Summary
Background
Multiple sclerosis is an inflammatory disorder of the central nervous system. Inflammation may create high susceptibility to subclinical atherosclerosis. The purpose of this study was to compare subclinical atherosclerosis and the role of inflammatory cytokines between the group of patients with relapsing-remitting multiple sclerosis (RRMS) and healthy controls matched for age and sex.
Methods
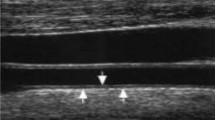
The study group consisted of 112 non-diabetic and non-hypertensive RRMS patients treated with disease modifying drugs (DMD) and the control group was composed of 51 healthy subjects. The common carotid artery (CCA) intima media thickness (IMT) was investigated. Serum levels of risk factors for atherosclerosis and inflammatory cytokines were also determined.
Results
The mean CCA IMT (0.572 ± 0.131 mm vs. 0.571 ± 0.114 mm) did not differ (p > 0.05) between patients and controls. The RRMS patients’ CCA IMT was significantly correlated with serum interleukin 6 (IL-6) (p = 0.027), high-sensitivity C-reactive protein (hs-CRP) (p = 0.027), cystatin C (p < 0.0005), glucose (p = 0.031), cholesterol (p = 0.008), LDL (p = 0.021), erythrocyte sedimentation rate (p = 0.001) and triglyceride (p = 0.018) level. We fitted generalized linear models in order to assess the relationship between CCA IMT and IL‑6 with adjustment for sex and age. The obtained results showed that adjusted for age (p < 0.001) and sex (p = 0.048) IL‑6 serum levels statistically significantly (p = 0.009) predict CCA IMT only in the RRMS group.
Conclusion
The findings of the present study suggest that when treated with DMD RRMS might not be an independent risk factor for early atherosclerosis presenting with arterial wall thickening; however, the results suggest a significant association of IL‑6 serum levels with CCA IMT only in the RRMS group.
Similar content being viewed by others
References
Wingerchuk DM, Weinshenker BG. Disease modifying therapies for relapsing multiple sclerosis. BMJ. 2016;354:i3518. https://doi.org/10.1136/bmj.i3518.
Solaro C, Ponzio M, Moran E, et al. The changing face of multiple sclerosis: prevalence and incidence in an aging population. Mult Scler. 2015;21:1244–50. https://doi.org/10.1177/1352458514561904.
Lunde HMB, Assmus J, Myhr KM, et al. Survival and cause of death in multiple sclerosis: a 60-year longitudinal population study. J Neurol Neurosurg Psychiatry. 2017;88:621–5. https://doi.org/10.1136/jnnp-2016-315238.
Marrie RA. Comorbidity in multiple sclerosis: implications for patient care. Nat Rev Neurol. 2017;13:375–82. https://doi.org/10.1038/nrneurol.2017.33.
Ranadive SM, Yan H, Weikert M, et al. Vascular dysfunction and physical activity in multiple sclerosis. Med Sci Sports Exerc. 2012;44(2):238–43. https://doi.org/10.1249/MSS.0b013e31822d7997.
Singh RB, Mengi SA, Xu YJ, et al. Pathogenesis of atherosclerosis: a multifactorial process. Exp Clin Cardiol. 2002;7:40–53.
Roshanisefat H, Bahmanyar S, Hillert J, et al. Multiple sclerosis clinical course and cardiovascular disease risk—Swedish cohort study. Eur J Neurol. 2014;21:1353–e88. https://doi.org/10.1111/ene.12518.
Christiansen CF. Risk of vascular disease in patients with multiple sclerosis: a review. Neurol Res. 2012;34(8):746–53. https://doi.org/10.1179/1743132812Y.0000000051.
Thormann A, Magyari M, Koch-Henriksen N, et al. Vascular comorbidities in multiple sclerosis: a nationwide study from Denmark. J Neurol. 2016;263:2484–93. https://doi.org/10.1007/s00415-016-8295-9.
Marie RA, Reider N, Cohen J, et al. A systematic review of incidence and prevalence of cardiac, cerebrovascular, and peripheral vascular disease in multiple sclerosis. Mult Scler. 2015;21:318–31. https://doi.org/10.1177/1352458514564485.
Manouchehrinia A, Tench CR, Maxted J, et al. Tobacco smoking and disability progression in multiple sclerosis: United Kingdom cohort study. Brain. 2013;136(Pt7):2298–304. https://doi.org/10.1093/brain/awt139.
Marrie RA, Rudick R, Horwitz R, et al. Vascular comorbidity is associated with more rapid disability progression in multiple sclerosis. Neurology. 2010;74:1041–7. https://doi.org/10.1212/WNL.0b013e3181d6b125.
Gisterå A, Hansson GK. The immunology of atherosclerosis. Nat Rev Nephrol. 2017;13:368–80. https://doi.org/10.1038/nrneph.2017.51.
Polman CH, Reingold SC, Banwell B, et al. Diagnostic criteria for multiple sclerosis: 2010 revisions to the McDonald criteria. Ann Neurol. 2011;69:292–302. https://doi.org/10.1002/ana.22366.
Thompson AJ, Banwell BL, Barkhof F, et al. Diagnosis of multiple sclerosis: 2017 revisions of the McDonald criteria. Lancet Neurol. 2018;17:162–73. https://doi.org/10.1016/S1474-4422(17)30470-2.
Craven TE, Ryu JE, Espeland MA, et al. Evaluation of the association between carotid artery atherosclerosis and coronary artery stenosis: a case control study. Circulation. 1990;82:1230–42. https://doi.org/10.1161/01.cir.82.4.1230.
Burdick L, Periti M, Salvaggio A, et al. Relation between carotid artery atherosclerosis and time on dialysis. A non-invasive study in vivo. Clin Nephrol. 1994;42:121–6.
London GM, Guerin AP, Marchais SJ, et al. Cardiac and arterial interactions in end-stage renal disease. Kidney Int. 1996;50:600–8. https://doi.org/10.1038/ki.1996.355.
Piggnoli P, Tremoli E, Poli A, et al. Intimal plus medial thickness of the arterial wall: a direct measurement with ultrasound imaging. Circulation. 1986;74:1399–406.
Kawagishi T, Nishizawa Y, Konishi T, et al. High-resolution B‑mode ultrasonography in evaluation of atherosclerosis in uremia. Kidney Int. 1995;48(3):820–6. https://doi.org/10.1038/ki.1995.356.
Savage T, Clarke AL, Giles M, et al. Calcified plaque is common in the carotid and femoral arteries of dialysis patients without clinical vascular disease. Nephrol Dial Transplant. 1998;13:2004–12. https://doi.org/10.1093/ndt/13.8.2004.
Pahor A, Hojs R, Gorenjak M, et al. Accelerated atherosclerosis in pre-menopausal female patients with rheumatoid arthritis. Rheumatol Int. 2006;27(2):119–23. https://doi.org/10.1007/s00296-006-0176-6.
Meyer-Moock S, Feng YS, Maeurer M, et al. Systematic literature review and validity evaluation of the Expanded Disability Status Scale (EDSS) and the Multiple Sclerosis Functional Composite (MSFC) in patients with multiple sclerosis. BMC Neurol. 2014;14:58. https://doi.org/10.1186/1471-2377-14-58.
Kurtzke JF. Rating neurologic impairment in multiple sclerosis: an expanded disability status scale. Neurology. 1983;5:580–3. https://doi.org/10.1212/wnl.33.11.
Cutter GR, Baier ML, Rudick RA, et al. Development of a multiple sclerosis functional composite as a clinical trial outcome measure. Brain. 1999;122:871–82. https://doi.org/10.1093/brain/122.5.871.
Fischer JS, Rudick RA, Cutter GR, Reingold SC. The Multiple Sclerosis Functional Composite Measure (MSFC): an integrated approach to MS clinical outcome. National MS Society Clinical Outcomes Assessment Task Force. Mult Scler. 1999;5(4):244–50. https://doi.org/10.1177/135245859900500409.
Piko N, Ekart R, Bevc S, et al. Atherosclerosis, epigenetic modifications, and arterial stiffness. Acta Medico-Biotechnica. 2017;10(2):10–7.
Simons PC, Algra A, Bots ML, et al. Common carotid intima-media thickness and arterial stiffness: indicators of cardiovascular risk in high-risk patients. The SMART Study (Second Manifestations of ARTerial disease). Circulation. 1999;100(9):951–7. https://doi.org/10.1161/01.cir.100.9.951.
Yuksel B, Koc P, Ozaydin Goksu E, et al. Is multiple sclerosis a risk factor for atherosclerosis? J Neuroradiol. 2019; https://doi.org/10.1016/j.neurad.2019.10.002.
Dagan A, Gringouz I, Kliers I, et al. Disability progression in multiple sclerosis is affected by the emergence of comorbid arterial hypertension. J Clin Neurol. 2016;12(3):345–50. https://doi.org/10.3988/jcn.2016.12.3.345.
Danesh J, Whincup P, Walker M, et al. Low grade inflammation and coronary heart disease: prospective study and updated meta-analyses. BMJ. 2000;321:199–204. https://doi.org/10.1136/bmj.321.7255.199.
Kirbis S, Breskvar UD, Sabovic M, et al. Inflammation markers in patients with coronary artery disease—comparison of intracoronary and systemic levels. Wien Klin Wochenschr. 2010;122:31–4. https://doi.org/10.1007/s00508-010-1343-z.
Ridker PM, Glynn RJ, Hennekens CH. C‑reactive protein adds to the predictive value of total and HDL cholesterol in determining risk of first myocardial infarction. Circulation. 1998;97:2007–11. https://doi.org/10.1161/01.cir.97.20.2007.
Alber HF, Suessenbacher A, Weidinger F. Die Rolle der Inflammation in der Pathophysiologie akuter Koronarsyndrome. Wien Klin Wochenschr. 2005;117(13/14):445–55. https://doi.org/10.1007/s00508-005-0399-7. The role of inflammation in the pathophysiology of acute coronary syndromes.
Kaneko R, Sawada S, Tokita A, et al. Serum cystatin C level is associated with carotid arterial wall elasticity in subjects with type 2 diabetes mellitus: a potential marker of early-stage atherosclerosis. Diabetes Res Clin Pract. 2018;139:43–51. https://doi.org/10.1016/j.diabres.2018.02.003.
Hartman J, Frishman W. Inflammation and atherosclerosis: a review of the role of Interleukin‑6 in the development of atherosclerosis and the potential for targeted drug therapy. Cardiol Rev. 2014;22(3):147–51. https://doi.org/10.1097/CRD.0000000000000021.
Acknowledgements
The study was funded by University Medical Centre Maribor.
Author information
Authors and Affiliations
Contributions
All authors contributed to the study conception and design. Material preparation, data collection and analysis were performed by Tomaž Omerzu, Jožef Magdič, Radovan Hojs, Uroš Potočnik, Mario Gorenjak and Tanja Hojs Fabjan. The first draft of the manuscript was written by Tomaž Omerzu and all authors commented on previous versions of the manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
T. Omerzu, J. Magdič, R. Hojs, U. Potočnik, M. Gorenjak and T.H. Fabjan declare that they have no competing interests.
Ethical standards
All procedures followed were in accordance with the ethical standards of the responsible committee on human experimentation (institutional and national) and with the Helsinki Declaration of 1975, as revised in 2008. Informed consent was obtained from all patients for being included in the study.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Omerzu, T., Magdič, J., Hojs, R. et al. Subclinical atherosclerosis in patients with relapsing-remitting multiple sclerosis. Wien Klin Wochenschr 136, 40–47 (2024). https://doi.org/10.1007/s00508-021-01862-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00508-021-01862-7