Summary
Background
Psoriasis is an autoimmune disease caused by overactivation of TH1 (Type 1 helper cells) and TH17 (T helper 17) cells. Overactivation of TH1 cells inhibits the activity of TH2 cells involved in type 1 allergies, therefore, psoriasis patients might be less affected by type 1 allergies. This study tested if allergies were less frequent in patients with moderate to severe than with mild psoriasis.
Methods
Psoriasis patients at the study site reported possible allergy symptoms and were tested for common allergens by skin prick test and IgE levels. Psoriasis was classified by PASI scores (Psoriasis Area and Severity Index) as mild (PASI <10) or moderate/severe (PASI ≥10). Patients without systemic therapy were assessed separately. Fisher’s exact test was used to test for differences.
Results
A total of 97 patients were included, 21 with mild and 76 with moderate to severe psoriasis. Allergies were found in 27.8%, most commonly against dust mites (23.4%) and grasses (18.1%). Allergies were found in 23.8% of the patients with mild vs. 29.0% allergic patients with moderate to severe psoriasis (P = 0.786). In patients without systemic medication, allergies were found in 21.1% vs. 35.3% (P = 0.463).
Conclusion
Allergy prevalence was not reduced in patients with moderate/severe psoriasis, and generally close to the prevalence in the general Austrian population (24%). The inhibiting effect of psoriasis on type 1 allergies was not confirmed.
Similar content being viewed by others
Introduction
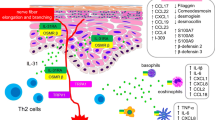
Psoriasis vulgaris is a chronic autoimmune skin disease characterized by keratinocyte hyperproliferation and chronic inflammation [1], which affects 1–3% of the world population [2]. Although the etiology is not completely understood, the crucial role of genetic predisposition, including PSORS-1 (psoriasis susceptiblity 1 locus), in combination with environmental factors is generally acknowledged [3, 4]. On the physiological level, psoriasis vulgaris is caused by autoantigens, such as LL37 (cathelicidin), ADAMTSL5 (thrombospondin type 1 motif-like 5) and PLA2G4D (phospholipase A2 group IVD) which induce T cell activation which, at least in the case of ADAMTSL5, release cytokines including but not restricted to interleukin 17 (IL-17), IL-26, IL-29 or tumour necrosis factor alpha (TNFα). These cytokines, in turn, activate signal transducers, such as STAT1, NFκB and C/EBP-β/γ in keratinocytes and other cells of the epidermis, leading to auto-inflammation, which involves the activation of TH17 and also TH22 cells. Furthermore, IL-17 induces epidermal hyperplasia [5, 6]. Together, inflammation and keratinocyte proliferation lead to the characteristic symptoms of reddening, desquamation, itching and hardening of the skin. Disease intensity depends on the severity of lesions and the area affected, with the psoriasis area and severity index (PASI) as a well-established tool to quantify disease intensity [7].
Allergies, such as allergic asthma, atopic dermatitis, rhinoconjunctivitis, food allergies and urticaria affect up to one third of the population in Germany [8] and Austria [9], with considerably lower rates in less developed countries. This study was restricted to immunoglobulin E (IgE)-mediated allergies (type 1), where T cells are involved as in psoriasis, although the underlying mechanism is quite different. Sensitization occurs when harmless haptens and other compounds bound to proteins are presented by antigen-presenting cells and trigger the transformation of naïve CD4+ TH0 cells to TH2 cells via the cytokines IL‑4 and IL‑6. Subsequently, TH2 cells stimulate IgE production by B cells via other cytokines and the CD40 ligand. This, in turn, leads to a wide range of reactions mediated by mast cells and basophils [10] which finally causes the typical allergic symptoms.
The various types of T cells do not act independently of each other. Up-regulation of TH1 cells, as seen in psoriasis or many infections may lead to down-regulation of TH2 cells involved in type 1 allergy [11, 12]. In more detail, IFN-gamma (Interferon type II) inhibits Th2 proliferation through an IL-1-dependent mechanism [13]. Therefore, it was suggested that active diseases involving TH1 cell activation might offer protection against undesired up-regulation of TH2 (Type 2 helper T) cells and that, in consequence, very few patients would be affected by both psoriasis and type 1 allergies [14]. Although this hypothesis is in accordance with our recent understanding of the regulation of the immune system, empirical data do not provide sufficient support [15]. Therefore, it is suggested that allergies are not prevented by psoriasis vulgaris in general, but that allergies would become less frequent with increasing psoriasis activity. This modified hypothesis was tested in psoriasis patients in Austria.
Material and methods
Occurrence of type 1 allergies was compared between patients with mild or moderate/severe psoriasis vulgaris within the framework of a prospective cohort study as approved by the ethics committee of the City of Vienna (vote EK-15-008-0415). Since this study focussed exclusively on the comparison of different severities of the same disease no symptom-free control group was required. Inclusion criteria were: (1) ≥18 years of age, (2) written informed consent and (3) active psoriasis vulgaris. HIV positive patients were excluded since the immune system might have been influenced by the infection. Eligible patients were recruited at the department of dermatology of the Hospital Hietzing from July 2015 to January 2017. No formal calculation of the sample size took place since this study primarily aimed at the generation of hypotheses for future trials.
After signing the informed consent form, patients filled in a study-specific questionnaire (provided as supplemental material) with demographic and disease data, a skin prick test was conducted and a blood sample was taken during of a single visit. Psoriasis activity was assessed by PASI scores according to the European consensus [16]. The PASI scores were retrieved from the medical records, since most patients were under treatment at the study visit and therefore exhibited greatly diminished PASI scores. Patients with PASI <10 without systemic therapy were classified as mild, and PASI ≥10 were classified as moderate/severe. Disease duration, previous and concomitant medication and concomitant psoriasis arthritis were assessed by the aforementioned study questionnaire.
Allergic sensitization was determined by a skin prick test [17] conducted at lesion-free skin of the forearm. Commercial solutions (ALK-Abello® Allergie Service, Linz, Austria) of the following antigens were used: birch (Betula sp. L.), grasses (Poaceae barnhart), dust mites (Dermatophagoides spp. bogdanov), mugwort (Artemisia spp. L.), ragweed (Ambrosia artemisiifolia L.), molds (Alternaria spp. nees, Cladosporum herbarum link) and dander of cats and dogs, supplemented by 10 mg/ml histamine dihydrochloride as positive and 0.9% sodium chloride as negative controls. Wheals ≥3 mm after 20 min were classified as positive [18]. Furthermore, specific and total serum immunoglobulin E (IgE) [19] were determined by the Immulite 2000 3 g AllergyTM—Specific IgE Universal Kit® (Siemens Healthcare Diagnostics, Erlangen, Germany). The kit detected sensitization for the following common antigens: Timothy grass (Phleum pratense L.), rye (Secale cereale L.), birch (Betula spp. L.), mugwort (Artemisia spp. L.), dust mites (Dermatophagoides spp. bogdanov), Cladosporum herbarum link and dander of cats and dogs. A patient was classified as sensitized if either the result of the skin prick test was positive or if the IgE kit revealed a value >0.35 kU/l according to the standard setting of the analytical device (Immulite 2000 3 gAllergyTM—specific IgE Universal Kit, Siemens Healthcare Diagnostics, Erlangen, Germany), in which case a more detailed analysis was carried out. For total IgE, values ≥87 IU/l were considered as increased. Clinical status was assessed by the aforementioned study questionnaire asking for known diagnoses as well as for disease history and specific symptoms (sneezing, runny nose, burning eyes etc.). A patient was classified as allergic if sensitized and reported clinical symptoms in accordance with the sensitization. Clinical symptoms were considered as confirmed if they were in accordance with sensitization data. In the case of lacking data, patients were assessed as not allergic/not sensitized (one patient affected).
Numeric data were summarized by arithmetic mean (μ), standard deviation (SD), median, quartiles and sample size (n). In the running text, μ ± SD is shown. Categorical data are summarized by absolute and relative frequencies. The subgroups with mild and moderate/severe psoriasis were compared by Fisher’s exact test. The potential interaction of systemic psoriasis treatment and allergies was assessed by a separate analysis of a subset of patients without systemic therapy (methotrexate, fumaric acid or biologicals). Analyses were carried out by Stata 14.2 (Stata Corporation, College Station, TX, USA).
Results
From July 2015 to January 2017 a total of 97 patients were included (Table 1), 21 patients (21.6%) were assigned to the PASI <10, and 76 (78.4%) to the PASI ≥10 groups. The mean age was 53.2 ± 13.5 years and 56.7% were male. Demographic differences between the two treatment groups were negligible. Systemic treatment was common (77.6%) in the PASI ≥10 group but also prescribed to 2 patients with PASI <10 due to genital involvement. No UV A phototherapy was reported as part of the medical history. Topical treatment was more common in the PASI <10 group (85.7% vs. 22.4%) and one patient with mild disease activity did not receive any medication. Supplementary Table 1 shows the reported medications.
The study questionnaire was filled in completely by 93 (95.9%), and incompletely by 2 patients (2.1%); for the remaining patients, no questionnaire data were available. In this questionnaire, symptoms which might have been caused by an allergy were reported by 52.4% in the PASI <10 group, and by 75.0% in the PASI ≥10 group (P = 0.060); however, typical allergic symptoms, such as asthma (5.0% vs. 6.9%; P = 1.000) and rhinoconjunctivitis (10.0% vs. 21.6%; P = 0.344) were diagnosed in considerably less patients.
The skin prick test indicated sensitization in >10% of the patients for the following allergens: Betulus pollen (20.0% vs. 10.8%; P = 0.275), grass pollen (20.0% vs. 17.6%; P = 0.753) and dust mites (20.0% vs. 24.3%; P = 0.775). At least one positive reaction against any of the allergens was found in 45.0% of the PASI <10 group, and in 36.5% of the PASI ≥10 group (P = 0.605). In the total patient population, 16.5% reacted to 1 allergen, 10.3% to 2, and 10.3% to 3 or more. Very similar results were found by using IgE data. Again, >10% of the study population were sensitized against the tested grasses (Phleum: 14.3% vs. 17.6%; P = 1.000. Secale: 9.5% vs. 14.9%; P = 0.726), against Betulus pollen (19.1% vs. 9.5%; P = 0.253) and against dust mites (9.5% vs. 13.5%; P = 1.000). Any increased levels of specific IgE were detected in 23.8% of the PASI <10 group, and in 25.7% of the PASI ≥10 group (P = 1.000). The majority of enhanced IgE levels were classified as I–V (i.e., 0.35–100 kU/l), with one patient (PASI ≥10) exhibiting dust mite allergy graded VI (i.e., >100 kU/l), 6.2% showed enhanced IgE values for 1 allergen, 7.2% for 2, and 11.3 for 3 or more. Increased levels of total IgE were found in 19.1% of the PASI <10, and in 34.7% of the PASI ≥10 groups. Mean total IgE levels were 73.8 ± 113.3 IU/l in the PASI <10, and 137.5 ≥ 236.7 IU/l in the PASI ±10 groups. Both differences were not significant, with P = 0.196 and P = 0.142, respectively.
In 68.0% of the patients the results of the skin prick test coincided perfectly with the specific IgE analysis. In 5.2%, a reconciliation of the two methods was made impossible by lacking data. In 21.6%, a positive skin prick test was not accompanied by enhanced IgE, whereas in 6.2% a negative skin prick test coincided with enhanced IgE values (percentages do not sum up to 100%). Detailed results of the skin prick test and the IgE assessment are shown in Supplementary Table 2. Combining data from the skin prick test and the IgE assessment, 47.6% of the PASI <10 group was assessed as sensitized, compared to 37.3% of the PASI ≥10 group (P = 0.453). After reconciliation with the data on clinical symptoms, 23.8% and 29.0%, respectively, were classified as allergic (P = 0.786; 27.8% for the total population with a 95% confidence interval of 19.2–37.9%), 23.8% of the PASI <10 group and 7.9% of the PASI ≥10 group were sensitized but did not exhibit allergies (P = 0.056). Increased total IgE values were found in 66.7% of allergic patients and in 17.4% of the non-allergic patients (P < 0.001).
The population without systemic treatment contained 36 patients, with almost equal proportions (19 vs. 17) from the PASI <10 and the PASI ≥10 groups. In this subset, results were very similar to the total patient population. Allergic symptoms were reported by 47.4% vs. 64.7% (P = 0.335). A positive skin prick test was found in 44.4% vs. 41.2% (P = 1.000) and enhanced IgE in 21.1% vs. 29.4% (P = 0.706), resulting in sensitization in 42.1% vs. 41.2% (P = 1.000). Reconciliation of sensitization and clinical symptoms resulted in 21.1% of the PASI <10 group being classified as allergic, compared to 35.3% of the PASI ≥10 group (P = 0.463; 27.7% with a 95% confidence interval of 14.2–45.2%). Increased levels of total IgE were found in 21.1% vs. 47.1% (P = 0.158), with mean levels of 76.4 ± 118.8 vs. 293.4 ± 431.3 IU/l (P = 0.121). Details on this subset are shown in Table 2, supplementary Table 2 and supplementary Table 3.
Discussion
Interpretation
The data presented here can be summarized by the following key results: (1) IgE-mediated allergies were common in psoriasis patients. (2) Sensitization and allergies seem to be equally abundant in patients with mild or with moderate/severe psoriasis.
The Austrian population in general shows a high prevalence of allergies, with up to one third reporting allergic symptoms [9], 24% suffering from a diagnosed allergy [20], and 12.7% exhibiting polysensitization, i.e., sensitization against three or more allergens [21]. The exact percentage of affected subjects at the time point of the study (i.e., July 2015 to January 2017) is only roughly known, since some studies described an ongoing increase in allergic diseases [22,23,24], whereas other did not observe recent changes [25, 26]. In this study, 70.1% reported allergic symptoms, 27.8% received a diagnosis of allergy and, according to the method, 10.3–11.3% exhibiting polysensitization. Among females, the patients of this studies represented the total population almost perfectly (26.2% vs. 27%) with respect to allergy prevalence, whereas in males, a slight increase was found (29.1 vs. 22%). As the two Austrian studies cited above [20, 24] both suggest an increase in allergy prevalence, comparisons between study and published results remain difficult; however, all available estimates for allergy prevalence in Austria fall well within the 95% confidence interval for allergy prevalence found in this study. Thus, the prevalence of allergy and polysensitization seem to be very similar in the participants and the general population, whereas self-reported allergic symptoms were more common among the participants. The difference concerning self-reported symptoms may have been caused by the nature of the study questionnaire which contained some questions of a general nature. In any case, the collected data do not indicate that allergic diseases might be less frequent in psoriasis patients compared to the general population in Austria. This finding is in good accordance with recent research: hay fever, asthma, and sensitization to common aeroallergens, as also tested in this study, were not significantly different in psoriasis patients and a control group [15]. Pigatto found allergic diseases in 21% of a sample of 140 psoriasis patients [27], which is close to the percentage retrieved by this study. Concerning IgE, one study [28] found increased values in psoriasis patients compared to the control, whereas another one using a far larger sample [29] found no difference in IgE levels.
Thus, mutual inhibition of psoriasis and allergy appears increasingly improbable; however, Rabin and Levinson suggested [30] that allergic diseases may suppress the severity but not necessarily the onset of autoimmune diseases like psoriasisbut no supportive evidence for this hypothesis could be found as well. Not only the frequency of allergic diseases did not differ between patients with mild and moderate/severe psoriasis, but differences were also inconspicuous and insignificant for all single and combined endpoints, including the reaction towards the tested allergens, clinical symptoms and sensitization. In the present study, borderline insignificant differences were found for patient-reported allergy symptoms (P = 0.060), for confirmed allergic symptoms (P = 0.080) and for sensitization in the absence of allergic symptoms (P = 0.056). These differences may indicate not a decrease, but even an increase of allergies in patients with more severe psoriasis. This observation, if confirmed, could inspire new hypotheses on the relationship between autoimmune diseases and allergies; however, these borderline insignificant results should be interpreted with greatest care, since they are based on patient-reported data not supported by laboratory analysis. Furthermore, patients suffering from high disease activity may be inclined to observe and report symptoms of any kind in more detail than patients who have less reasons to be concerned about their health. None of the possible interpretations, however, point towards reduced allergies in patients with higher psoriasis activity. These three parameters were not measured directly, but calculated based on the study questionnaire, where possible limitations have been described above.
Furthermore, increased total IgE levels were significantly more frequent in allergic patients, but borderline insignificantly (P = 0.196) also more frequent in patients with moderate/severe psoriasis. Such increased levels are common in psoriasis patients [31]; the present study was not designed to identify the separate influence of allergy and psoriasis on IgE levels.
The presence of an autoimmune disease is not the only parameter which might influence the prevalence of allergies. Most patients with moderate/severe psoriasis were exposed to systemic immunosuppressive treatment, whereas such treatment was administered only exceptionally in mild psoriasis. To the best of our knowledge, the interaction of systemic psoriasis treatment and allergies has not been studied so far. Immunosuppressive treatment administered subsequently to transplantations, however, has been shown to stimulate the emergence of allergies [32]. Although the available data on patients receiving transplants are still inconclusive, it may be suggested that patients exposed to immunosuppressive treatment might be more prone to allergic diseases [33], thereby masking the allergy-suppressing effect of severe psoriasis. In order to test this hypothesis, a subset of patients not exposed to systemic treatment was analyzed as well. The results, however, were very similar to those achieved from the complete study population. Differences between mild and moderate to severe psoriasis were even less significant. Especially the borderline non-significant differences concerning patient reported allergic symptoms and patients showing only sensitization became far less significant (P = 0.335 and P = 0.342, respectively). Thus, the inconspicuous differences between patients with mild and moderate/severe psoriasis cannot be explained by exposure to systemic treatment.
Limitations
This study tested for allergic reaction to common antigens which, indeed, cause the majority of allergic diseases. Rare [34] and new [35] allergies, however, were not tested for and patients with missing data were assessed as non-allergic. The true percentage of allergic patients might therefore have been higher than the 27.8% reported here. This, however, rather supports the main finding of this study that the prevalence of allergies not reduced in psoriasis patients.
Within the total study population, patients with mild psoriasis were significantly underrepresented due to problems related to recruitment; however, this resulted in virtually equally sized groups within the subset of patients without systemic treatment. Due to the widespread and predominantly successful use of systemic treatments, no meaningful PASI scores were available for the time point of the study. Thus, it was not possible to discriminate between patients with active and chronic plaque-type psoriasis, which may differ with respect to allergy prevalence [36]. The results of the skin prick test and of the IgE analysis coincided only in 68.0%. Discrepancies between IgE analyses and clinically diagnosed allergies were also described in the literature [37, 38]; thus, our strategy to classify patients as sensitized if either the skin prick test or IgE levels yielded a positive result may have led to an overestimation of sensitized patients.
Conclusion
-
Prevalence of type 1 allergy in patients with psoriasis is similar to the general population in Austria and differs little from the results of other studies. Therefore, psoriasis seems to have little effect on allergies.
-
Between patients with mild and moderate to severe psoriasis, no significant differences are found with respect to allergic symptoms, sensitization and diagnosed type 1allergy.
-
These results are confirmed for the subset not exposed to systemic psoriasis treatment. Only few data are available on the interaction of immunosuppressives and allergies; however, our results do not indicate that the occurrence of allergies in patients with moderate/severe psoriasis is caused by the treatment.
-
The hypothetical inhibiting effect of psoriasis on type 1 allergies was not confirmed.
References
Cited Literature
Patel AB, Tsilioni I, Weng Z, Theoharides TC. TNF stimulates IL‑6, CXCL8 and VEGF secretion from human keratinocytes via activation of mTOR, inhibited by tetramethoxyluteolin. Exp Dermatol. 2018;27:135–43. https://doi.org/10.1111/exd.13461.
Mansouri Y, Goldenberg G. Biologic safety in psoriasis: review of long-term safety data. J Clin Aesthet Dermatol. 2015;8:30–42.
Blumenthal-Barby E. Charakterisierung einer humanen endogenen retroviralen dUTPase als Suszeptibilitätsgen für Psoriasis vulgaris: [Characterization of a human endogenous retroviral dUTPase as susceptibility gene for psoriasis vulgaris] [PhD Thesis]. Berlin: Universitätsmedizin Berlin; 2012.
Nair RP, Stuart PE, Nistor I, Hiremagalore R, Chia NVC, Jenisch S, et al. Sequence and haplotype analysis supports HLA‑C as the psoriasis susceptibility 1 gene. Am J Hum Genet. 2006;78:827–51. https://doi.org/10.1086/503821.
Guttman-Yassky E, Krueger JG. Atopic dermatitis and psoriasis: two different immune diseases or one spectrum? Curr Opin Immunol. 2017;48:68–73. https://doi.org/10.1016/j.coi.2017.08.008.
Chiricozzi A, Suárez-Fariñas M, Fuentes-Duculan J, Cueto I, Li K, Tian S, et al. Increased expression of interleukin-17 pathway genes in nonlesional skin of moderate-to-severe psoriasis vulgaris. Br J Dermatol. 2016;174:136–45. https://doi.org/10.1111/bjd.14034.
Kreft S, Kreft M, Resman A, Marko P, Kreft KZ. Computer-aided measurement of psoriatic lesion area in a multicenter clinical trial—comparison to physician’s estimations. J Dermatol Sci. 2006;44:21–7. https://doi.org/10.1016/j.jdermsci.2006.05.006.
Langen U, Schmitz R, Steppuhn H. Häufigkeit allergischer Erkrankungen in Deutschland: Ergebnisse der Studie zur Gesundheit Erwachsener in Deutschland (DEGS1). Bundesgesundheitsblatt Gesundheitsforschung Gesundheitsschutz. 2013;56:698–706. https://doi.org/10.1007/s00103-012-1652-7.
Maucher J. Erster österreichischer Allergiebericht: Einschätzung und Realität unterschiedlich. Osterr Arzteztg. 2006;11:56–7.
Averbeck M, Gebhardt C, Emmrich F, Treudler R, Simon JC. Immunologic principles of allergic disease. J Dtsch Dermatol Ges. 2007;5:1015–28. https://doi.org/10.1111/j.1610-0387.2007.06538.x.
Benn CS, Bendixen M, Krause TG, Olesen AB. Questionable coexistence of T(H)1- and T(H)2-related diseases. J Allergy Clin Immunol. 2002;110:328–9. author reply 329–30.
Graham-Rowe D. Lifestyle: When allergies got west. Nature. 2011;479:S2–S4.
Oriss TB, McCarthy SA, Morel BF, Campana MA, Morel PA. Crossregulation between T helper cell (Th)1 and Th2: Inhibition of Th2 proliferation by IFN-gamma involves interference with IL‑1. J Immunol. 1997;158:3666–72.
Christophers E. Psoriasis—epidemiology and clinical spectrum. Clin Exp Dermatol. 2001;26:314–20.
Hajdarbegovic E, Nijsten T, Westgeest A, Habraken F, Hollestein L, Thio B. Decreased prevalence of atopic features in patients with psoriatic arthritis, but not in psoriasis vulgaris. J Am Acad Dermatol. 2013;68:270–7. https://doi.org/10.1016/j.jaad.2012.07.018.
Mrowietz U, Kragballe K, Reich K, Spuls P, Griffiths CE, Nast A, et al. Definition of treatment goals for moderate to severe psoriasis: A European consensus. Arch Dermatol Res. 2011;303:1–10.
Ruëff F, Bergmann K‑C, Brockow K, Fuchs T, Grübl A, Jung K, et al. Hauttests zur Diagnostik von allergischen Soforttypreaktionen: Leitlinie der Deutschen Gesellschaft für Allergologie und klinischen Immunologie (DGAKI). Pneumologie. 2011;65:484–95.
Bernstein IL, Li JT, Bernstein DI, Hamilton R, Spector SL, Tan R, et al. Allergy diagnostic testing: An updated practice parameter. Ann Allergy Asthma Immunol. 2008;100:S1–S148.
Kleine-Tebbe J, Ballmer-Weber B, Beyer K, Erdmann S, Fuchs T, Henzgen M, et al. In-vitro-Diagnostik und molekulare Grundlagen von IgE-vermittelten Nahrungsmittelallergien: Leitlinie der Deutschen Gesellschaft für Allergologie und klinische Immunologie (DGAKI), des Ärzteverbandes Deutscher Allergologen (ÄDA), der Gesellschaft für Pädiatrische Allergologie und Umweltmedizin (GPA), der Österreichischen Gesellschaft für Allergologie und Immunologie (ÖGAI) und der Schweizerischen Gesellschaft für Allergologie und Immunologie (SGAI). Allergo J. 2009;18:132–46.
Griebler R, Winkler P, Gaiswinkler S, Delcour J, Jusaszovich B, Nowotny M, et al. Österreichischer Gesundheitsbericht 2016 [Austrian health report 2016]. 2017. Berichtszeitraum 2005–2014/15.
Dittmar D, Uter W, Bauer A, Fortina AB, Bircher AJ, Czarnecka-Operacz M, et al. European Surveillance System on Contact Allergies (ESSCA): polysensitization, 2009–2014. Contact Derm. 2018;78:373–85. https://doi.org/10.1111/cod.12966.
Österreichische Gesellschaft für Pneumologie.. Klimawandel verstärkt Risiko für Allergien und Asthma: Klimawandel und die Folgen für die Lungengesundheit – Ergebnisse aus der LEAD-Studie. Wien: ÖGP; 2017.
Asher MI, Montefort S, Björkstén B, Lai CKW, Strachan DP, Weiland SK, et al. Worldwide time trends in the prevalence of symptoms of asthma, allergic rhinoconjunctivitis, and eczema in childhood: ISAAC Phases One and Three repeat multicountry cross-sectional surveys. Lancet. 2006;368:733–43. https://doi.org/10.1016/S0140-6736(06)69283-0.
Schernhammer ES, Vutuc C, Waldhör T, Haidinger G. Time trends of the prevalence of asthma and allergic disease in Austrian children. Pediatr Allergy Immunol. 2008;19:125–31. https://doi.org/10.1111/j.1399-3038.2007.00597.x.
Bjerg A, Sandström T, Lundbäck B, Rönmark E. Time trends in asthma and wheeze in Swedish children 1996–2006: prevalence and risk factors by sex. Allergy. 2010;65:48–55. https://doi.org/10.1111/j.1398-9995.2009.02105.x.
Zöllner IK, Weiland SK, Piechotowski I, Gabrio T, von Mutius E, Link B, et al. No increase in the prevalence of asthma, allergies, and atopic sensitisation among children in Germany: 1992-2001. Thorax. 2005;60:545–8. https://doi.org/10.1136/thx.2004.029561.
Pigatto PD. Atopy and contact sensitization in psoriasis. Acta Derm Venereol Suppl (Stockh). 2000;80:19–20.
Chen C, Zheng X, Duan Q, Yang P, Zheng Y. High serum IgE concentration in patients with psoriasis. Clin Res Dermatol. 2017;4:1–4.
Skaaby T, Husemoen LLN, Thuesen BH, Fenger RV, Linneberg A. Specific IgE positivity against inhalant allergens and development of autoimmune disease. Autoimmunity. 2015;48:282–8. https://doi.org/10.3109/08916934.2014.1003640.
Rabin RL, Levinson AI. The nexus between atopic disease and autoimmunity: a review of the epidemiological and mechanistic literature. Clin Exp Immunol. 2008;153:19–30. https://doi.org/10.1111/j.1365-2249.2008.03679.x.
Yan K‑X, Huang Q, Fang X, Zhang Z‑H, Han L, Gadaldi K, et al. IgE and FcεRI are highly expressed on innate cells in psoriasis. Br J Dermatol. 2016;175:122–33. https://doi.org/10.1111/bjd.14459.
Gruber S, Tiringer K, Dehlink E, Eiwegger T, Mayer E, Konstantin H, et al. Allergic sensitization in kidney-transplanted patients prevails under tacrolimus treatment. Clin Exp Allergy. 2011;41:1125–32. https://doi.org/10.1111/j.1365-2222.2011.03761.x.
Ozdemir O. New developments in transplant-acquired allergies. World J Transplant. 2013;3:30–5. https://doi.org/10.5500/wjt.v3.i3.30.
Bandelier C, Leimgruber A, Wassenberg J, Bart PA, Spertini F. Allergies alimentaires rares. Rev Med Suisse. 2008;4:1024–9.
Wassenberg J, Bart PA. Modern nutrition and development of new allergies. Rev Med Suisse. 2007;3:1032–7.
Schernhammer ES, Vutuc C, Waldhör T, Haidinger G. Time trends of the prevalence of asthma and allergic disease in Austrian children. Pediatric Allergy and Immunology. 2008;19(2):125–131
de Vos G, Nazari R, Ferastraoaru D, Parikh P, Geliebter R, Pichardo Y, et al. Discordance between aeroallergen specific serum IgE and skin testing in children younger than 4 years. Ann Allergy Asthma Immunol. 2013;110:438–43. https://doi.org/10.1016/j.anai.2013.03.006.
Bergmann K‑C. Current status of allergy prevalence in Germany: Position paper of the Environmental Medicine Commission of the Robert Koch Institute. 2016.
Essl A. Vergleich der Prävalenz von IGE-vermittelten Sensibilisierungen und Allergien bei Patienten mit leichter (PASO 〈 10) und schwerer (PASI 〉 10) Psoriasis vulgaris: [Comparison of the prevalence of IgE mediated sensibilisation and allergy in patients with mild (PASI 〈 10) and severe (PASI 〉 10) psoriasis vulgaris] [Thesis]. Vienna: Medical University Vienna; 2018.
Further Reading
Eyerich S, Onken AT, Weidinger S, Franke A, Nasorri F, Pennino D, et al. Mutual antagonism of T cells causing psoriasis and atopic eczema. N Engl J Med. 2011;365:231–8. https://doi.org/10.1056/NEJMoa1104200.
Acknowledgements
These results were first presented as A. Essl’s thesis [39], supervised by D. Loader and P. Sator. Writing assistance was provided by W. Adlassnig (CW Research and Management GmbH).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
A. Essl, D. Loader, R. Feldmann, A. Steiner, and P. Sator declare that they have no competing interests.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Essl, A., Loader, D., Feldmann, R. et al. Psoriasis and IgE-mediated allergy: correlation or mutual inhibition?. Wien Klin Wochenschr 133, 997–1003 (2021). https://doi.org/10.1007/s00508-020-01683-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00508-020-01683-0