Abstract
Background
Hyperuricemia might induce additional renal damage in children with hemolytic uremic syndrome related to Shiga toxin-producing Escherichia coli (STEC-HUS). A few case reports have shown rasburicase to be effective in decreasing serum uric acid (UA) and improving renal function. However, there is only one report on the use of rasburicase in a child with STEC-HUS, which shows satisfactory results. We describe here the safety and efficacy of rasburicase in nine additional cases.
Case-diagnosis/treatment
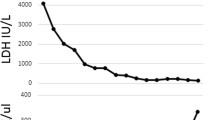
Data from 9 children (5 females, median age 2 years) who received rasburicase were reviewed. At admission, 6 were dehydrated and 3 euvolemic. Dehydrated patients received saline solution and afterwards, as well as for those initially euvolemic, we aimed to keep a neutral fluid balance. Despite this, urine output did not increase. Baseline creatinine was 3.35 mg/dL (1.47–9.1) and UA 11.4 mg/dL (8.3–19.2). A single dose of rasburicase (0.2 mg/kg) was given 6–8 h after admission, which reduced UA levels to 1.8 mg/dL (0.3–5, p = 0.009) on the next day. However, renal parameters worsen and dialysis had to be initiated. Then, while still on dialysis, a UA rebound occurred in all cases reaching a peak of 8.9 mg/dL (4.5–13.8). Just after a steady increase in urine output, a sustained decline in UA levels concomitantly occurred with an improvement in renal function. At discharge, all patients reached normal UA levels. No side effects were recorded.
Conclusions
Administration of rasburicase in children with STEC-HUS was safe but failed to provide any significant benefit despite fall in serum UA levels.
Similar content being viewed by others
References
Ardissino G, Tel F, Possenti I, Testa S, Consonni D, Paglialonga F, Salardi S, Borsa-Ghiringhelli N, Salice P, Tedeschi S, Castorina P, Colombo RM, Arghittu M, Daprai L, Monzani A, Tozzoli R, Brigotti M, Torresani E (2016) Early volume expansion and outcomes of hemolytic uremic syndrome. Pediatrics 137(1)
Balestracci A, Meni Battaglia L, Toledo I, Martin SM, Alvarado C (2018) Blood urea nitrogen to serum creatinine ratio as a prognostic factor in diarrhea-associated hemolytic uremic syndrome: a validation study. Eur J Pediatr 177:63–68
Khalid M, Andreoli S (2019) Extrarenal manifestations of the hemolytic uremic syndrome associated with Shiga toxin-producing Escherichia coli (STEC HUS). Pediatr Nephrol 34(12):2495–2507
O’Regan S, Rousseau E (1998) Hemolytic uremic syndrome: urate nephropathy superimposed on an acute glomerulopathy? An hypothesis. Clin Nephrol 30:207–210
Hobbs DJ, Steinke JM, Chung JY, Barletta GM, Bunchman TE (2010) Rasburicase improves hyperuricemia in infants with acute kidney injury. Pediatr Nephrol 25:305–309
Hooman N, Otukesh H (2011) Single dose of rasburicase for treatment of hyperuricemia in acute kidney injury: a report of 3 cases. Iran J Kidney Dis 5:130–132
Acosta AA, Hogg RJ (2012) Rasburicase for hyperuricemia in hemolytic uremic syndrome. Pediatr Nephrol 27:325–329
Gopakumar KG, Thankamony P, Seetharam S, P K (2017) Treatment of tumor lysis syndrome in children with leukemia/lymphoma in resource-limited settings—efficacy of a fixed low-dose rasburicase. Pediatr Hematol Oncol 34(4):206–211
Ejaz AA, Mu W, Kang DH, Roncal C, Sautin YY, Henderson G, Tabah-Fisch I, Keller B, Beaver TM, Nakagawa T, Johnson RJ (2007) Could uric acid have a role in acute renal failure? Clin J Am Soc Nephrol 2(1):16–21
Ejaz AA, Johnson RJ, Shimada M, Mohandas R, Alquadan KF, Beaver TM, Lapsia V, Dass B (2019) The role of uric acid in acute kidney injury. Nephron 142(4):275–283
Ake JA, Jeacic S, Ciol MA, Watkins SL, Murray KF, Christie DL, Klein EJ, Tarr PI (2005) Relative nephroprotection during Escherichia coli O157: H7 infections: association with intravenous volume expansion. Pediatrics 115:e673–e680
Wilson FP, Berns JS (2012) Onco-nephrology: tumor lysis syndrome. Clin J Am Soc Nephrol 7(10):1730–1739
Sinha R, Dugar P (2013) Rasburicase for acute kidney injury. Indian Pediatr 50(11):1051–1052
Balestracci A, Martin SM, Toledo I (2012) Hyperuricemia in children with post-diarrheal hemolytic uremic syndrome. Pediatr Nephrol 27(8):1421–1422
Dinnel J, Moore BL, Skiver BM, Bose P (2015) Rasburicase in the management of tumor lysis: an evidence-based review of its place in therapy. Core Evid 10:23–38
Patel C, Wilson CP, Ahmed N, Hattab Y (2019) acute uric acid nephropathy following epileptic seizures: case report and review. Case Rep Nephrol 2019:4890287
Yu X, Liu L, Nie X, Li J, Zhang J, Zhao L, Wang X (2017) The optimal single-dose regimen of rasburicase for management of tumour lysis syndrome in children and adults: a systematic review and meta-analysis. J Clin Pharm Ther 42(1):18–26
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethics
The study was performed in accordance with the ethical standards of the institutional research and ethics committee.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Balestracci, A., Meni Battaglia, L., Martin, S.M. et al. Rasburicase in hemolytic uremic syndrome related to Shiga toxin-producing Escherichia coli: a report of nine cases. Pediatr Nephrol 35, 1133–1137 (2020). https://doi.org/10.1007/s00467-020-04528-0
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00467-020-04528-0