Abstract
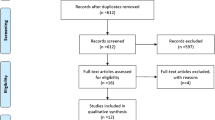
Fluid overload (FO) is associated with higher rates of mortality and morbidity in pediatric and adult populations. The aim of this systematic review and meta-analysis was to investigate the association between FO and mortality in critically ill neonates. Systematic search of Ovid MEDLINE, EMBASE, Cochrane Library, trial registries, and gray literature from inception to January 2021. We included all studies that examined neonates admitted to neonatal intensive care units and described FO and outcomes of interest. We identified 17 observational studies with a total of 4772 critically ill neonates who met the inclusion criteria. FO was associated with higher mortality (OR, 4.95 [95% CI, 2.26–10.87]), and survivors had a lower percentage of FO compared with nonsurvivors (WMD, − 4.33 [95% CI, − 8.34 to − 0.32]). Neonates who did not develop acute kidney injury (AKI) had lower FO compared with AKI patients (WMD, − 2.29 [95% CI, − 4.47 to − 0.10]). Neonates who did not require mechanical ventilation on postnatal day 7 had lower fluid balance (WMD, − 1.54 [95% CI, − 2.21 to − 0.88]). FO is associated with higher mortality, AKI, and need for mechanical ventilation in critically ill neonates in the intensive care unit. Strict control of fluid balance to prevent FO is essential.
Graphical abstract
A higher resolution version of the Graphical abstract is available as Supplementary information







Similar content being viewed by others
References
Lopes CLS, Piva JP (2017) Fluid overload in children undergoing mechanical ventilation. Rev Bras Ter Intensiva 29:346–353
Stritzke A, Thomas S, Amin H, Fusch C, Lodha A (2017) Renal consequences of preterm birth. Mol Cell Pediatr 4:2. https://doi.org/10.1186/s40348-016-0068-0
Murphy CV, Schramm GE, Doherty JA, Reichley RM, Gajic O, Afessa B, Micek ST, Kollef MH (2009) The importance of fluid management in acute lung injury secondary to septic shock. Chest 136:102–109
Claure-Del Granado R, Mehta RL (2016) Fluid overload in the ICU: evaluation and management. BMC Nephrol 17:109
Ogbu OC, Murphy DJ, Martin GS (2015) How to avoid fluid overload. Curr Opin Crit Care 21:315–321
Sakr Y, Vincent JL, Reinhart K, Groeneveld J, Michalopoulos A, Sprung CL, Artigas A, Ranieri VM (2005) High tidal volume and positive fluid balance are associated with worse outcome in acute lung injury. Chest 128:3098–3108
National Heart, Lung, and Blood Institute Acute Respiratory Distress Syndrome (ARDS) Clinical Trials Network, Wiedemann HP, Wheeler AP, Bernard GR, Thompson BT, Hayden D, deBoisblanc B, Connors AF Jr, Hite RD, Harabin AL (2005) Comparison of Two Fluid-Management Strategies in Acute Lung Injury. N Engl J Med 51(229):230
Sakr Y, Rubatto Birri PN, Kotfis K, Nanchal R, Shah B, Kluge S, Schroeder ME, Marshall JC, Vincent JL (2017) Higher fluid balance increases the risk of death from sepsis: results from a large international audit∗. Crit Care Med 45:386–394
Messmer AS, Zingg C, Müller M, Gerber JL, Schefold JC, Pfortmueller CA (2020) Fluid Overload and Mortality in Adult Critical Care Patients-A Systematic Review and Meta-Analysis of Observational Studies. Crit Care Med 48:1862–1870
Alobaidi R, Morgan C, Basu RK, Stenson E, Featherstone R, Majumdar SR, Bagshaw SM (2018) Association between fluid balance and outcomes in critically ill children: a systematic review and meta-analysis. JAMA Pediatr 172:257–268
Selewski DT, Akcan-Arikan A, Bonachea EM, Gist KM, Goldstein SL, Hanna M, Joseph C, Mahan JD, Nada A, Nathan AT, Reidy K, Staples A, Wintermark P, Boohaker LJ, Griffin T, Askenazi DJ, Guillet R (2018) The impact of fluid balance on outcomes in critically ill near-term/term neonates: a report from the AWAKEN study group. Pediatr Res 85:79–85
Shamseer L, Moher D, Clarke M, Ghersi D, Liberati A, Petticrew M, Shekelle P, Stewart LA (2015) Preferred reporting items for systematic review and meta-analysis protocols (prisma-p) 2015: Elaboration and explanation. BMJ 349:1–25
Higgins JPT, Thomas J, Chandler J, Cumpston M, Li T, Page MJ, Welch VA (editors). Cochrane Handbook for Systematic Reviews of Interventions version 6.2 (updated February 2021). Cochrane, 2021. Available from https://www.training.cochrane.org/handbook.
McGowan J, Sampson M, Salzwedel DM, Cogo E, Foerster V, Lefebvre C (2016) PRESS Peer Review of Electronic Search Strategies: 2015 Guideline Statement. J Clin Epidemiol 75:40–46
Ouzzani M, Hammady H, Fedorowicz Z, Elmagarmid A (2016) Rayyan-a web and mobile app for systematic reviews. Syst Rev 5:210
GA Wells, B Shea, D O'Connell, J Peterson, V Welch, M Losos, P Tugwell. The Newcastle-Ottawa Scale (NOS) for assessing the quality of nonrandomised studies in meta-analyses. http://www.ohri.ca/programs/clinical_epidemiology/oxford.asp. Published 2000. Accessed 1 Jan 2021
Wan X, Wang W, Liu J, Tong T (2014) Estimating the sample mean and standard deviation from the sample size, median, range and/or interquartile range. BMC Med Res Methodol 14:135
Ueno K, Shiokawa N, Takahashi Y, Nakae K, Kawamura J, Imoto Y, Kawano Y (2019) Kidney disease: improving global outcomes in neonates with acute kidney injury after cardiac surgery. Clin Exp Nephrol 24:167–173
Matsushita FY, Krebs VLJ, Ferraro AA, de Carvalho WB (2020) Early fluid overload is associated with mortality and prolonged mechanical ventilation in extremely low birth weight infants. Eur J Pediatr 179:1665–1671
Rallis D, Drougia A, Balomenou F, Fintzou M, Benekos T, Vlahos A, Giapros V (2019) The association of fluid overload during the first postnatal day with patent ductus arteriosus and bronchopulmonary dysplasia in preterm infants. Eur J Pediatr 178:1733–1734
Stojanović V, Bukarica S, Antić J, Doronjski A (2017) Peritoneal dialysis in very low birth weight neonates. J Matern Neonatal Med 29:283–284
Noh ES, Kim HH, Kim HS, Han YS, Yang M, Ahn SY, Sung SI, Chang YS, Park WS (2019) Continuous Renal Replacement Therapy in Preterm Infants. Yonsei Med J 60:984–991
Askenazi DJ, Koralkar R, Hundley HE, Montesanti A, Patil N, Ambalavanan N (2013) Fluid overload and mortality are associated with acute kidney injury in sick near-term/term neonate. Pediatr Nephrol 28:661–666
Selewski DT, Gist KM, Nathan AT, Goldstein SL et al (2020) The impact of fluid balance on outcomes in premature neonates: a report from the AWAKEN study group. Pediatr Res 87:550–557
Wilder NS, Yu S, Donohue JE, Goldberg CS, Blatt NB (2016) Fluid overload is associated with late poor outcomes in neonates following cardiac surgery. Pediatr Crit Care Med 17:420–427
Mah KE, Hao S, Sutherland SM, Kwiatkowski DM, Axelrod DM, Almond CS, Krawczeski CD, Shin AY (2017) Fluid overload independent of acute kidney injury predicts poor outcomes in neonates following congenital heart surgery. Pediatr Nephrol 33:511–520
Lee HJ, Lee BS, Do H-J, Oh S-H, Choi Y-S, Chung S-H, Kim EA-R, Kim K-S (2015) Early sodium and fluid intake and severe intraventricular hemorrhage in extremely low birth weight infants. J Korean Med Sci 30:283–289
Lee ST, Cho H (2016) Fluid overload and outcomes in neonates receiving continuous renal replacement therapy. Pediatr Nephrol 31:2145–2152
Adcock B, Carpenter S, Bauer J, Giannone P, Schadler A, Chishti A, Hanna M (2020) Acute kidney injury, fluid balance and risks of intraventricular hemorrhage in premature infants. J Perinatol 40:1296–1300
Guo MM-H, Chung C-H, Chen F-S, Chen C-C, Huang H-C, Chung M-Y (2015) Severe bronchopulmonary dysplasia is associated with higher fluid intake in very low-birth-weight infants: a retrospective study. Am J Perinatol 30:155–162
Piggott KD, Soni M, Decampli WM, Ramirez JA, Holbein D, Fakioglu H, Blanco CJ, Pourmoghadam KK (2015) Acute kidney injury and fluid overload in neonates following surgery for congenital heart disease. World J Pediatr Congenit Heart Surg 6:401–406
Yum SK, Sung HJ, Sung IK (2019) Risk factors associated with acute kidney injury after bedside open laparotomy in neonates. Crit Care Med 47:712. https://doi.org/10.1097/01.ccm.0000552215.59880.6c
Oh W, Poindexter BB, Perritt R, Lemons JA, Bauer CR, Ehrenkranz RA, Stoll BJ, Poole K, Wright LL (2005) Association between fluid intake and weight loss during the first ten days of life and risk of bronchopulmonary dysplasia in extremely low birth weight infants. J Pediatr 147:786–790
Jetton JG, Boohaker LJ, Sethi SK, Wazir S et al (2017) Incidence and outcomes of neonatal acute kidney injury (AWAKEN): a multicentre, multinational, observational cohort study. Lancet Child Adolesc Health 1:184–194
Mehta RL, Kellum JA, Shah SV, Molitoris BA et al (2007) Acute kidney injury network: Report of an initiative to improve outcomes in acute kidney injury. Crit Care 11:R31
Akcan-Arikan A, Zappitelli M, Loftis LL, Washburn KK, Jefferson LS, Goldstein SL (2007) Modified RIFLE criteria in critically ill children with acute kidney injury. Kidney Int 71:1028–1035
Kreimeier U (2000) Pathophysiology of fluid imbalance. Crit Care 4(Suppl 2):S3-7
Marx G, Vangerow B, Burczyk C, Gratz KF, Maassen N, Cobas Meyer M, Leuwer M, Kuse E, Rueckoldt H (2000) Evaluation of noninvasive determinants for capillary leakage syndrome in septic shock patients. Intensive Care Med 26:1252–1258
Sánchez M, Jiménez-Lendínez M, Cidoncha M, Asensio MJ, Herrero E, Collado A, Santacruz M (2011) Comparison of fluid compartments and fluid responsiveness in septic and non-septic patients. Anaesth Intensive Care 39:1022–1029
Yerram P, Karuparthi PR, Misra M (2010) Fluid overload and acute kidney injury. Hemodial Int 14:348–354
Flori HR, Church G, Liu KD, Gildengorin G, Matthay MA (2011) Positive fluid balance is associated with higher mortality and prolonged mechanical ventilation in pediatric patients with acute lung injury. Crit Care Res Pract 2011:854142
Ostermann M, van Straaten HMO, Forni LG (2015) Fluid overload and acute kidney injury: cause or consequence? Crit Care 19:19–21
Wang N, Jiang L, Zhu B, Wen Y, Xi XM (2015) Fluid balance and mortality in critically ill patients with acute kidney injury: a multicenter prospective epidemiological study. Crit Care 19:371
Kavvadia V, Greenough A, Dimitriou G, Hooper R (2000) Randomised trial of fluid restriction in ventilated very low birthweight infants. Arch Dis Child Fetal Neonatal Ed 83:5–10
Tanigasalam V, Plakkal N, Vishnu Bhat B, Chinnakali P (2018) Does fluid restriction improve outcomes in infants with hypoxic ischemic encephalopathy? A pilot randomized controlled trial. J Perinatol 38:1512–1517
Gupta N, Bruschettini M, Chawla D (2021) Fluid restriction in the management of transient tachypnea of the newborn. Cochrane Database Syst Rev 2:CD011466. https://doi.org/10.1002/14651858.CD011466.pub2
Barrington KJ, Fortin-Pellerin E, Pennaforte T (2017) Fluid restriction for treatment of preterm infants with chronic lung disease. Cochrane Database Syst Rev 2:CD005389. https://doi.org/10.1002/14651858.CD005389.pub2
Acknowledgements
We thank all the colleagues at the NICU staff at the Faculty of Medicine of the University of São Paulo.
Author information
Authors and Affiliations
Contributions
F.Y.M., V.L.J.K, and W.B.C conceptualized and designed the study and reviewed and revised the manuscript. F.Y.M. and V.L.J.K collected data, carried out statistical analysis, interpreted the data, and drafted the initial manuscript. All authors approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Patient consent
Because this is a meta-analysis, patient consent was not required.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Impact
• Fluid overload is associated with higher mortality rate, acute kidney injury, and mechanical ventilation necessity in newborns.
• This is the first systematic review and meta-analysis to analyze the association between fluid overload and outcomes in newborns.
• More careful attention to fluid balance control in neonates is needed.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Matsushita, F.Y., Krebs, V.L.J. & de Carvalho, W.B. Association between fluid overload and mortality in newborns: a systematic review and meta-analysis. Pediatr Nephrol 37, 983–992 (2022). https://doi.org/10.1007/s00467-021-05281-8
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00467-021-05281-8