Abstract
Background
Electrical stimulation has been used as an alternative therapy for adult urinary syndromes and for children with constipation. We have evaluated the safety and efficacy of interferential (IF) electrical stimulation in children with nocturnal enuresis (NE).
Methods
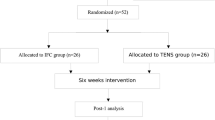
This was a randomized clinical trial in which 54 children (23 girls, 31 boys) aged 6–14 years with primary NE were recruited and randomly divided into two groups. Children in the control group underwent standard urotherapy only (hydration, scheduled voiding, toilet training, diet), whereas children in the IF group (cases) were treated with standard urotherapy + 15 sessions of IF electrical stimulation for 20 min twice per week. An improvement score was calculated to identify relative decrease in wet nights after the treatment for each child. All children were followed for 1 year.
Results
Overall, 15/27 (55.5 %) and 6/27 (22 %) of children in the IF and control groups responded to treatment at the 1-year follow-up (P = 0.01). The mean number of wet nights per week in the control and IF groups decreased from 5.4 ± 2 and 5.7 ± 2 to 3.3 ± 3 and 1.1 ± 2, respectively, at first evaluation (P = 0.003). The mean improvement score in the IF group was significantly higher than that of the control group after 1 year (78 vs. 46 %, respectively; P = 0.004).
Conclusion
Interferential therapy can be applied as a safe, effective and well-tolerable alternative therapy in the treatment of children with NE.



Similar content being viewed by others
References
Austin PF, Bauer SB, Bower W, Chase J, Franco I, Hoebeke P, Rittig S, Walle JV, von Gontard A, Wright A, Yang SS, Nevéus T (2014) The standardization of terminology of lower urinary tract function in children and adolescents: update report from the Standardization Committee of the International Children’s Continence Society. J Urol 191(6):1863–1865.e13
Butler RJ (2004) Childhood nocturnal enuresis: developing a conceptual framework. Clin Psychol Rev 24(8):909–931
Lordelo P, Benevides I, Kerner EG, Teles A, Lordelo M, Barroso U Jr (2010) Treatment of non-monosymptomatic nocturnal enuresis by transcutaneous parasacral electrical nerve stimulation. J Pediatr Urol 6(5):486–489
Vande Walle J, Rittig S, Bauer S, Eggert P, Marschall-Kehrel D, Tekgul S, American Academy of P, European Society for Paediatric U, European Society for Paediatric N, International Children’s Continence S (2012) Practical consensus guidelines for the management of enuresis. Eur J Pediatr 171(6):971–983
Schreiner L, dos Santos TG, de Souza AB, Nygaard CC, da Silva Filho IG (2013) Electrical stimulation for urinary incontinence in women: a systematic review. Braz J Urol 39(4):454–464
De Gennaro M, Capitanucci ML, Mosiello G, Zaccara A (2011) Current state of nerve stimulation technique for lower urinary tract dysfunction in children. J Urol 185(5):1571–1577
Fuentes JP, Armijo Olivo S, Magee DJ, Gross DP (2010) Effectiveness of interferential current therapy in the management of musculoskeletal pain: a systematic review and meta-analysis. Phys Ther 90(9):1219–1238
Clarke MC, Chase JW, Gibb S, Robertson VJ, Catto-Smith A, Hutson JM, Southwell BR (2009) Decreased colonic transit time after transcutaneous interferential electrical stimulation in children with slow transit constipation. J Pediatr Surg 44(2):408–412
Kajbafzadeh AM, Sharifi-Rad L, Nejat F, Kajbafzadeh M, Talaei HR (2012) Transcutaneous interferential electrical stimulation for management of neurogenic bowel dysfunction in children with myelomeningocele. Int J Colorectal Dis 27(4):453–458
Oh-Oka H, Fujisawa M (2007) Efficacy on interferential low frequency therapy for elderly overactive bladder patients with urinary incontinence. Nihon Hinyokika Gakkai Zasshi 98(3):547–551
de Oliveira LF, de Oliveira DM, Da Silva de Paula LI, de Figueiredo AA, de Bessa J Jr, de Sa CA, Bastos Netto JM (2013) Transcutaneous parasacral electrical neural stimulation in children with primary monosymptomatic enuresis: a prospective randomized clinical trial. J Urol 190(4):1359–1363
Rasquin A, Di Lorenzo C, Forbes D, Guiraldes E, Hyams JS, Staiano A, Walker LS (2006) Childhood functional gastrointestinal disorders: child/adolescent. Gastroenterology 130(5):1527–1537
Neveus T, von Gontard A, Hoebeke P, Hjalmas K, Bauer S, Bower W, Jorgensen TM, Rittig S, Walle JV, Yeung CK, Djurhuus JC (2006) The standardization of terminology of lower urinary tract function in children and adolescents: report from the standardisation committee of the International Children’s Continence Society. J Urol 176(1):314–324
Kajbafzadeh AM, Sharifi-Rad L, Baradaran N, Nejat F (2009) Effect of pelvic floor interferential electrostimulation on urodynamic parameters and incontinency of children with myelomeningocele and detrusor overactivity. Urology 74(2):324–329
Butler RJ, Holland P (2000) The three systems: a conceptual way of understanding nocturnal enuresis. Scand J Urol Nephrol 34(4):270–277
Park SJ, Park JM, Pai KS, Ha TS, Lee SD, Baek M, Korean Children’s Continence Enuresis Society (2014) esmopressin alone versus desmopressin and an anticholinergic in the first-line treatment of primary monosymptomatic nocturnal enuresis: a multicenter study. Pediatr Nephrol 29(7):1195–1200
Dasgupta R, Critchley HD, Dolan RJ, Fowler CJ (2005) Changes in brain activity following sacral neuromodulation for urinary retention. J Urol 174(6):2268–2272
Trontelj JV, Janko M, Godec C, Rakovec S, Trontelj M (1974) Proceedings: electrical stimulation for urinary incontinence: a neurophysiological study. Urol Int 29(3):213–220
Gladh G, Mattsson S, Lindstrom S (2001) Anogenital electrical stimulation as treatment of urge incontinence in children. BJU Int 87(4):366–371
Esa A, Kiwamoto H, Sugiyama T, Park YC, Kaneko S, Kurita T (1991) Functional electrical stimulation in the management of incontinence: studies of urodynamics. Int Urol Nephrol 23(2):135–141
Hagstroem S, Mahler B, Madsen B, Djurhuus JC, Rittig S (2009) Transcutaneous electrical nerve stimulation for refractory daytime urinary urge incontinence. J Urol 182[4 Suppl]:2072–2078
Ozcan J, Ward AR, Robertson VJ (2004) A comparison of true and premodulated interferential currents. Arch Phys Med Rehab 85(3):409–415
Raheem AA, Farahat Y, El-Gamal O, Ragab M, Radwan M, El-Bahnasy AH, El-Gamasy AN, Rasheed M (2013) Role of posterior tibial nerve stimulation in the treatment of refractory monosymptomatic nocturnal enuresis: a pilot study. J Urol 189(4):1514–1518
Lordêlo P, Teles A, Veiga ML, Correia LC, Barroso U Jr (2010) Transcutaneous electrical nerve stimulation in children with overactive bladder: a randomized clinical trial. J Urol 184(2):683–689
Sillén U, Arwidsson C, Doroszkiewicz M, Antonsson H, Jansson I, Stålklint M, Abrahamsson K, Sjöström S (2014) Effects of transcutaneous neuromodulation (TENS) on overactive bladder symptoms in children: a randomized controlled trial. J Pediatr Urol 10(6):1100–1105
Conflict of interest
None.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Kajbafzadeh, AM., Sharifi-Rad, L., Mozafarpour, S. et al. Efficacy of transcutaneous interferential electrical stimulation in treatment of children with primary nocturnal enuresis: a randomized clinical trial. Pediatr Nephrol 30, 1139–1145 (2015). https://doi.org/10.1007/s00467-014-3039-5
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00467-014-3039-5