Abstract
Background
Protein energy wasting (PEW) is a common cause of morbidity and mortality in patients with stage 5 chronic kidney disease (CKD 5). Intradialytic parenteral nutrition (IDPN) has been used as a therapy for preventing and treating PEW in children with CKD 5 when other conventional modalities fail. However, not enough data is available to define its effectiveness in treating malnutrition in children. This study aims to investigate potential benefits of IDPN in Egyptian children with CKD 5.
Methods
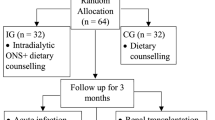
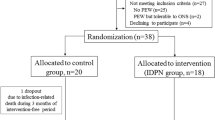
In this prospective, placebo-controlled, parallel-group single blinded study, we enrolled 50 CKD 5 patients; 25 patients (intervention group) received intravenous amino acids (KIDIMN), while 25 patients (control group) received normal saline as placebo, each given during regular dialysis 3 times a week for 9 months. Patients were subjected to nutritional assessment at baseline and 3-, 6-, and 9-month follow-up using height Z-score, hand grip strength (HGS) for muscle power assessment, body composition monitor (BCM) for assessing lean tissue mass (LTM) and adipose tissue mass (ATM), and biochemical measures including serum albumin, serum triglyceride, and serum cholesterol.
Results
When comparing baseline and 9-month follow-up values, significant improvement was recorded in height Z-score, LTM, and serum albumin in the intervention group unlike the control group where no significant changes were recorded.
Conclusion
IDPN is proposed to be an effective method for preventing and treating malnutrition in children with CKD 5. However, further multi-centric studies with larger sample size and longer duration of follow-up are still recommended.



Similar content being viewed by others
References
Fouque D, Kalantar-Zadeh K, Kopple J, Cano N, Chauveau P, Cuppari L, Franch H, Guarnieri G, Ikizler TA, Kaysen G, Lindholm B, Massy Z, Mitch W, Pineda E, Stenvinkel P, Treviño-Becerra A, Wanner C (2008) A proposed nomenclature and diagnostic criteria for protein–energy wasting in acute and chronic kidney disease. Kidney Int 73:391–398
Ikizler TA, Cano NJ, Franch H, Fouque D, Himmelfarb J, Kalantar-Zadeh K, Kuhlmann MK, Stenvinkel P, Ter Wee P, Teta D, Wang AY, Wanner C, International Society of Renal Nutrition and Metabolism (2013) Prevention and treatment of protein energy wasting in chronic kidney disease patients: a consensus statement by the International Society of Renal Nutrition and Metabolism. Kidney Int 84:1096–1107
Carrero JJ, Stenvinkel P, Cuppari L, Ikizler TA, Kalantar-Zadeh K, Kaysen G, Mitch WE, Price SR, Wanner C, Wang AYM, ter Wee P, Franch HA (2013) Etiology of the protein-energy wasting syndrome in chronic kidney disease: a consensus statement from the International Society of Renal Nutrition and Metabolism (ISRNM). J Ren Nutr 23:77–90
Kalantar-Zadeh K, Rhee C, Sim JJ, Stenvinkel P, Anker SD, Kovesdy CP (2013) Why cachexia kills: examining the causality of poor outcomes in wasting conditions. J Cachexia Sarcopenia Muscle 4:89–94
Lacson E Jr, Wang W, Zebrowski B, Wingard R, Hakim RM (2012) Outcomes associated with intradialytic oral nutritional supplements in patients undergoing maintenance hemodialysis: a quality improvement report. Am J Kidney Dis 60:591–600
Rees L, Jones HJ (2013) Nutritional management and growth in children with chronic kidney disease. Pediatr Nephrol 28:527–536
Rees L, Azocar M, Borzych D, Watson AR, Büscher A, Edefonti A, Bilge I, Askenazi D, Leozappa G, Gonzales C, van Hoeck K, Secker D, Zurowska A, Rönnholm K, Bouts AH, Stewart H, Ariceta G, Ranchin B, Warady BA, Schaefer F, International Pediatric Peritoneal Dialysis Network (IPPN) registry (2011) Growth in very young children undergoing chronic peritoneal dialysis. J Am Soc Nephrol 22:2303–2312
Worthington P, Balint J, Bechtold M, Bingham A, Chan LN, Durfee S, Jevenn AK, Malone A, Mascarenhas M, Robinson DT, Holcombe B (2017) When is parenteral nutrition appropriate? JPEN J Parenter Enteral Nutr 41:324–377
Capelli JP, Kushner H, Camiscioli TC, Chen S-M, Torres MA (1994) Effect of intradialytic parenteral nutrition on mortality rates in end-stage renal disease care. Am J Kidney Dis 23:808–816
Chertow GM, Ling J, Lew NL, Lazarus JM, Lowrie EG (1994) The association of intradialytic parenteral nutrition administration with survival in hemodialysis patients. Am J Kidney Dis 24:912–920
Hiroshige K, Iwamoto M, Kabashima N, Mutoh Y, Yuu K, Ohtani A (1998) Prolonged use of intradialysis parenteral nutrition in elderly malnourished chronic haemodialysis patients. Nephrol Dial Transplant 13:2081–2087
Cherry N, Shalansky K (2002) Efficacy of intradialytic parenteral nutrition in malnourished hemodialysis patients. Am J Health Syst Pharm 59:1736–1741
Krause I, Shamir R, Davidovits M, Frishman S, Cleper R, Gamzo Z, Poraz I, Eisenstein B (2002) Intradialytic parenteral nutrition in malnourished children treated with hemodialysis. J Ren Nutr 12:55–59
Sigrist MK, Levin A, Tejani AM (2010) Systematic review of evidence for the use of intradialytic parenteral nutrition in malnourished hemodialysis patients. J Ren Nutr 20:1–7
Roberts HC, Denison HJ, Martin HJ, Patel HP, Syddall H, Cooper C, Sayer AA (2011) A review of the measurement of grip strength in clinical and epidemiological studies: towards a standardised approach. Age Ageing 40:423–429
Cano N, Aparicio M, Brunori G, Carrero J, Cianciaruso B, Fiaccadori E, Lindholm B, Teplan V, Fouque D, Guarnieri G, ESPEN (2009) ESPEN guidelines on parenteral nutrition: adult renal failure. Clin Nutr 28:401–414
Johansen KL, Lee C (2015) Body composition in chronic kidney disease. Curr Opin Nephrol Hypertens 24:268–275
Qamar IU, Levin L, Balfe JW, Balfe JA, Secker D, Zlotkin S (1994) Effects of 3-month amino acid dialysis compared to dextrose dialysis in children on continuous ambulatory peritoneal dialysis. Perit Dial Int 14:34–41
Brem A, Maaz D, Shemin D, Wolfson M (1996) Use of amino acid peritoneal dialysate for one year in a child on CCPD. Perit Dial Int 16:634–636
Bakr AMAEB, Hasaneen BM, Bassiouni DAH (2018) Assessment of nutritional status in children with chronic kidney disease using hand grip strength tool. J Ren Nutr 28:265–269
Cruz-Jentoft AJ, Baeyens JP, Bauer JM, Boirie Y, Cederholm T, Landi F, Martin FC, Michel JP, Rolland Y, Schneider SM, Topinková E, Vandewoude M, Zamboni M, European Working Group on Sarcopenia in Older People (2010) Sarcopenia: European consensus on definition and diagnosis Report of the European working group on sarcopenia in older people. Age Ageing 39:412–423
Wong CS, Hingorani S, Gillen DL, Sherrard DJ, Watkins SL, Brandt JR, Ball A, Stehman-Breen CO (2002) Hypoalbuminemia and risk of death in pediatric patients with end-stage renal disease. Kidney Int 61:630–637
Haskin O, Sutherland SM, Wong CJ (2017) The effect of intradialytic intralipid therapy in pediatric hemodialysis patients. J Ren Nutr 27:132–137
Czekalski S, Hożejowski R, Malnutrition Working Group (2004) Intradialytic amino acids supplementation in hemodialysis patients with malnutrition: results of a multicenter cohort study. J Ren Nutr 14:82–88
Joannidis M, Rauchenzauner M, Leiner B, Rosenkranz A, Ebenbichler C, Laimer M, Tatarczyk T, Meusburger E, Mayer G (2008) Effect of intradialytic parenteral nutrition in patients with malnutrition–inflammation complex syndrome on body weight, inflammation, serum lipids and adipocytokines: results from a pilot study. Eur J Clin Nutr 62:789–795
Cano NJ, Fouque D, Roth H, Aparicio M, Azar R, Canaud B, Chauveau P, Combe C, Laville M, Leverve XM, French Study Group for Nutrition in Dialysis (2007) Intradialytic parenteral nutrition does not improve survival in malnourished hemodialysis patients: a 2-year multicenter, prospective, randomized study. J Am Soc Nephrol 18:2583–2591
Marsen TA, Beer J, Mann H; German IDPN-Trial group (2017) Intradialytic parenteral nutrition in maintenance hemodialysis patients suffering from protein-energy wasting. Results of a multicenter, open, prospective, randomized trial. Clin Nutr 36:107–117
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
The study protocol was submitted to the institution research board of the Faculty of Medicine, Mansoura University, for approval. The protocol was granted approval in December 2016, IRB Code number: MS/16.07.46. Written consent was taken from parents, and patients in the adolescent age group additionally gave consent.
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
El-Serw, H.ES.S., Bassiouni, D.A.R.H., Al-Wakeil, A.A. et al. Efficacy of intradialytic amino acids on nutritional status in children with stage 5 chronic kidney disease. Pediatr Nephrol 36, 1561–1569 (2021). https://doi.org/10.1007/s00467-020-04806-x
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00467-020-04806-x