Summary
Background
Tuberculosis (TB) has become a rare disease in developed countries. Austria is a low incidence country for TB with an incidence rate of 7.2/100,000 in 2016. The incidence of TB has shown a constant decline in Austria from 2008 (9.8/100,000) to 2015 (6.7/100,000) but recently stagnated in 2016 (7.2/100,000). In recent years migration to Austria from countries with high TB incidence rates has increased. Therefore, this study aimed to describe the recent epidemiology of childhood TB in Vienna.
Methods
Data of pediatric patients with active TB infections, who were hospitalized for further investigations or isolation precautions between 2010 and 2016 at the Wilhelminenspital, Austria’s reference center for childhood tuberculosis, were retrospectively analyzed. Demographic and clinical data (symptoms, microbiology, radiology, immunology) were collected, compared and evaluated.
Results
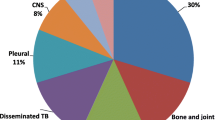
A total of 127 patients with active tuberculosis were included in the study. The number of admissions varied between n = 7 in 2010 and n = 26 in 2016. There were two age peaks of infected children (0–5 years: n = 41 and 15–18 years: n = 45). In 35% of the cases one parent had active TB and was suspected to be the index case. In 36% the source of infection remained unknown. Compared to young children (<5 years), adolescents (15–18 years) showed proportionally more TB-related symptoms, such as cough (41% vs. 24%), fever (15% vs. 14%) and weight loss (22% vs. 0%). At the time of admission 51% of the young children and 33% of the adolescents were free of symptoms. Intrathoracic disease was found in 80.8%, extrathoracic disease in 19.2% and 11% of the cases were tuberculous lymphadenitis. Of the patients with intrathoracic TB 54% (n = 64) had a positive microbiological result (auramine staining, bacteriological culture, PCR). In young children hilar lymphadenopathy was the most frequent radiological finding (50%), whereas in adolescents lung infiltrates were most common (36%). The sensitivity of interferon-gamma release assays (IGRA) was 0.94 compared to 0.88 of the tuberculin skin test (TST). Both test methods showed moderate concordance (ϕ-coefficient = 0.48).
Conclusion
A high number of asymptomatic children and adolescents with active TB were observed, which underlines the importance of efficient screening measures. Thorough history taking in all patients with TB is essential to maximize the effect of contact tracing. Overall, infection rates remained consistently low during the observation period.



Similar content being viewed by others
References
Global tuberculosis report 2017. Geneva: World Health Organization; 2017. Licence: CC BY-NCSA 3.0 IGO.
Schaberg T, Bauer T, Castell S, Dalhoff K, Detjen A, Diel R, et al. Recommendations for therapy, chemoprevention and chemoprophylaxis of tuberculosis in adults and children. German Central Committee against Tuberculosis (DZK), German Respiratory Society (DGP). Pneumol Stuttg Ger. 2012;66(3):133–71. Mar.
Hoffmann H, et al. Tuberkulosediagnostik mit modernen Mitteln. 1st ed. Bremen: UNI-MED Verlag AG; 2015.
Kumar MK, Kumar P, Singh A. Recent advances in the diagnosis and treatment of childhood tuberculosis. J Nat Sci Biol Med. 2015;6(2):314–20.
Marais BJ, Gie RP, Schaaf HS, Hesseling AC, Obihara CC, Starke JJ, et al. The natural history of childhood intra-thoracic tuberculosis: a critical review of literature from the pre-chemotherapy era. Int J Tuberc Lung Dis. 2004;8(4):392–402. Apr.
Cruz AT, Starke JR. Safety and completion of a 4-month course of rifampicin for latent tuberculous infection in children. Int J Tuberc Lung Dis. 2014;18(9):1057–61.
Spyridis NP, Spyridis PG, Gelesme A, Sypsa V, Valianatou M, Metsou F, et al. The effectiveness of a 9-month regimen of isoniazid alone versus 3‑ and 4‑month regimens of isoniazid plus rifampin for treatment of latent tuberculosis infection in children: results of an 11-year randomized study. Clin Infect Dis. 2007;45(6):715–22.
Diallo T, Adjobimey M, Ruslami R, Trajman A, Sow O, Obeng Baah J, et al. Safety and side effects of rifampin versus isoniazid in children. N Engl J Med. 2018;2;379(5):454–63.
Österreichische Agentur für Gesundheits und Ernährungssicherheit, Indra, Alexander, Schmid, Daniela. Nationale Referenzzentrale für Tuberkulose, Jahresbericht 2015, Wien.
Marais BJ, Gie RP, Schaaf HS, Beyers N, Donald PR, Starke JR. Childhood pulmonary tuberculosis: old wisdom and new challenges. Am J Respir Crit Care Med. 2006;173(10):1078–90.
Mulenga H, Tameris MD, Luabeya KKA, Geldenhuys H, Scriba TJ, Hussey GD, et al. The role of clinical symptoms in the diagnosis of Intrathoracic tuberculosis in young children. Pediatr Infect Dis J. 2015;34(11):1157.
Esposito S. Tuberculosis in children. Mediterr J Hematol Infect Dis. 2013;5(1):2013064.
Roya-Pabon CL, Perez-Velez CM. Tuberculosis exposure, infection and disease in children: a systematic diagnostic approach. Pneumonia. 2016;8(1) https://doi.org/10.1186/s41479-016-0023-9.
Nachiappan AC, Rahbar K, Shi X, Guy ES, Mortani Barbosa EJ, Shroff GS, et al. Pulmonary tuberculosis: role of radiology in diagnosis and management. Radiographics. 2017;37(1):52–72.
Heemskerk D, Caws M, Marais B, Farrar J. Tuberculosis in adults and children. Wellcome Trust–Funded Monographs and Book Chapters. London: Springer; 2015. http://www.ncbi.nlm.nih.gov/books/NBK344402/.
Knappik M, Schönfeld N, Günther A, Bergmann T, Magdorf K, Rüssmann H, et al. Interferon-gamma release assays for hospital-based tuberculosis diagnostics in children and adolescents—a retrospective analysis. Pneumol Stuttg Ger. 2012;66(4):207–11.
Pavić I, Topić RZ, Raos M, Aberle N, Dodig S. Interferon-γ release assay for the diagnosis of latent tuberculosis in children younger than 5 years of age. Pediatr Infect Dis J. 2011;30(10):866–70.
Bergamini BM, Losi M, Vaienti F, D’Amico R, Meccugni B, Meacci M, et al. Performance of commercial blood tests for the diagnosis of latent tuberculosis infection in children and adolescents. Pediatrics. 2009;123(3):e419–e24.
Feiterna-Sperling C, Brinkmann F, Adamczick C, Ahrens F, Barker M, Berger C, et al. S2k-Leitlinie zur Diagnostik, Prävention und Therapie der Tuberkulose im Kindes- und Jugendalter: Eine Leitlinie unter Federführung der Deutschen Gesellschaft für Pädiatrische Infektiologie (DGPI) e. V. Pneumologie. 2017;71(10):629–80.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
M. Unterweger, F. Götzinger, M. Bogyi, A. Zacharasiewicz, C. Mädel, K. Tiringer, M. Reinweber, and T. Frischer declare that they have no competing interests.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Unterweger, M., Götzinger, F., Bogyi, M. et al. Childhood tuberculosis in Vienna between 2010 and 2016. Wien Klin Wochenschr 131, 356–361 (2019). https://doi.org/10.1007/s00508-019-1510-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00508-019-1510-9