Abstract
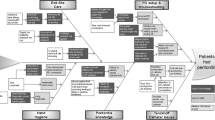
Peritonitis is a leading cause of hospitalizations, morbidity, and modality change in pediatric chronic peritoneal dialysis (CPD) patients. Despite guidelines published by the International Society for Peritoneal Dialysis aimed at reducing the risk of peritonitis, registry data have revealed significant variability in peritonitis rates among centers caring for children on CPD, which suggests variability in practice. Improvement science methods have been used to reduce a variety of healthcare-associated infections and are also being applied successfully to decrease rates of peritonitis in children. A successful quality improvement program with the goal of decreasing peritonitis will not only include primary drivers directly linked to the outcome of peritonitis, but will also direct attention to secondary drivers that are important for the achievement of primary drivers, such as health literacy and patient and family engagement strategies. In this review, we describe a comprehensive improvement science model for the reduction of peritonitis in pediatric patients on CPD.

Similar content being viewed by others
References
Alexander SR, Warady BA (2004) The demographics of dialysis in children, in pediatric dialysis. In: Warady BA, Schaefer FS, Fine RN, Alexander SR (eds) Pediatric dialysis. Kluwer Academic Publishers, Dordrecht, pp 35–46
United States Renal Data System (2015) 2015 USRDS annual data report: epidemiology of kidney disease in the United States. National Institutes of Health, National Institute of Diabetes and Digestive and Kidney Diseases, Bethesda
North American Pediatric Renal Trials andCollaborative Studies (2011) NAPRTCS 2011 annual dialysis report. Available at: web.emmes.com/study/ped/announce.htm. Accessed 1 June 2016
Schaefer F, Feneberg R, Aksu N, Donmez O, Sadikoglu B, Alexander SR, Mir S, Ha IS, Fischbach M, Simkova E, Watson AR, Moller K, von Baum H, Warady BA (2007) Worldwide variation of dialysis-associated peritonitis in children. Kidney Int 72:1374–1379
Children’s Hospital Association. Standardizing Care to Improve Outcomes in Pediatric ESRD Collaborative. Children’s Hospital Association. Available at: www.childrenshospitals.org/Programs-and-Services/Quality-Improvement-and-Measurement/Collaboratives/SCOPE. Accessed 6 Aug 2016
Coyte PC, Young LG, Tipper BL, Mitchell VM, Stoffman PR, Willumsen J, Geary DF (1996) An economic evaluation hospital-based hemodialysis and home-based peritoneal dialysis for pediatric patients. Am J Kidney Dis 27:557–565
Warady BA, Bakkaloglu S, Newland J, Cantwell M, Verrina E, Neu A, Chadha V, Yap HK, Schaefer F (2012) Consensus guidelines for the prevention and treatment of catheter-related infections and peritonitis in pediatric patients receiving peritoneal dialysis: 2012 update. Perit Dial Int 32[Suppl 2]:S32–86
Li PD, Szeto CC, Piraino B, de Arteaga J, Fan S, Figueiredo AE, Fish DN, Goffin E, Kim YL, Salzer W, Struijk DG, Teitelbaum I, Johnson DW (2016) ISPD Peritonitis recommendations: 2016 update on prevention and treatment. Perit Dial Int 36:481–508
Neu AM, Miller MR, Stuart J, Lawlor J, Richardson T, Martz K, Rosenberg C, Newland J, McAfee N, Begin B, Warady BA, Collaborative Participants SCOPE (2014) Design of the standardizing care to improve outcomes in pediatric end stage renal disease collaborative. Pediatr Nephrol 29:1477–1484
Rinke ML, Chen AR, Bundy DG, Colantuoni E, Fratino L, Drucis KM, Panton SY, Kokoszka M, Budd AP, Milstone AM, Miller MR (2012) Implementation of a central line maintenance care bundle in hospitalized pediatric oncology patients. Pediatrics 130:e996–e1004
Bundy DG, Gaur AH, Billett AL, He B, Colantuoni EA, Miller MR, Children’s Hospital Association Hematology/Oncology CLABSI Collaborative (2014) Preventing CLABSIs among pediatric hematology/oncology inpatients: national collaborative results. Pediatrics 134:e1678–1685
Wilson MZ, Deeter D, Rafferty C, Comito MM, Hollenbeak CS (2014) Reduction of central line-associated bloodstream infections in a pediatric hematology/oncology population. Am J Med Qual 29:484–490
Miller MR, Griswold M, Harris JM 2nd, Yenokyan G, Huskins WC, Moss M, Rice TB, Ridling D, Campbell D, Margolis P, Muething S, Brilli RJ (2010) Decreasing PICU catheter-associated bloodstream infections: NACHRI’s quality transformation efforts. Pediatrics 125:206–213
Miller MR, Niedner MF, Huskins WC, Colantuoni E, Yenokyan G, Moss M, Rice TB, Ridling D, Campbell D, Brilli RJ, National Association of Children’s Hospitals and Related Institutions Pediatric Intensive Care Unit Central Line-Associated Bloodstream Infection Quality Transformation (2011) Reducing PICU central line-associated bloodstream infections: 3-year results. Pediatrics 128:e1077–e1038
Wagar SS, Nigh K, Sisler L, Fanning M, Tancin S, Brozik E, Jones R, Briggs F, Keller L, LaSala PR, Krautz S, Khakoo R (2016) Multidisciplinary performance improvement team for reducing health care-associated Clostridium difficile infection. Am J Infect Control 44:352–354
Johnson MP, Kim SJ, Langstraat CL, Jain S, Habermann EB, Wentink JE, Grubbs PL, Nehring SA, Weaver AL, McGree ME, Cima RR, Dowdy SC, Bakkum-Gamez JN (2016) Using bundled interventions to reduce surgical site infection after major gynecologic cancer surgery. Obstet Gynecol 127:1135–1144
Taylor MJ, McNicholas C, Nicolay C, Darzi A, Bell D, Reed JE (2014) Systematic review of the application of the plan-do-study-act method to improve quality in healthcare. BMJ Qual Saf 23:290–298
Associates in Process Improvement (2016). Available at: http://www.apiweb.org/. Accessed 5 Sept 2016
U.S. Department of Health and Human Services Centers for Medicare & Medicaid Services Center for Medicare and Medicaid Innovation Learning and Diffusion Group (2013) Defining and using aims and drivers for improvement: a how-to guide.” Available at: https://innovation.cms.gov/files/x/hciatwoaimsdrvrs.pdf. Accessed 7 Aug 2016
Gadola L, Poggi C, Poggio M, Saez L, Ferrari A, Romero J, Fumero S, Ghelfi G, Chifflet L, Borges PL (2013) Using a multidisciplinary training program to reduce peritonitis in peritoneal dialysis patients. Perit Dial Int 33:38–45
Nouwen JL, Fieren MW, Snijders S, Verbrugh HA, van Belkum A (2005) Persistent (not intermittent) nasal carriage of Staphylococcus aureus is the determinant of CPD-related infections. Kidney Int 67:1084–1092
Kopriva-Altfahrt G, König P, Mündle M, Prischl F, Roob JM, Wiesholzer M, Vychytil A, Austrian Study Group for Prevention of Peritoneal Catheter-Associated Infections, Arneitz K, Karner A, Artes R, Wolf E, Auinger M, Pawlak A, Fraberger J, Hofbauer S, Galvan G, Salmhofer H, Pichler B, Wazel M, Gruber M, Thonhofer A, Hager A, Malajner S, Heiss S, Braunsteiner T, Zweiffler M, König P, Rudnicki M, Kogler R, Kohlhauser D, Wiesinger T, Kopriva-Altfahrt G, Moser E, Kotanko P, Loibner H, Nitz H, Miska HJ, Wenzel R, Wölfer M, Mündle M, Breuss H, Hölzl B, Prischi F, Schmekal B, Riener EM, Roob JM, Wonisch W, Vikydal R, Vychytil A, Frank B, Wieser C, Wiesholzer M, Pokorny K (2009) Exit-site care in Austrian peritoneal dialysis centers—a nationwide survey. Perit Dial Int 29:330–339
Hagen SM, Lafranca JA, IJzermans JN, Dor FJ (2014) A systematic review and meta-analysis of the influence of peritoneal dialysis catheter type on complication rate and catheter survival. Kidney Int 85:920–932
Lo WK, Lui SL, Li FK, Choy BY, Lam MF, Tse KC, Yip TP, Ng FS, Lam SC, Chu WL, Cheng SW (2003) A prospective randomized study on three different peritoneal dialysis catheters. Perit Dial Int 23[Suppl 2]:S127–131
Strippoli GF, Tong A, Johnson D, Schena FP, Craig JC (2004) Catheter-related interventions to prevent peritonitis in peritoneal dialysis: a systematic review of randomized, controlled trials. J Am Soc Nephrol 15:2735–2746
Copeland CR, Blaszak RT, Tolleson JS, Saad DF, Jackson RJ, Smith SD, Kokosk ER (2008) Laparoscopic Tenckhoff catheter placement in children using a securing suture in the pelvis: comparison to the open approach. J Pediatr Surg 43:2256–2259
Mattioli G, Castagnetti M, Verrina E, Trivelli A, Torre M, Jasonni V, Perfumo F (2007) Laparoscopic-assisted peritoneal dialysis catheter implantation in pediatric patients. Urology 69:1185–1189
Cribbs RK, Greenbaum LA, Heiss KF (2010) Risk factors for early peritoneal dialysis catheter failure in children. J Pediatr Surg 45:585–589
Wright M, Bel’eed JB, Eadington D, Sellars L, Farr M (1999) Randomized prospective comparison of laparoscopic and open peritoneal dialysis catheter insertion. Perit Dial Int 19:372–375
Jwo SC, Chen KS, Lee CC, Chen HY (2010) Prospective randomized study for comparison of open surgery with laparoscopic-assisted placement of Tenckhoff peritoneal dialysis catheter—a single center experience and literature review. J Surg Res 159:489–496
Sardegna KM, Beck AM, Strife CF (1998) Evaluation of peri-operative antibiotics at the time of dialysis catheter placement. Pediatr Nephrol 12:149–152
Strippoli GF, Tong A, Johnson D, Schena FP, Craig JC (2004) Antimicrobial agents to prevent peritonitis in peritoneal dialysis: a systematic review of randomized controlled trials. Am J Kidney Dis 44:591–603
Gadallah MF, Ramdeen G, Mignone J, Patel D, Mitchell L, Tatro S (2000) Role of preoperative antibiotic prophylaxis in preventing postoperative peritonitis in newly placed peritoneal dialysis catheters. Am J Kidney Dis 36:1014–1019
Prowant BF, Twardowski ZJ (1996) Recommendations for exit care. Perit Dial Int 16[Suppl 3]:S94–S99
Twardowski ZJ, Prowant BF (1996) Exit-site healing post catheter implantation. Perit Dial Int 16[Suppl 3]:S51–S70
Luzar MA, Brown CB, Balf D, Hill L, Issad B, Monnier B, Moulart J, Sabatier JC, Wauquier JP, Peluso F (1990) Exit-site care and exit-site infection in continuous ambulatory peritoneal dialysis (CAPD): results of a randomized multicenter trial. Perit Dial Int 10:25–29
Jones LL, Tweedy L, Warady BA (1995) The impact of exit-site care and catheter design on the incidence of catheter-related infections. Adv Perit Dial 11:302–305
Mendoza-Guevara L, Castro-Vazquez F, Aguilar-Kitsu A, Morales-Nava A, Rodriguez-Leyva F, Sanchez-Barbosa JL (2007) Amuchina 10% solution, safe antiseptic for preventing infections of exit-site of Tenckhoff catheters, in the pediatric population of a dialysis program. Contrib Nephrol 154:139–144
van Esch S, Krediet RT, Struijk DG (2014) 32 years’ experience of peritoneal dialysis-related peritonitis in a university hospital. Perit Dial Int 34:162–170
Mahajan S, Tiwari SC, Kalra V, Bhowmik DM, Agarwal SK, Dash SC, Kumar P (2005) Effect of local mupirocin application on exit-site infection and peritonitis in an Indian peritoneal dialysis population. Perit Dial Int 25:473–477
Uttley L, Vardhan A, Mahajan S, Smart B, Hutchison A, Gokal R (2004) Decrease in infections with the introduction of mupirocin cream at the peritoneal dialysis catheter exit site. J Nephrol 17:242–245
Bernardini J, Bender F, Florio T, Sloand J, Palmmontalbano L, Fried L, Piraino B (2005) Randomized, double-blind trial of antibiotic exit site cream for prevention of exit site infection in peritoneal dialysis patients. J Am Soc Nephrol 16:539–545
Wong PN, Tong GM, Wong YY, Lo KY, Chan SF, Lo MW, Lo KC, Ho LY, Tse CW, Mak SK, Wong AK (2016) Alternating mupirocin/gentamicin is associated with increased risk of fungal peritonitis as compared with gentamicin alone—results of a randomized open-label controlled trial. Perit Dial Int 36:340–346
McQuillan RF, Chiu E, Nessim S, Lok CE, Roscoe JM, Tam P, Jassal SV (2012) A randomized controlled trial comparing mupirocin and polysporin triple ointments in peritoneal dialysis patients: the MP3 Study. Clin J Am Soc Nephrol 7:297–303
Firank C, Guest S (2011) Hand hygiene in peritoneal dialysis. Perit Dial Int 31:399–408
World Health Organization (2009) WHO guidelines on hand hygiene in heath care. World Health Organization, Geneva. Available at: http://apps.who.int/iris/bitstream/10665/44102/1/9789241597906_eng.pdf. Accessed 5 Aug 2016
Sethna CB, Bryant K, Munshi R, Warady BA, Richardson T, Lawlor J, Newland JG, Neu A (2016) Risk factors for and outcomes of catheter-associated peritonitis in children: the SCOPE collaborative. Clin J Am Soc Nephrol 11:1590–1596
Bender FH, Bernardini J, Piraino B (2006) Prevention of infectious complications in peritoneal dialysis: best demonstrated practices. Kidney Int Suppl 103:S44–S54
Figueiredo AE, Bernardini J, Bowes E, Hiramatsu M, Price V, Su C, Walker R, Brunier G (2016) ISPD guidelines/recommendations: a syllabus for teaching peritoneal dialysis to patients and caregivers. Perit Dial Int. doi:10.3747/pdi.2015.00277
Lloyd A, Tangri N, Shafer LA, Rigatto C, Perl J, Komeda P, Sood MM (2013) The risk of peritonitis after an exit site infection: a time-matched, case–control study. Nephrol Dial Transplant 28:1915–1921
Schaefer F, Klaus G, Müeller–Wiefel DE, Mehls O, The Mid- European Pediatric Peritoneal Dialysis Study Group (MEPPS) (1999) Intermittent versus continuous intraperitoneal glycopeptide/ceftazidime treatment in children with peritoneal dialysis-associated peritonitis. J Am Soc Nephrol 10:136–145
Bernardini J, Price V, Figueiredo A, Riemann A, Leung D (2006) International survey of peritoneal dialysis training programs. Perit Dial Int 26:658–663
Chow KM, Szeto CC, Law MC, Fun Fung JS, Kam-Tao Li P (2007) Influence of peritoneal dialysis training nurses’ experience on peritonitis rates. Clin J Am Soc Nephrol 2:647–652
Hall G, Bogan A, Dreis S, Duffy A, Greene S, Kelley K, Lizak H, Nabut J, Schinker V, Schwartz N (2004) New directions in peritoneal dialysis patient training. Nephrol Nurs J 31(149–154):159–163
Bernardini J, Price V, Figueiredo A, International Society for Peritoneal Dialysis (ISPD) Nursing Liaison Committee (2006) Peritoneal dialysis patient training, 2006. Perit Dial Int 26:625–632
Ellis EN, Blaszak C, Wright S, Van Lierop A (2012) Effectiveness of home visits to pediatric peritoneal dialysis patients. Perit Dial Int 32:419–423
Bordin G, Casati M, Sicolo N, Zuccherato N, Eduati V (2007) Patient education in peritoneal dialysis: an observational study in Italy. J Ren Care 33:165–171
Verger C, Duman M, Durand PY, Veniez G, Fabre E, Ryckelynck JP (2007) Influence of autonomy and type of home assistance on the prevention of peritonitis in assisted automated peritoneal dialysis patients. An analysis of data from the French Language Peritoneal Dialysis Registry. Nephrol Dial Transplant 22:1218–1223
Sayed SA, Abu-Aisha H, Ahmed ME, Elamin S (2013) Effect of the patient’s knowledge on peritonitis rates in peritoneal dialysis. Perit Dial Int 33:362–366
Bernardini J, Piraino B (1998) Compliance in CAPD and CCPD patients as measured by supply inventories during home visits. Am J Kidney Dis 31:101–107
Ozturk S, Yucel L, Guvenc S, Ekiz S, Kazancioglu R (2009) Assessing and training patients on peritoneal dialysis in their own homes can influence better practice. J Ren Care 35:141–146
U.S. Department of Health and Human Services, Centers for Medicare & Medicaid Services (2008) Conditions for coverage for end-stage renal disease facilities; final rule. Federal Register 73/April 15, 2008. Available at: www.cms.hhs.gov/CFCsAndCoPs/downloads/ESRDfinalrule0415.pdf. Accessed 11 Aug 2016
Berkman ND, Davis TC, McCormack L (2010) Health literacy: what is it? J Health Commun 15[Suppl 2]:9–19
Berkman ND, Sheridan SL, Donahue KE, Halpern DJ, Viera A, Crotty K (2011) Low health literacy and health outcomes: an updated systematic review. Ann Intern Med 55:97–107
Green JA, Mor MK, Shields AM, Sevick MA, Arnold RM, Palevsky PM, Fine MJ, Weisbord SD (2013) Associations of health literacy with dialysis adherence and health resource utilization in patients receiving maintenance hemodialysis. Am J Kidney Dis 62:73–80
Wright JA, Wallston KA, Elasy TA, Ikizler TA, Cavanaugh KL (2011) Development and results of a kidney disease knowledge survey given to patients with CKD. Am J Kidney Dis 57:387–395
Cavanaugh KL, Wingard RL, Hakim RM, Eden S, Shintani A, Wallston KA, Huizinga MM, Elasy TA, Rothman RL, Ikizler TA (2010) Low health literacy associates with increased mortality in ESRD. J Am Soc Nephrol 21:1979–1985
Yin HS, Johnson M, Mendelsohn AL, Abrams MA, Sanders LM, Dreyer BP (2009) The health literacy of parents in the United States: a nationally representative study. Pediatrics 124[Suppl 3]:S289–S298
Sanders LM, Federico S, Klass P, Abrams MA, Dreyer B (2009) Literacy and child health: a systematic review. Arch Pediatr Adolesc Med 163:131–140
DeWalt DA, Hink A (2009) Health literacy and child health outcomes: a systematic review of the literature. Pediatrics 124[Suppl 3]:S265–S274
Ferris ME, Mahan JD (2009) Pediatric chronic kidney disease and the process of health care transition. Semin Nephrol 29:435–444
Ferris M, Patel UD, Massengill S, Gipson D, Conley W, Layton JB, Nagaraj S, Primack W (2008) Pediatric chronic kidney disease in North Carolina. N C Med J 69:208–214
Maurer M, Dardess P, Carman, KL, Frazier K, Smeeding L (2012) Guide to patient and family engagement: environmental scan report. American Institutes for Research publication no. 12-0042-EF. Agency for Healthcare Research and Quality, Rockville
Davis S, Berkson S, Gaines ME, Prajapati P, Schwab W, Pandhi N, Edgman-Levitan S (2016) Implementation science workshop: engaging patients in team-based practice redesign - critical reflections on program design. J Gen Intern Med 31:688–695
Health Canada (2000) Health Canada policy toolkit for public involvement in decision making. Available at: www.hc-sc.gc.ca/ahc-asc/pubs/_public-consult/2000decision/index-eng.php. Accessed 5 Aug 2016
White S, Vinet A (2010) Partnering with patients to improve peritonitis rates. CANNT J 20:38–41
University of Wisconsin. HipxChange. Patient engagement toolkits. Available at: https://www.hipxchange.org/browse. Accessed 8 Aug 2016
Neu AM, Richardson T, Lawlor J, Stuart J, Newland J, McAfee N, Warady BA, Collaborative Participants SCOPE (2016) Implementation of standardized follow-up care significantly reduces peritonitis in children on chronic peritoneal dialysis. Kidney Int 89:1346–1354
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare that they have no conflict of interest.
Additional information
Answers to questions:
1: d
2: d
3: d
4: b
5: b
Rights and permissions
About this article
Cite this article
Redpath Mahon, A., Neu, A.M. A contemporary approach to the prevention of peritoneal dialysis-related peritonitis in children: the role of improvement science. Pediatr Nephrol 32, 1331–1341 (2017). https://doi.org/10.1007/s00467-016-3531-1
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00467-016-3531-1