program can be easily incorporated into care for cancer patients who are suffering from sleep disturbances.




Similar content being viewed by others
References
Espie CA, Fleming L, Cassidy J et al (2008) Randomized controlled clinical effectiveness trial of cognitive behavior therapy compared with treatment as usual for persistent insomnia in patients with cancer. J Clin Oncol 26:4651–4658
Andrykowski MA, Curran SL, Lightner R (1998) Off-treatment fatigue in breast cancer survivors: a controlled comparison. J Behav Med 21:1–18
Carpenter JS, Elam JL, Ridner SH, Carney PH, Cherry GJ, Cucullu HL (2004) Sleep, fatigue, and depressive symptoms in breast cancer survivors and matched healthy women experiencing hot flashes. Oncol Nurs Forum 31:591–598
Mock V, Dow KH, Meares CJ et al (1997) Effects of exercise on fatigue, physical functioning, and emotional distress during radiation therapy for breast cancer. Oncol Nurs Forum 24:991–1000
Redeker NS, Lev EL, Ruggiero J (2000) Insomnia, fatigue, anxiety, depression, and quality of life of cancer patients undergoing chemotherapy. Sch Inq Nurs Pract 14:275–298
Wang RC, Wang SJ, Chang YC, Lin CC (2007) Mood state and quality of sleep in cancer pain patients: a comparison to chronic daily headache. J Pain Symptom Manage 33:32–39
Sateia MJ, Nowell PD (2004) Insomnia. Lancet 364:1959–1973
Savard J, Morin CM (2001) Insomnia in the context of cancer: a review of a neglected problem. J Clin Oncol 19:895–908
Bélanger L, Vallières A, Ivers H, Moreau V, Lavigne G, Morin CM (2007) Meta-analysis of sleep changes in control groups of insomnia treatment trials. J Sleep Res 16(1):77–84
Sherrill DL, Kotchou K, Quan SF (1998) Association of physical activity and human sleep disorders. Arch Intern Med 158:1894–1898
Shapiro CM, Bachmayer D (1988) Epidemiological aspects of sleep in general public and hospital outpatient samples. Acta Physiol Scand Suppl 574:41–43
Vuori I, Urponen H, Hasan J, Partinen M (1988) Epidemiology of exercise effects on sleep. Acta Physiol Scand Suppl 574:3–7
Singh NA, Clements KM, Fiatarone MA (1997) A randomized controlled trial of the effect of exercise on sleep. Sleep 20:95–101
King AC, Oman RF, Brassington GS, Bliwise DL, Haskell WL (1997) Moderate-intensity exercise and self-rated quality of sleep in older adults. A randomized controlled trial. JAMA 277:32–37
Yeh GY, Mietus JE, Peng CK et al (2008) Enhancement of sleep stability with Tai Chi exercise in chronic heart failure: preliminary findings using an ECG-based spectrogram method. Sleep Med 9:527–536
Tworoger SS, Yasui Y, Vitiello MV et al (2003) Effects of a yearlong moderate-intensity exercise and a stretching intervention on sleep quality in postmenopausal women. Sleep 26:830–836
Savard J, Simard S, Ivers H, Morin CM (2005) Randomized study on the efficacy of cognitive-behavioral therapy for insomnia secondary to breast cancer, part I: sleep and psychological effects. J Clin Oncol 23:6083–6096
Berger AM, Kuhn BR, Farr LA et al (2009) Behavioral therapy intervention trial to improve sleep quality and cancer-related fatigue. Psychooncology 18(6):634–646
Payne JK, Held J, Thorpe J, Shaw H (2008) Effect of exercise on biomarkers, fatigue, sleep disturbances, and depressive symptoms in older women with breast cancer receiving hormonal therapy. Oncol Nurs Forum 35:635–642
Bland M (2000) An introduction to medical statistics. Oxford University Press, Oxford
Schwartz AL (2000) Daily fatigue patterns and effect of exercise in women with breast cancer. Cancer Pract 8:16–24
Schwartz AL (2000) Exercise and weight gain in breast cancer patients receiving chemotherapy. Cancer Pract 8:231–237
Guilleminault C, Clerk A, Black J, Labanowski M, Pelayo R, Claman D (1995) Nondrug treatment trials in psychophysiologic insomnia. Arch Intern Med 155:838–844
Buysse DJ, Reynolds CF III, Monk TH, Berman SR, Kupfer DJ (1989) The Pittsburgh Sleep Quality Index: a new instrument for psychiatric practice and research. Psychiatry Res 28:193–213
Ware JE, Sherbourne CD (1992) The MOS 36-item short-form health survey (SF-36). I. Conceptual framework and item selection. Med Care 30:473–483
Lu JR, Tseng HM, Tsai YJ (2003) Assessment of health-related quality of life in Taiwan (I): development and psychometric testing of SF-36 Taiwan version. Taiwan J Public Health 22:501–511 (in Chinese)
Tseng HM, Lu JR, Tsai YJ (2003) Assessment of health-related quality of life in Taiwan (II): norming and validation of SF-36 Taiwan version. Taiwan J Public Health 22:512–518 (in Chinese)
Borg GA (1982) Psychophysical bases of perceived exertion. Med Sci Sports Exerc 14:377–381
Borg G, Linderholm H (1967) Perceived exertion and pulse rate during graded exercise in various age group. Acta Med Scand Suppl 472:194–206
Skinner JS, Hutsler R, Bergsteinova V, Buskirk ER (1973) The validity and reliability of a rating scale of perceived exertion. Med Sci Sports 5:94–96
Ulmer H, Janz U, Loogen H (1977) Aspects of the validity of Borg's scale, is it measuring stress or strain? In: Borg G (ed) Physical work and effort. Pergamon Press, New York, pp 181–196
Liang KY, Zeger SL (1986) Longitudinal data analysis using generalized liner models. Biometrika 73:13–22
Liang KY, Zeger SL, Qaqish B (1992) Multivariate regression analyses for categorical data. J R Stat Soc 54:3–40
Zeger SL, Liang KY (1986) Longitudinal data analysis for discrete and continuous outcomes. Biometrics 42:121–130
Berger AM, Farr L (1999) The influence of daytime inactivity and nighttime restlessness on cancer-related fatigue. Oncol Nurs Forum 26(10):1663–1671
Mystakidou K, Parpa E, Tsilika E et al (2007) Sleep quality in advanced cancer patients. J Psychosom Res 62:527–533
Verster JC, Veldhuijzen DS, Volkerts ER (2004) Residual effects of sleep medication on driving ability. Sleep Med Rev 8:309–325
Lawlor DA, Hopker SW (2001) The effectiveness of exercise as an intervention in the management of depression: systematic review and meta-regression analysis of randomized controlled trials. BMJ 322:763–767
Driver HS, Taylor SR (2000) Exercise and sleep. Sleep Med Rev 4:387–402
Youngstedt SD, Kline CE (2006) Epidemiology of exercise and sleep. Sleep Biol Rhythms 4:215–221
Mereles D, Ehlken N, Kreuscher S et al (2006) Exercise and respiratory training improve exercise capacity and quality of life in patients with severe chronic pulmonary hypertension. Circulation 114:1482–1489
Segal R, Evans W, Johnson D et al (2001) Structured exercise improves physical functioning in women with stages I and II breast cancer: results of a randomized controlled trial. J Clin Oncol 19:657–665
McGinty D, Szymusiak R (1990) Keeping cool: a hypothesis about the mechanisms and functions of slow-wave sleep. Trends Neurosci 13:480–487
Kräuchi K, Cajochen C, Werth E, Wirz-Justice A (1999) Warm feet promote the rapid onset of sleep. Nature 401:36–37
Horne JA, Moore VJ (1985) Sleep EEG effects of exercise with and without additional body cooling. Electroencephalogr Clin Neurophysiol 60:33–38
Berger RJ, Phillips NH (1988) Comparative aspects of energy metabolism, body temperature and sleep. Acta Physiol Scand Suppl 574:21–27
Adam K, Oswald I (1983) Protein synthesis, bodily renewal and the sleep–wake cycle. Clin Sci (Lond) 65:561–567
Naylor E, Penev PD, Orbeta L et al (2000) Daily social and physical activity increases slow-wave sleep and daytime neuropsychological performance in the elderly. Sleep 23:87–95
Blanco-Centurion CA, Shiromani PJ (2006) Beneficial effects of regular exercise on sleep in old F344 rats. Neurobiol Aging 27(12):1859–1869
Courneya KS, Friedenreich CM (1997) Determinants of exercise during colorectal cancer treatment: an application of the theory of planned behavior. Oncol Nurs Forum 24:1715–1723
Courneya KS, Friedenreich CM (1997) Relationship between exercise during treatment and current quality of life among survivors of breast cancer. J Psychosoc Oncol 15:35–57
Courneya KS, Blanchard CM, Laing DM (2001) Exercise adherence in breast cancer survivors training for a dragon boat race competition: a preliminary investigation. Psychooncology 10:444–452
Courneya KS, Keats MR, Turner AR (2000) Social cognitive determinants of hospital-based exercise in cancer patients following high dose chemotherapy and bone marrow transplantation. Int J Behav Med 7:189–203
Jones LW, Courneya KS (2002) Exercise counseling and programming preferences of cancer survivors. Cancer Pract 10:208–215
Acknowledgments
The authors are grateful to Ms. Denise Dipert for her expertise in editing this paper.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Tang, MF., Liou, TH. & Lin, CC. Improving sleep quality for cancer patients: benefits of a home-based exercise intervention. Support Care Cancer 18, 1329–1339 (2010). https://doi.org/10.1007/s00520-009-0757-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00520-009-0757-5