Abstract
Background
This study aimed to determine incidence of kidney complications in pediatric allogeneic hematopoietic stem cell transplantation (HSCT) patients.
Methods
Pediatric allogeneic HSCT patients were included. Post-transplantation urinary system complications were collected from medical records and glomerular filtration rates at last visit compared with clinical parameters. Additionally, 24-h ambulatory blood pressure monitoring was performed.
Results
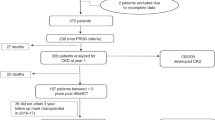
The study included 165 pediatric patients. Acute kidney injury (AKI) developed in 125 (75.8%) patients of whom 54 (43.2%) had stage 1, 36 (28.8%) stage 2, and 35 (28%) stage 3 AKI. Primary malignant disease and viral infection post-HSCT were associated with increased risk of AKI (OR: 4; 95%CI: 1.2–13, p = 0.022 and OR: 2.9; 95%CI: 1.2–6.8, p = 0.014, respectively). Mean duration of post-HSCT follow-up was 4.4 ± 2.5 years, during which time 8 patients had chronic kidney disease (CKD) (stage 1, 4 patients; stage 2, 3 patients; stage 3, 1 patient). CKD incidence was higher in patients in whom stem cell product was bone marrow + cord blood and mobilized peripheral blood, compared to bone marrow alone (40–37.5% versus 5.1%, p = 0.002). Based on 24-h ABPM, 14.7% and 7.4% of patients with normal office blood pressure had pre-hypertension and hypertension, respectively. In patients with albuminuria/severe albuminuria, daytime and nighttime systolic SDS scores were higher than those without albuminuria/severe albuminuria (p = 0.010 and p = 0.004, respectively).
Conclusions
Incidence of AKI is higher in pediatric HSCT patients with primary malignant disease and those with documented viral infection. Our study highlights the beneficial role of 24-h ABPM as a routine part of standard care of pediatric HSCT recipients.

Similar content being viewed by others
References
Hingorani S (2016) Renal complications of hematopoietic-cell transplantation. N Engl J Med 374:2256–2267
Raina R, Herrera N, Krishnappa V, Sethi SK, Deep A, Kao WM, Bunchman T, Abu-Arja R (2017) Hematopoietic stem cell transplantation and acute kidney injury in children: a comprehensive review. Pediatr Transplant 21(4). https://doi.org/10.1111/petr.12935
Koh KN, Sunkara A, Kang G, Sooter A, Mulrooney DA, Triplett B, Onder AM, Bissler J, Cunningham LC (2018) Acute kidney injury in pediatric patients receiving allogeneic hematopoietic cell transplantation: ıncidence, risk factors, and outcomes. Biol Blood Marrow Transplant 24:758–764
Pao E, Gove NE, Flynn JT, Hingorani S (2018) Ambulatory blood pressure and endothelial dysfunction in hematopoietic cell transplantation recipients. Biol Blood Marrow Transplant 24:1678–1684
Hoffmeister PA, Hingorani SR, Storer BE, Baker KS, Sanders JE (2010) Hypertension in long-term survivors of pediatric hematopoietic cell transplantation. Biol Blood Marrow Transplant 16:515–524
Bacigalupo A, Ballen K, Rizzo D, Giralt S, Lazarus H, Ho V, Apperley J, Slavin S, Pasquini M, Sandmaier BM, Barrett J, Blaise D, Lowski R, Horowitz M (2009) Defining the intensity of conditioning regimens: working definitions. Biol Blood Marrow Transplant 15:1628–1633
Glucksberg H, Storb R, Fefer A, Buckner CD, Neiman PE, Clift RA, Lerner KG, Thomas ED (1974) Clinical manifestations of graft versus-host disease in human recipients of marrow from HLA-matched sibling donors. Transplantation 18:295–304
Storb R, Prentice RL, Sullivan KM, Shulman HM, Deeg HJ, Doney KC, Buckner CD, Clift RA, Witherspoon RP, Appelbaum FA, Sanders JE, Stewart PS, Thomas ED (1983) Predictive factors in chronic graft versus-host disease in patients with aplastic anemia treated by bone marrow transplantation from HLA-identical siblings. Ann Intern Med 98:461–466
McDonald GB, Sharma P, Matthews DE, Shulman HM, Thomas ED (1984) Venocclusive disease of the liver after bone marrow transplantation: diagnosis, incidence, and predisposing factors. Hepatology 4:116–122
Tsuboi K, Kishi K, Ohmachi K, Yasuda Y, Shimizu T, Inoue H, Matsumoto M, Hattori K, Yoshiba F, Watanabe S, Ogawa Y, Kawada H, Yabe H, Yabe M, Kato S, Hotta T (2003) Multivariate analysis of risk factors for hemorrhagic cystitis after hematopoietic stem cell transplantation. Bone Marrow Transplant 32:903–907
Zanis-Neto J, Flowers ME, Medeiros CR, Bitencourt MA, Bonfim CM, Setúbal DC, Funke V, Sanders J, Deeg HJ, Kiem HP, Martin P, Leisenring W, Storb R, Pasquini R (2005) Low-dose cyclophosphamide conditioning for haematopoietic cell transplantation from HLA-matched related donors in patients with Fanconi anemia. Br J Haematol 130:99–106
Kidney Disease: Improving Global Outcomes (KDIGO) Acute Kidney Injury Work Group (2012) KDIGO clinical practice guideline for acute kidney injury. Kidney Int Suppl 2:1–138
Lurbe E, Agabiti-Rosei E, Cruickshank JK, Dominiczak A, Erdine S, Hirth A, Invitti C, Litwin M, Mancia G, Pall D, Rascher W, Redon J, Schaefer F, Seeman T, Sinha M, Stabouli S, Webb NJ, Wühl E, Zanchetti A (2016) 2016 European Society of Hypertension guidelines for the management of high blood pressure in children and adolescents. J Hypertens 34:1887–1920
Wühl E, Witte K, Soergel M, Mehls O, Schaefer F, German Working Group on Pediatric Hypertension (2002) German working group of pediatric hypertension. Distribution of 24-h ambulatory blood pressure in children: normalized reference values and role of body dimensions. J Hypertens 20:1995–2007
Flynn JT, Daniels SR, Hayman LL, Maahs DM, McCrindle BW, Mitsnefes M, Zachariah JP, Urbina EM, American Heart Association Atherosclerosis, Hypertension and Obesity in Youth Committee of the Council on Cardiovascular Disease in the Young (2014) Update: ambulatory blood pressure monitoring in children and adolescents: a scientific statement from the American Heart Association. Hypertension 63:1116–1135
KDIGO AKI Work Group (2012) KDIGO clinical practice guideline for acute kidney injury. Kidney Int Suppl 2:1–138
Raina R, Abu-Arja R, Sethi S, Dua R, Chakraborty R, Dibb JT, Basu RK, Bissler J, Felix MB, Brophy P, Bunchman T, Alhasan K, Haffner D, Kim YH, Licht C, McCulloch M, Menon S, Onder AM, Khooblall P, Khooblall A, Polishchuk V, Rangarajan H, Sultana A, Kashtan C (2022) Acute kidney injury in pediatric hematopoietic cell transplantation: critical appraisal and consensus. Ped Nephrol. https://doi.org/10.1007/s00467-022-05448-x
Hazar V, Gungor O, Guven AG, Aydin F, Akbas H, Gungor F, Tezcan G, Akman S, Yesilipek A (2009) Renal function after hematopoietic stem cell transplantation in children. Pediatr Blood Cancer 53:197–202
Ileri T, Ertem M, Ozcakar ZB, Ince EU, Biyikli Z, Uysal Z, Ekim M, Yalcinkaya F (2010) Prospective evaluation of acute and chronic renal function in children following matched related donor hematopoietic stem cell transplantation. Pediatr Transplant 14:138–144
Kurokawa M, Nishiyama K, Koga Y, Eguchi K, Imai T, Oba U, Shiraishi A, Nagata H, Kaku N, Ishimura M, Honjo S, Ohga S (2020) Hyperferritinemia and acute kidney injury in pediatric patients receiving allogeneic hematopoietic cell transplantation. Pediatr Nephrol 35:1977–1984
Armenian SH, Chemaitilly W, Chen M, Chow EJ, Duncan CN, Jones LW, Pulsipher MA, Remaley AT, Rovo A, Salooja N, Battiwalla M (2017) National Institutes of Health hematopoietic cell transplantation late effects initiative: the cardiovascular disease and associated risk factors working group report. Biol Blood Marrow Transplant 23:201–210
Gülhan B, Topaloğlu R, Karabulut E, Ozaltın F, Aki FT, Bilginer Y, Beşbaş N (2014) Post-transplant hypertension in pediatric kidney transplant recipients. Pediatr Nephrol 29:1075–1080
Kist-van Holthe JE, van Zwet JM, Brand R, van Weel MH, Vossen JM, van der Heijden AJ (1998) Bone marrow transplantation in children: consequences for renal function shortly after and 1 year post-BMT. Bone Marrow Transplant 22:559–564
Kist-van Holthe JE, Bresters D, Ahmed-Ousenkova YM, Goedvolk CA, Abbink FC, Wolterbeek R, Bredius RG, Pauwels EK, van der Heijden AJ (2005) Long-term renal function after hemopoietic stem cell transplantation in children. Bone Marrow Transplant 36:605–610
Frisk P, Bratteby LE, Carlson K, Lönnerholm G (2002) Renal function after autologous bone marrow transplantation in children: a long-term prospective study. Bone Marrow Transplant 29:129–136
Lugthart G, Jordans CCE, de Pagter APJ, Bresters D, Jol-van der Zijde CM, Bense JE, van Rooij-Kouwenhoven RWG, Sukhai RN, Louwerens M, Dorresteijn EM, Lankester AC (2021) Chronic kidney disease ten years after pediatric allogeneic hematopoietic stem cell transplantation. Kidney Int 100:906–914
Author information
Authors and Affiliations
Contributions
All authors contributed to the study conception and design. Material preparation, data collection, and analysis were performed by Anar Gurbanov, Bora Gulhan, and Barış Kuşkonmaz. The first draft of the manuscript was written by Anar Gurbanov and Bora Gulhan and all authors commented on previous versions of the manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Gurbanov, A., Gülhan, B., Kuşkonmaz, B. et al. Predictors of kidney complications and analysis of hypertension in children with allogeneic hematopoietic stem cell transplantation. Pediatr Nephrol 38, 461–469 (2023). https://doi.org/10.1007/s00467-022-05599-x
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00467-022-05599-x