Abstract
Background
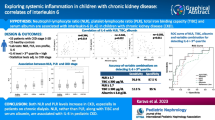
Chronic inflammation in patients with predialysis chronic kidney disease (CKD) is quite common. We aimed to investigate the relationship of the percentage of immature granulocytes (IG%) and immature granulocyte count (IGC) with inflammation in children with predialysis CKD.
Methods
The data from children with stage 2–4 CKD and a control group of healthy children were evaluated retrospectively. A highly-sensitive C-reactive protein (hs-CRP) level above 5 mg/dL was considered the presence of inflammation. The IGCs were calculated in the white cell differential channel of the Sysmex XN-9000 using the fluorescent flow cytometry method. The IG% was expressed as percentage of total leucocyte concentration.
Results
The data from 57 patients (30 stage 2 CKD, 15 stage 3 CKD, 12 stage 4 CKD) and 46 controls were analyzed. hs-CRP levels, IG%, IGC, white blood cell (WBC) and neutrophil counts, and neutrophil-to-lymphocyte ratio (NLR) were higher in patients than the control group (p < 0.000, p < 0.000, p < 0.000, p = 0.001, p = 0.002, p < 0.000, respectively). Both IG% and IGC were positively correlated with hs-CRP, WBC and neutrophil counts, and NLR (r = 0.485, p < 0.000; r = 0.379, p = 0.004; r = 0.543, p < 0.000; r = 0.628, p < 0.000 for IG%; r = 0.379, p = 0.004; r = 0.351, p = 0.007; r = 0.525, p < 0.000; r = 0.601, p < 0.000 for IGC, respectively). A ROC analysis of the relationship between IGC, IG%, and inflammation showed IGC and IG% had predictive value for the presence of inflammation (cut-off value: 0.035 × 106/mL, AUC: 0.799 ± 0.061, sensitivity: 74.2%, specifity: 63%, p < 0.001 for IGC; cut-off value: 0.45%, AUC: 0.838 ± 0.056, sensitivity: 70.8%, specifity: 67.3%, p = 0.001 for IG%).
Conclusions
Immature granulocytes may be used as a biomarker of inflammation in children with predialysis CKD.
Graphical abstract
A higher resolution version of the Graphical abstract is available as Supplementary information




Similar content being viewed by others
Data availability
The datasets generated during and/or analyzed during the current study are available from the corresponding author on reasonable request.
References
Harambat J, van Stralen KJ, Kim JJ, Tizard EJ (2011) Epidemiology of chronic kidney disease in children. Pediatr Nephrol 27:363–373. https://doi.org/10.1007/s00467-011-1939-1
Akchurin OM, Kaskel F (2015) Update on inflammation in chronic kidney disease. Blood Purif 39:84–92. https://doi.org/10.1159/000368940
Fernandes B, Hamaguchi Y (2007) Automated enumeration of immature granulocytes. Am J Clin Pathol 128:454–463. https://doi.org/10.1309/TVGKD5TVB7W9HHC7
Senthilnayagam B, Kumar T, Sukumaran J, Jeya M, Rao KR (2012) Automated measurement of immature granulocytes: performance characteristics and utility in routine clinical practice. Patholog Res Int 2012:483670. https://doi.org/10.1155/2012/483670
Tan C, Huang Y, Zhang L, Chen J, Wang Y, Peng J et al (2018) Predictive value of immature granulocytes for persistent systemic inflammatory response syndrome in patients with acute pancreatitis: analysis of 1973 cases. Zhonghua Wei Zhong Bing Ji Jiu Yi Xue 30:1123–1127. https://doi.org/10.3760/cma.j.issn.2095-4352.2018.012.004
Unal Y, Barlas AM (2019) Role of increased immature granulocyte percentage in the early prediction of acute necrotizing pancreatitis. Ulus Travma Acil Cerrahi Derg 25:177–182. https://doi.org/10.14744/tjtes.2019.70679
Unal Y (2018) A new and early marker in the diagnosis of acute complicated appendicitis: immature granulocytes. Ulus Travma Acil Cerrahi Derg 24:434–439. https://doi.org/10.5505/tjtes.2018.91661
Briggs C, Longair I, Kumar P, Singh D, Machin SJ (2012) Performance evaluation of the Sysmex haematology XN modular system. J Clin Pathol 65:1024–1030. https://doi.org/10.1136/jclinpath-2012-200930
Kidney Disease: Improving Global Outcomes (KDIGO) CKD Work Group (2013) KDIGO 2012 clinical practice guideline for the evaluation and management of chronic kidney disease. Kidney Int Suppl 3:1–150
Brito GMC, Fontenele AMM, Carneiro ECRL, Nogueira IAL, Cavalcante TB, Vale AAM et al (2021) Neutrophil-to-lymphocyte and platelet-to-lymphocyte ratios in nondialysis chronic kidney patients. Int J Inflam 2021:6678960. https://doi.org/10.1155/2021/6678960
Schwartz GJ, Brion LP, Spitzer A (1987) The use of plasma creatinine concentration for estimating glomerular filtration rate in infants, children, and adolescents. Pediatr Clin North Am 34:571–590. https://doi.org/10.1016/s0031-3955(16)36251-4
Rosengren BI, Sagstad SJ, Karlsen TV, Wiig H (2013) Isolation of interstitial fluid and demonstration of local proinflammatory cytokine production and increased absorptive gradient in chronic peritoneal dialysis. Am J Physiol Renal Physiol 304:F198–F206. https://doi.org/10.1152/ajprenal.00293.2012
Kim HJ, Vaziri ND (2010) Contribution of impaired Nrf2-Keap1 pathway to oxidative stress and inflammation in chronic renal failure. Am J Physiol Renal Physiol 298:F662–F671. https://doi.org/10.1152/ajprenal.00421.2009
Aveles PR, Criminacio CR, Goncalves S, Bignelli AT, Claro LM, Siqueira SS et al (2010) Association between biomarkers of carbonyl stress with increased systemic inflammatory response in different stages of chronic kidney disease and after renal transplantation. Nephron Clin Pract 116:294–299. https://doi.org/10.1159/000318792
Mihai S, Codrici E, Popescu ID, Enciu AM, Albulescu L, Necula LG et al (2018) Inflammation-related mechanisms in chronic kidney disease prediction, progression, and outcome. J Immunol Res 2018:2180373. https://doi.org/10.1155/2018/2180373
Costa E, Lima M, Alves JM, Rocha S, Rocha-Pereira P, Castro E et al (2008) Inflammation, T-cell phenotype, and inflammatory cytokines in chronic kidney disease patients under hemodialysis and its relationship to resistance to recombinant human erythropoietin therapy. J Clin Immunol 28:268–275. https://doi.org/10.1007/s10875-007-9168-x
Goldstein SL, Currier H, Waters L, Hempe JM, Sheth RD, Silverstein DM (2003) Acute and chronic inflammation in pediatric patients receiving hemodialysis. J Pediatr 143:653–657. https://doi.org/10.1067/S0022-3476(03)00534-1
Ridker PM (2001) High-sensitivity C-reactive protein potential adjunct for global risk assessment in the primary prevention of cardiovascular disease. Circulation 103:1813–1818. https://doi.org/10.1161/01.cir.103.13.1813
Roberts WL, Sedrick R, Moulton L, Spencer A, Rifai N (2000) Evaluation of four automated high-sensitivity C-reactive protein methods: implications for clinical and epidemiological applications. Clin Chem 46:461–468
Okyay GU, Inal S, Oneç K, Er RE, Paşaoğlu O, Paşaoğlu H et al (2013) Neutrophil to lymphocyte ratio in evaluation of ınflammation in patients with chronic kidney disease. Ren Fail 35:29–36. https://doi.org/10.3109/0886022X.2012.734429
Abu Alfeilat M, Slotki I, Shavit L (2018) Single emergency room measurement of neutrophil/lymphocyte ratio for early detection of acute kidney injury (AKI). Intern Emerg Med 13:717–725. https://doi.org/10.1007/s11739-017-1715-8
Azab B, Daoud J, Naeem FB, Nasr R, Ross J, Ghimire P et al (2012) Neutrophil-to-lymphocyte ratio as a predictor of worsening renal function in diabetic patients (3-year follow-up study). Ren Fail 34:571–576. https://doi.org/10.3109/0886022X.2012.668741
Sadik CD, Kim ND, Luster AD (2011) Neutrophils cascading their way to inflammation. Trends Immunol 32:452–460. https://doi.org/10.1016/j.it.2011.06.008
Goag EK, Lee JW, Roh YH, Leem AY, Kim SY, Song JH et al (2018) A simplified mortality score using delta neutrophil index and the thrombotic microangiopathy score for prognostication in critically 111 patients. Shock 49:39–43. https://doi.org/10.1097/SHK.0000000000000936
Nigro KG, O’Riordan M, Mollloy EJ, Walsh MC, Sandhaus LM (2005) Performance of an automated immature granulocyte count as a predictor of neonatal sepsis. Am J Clin Pathol 123:618–624. https://doi.org/10.1309/73H7-K7UB-W816-PBJJ
Karakulak S, Narcı H, Ayrık C, Erdoğan S, Üçbilek E (2021) The prognostic value of immature granulocyte in patients with acute pancreatitis. Am J Emerg Med 44:203–207. https://doi.org/10.1016/j.ajem.2020.03.028
Geest PJ, Mohseni M, Brouwer R, van der Hoven B, Steyerberg EW, Groeneveld AB (2014) Immature granulocytes predict microbial infection and its adverse sequelae in the intensive care unit. J Crit Care 29:523–527. https://doi.org/10.1016/j.jcrc.2014.03.033
Nierhaus A, Klatte S, Linssen J, Eismann NM, Wichmann D, Hedke J et al (2013) Revisiting the white blood cell count: ımmature granulocytes count as a diagnostic marker to discriminate between SIRS and sepsis—a prospective, observational study. BMC Immunol 14:8. https://doi.org/10.1186/1471-2172-14-8
Güngör T, Özdel S, Çakici EK, Yazilitaş F, Bağlan E, Karakaya D et al (2021) An assessment on the effectiveness of the ımmature granulocyte percentage in predicting ınternal organ ınvolvement among children With Henoch-Schönlein purpura. J Pediatr Hematol Oncol. https://doi.org/10.1097/MPH.0000000000002288
Pavare J, Grope I, Gardovska D (2018) Assessment of ımmature granulocytes percentage to predict severe bacterial ınfection in latvian children: an analysis of secondary data. Medicina 54:56. https://doi.org/10.3390/medicina54040056
Yoon SH, Shin H, Lee KH, Kim MK, Kim DS, Ahn JG et al (2020) Predictive factors for bacteremia in febrile infants with urinary tract infection. Sci Rep 10:4469. https://doi.org/10.1038/s41598-020-61421-4
Author information
Authors and Affiliations
Contributions
Research conception and design: Nuran Cetin. Data acquisition: Nuran Cetin, Evin Kocatürk, Aslı Kavaz Tufan. Statistical analysis: Nuran Cetin, Evin Kocatürk, Aslı Kavaz Tufan. Data analysis and interpretation: Nuran Cetin, Evin Kocatürk, Zeynep Küskü Kiraz, Ozkan Alatas. Drafting of the manuscript: Nuran Cetin, Evin Kocatürk. Critical revision of the manuscript: Nuran Cetin, Aslı Kavaz Tufan, Zeynep Küskü Kiraz, Ozkan Alatas. Obtaining funding: Nuran Cetin, Evin Kocatürk, Aslı Kavaz Tufan. Supervision: Zeynep Küskü Kiraz, Ozkan Alatas. Approval of the final manuscript: All authors approved the final manuscript.
Corresponding author
Ethics declarations
Consent to participate
Not applicable.
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Cetın, N., Kocaturk, E., Tufan, A.K. et al. Immature granulocytes as biomarkers of inflammation in children with predialysis chronic kidney disease. Pediatr Nephrol 38, 219–225 (2023). https://doi.org/10.1007/s00467-022-05530-4
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00467-022-05530-4



