Abstract
Background
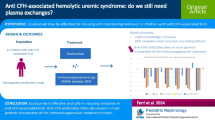
Atypical hemolytic and uremic syndrome (aHUS), a thrombotic micro-angiopathy (TMA) caused by deregulation in the complement pathway, is sometimes due to the presence of anti-complement factor H (CFH) auto-antibodies. The “standard” treatment for such aHUS combines plasma exchange therapy and immunosuppressive drugs. Eculizumab, a monoclonal antibody that blocks the terminal pathway of the complement cascade, could be an interesting alternative in association with an immunosuppressive treatment for maintenance regimen.
Case–diagnosis/treatment
We report on two children, diagnosed with mildly severe aHUS due to anti-CFH antibodies, who were treated with the association eculizumab–mycophenolate mofetil (MMF). Neither side effects nor relapses were observed during the 3 years of follow-up; MMF was even progressively tapered and withdrawn successfully in one patient.
Conclusions
The association of eculizumab and MMF appears to be an effective and safe option in pediatric cases of aHUS due to anti-CFH antibodies of mild severity.

Similar content being viewed by others
References
Loirat C, Fakhouri F, Ariceta G, Besbas N, Bitzan M, Bjerre A, Coppo R, Emma F, Johnson S, Karpman D, Landau D, Langman CB, Lapeyraque AL, Licht C, Nester C, Pecoraro C, Riedl M, van de Kar NC, Van de Walle J, Vivarelli M, Frémeaux-Bacchi V, HUS International (2016) An international consensus approach to the management of atypical hemolytic uremic syndrome in children. Pediatr Nephrol 31:15–39. https://doi.org/10.1007/s00467-015-3076-8
Loirat C, Frémeaux-Bacchi V (2011) Atypical hemolytic uremic syndrome. Orphanet J Rare Dis 6:60. https://doi.org/10.1186/1750-1172-6-60
Ariceta G, Besbas N, Johnson S, Karpman D, Landau D, Licht C, Loirat C, Pecoraro C, Taylor CM, Van de Kar N, Vandewalle J, Zimmerhackl LB, European Paediatric Study Group for HUS (2009) Guideline for the investigation and initial therapy of diarrhea-negative hemolytic uremic syndrome. Pediatr Nephrol 24:687–696. https://doi.org/10.1007/s00467-008-0964-1
Diamante Chiodini B, Davin JC, Corazza F, Khaldi K, Dahan K, Ismaili K, Adams B (2014) Eculizumab in anti-factor H antibodies associated with atypical hemolytic uremic syndrome. Pediatrics 133:e1764–e1768. https://doi.org/10.1542/peds.2013-1594
Brocklebank V, Johnson S, Sheerin TP, Marks SD, Gilbert RD, Tyerman K, Kinoshita M, Awan A, Kaur A, Webb N, Hegde S, Finlay E, Fitzpatrick M, Walsh PR, Wong EKS, Booth C, Kerecuk L, Salama AD, Almond M, Inward C, Goodship TH, Sheerin NS, Marchbank KJ, Kavanagh D (2017) Factor H autoantibody is associated with atypical hemolytic uremic syndrome in children in the United Kingdom and Ireland. Kidney Int 92:1261–1271. https://doi.org/10.1016/j.kint.2017.04.028
Eculizumab in Shiga-toxin related hemolytic and uremic syndrome pediatric patients - ECULISHU - full text view - ClinicalTrials.gov. https://clinicaltrials.gov/ct2/show/NCT02205541. Accessed 11 Dec 2018
Dragon-Durey MA, Sethi SK, Bagga A, Blanc C, Blouin J, Ranchin B, André JL, Takagi N, Cheong HI, Hari P, Le Quintrec M, Niaudet P, Loirat C, Fridman WH, Frémeaux-Bacchi V (2010) Clinical features of anti-factor H autoantibody–associated hemolytic uremic syndrome. J Am Soc Nephrol 21:2180–2187. https://doi.org/10.1681/ASN.2010030315
Noris M, Remuzzi G (2009) Atypical hemolytic–uremic syndrome. N Engl J Med 361:1676–1687. https://doi.org/10.1056/NEJMra0902814
Loirat C, Garnier A, Sellier-Leclerc AL, Kwon T (2010) Plasmatherapy in atypical hemolytic uremic syndrome. Semin Thromb Hemost 36:673–681. https://doi.org/10.1055/s-0030-1262890
Sana G, Dragon-Durey M-A, Charbit M, Bouchireb K, Rousset-Rouvière C, Bérard E, Salomon R, Frémeaux-Bacchi V, Niaudet P, Boyer O (2014) Long-term remission of atypical HUS with anti-factor H antibodies after cyclophosphamide pulses. Pediatr Nephrol 29:75–83. https://doi.org/10.1007/s00467-013-2558-9
Puraswani M, Khandelwal P, Saini H, Saini S, Gurjar BS, Sinha A, Shende RP, Maiti TK, Singh AK, Kanga U, Ali U, Agarwal I, Anand K, Prasad N, Rajendran P, Sinha R, Vasudevan A, Saxena A, Agarwal S, Hari P, Sahu A, Rath S, Bagga A (2019) Clinical and immunological profile of anti-factor H antibody associated atypical hemolytic uremic syndrome: a nationwide database. Front Immunol 10:1282. https://doi.org/10.3389/fimmu.2019.01282
Dragon-Durey MA, Blanc C, Garnier A, Hofer J, Sethi SK, Zimmerhackl LB (2010) Anti-factor H autoantibody-associated hemolytic uremic syndrome: review of literature of the autoimmune form of HUS. Semin Thromb Hemost 36:633–640. https://doi.org/10.1055/s-0030-1262885
Querfeld U, Weber LT (2018) Mycophenolate mofetil for sustained remission in nephrotic syndrome. Pediatr Nephrol 33:2253–2265. https://doi.org/10.1007/s00467-018-3970-y
Woillard JB, Bader-Meunier B, Salomon R, Ranchin B, Decramer S, Fischbach M, Berard E, Guigonis V, Harambat J, Dunand O, Tenenbaum J, Marquet P, Saint-Marcoux F (2014) Pharmacokinetics of mycophenolate mofetil in children with lupus and clinical findings in favour of therapeutic drug monitoring. Br J Clin Pharmacol 78:867–876. https://doi.org/10.1111/bcp.12392
Loirat C, Frémeaux-Bacchi V (2014) Anti-factor H autoantibody-associated hemolytic uremic syndrome: the earlier diagnosed and treated, the better. Kidney Int 85:1019–1022. https://doi.org/10.1038/ki.2013.447
Acknowledgements
The authors would like to thank Dr Véronique Frémeaux-Bacchi for the genetic explorations performed in the patients.
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Conflict of interest
JB received travel grants and honoraria from Alexion.
ALL received travel grants from Alexion and honararia from Alexion (2013, 2014).
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Matrat, L., Bacchetta, J., Ranchin, B. et al. Pediatric atypical hemolytic–uremic syndrome due to auto-antibodies against factor H: is there an interest to combine eculizumab and mycophenolate mofetil?. Pediatr Nephrol 36, 1647–1650 (2021). https://doi.org/10.1007/s00467-021-05025-8
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00467-021-05025-8