Summary
Objective
To define reliable Doppler parameters in mural arteries of affected bowel loops for quantitative assessment of Crohn disease (CD) activity in pediatric population and compare Doppler parameters with Pediatric Crohn Disease Activity Index (PCDAI).
Patients and methods
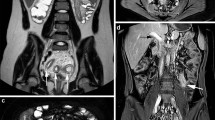
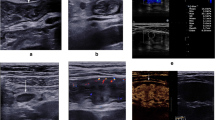
Thirty-four pediatric patients (7 with inactive, 27 with active disease of different severity; 13 male and 21 female; mean age 13; range 7–18) with CD were prospectively evaluated by Doppler ultrasound (DUS) of affected bowel segments. Using semiquantitative color and power Doppler assessment of vascularization of thickened bowel wall and mesentery, patients were divided in four grades. Spectral measurements (peak systolic velocity (PSV), end diastolic velocity (EDV), resistance index (RI)) of mural arteries were compared with PCDAI.
Results
There was a significant difference in distribution of semiquantitative color values between inactive and active group. PSV and EDV values showed no significant difference between inactive and active group, while mean RI was significantly higher in the inactive group. RI was also significantly negatively correlated with PCDAI.
Conclusion
Intensity of color and power Doppler signals and RI measurement of mural arteries in thickened bowel wall is linked to CD activity and therefore might be of use in pediatric patients.
Zusammenfassung
Ziel
Das Ziel dieser Studie war es, die zuverlässigen Doppler-Parameter in den intramularen Arterien der betroffenen Darmschlingen zur quantitativen Bewertung der Aktivität des Morbus Crohn (CD) bei der pädiatrischen Population zu definieren und die Doppler-Parameter mit dem pädiatrischem Morbus Crohn Aktivitätsindex (PCDAI) zu vergleichen.
Patienten und Methoden
Der Zustand von 34 pädiatrischen Patienten (7 mit inaktiver, 27 mit aktiver Erkrankung unterschiedlichen Schweregrades, 13 männliche und 21 weibliche, Alter 7–18, Durschnittsalter 13) mit M. Crohn wurde prospektiv anhand des Doppler-Ultraschall (DUS) betroffener Darmsegmente ausgewertet. Anhand der semi-quantitativen Farb- und Power-Doppler-Beurteilung der Vaskularisation der verdickten Darmwand und des Mesenteriums wurden die Patienten in 4 Gruppen unterteilt. Die spektrale Messungen (die maximale systolische Strömungsgeschwindigkeit – PSV, die enddiastolische Strömungsgeschwindigkeit – EDV, der Resistance-Index – RI) intramuraler Arterien wurden mit PCDAI verglichen.
Ergebnisse
Es bestand ein signifikanter Unterschied in der Verteilung der semi-quantitativen Farbwerte zwischen der inaktiven und aktiven Gruppe. PSV und EDV-Werte zeigten keinen signifikanten Unterschied zwischen der inaktiven und der aktiven Gruppe, während der mittlere RI in der inaktiven Gruppe signifikant höher war. Der RI war ebenfalls signifikant negativ mit dem PCDAI korreliert.
Schlussfolgerung
Die Intensität der Farb- und Power-Doppler-Signale und die RI-Messung in den intramuralen Arterien der verdickten Darmwand stehen im Zusammenhang mit der Aktivität des Morbus Crohn und können daher bei pädiatrischen Patienten von Nutzen sein.



Similar content being viewed by others
References
Wills JS, Lobis IF, Denstman FJ. Crohn disease: state of the art. Radiology. 1997;202: 597–610.
Ali SI, Carty HML. Pediatric Crohn’s disease: a radiological review. Eur Radiol. 2000;10: 1085–94.
Charron M, Del Rosario JF, Kocoshis S. Pediatric inflammatory bowel disease: assessment with scintigraphy with 99 mTc white blood cells. Radiology. 1999;212(2):507–13.
Kjeldsen J, Schaffalitzky de Muckadell OB. Assessment of disease severity and activity in inflammatory bowel disease. Scand J Gastroenterol. 1993;28:1–9.
Tromm A, Tromm CD, Huppe D, Schwegler U, Krieg M, May B. Evaluation of different laboratory tests and activity indices reflecting the inflammatory activity of Crohn’s disease. Scand J Gastroenterol. 1992;27:774–8.
Rioux M, Gagnon J. Imaging modalities in the puzzling world of inflammatory bowel disease. Abdom Imaging. 1997;22:173–4.
Mako EK, Mester AR, Tarjan Z, Karlinger K, Toth G. Enteroclysis and spiral CT examination in diagnosis and evaluation of small bowel Crohn’s disease. Eur J Radiol. 2000;35:168–75.
Prassopoulos P, Papanikolaou N, Grammatikakis J, Rousomoustakal M, Maris T, Gourtsoyiannis N. MR enteroclysis imaging of Crohn disease. Radiographics. 2001;21:161–72.
Maconi G, Radice E, Greco S, Bianchi Porro G. Bowel ultrasound in Crohn’s disease. Best Pract Res Clin Gastroenterol. 2006;20:93–112.
Miao YM, Koh Dm, Amin Z, Healy JC, Chinn RJ, Zeegen R, et al. Ultrasound and magnetic resonance imaging assessment of active bowel segments in Crohn’s disease. Clin Radiol. 2002;57(10):913–8.
Pascu M, Roznowski AB, Muller H-P, Adler A, Wiedenmann B, Dignass AU. Clinical relevance of transabdominal ultrasonography and magnetic resonance imaging in patients with inflammatory bowel disease of the terminal ileum and large bowel. Inflamm Bowel Dis. 2004;10:373–82.
Koh DM, Miao Y, Chinn RJ, Amin Z, Zeegen R, Westaby D, et al. MR imaging evaluation of the activity of Crohn’s disease. AJR Am J Roentgenol. 2001;177(6):1325–32.
Colombel JF, Solem CA, Sandborn WJ, Booya F, Loftus EV, Harmsen WS, et al. Quantitative measurement and visual assessment of ileal Crohn’s disease activity by computed tomography enterography: correlation with endoscopic severity and C reactive protein. Gut. 2006;55:1561–7.
Bodily KD, Fletcher JG, Solem CA, Johnson DC, Fidler JL, Barlow JM, et al. Crohn disease: mural attenuation and thickness at contrast-enhanced CT enterography-correlation with endoscopic and histologic findings of inflammation. Radiology. 2006;238:505–16.
Maccioni F, Viscido A, Broglia L, Marollo M, Masciangelo R, Caprilli R, et al. Evaluation of Crohn disease activity with magnetic resonance imaging. Abdom Imaging. 2000;25:219–28.
Siegel MJ, Friedland JA, Hildebolt CF. Bowel wall thickening in children: differentiation with US. Radiology. 1997;203:631–5.
Valette PJ, Rioux M, Pilleul F, Saurin JC, Fouque P, Henry L. Ultrasonography of chronic inflammatory bowel diseases. Eur Radiol. 2001;11(10):1859–66.
Spalinger J, Patriquin H, Miron MC, Marx G, Herzog D, Dubois J, et al. Doppler US in patients with Crohn disease: vessel density in the diseased bowel reflects disease activity. Radiology. 2000;217:787–91.
Heyne R, Rickes S, Bock P, Schreiber S, Wermke W, Lochs H. Noninvasive evaluation of activity in inflammatory bowel disease by power Doppler sonography. Z Gastroenterol. 2002;40(3):171–5.
Tarjan Z, Toth G, Gyorke T, Mester A, Karlinger K, Mako EK. Ultrasound in Crohn’s disease of the small bowel. Eur J Radiol. 2000;35(3):176–82.
Scholbach T, Herrero I, Scholbach J. Dynamic Color Doppler sonography of intestinal wall in patients with Crohn disease compared with healthy subjects. J Pediatr Gastr Nutr. 2004;39:524–8.
Migaleddu V, Quaia E, Scano D, Virgilio G. Inflammatory activity in Crohn disease: ultrasound findings. Abdom Imaging. 2008;33:589–97.
Di Sabatino A, Fulle I, Ciccocioppo R, Ricevuti L, Tinozzi FP, Tinozzi S, et al. Doppler enhancement after intravenous Levovist injection in Crohn’s disease. Inflamm Bowel Dis. 2002;8:251–7.
Kratzer W, von Tirpitz C, Mason R, Reinshagen M, Adler G, Moller P, et al. Contrast-enhanced power Doppler sonography of the intestinal wall in differentiation of hypervascularized and hypovascularized intestinal obstructions in patients with Crohn’s disease. J Ultrasound Med. 2002;21:149–57.
Serra C, Menozzi G, Labate AM, Giangregorio F, Gionchetti P, Beltrami M, et al. Ultrasound assessment of vascularization of the thickened terminal ileum wall in Crohn’s disease patients using a low-mechanical index real-time scanning technique with a second generation ultrasound contrast agent. Eur J Radiol. 2007;62:114–21.
Schreyer AG, Finkenzeller T, Gossmann H, Daneschnejad M, Muller-Wille R, Schacherer D, et al. Microcirculation and perfusion with contrast-enhanced ultrasound (CEUS) in Crohn’s disease: first results with linear contrast harmonic imaging (CHI). Clin Hemorheol Microcirc. 2008;40:143–55.
Esteban JM, Maldonado L, Sanchiz V, Minguez M, Benages A. Activity of Crohn’s disease assessed by Color Doppler ultrasound analysis of the affected loops. Eur Radiol. 2001;11:1423–8.
Sjekavica I, Barbarić-Babić V, Krznarić Ž, Molnar M, Čuković-Čavka S, Ŵern-Padovan R. Assessment of Crohn Disease activity by Doppler ultrasound of the superior mesenteric artery and mural arteries in thickened bowel wall: cross-sectional study. Croat Med J. 2007;48:822–30.
Haber HP, Busch A, Ziebach R, Stern M. Bowel wall thickness measured by ultrasound as a marker of Crohn’s disease activity in children. Lancet. 2000;55(4):1239–40.
Futagami Y, Haruma K, Hata J, Fujimura J, Tani H, Okamoto E, et al. Development and validation of an ultrasonographic activity index of Crohn’s disease. Eur J Gastroenterol Hepatol. 2000;12(12):1355–6.
Mayer D, Reinshagen M, Mason RA, Muche R, von Tirpitz C, Eckelt K, et al. Sonographic measurement of thickened bowel wall segments: a quantitative parameter for activity in inflammatory bowel disease. Z Gastroenterol. 2000;38(4):295–300.
Yekeler E, Danalioglu A, Movasseghi B, Yilmaz S, Karac C, Kaymakoglu S, et al. Crohn disease activity evaluated by Doppler ultrasonography of the superior mesenteric artery and the affected small-bowel segments. J Ultrasound Med. 2005;24:59–65.
Thomson M, Rao P, Berger L, Rawat D. Graded compression and power Doppler ultrasonography versus endoscopy to assess pediatric Crohn disease activity pre- and post treatment. J Pediatr Gastroenterol Nutr. 2012;54:404–8.
De Pascale A, Garofalo G, Perna M, Priola S, Fava C. Contrast-enhanced ultrasonography in Crohn’s disease. Radiol Med. 2006;111:539–50.
Rapaccini GL, Pompili M, Orefice R, Covino M, Riccardi L, Cedrone A, Gasbarrini G. Contrast-enhanced power Doppler of the intestinal wall in the evaluation of patients with Crohn disease. Scand J Gastroenterol. 2004;39:188–94.
Robotti D, Cammarota T, Debani P, Sarno A, Astegiano M. Activity of Crohn disease: value of color-power-Doppler and contrast-enhanced ultrasonography. Abdom Imaging. 2004;29:648–52.
Migaleddu V, Scanu AM, Quaia E, Cossu-Rocca P, Pina-Dore M, Scanu D et al. Contrast-enhanced ultrasonographic evaluation of inflammatory activity in Crohn’s disease. Gastroenterology. 2009;137: 43–52.
Girlich C, Jung EM, Iesalnieks I, Schreyer AG, Zorger N, Strauch U, et al. Quantitative assessment of bowel wall vascularization in Crohn’s disease with contrast-enhanced ultrasound and perfusion analysis. Clin Hemorheol Microcirc. 2009;43:141–8.
Quaia E, Migaleddu V, Baratella E, Pizzolato R, Rossi A, Grotto M, et al. The diagnostic value of small bowel wall vascularity after sulfur hexafluoride-filled microbubble injection in patients with Crohn’s disease. Correlation with the therapeutic effectiveness of specific antiinflammatory treatment. Eur J Radiol. 2008;69:438–44.
Piscaglia F, Nolsoe C, Dietrich CF, Cosgrove DO, Gilja OH, Bachmann Nielsen M. The EFSUMB guidelines and recommendations on the clinical practice of contrast-enhanced ultrasound (CEUS): Update 2011 on nonhepatic applications. Ultraschall in Med. 2011;33:33–59.
Conflicts of interest
The authors declare that they have no conflicts of interest or financial interests with any organization involved in the research.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Sjekavica, I., Barbarić-Babić, V., Šunjara, V. et al. Resistance index in mural arteries of thickened bowel wall: predictive value for Crohn disease activity assessment in pediatric patients. Wien Klin Wochenschr 125, 254–260 (2013). https://doi.org/10.1007/s00508-013-0357-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00508-013-0357-8