Abstract
Background
The endocapillary proliferative (EP) lesion is not included in the International Study of Kidney Disease in Children (ISKDC) pathological classification of Henoch-Schönlein purpura nephritis (HSPN). The main objective of the study was to determine the pathological importance of EP in the development of proteinuria in children with Henoch-Schönlein purpura nephritis (HSPN).
Methods
The pathological features of 148 HSPN children with nephrotic-range proteinuria were investigated retrospectively. Urinary IgG, transferrin, and albumin levels were measured by immunonephelometry. The correlations between EP lesion and 24-h proteinuria, urinary IgG, urinary transferrin, and urinary albumin were analyzed. Renal biopsy specimens were immunohistochemically stained for nephrin and podocalyxin.
Results
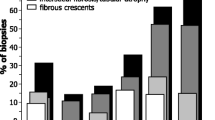
Of the total 581 cases of children with HSPN who underwent renal biopsy, 148 cases (25.5%) presented with nephrotic-range proteinuria. The pathological types of HSPN with nephrotic-range proteinuria were categorized as IIb, IIIa, IIIb, IIIb with diffuse EP, IVb, pure focal EP type, and pure diffuse EP type. Among these types, pure diffuse EP type accounted for 7.4%. The levels of 24-h proteinuria and urinary albumin were the highest in pure diffuse EP type among all pathological types, and the percentage of EP correlated with 24-h proteinuria and urinary albumin levels. 24-h proteinuria was significantly higher in pure diffuse EP type relative to HSPN IIb type, and significantly higher in IIIb with EP, compared with HSPN IIIb. Nephrin, but not podocalyxin, was downregulated in EP segment.
Conclusions
EP is an independent pathogenic factor in HSPN with nephrotic-range proteinuria. Downregulation of nephrin in EP segment is a potential molecular mechanism of nephrotic-range proteinuria. Albumin is the major urinary protein component in HSPN with EP.




Similar content being viewed by others
References
Davin JC, Coppo R (2014) Henoch-Schonlein purpura nephritis in children. Nat Rev Nephrol 10:563–573
Rennke HG (1994) How does glomerular epithelial cell injury contribute to progressive glomerular damage. Kidney Int 45:S58–S63
Soylemezoglu O, Ozkaya O, Ozen S, Bakkaloglu A, Dusunsel R, Peru H, Cetinyurek A, Yildiz N, Donmez O, Buyan N, Mir S, Arisoy N, Gur-Guven A, Alpay H, Ekim M, Aksu N, Soylu A, Gok F, Poyrazoglu H, Sonmez F (2009) Henoch-Schonlein nephritis: a nationwide study. Nephron Clin Pract 112:c199–c204
Counahan R, Winterborn MH, White RH, Heaton JM, Meadow SR, Bluett NH, Swetschin H, Cameron JS, Chantler C (1977) Prognosis of Henoch-Schonlein nephritis in children. Br Med J 2:11–14
Roberts IS, Cook HT, Troyanov S, Alpers CE, Amore A, Barratt J, Berthoux F, Bonsib S, Bruijn JA, Cattran DC, Coppo R, D'Agati V, D'Amico G, Emancipator S, Emma F, Feehally J, Ferrario F, Fervenza FC, Florquin S, Fogo A, Geddes CC, Groene HJ, Haas M, Herzenberg AM, Hill PA, Hogg RJ, Hsu SI, Jennette JC, Joh K, Julian BA, Kawamura T, Lai FM, Li LS, Li PK, Liu ZH, Mackinnon B, Mezzano S, Schena FP, Tomino Y, Walker PD, Wang H, Weening JJ, Yoshikawa N, Zhang H (2009) The Oxford classification of IgA nephropathy: pathology definitions, correlations, and reproducibility. Kidney Int 76:546–556
Li Y, Wang J, Zhu X, Feng Q, Li X, Feng X (2012) Urinary protein markers predict the severity of renal histological lesions in children with mesangial proliferative glomerulonephritis. BMC Nephrol 13:29
Chen S, Tang Z, Zhang Y, Liu Z, Zhang H, Hu W (2013) Significance of histological crescent formation in patients with diffuse proliferative lupus nephritis. Am J Nephrol 38:445–452
Fu G, He XQ, Hu YX, Yu LF, Yang Q, Zhuang JQ (2016) Analysis of clinicopathology and outcome of childhood Henoch-Schonlein purpura nephritis with endocapillary proliferation. J Wenzhou Med Univ 46:330–334
Fu H, Mao J, Xu Y, Gu W, Zhu X, Liu A (2016) Clinical features and outcomes of diffuse endocapillary proliferation Henoch-Schönlein purpura nephritis in children. Clinics 71:550–554
Song CD, Ding Y, Zhai ZG, Zhai WS, Ren XQ, Guo QY, Zhang X, Yang M, Zhang J (2016) The clinical and pathological features of capillary proliferative purpura nephritis in 19 children. J Clin Pediatr 34:414–417
Zhao S, Huang SM, Zhang WZ, Bao HY, Wu HM, Zhang AH, Chen Y, Han Y, Zhao F (20l0) Analysis of clinicopathology and prognosis of childhood HenochSchonlein purpura nephritis with diffused endothelial cell proliferation. Chin J Nephrol 26:416–421
Beirne GJ, Wagnild JP, Zimmerman SW, Macken PD, Burkholder PM (1977) Idiopathic crescentic glomerulonephritis. Medicine (Baltimore) 56:349–381
Liu LJ, Li GT, Zhou Y, Lv JC, Zhang H (2010) Clinicopathologic features and outcomes in endocapillary proliferative IgA nephropathy. Nephron Clin Pract 115:c161–c167
Shankland SJ (2006) The podocyte’s response to injury: role in proteinuria and glomerulosclerosis. Kidney Int 69:2131–2147
Raij L, Tian R, Wong JS, He JC, Campbell KN (2016) Podocyte injury: the role of proteinuria, urinary plasminogen, and oxidative stress. Am J Physiol Ren Physiol 311:F1308–F1317
Doublier S, Ruotsalainen V, Salvidio G, Lupia E, Biancone L, Conaldi PG, Reponen P, Tryggvason K, Camussi G (2000) Nephrin redistribution on podocytes is a potential mechanism nephritic syndrome. J Am Pathol 158:1723–1731
Kerjaschki D, Sharkey DJ, Farquhar MG (1984) Identification and characterization of podocalyxin-the major sialoprotein of the renal glomerular epithelial cell. J Cell Biol 98:1591–1596
Koop K, Eikmans M, Baelde HJ, Kawachi H, De Heer E, Paul LC, Bruijn JA (2003) Expression of podocyte-associated molecules in acquired human kidney diseases. J Am Soc Nephrol 14:2063–2071
Wang SX, Rastaldi MP, Patari A, Ahola H, Heikkila E, Holthofer H (2002) Patterns of nephrin and a new proteinuria-associated protein expression in human renal diseases. Kidney Int 61:141–147
Kavoura E, Gakiopoulou H, Paraskevakou H, Marinaki S, Agrogiannis G, Stofas A, Boletis I, Patsouris E, Lazaris AC (2011) Immunohistochemical evaluation of podocalyxin expression in glomerulopathies associated with nephrotic syndrome. Hum Pathol 42:227–235
Huang D, Wu X, Zheng W, Peng X, He X, Mo S (2012) Podocalyxin expression in renal tissues and correlation with the number of urinary podocytes in children with Henoch-Schonlein purpura nephritis. Zhong Nan Da Xue Xue Bao Yi Xue Ban 37:161–167
Ohara N, Hanyu O, Hirayama S, Nakagawa O, Aizawa Y, Ito S, Sone H (2014) Hypertension increases urinary excretion of immunoglobulin G, ceruloplasmin and transferrin in normoalbuminuric patients with type 2 diabetes mellitus. J Hypertens 32:432–438
Fujita E, Nagahama K, Shimizu A, Aoki M, Higo S, Yasuda F, Mii A, Fukui M, Kaneko T, Tsuruoka S (2015) Glomerular capillary and endothelial cell injury is associated with the formation of necrotizing and crescentic lesions in crescentic glomerulonephritis. J Nippon Med Sch 82:27–35
Kasahara T, Hayakawa H, Okubo S, Okugawa T, Kabuki N, Tomizawa S, Uchiyama M (2001) Prognosis of acute poststreptococcal glomerulonephritis (APSGN) is excellent in children, when adequately diagnosed. Pediatr Int 43:364–367
Kambham N (2012) Postinfectious glomerulonephritis. Adv Anat Pathol 19:338–347
Peh CA (2013) Commentary on the KDIGO clinical practice guideline for glomerulonephritis. Nephrology (Carlton) 18:483–484
Funding
This study was funded by independent innovation and applied basic research project of university basic scientific research business in 2014 (No. 2014KYYWF-ZZCX2-03) and innovation team for treatment of Henoch-Schönlein purpura nephritis in children by Integrated Chinese and Western medicine methods (No. 18IRTSTHN028).
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Conflicts of interest
The authors declare that they have no conflict of interest.
Informed consent
For this type of study formal consent is not required.
Rights and permissions
About this article
Cite this article
Yang, Xq., Huang, Yj., Zhai, Ws. et al. Correlation between endocapillary proliferative and nephrotic-range proteinuria in children with Henoch-Schönlein purpura nephritis. Pediatr Nephrol 34, 663–670 (2019). https://doi.org/10.1007/s00467-018-4134-9
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00467-018-4134-9