Abstract
Background
Down-regulation of epidermal growth factor (EGF) in the renal parenchyma has been demonstrated in children who underwent pyeloplasty due to ureteropelvic junction obstruction (UPJO). Urine levels of EGF were confirmed to parallel this finding before and after surgery. The aim of our study was to evaluate the relationship between urinary EGF (uEGF) concentrations and Society of Fetal Urology (SFU) high-grade hydronephrosis in infants presenting unilateral antenatal hydronephrosis (ANH).
Methods
This was a prospective study involving 45 infants (33 in the observational group, 12 in the surgical group) who presented with unilateral ANH. Postnatal evaluation included a clinical examination, renal ultrasonography, and voiding cystourethrography. Diuretic renal scans were performed in infants with an initial SFU grade 3 or 4 hydronephrosis or increasing hydronephrosis during follow-up. Pyeloplasty was performed when a well-tempered renogram showed an obstructive drainage curve with a half-life of >20 min and/or an obstructive washout curve pattern during the diuretic phase. We studied the longitudinal changes in SFU hydronephrosis grade and uEGF in each group and compared concentration levels at three time points in both groups. The enzyme-linked immunosorbent assay (ELISA) method was used to measure EGF concentrations in the urine. The results were normalized with urinary creatinine (Cr).
Results
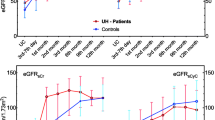
During the first 6 months, from 6 to 12 months, and in the second year of life, median SFU hydronephrosis grade and uEGF levels were 2, 2 (p = 0.015), and 1 (p < 0.01), and 50, 59 (p = 0.015), and 69.5 ng/mg Cr (p < 0.01), respectively, in the observational group. In the first 6 months, preoperatively and at 3–12 months postoperatively, the median SFU hydronephrosis grade and uEGF levels were 4, 4, and 3 (p > 0.05), and 38, 46, (p > 0.05), and 55 ng/mg Cr (p < 0.01), respectively, in the surgical group. uEGF levels in the first 6 months of life were significantly lower in the surgical group than in the observational group (p < 0.01). Patients in the observational group with SFU grade 3–4 hydronephrosis showed higher uEGF levels than those in the surgical group with SFU grade 3–4 in (p = 0.048).
Conclusions
Urinary EGF changes over time are associated with inverse changes in SFU hydronephrosis grade, which suggests a role for uEGF as a predictive marker of worsening hydronephrosis grades in infants with ANH. uEGF in the first 6 months of life may predict the need for surgery in infants with ANH.



Similar content being viewed by others
References
Nguyen HT, Herndon CD, Cooper C, Gatti J, Kirsch A, Kokorowski P, Kokorowski P, Lee R, Perez-Brayfield M, Metcalfe P, Yerkes E, Cendron M, Campbell JB (2010) The Society for Fetal Urology consensus statement on the evaluation and management of antenatal hydronephrosis. J Pediatr Urol 6:212–231
Sairam S, Al-Habib A, Sasson S, Thilaganathan B (2001) Natural history of fetal hydronephrosis diagnosed on mid-trimester ultrasound. Ultrasound Obstet Gynecol 17:191–196
Damen-Ellias HA, De Jong TP, Stigter RH, Visser GH, Stoutenbeek PH (2005) Congenital renal tract anomalies: outcome and follow up of 402 cases detected antenatally between 1986 and 2001. Ultrasound Obstet Gynecol 25:134–143
Mallik M, Watson AR (2008) Antenatally detected urinary tract abnormalities: more detection but less action. Pediatr Nephrol 23:897–904
Koff SA (2000) Postnatal management of antenatal hydronephrosis using an observational approach. Urology 55:609–611
Peters CA (1995) Urinary tract obstruction in children. J Urol 154:1874–1883, discussion 1883-1884
Koff SA, Campbell K (1992) Nonoperative management of unilateral neonatal hydronephrosis. J Urol 148:525–531
Salem YH, Majd M, Rushton HG, Belman AB (1995) Outcome analysis of pediatric pyeloplasty as a function of patient age, presentation and differential renal function. J Urol 154:1889–1893
Kass EJ, Majd M, Belman AB (1985) Comparison of the diuretic renogram and the pressure perfusion study in children. J Urol 134:92–96
Walton G, Buttyan R, Garcia-Montes E, Olsson CA, Hensle TW, Sawczuk IS (1992) Renal growth factor expression during the early phase of experimental hydronephrosis. J Urol 148:510–514
Bartoli F, Gesualdo L, Paradies G, Caldarulo E, Infante B, Grandaliano G, Monno R, Leggio S, Salzillo F, Schena FP, Leggio A (2000) Renal expression of monocyte chemotactic protein-1 and epidermal growth factor in children with obstructive hydronephrosis. J Pediatr Surg 35:569–572
Yang Y, Hou Y, Wang CL, Ji SJ (2006) Renal expression of epidermal growth factor and transforming growth factor-beta1 in children with congenital hydronephrosis. Urology 67:817–821, discussion 821-822
Grandaliano G, Gesualdo L, Bartoli F, Ranieri E, Monno R, Leggio A, Paradies G, Caldarulo E, Infante B, Schena FP (2000) MCP-1 and EGF renal expression and urine excretion in human congenital obstructive nephropathy. Kidney Int 58:182–192
Bartoli F, Penza R, Aceto G, Niglio F, D’Addato O, Pastore V, Campanella V, Magaldi S, Lasalandra C, Di Bitonto G, Gesualdo L (2011) Urinary epidermal growth factor, monocyte chemotactic protein-1, and β2-microglobulin in children with ureteropelvic junction obstruction. J Pediatr Surg 46:530–536
Stangou M, Papagianni A, Bantis C, Liakou H, Pliakos K, Giamalis P, Gionanlis L, Pantzaki A, Efstratiadis G, Memmos D (2012) Detection of multiple cytokines in the urine of patients with focal necrotising glomerulonephritis may predict short and long term outcome of renal function. Cytokine 57:120–126
Stangou M, Alexopoulos E, Papagianni A, Pantzaki A, Bantis C, Dovas S, Economidou D, Leontsini M, Memmos D (2009) Urinary levels of epidermal growth factor, interleukin-6 and monocyte chemoattractant protein-1 may act as predictor markers of renal function outcome in immunoglobulin A nephropathy. Nephrology (Carlton) 14:613–620
Fernbach SK, Maizels M, Conway JJ (1993) Ultrasound grading of hydronephrosis: introduction to the system used by the Society for Fetal Urology. Pediatr Radiol 23:478–480
Madsen MG, Nørregaard R, Frøkiær J, Jørgensen TM (2011) Urinary biomarkers in prenatally diagnosed unilateral hydronephrosis. J Pediatr Urol 7:105–112
Truong LD, Petrusevska G, Yang G, Gurpinar T, Shappell S, Lechago J, Rouse D, Suki WN (1996) Cell apoptosis and proliferation in experimental chronic obstructive uropathy. Kidney Int 50:200–207
Storch S, Saggi S, Megyesi J, Price PM, Safirstein R (1992) Ureteral obstruction decreases renal prepro-epidermal growth factor and Tamm-Horsfall expression. Kidney Int 42:89–94
Kennedy WA II, Buttyan R, Garcia-Montes E, D’Agati V, Olsson CA, Sawczuk IS (1997) Epidermal growth factor suppresses renal tubular apoptosis following ureteral obstruction. Urology 49:973–980
Oka A, Tanji N, Toshino A, Miyauchi Y, Yokoyama M (1999) Expression of growth factors after the release of ureteral obstruction in the rat kidney. Int J Urol 6:607–615
Taha AM, Shokeir AA, Osman HG, Abd El-Aziz AF, Farahat SE (2007) Pelvi-ureteric junction obstruction in children: the role of urinary transforming growth factor-β1 and epidermal growth factor. BJU Int 99:899–903
Chung KH, Chevalier RL (1996) Arrested development of the neonatal kidney following chronic ureteral obstruction. J Urol 155:1139–1144
Kwon O, Ahn K, Zhang B, Lockwood T, Dhamija R, Anderson D, Saqib N (2010) Simultaneous monitoring of multiple urinary cytokines may predict renal and patient outcome in ischemic AKI. Ren Fail 32:699–708
Acknowledgments
This study was supported by “The Youth Innovation Fund of the First Affiliated Hospital of Zhengzhou University” and Special Research Fund for the Doctoral Program of Colleges of Ministry of Education (No. 20114101120010). Prof. Robert Levin, Albany College of Pharmacy, Albany, NY, USA and Dr. Forrest Arp, Nant Works Corp, Los Angeles, CA, USA are thanked for their valuable comments.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Li, Z., Zhao, Z., Liu, X. et al. Prediction of the outcome of antenatal hydronephrosis: significance of urinary EGF. Pediatr Nephrol 27, 2251–2259 (2012). https://doi.org/10.1007/s00467-012-2243-4
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00467-012-2243-4