Abstract
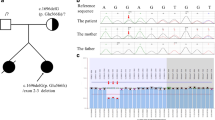
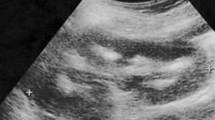
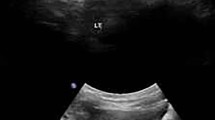
Bartter syndrome (BS) is a genetic disorder with hypokalemic metabolic alkalosis and is classified into five types. One of these, type II BS (OMIM 241200), is classified as neonatal Bartter syndrome, which is caused by mutations in the KCNJ1 gene. Transient hyperkalemia and hyponatremia are usually noted in the early postnatal period, but as type II BS is a relatively rare disease, its exact clinical course and genetic background have not yet been thoroughly characterized. This report concerns a male type II BS patient with a novel mutation in the KCNJ1 gene. The unique clinical findings of this case are that hyperkalemia (8.9 mEq/l), hyponatremia, and metabolic acidosis detected in the early postnatal period led to a diagnosis of pseudohypoaldosteronism (PHA). As an adolescent, however, the patient currently shows normal potassium levels and normal renal function, although with hypercalciuria and nephrocalcinosis, without having received any treatment. In such cases, KCNJ1 mutations should be suspected. In our case, genetic analysis of the KCNJ1 gene identified a novel homozygous 1-bp deletion mutation (c.607 del. C in exon 5).


Similar content being viewed by others
References
Bartter FC, Pronove P, Gill JR Jr, Maccardle RC (1962) Hyperplasia of the juxtaglomerular complex with hyperaldosteronism and hypokalemic alkalosis. A new syndrome. Am J Med 33:811–828
Simon DB, Karet FE, Hamdan JM, DiPietro A, Sanjad SA, Lifton RP (1996) Bartter’s syndrome, hypokalaemic alkalosis with hypercalciuria, is caused by mutations in the Na-K-2Cl cotransporter NKCC2. Nat Genet 13(2):183–188
Simon DB, Karet FE, Rodriguez-Soriano J, Hamdan JH, DiPietro A, Trachtman H, Sanjad SA, Lifton RP (1996) Genetic heterogeneity of Bartter’s syndrome revealed by mutations in the K+ channel, ROMK. Nat Genet 14(2):152–156
Simon DB, Bindra RS, Mansfield TA, Nelson-Williams C, Mendonca E, Stone R, Schurman S, Nayir A, Alpay H, Bakkaloglu A, Rodriguez-Soriano J, Morales JM, Sanjad SA, Taylor CM, Pilz D, Brem A, Trachtman H, Griswold W, Richard GA, John E, Lifton RP (1997) Mutations in the chloride channel gene, CLCNKB, cause Bartter’s syndrome type III. Nat Genet 17(2):171–178
Birkenhager R, Otto E, Schurmann MJ, Vollmer M, Ruf EM, Maier-Lutz I, Beekmann F, Fekete A, Omran H, Feldmann D, Milford DV, Jeck N, Konrad M, Landau D, Knoers NV, Antignac C, Sudbrak R, Kispert A, Hildebrandt F (2001) Mutation of BSND causes Bartter syndrome with sensorineural deafness and kidney failure. Nat Genet 29(3):310–314
Vargas-Poussou R, Huang C, Hulin P, Houillier P, Jeunemaitre X, Paillard M, Planelles G, Dechaux M, Miller RT, Antignac C (2002) Functional characterization of a calcium-sensing receptor mutation in severe autosomal dominant hypocalcemia with a Bartter-like syndrome. J Am Soc Nephrol 13(9):2259–2266
Watanabe S, Fukumoto S, Chang H, Takeuchi Y, Hasegawa Y, Okazaki R, Chikatsu N, Fujita T (2002) Association between activating mutations of calcium-sensing receptor and Bartter’s syndrome. Lancet 360(9334):692–694
Jeck N, Derst C, Wischmeyer E, Ott H, Weber S, Rudin C, Seyberth HW, Daut J, Karschin A, Konrad M (2001) Functional heterogeneity of ROMK mutations linked to hyperprostaglandin E syndrome. Kidney Int 59(5):1803–1811
Peters M, Jeck N, Reinalter S, Leonhardt A, Tonshoff B, Klaus GG, Konrad M, Seyberth HW (2002) Clinical presentation of genetically defined patients with hypokalemic salt-losing tubulopathies. Am J Med 112(3):183–190
Finer G, Shalev H, Birk OS, Galron D, Jeck N, Sinai-Treiman L, Landau D (2003) Transient neonatal hyperkalemia in the antenatal (ROMK defective) Bartter syndrome. J Pediatr 142(3):318–323
Landau D (2004) Potassium handling in health and disease: lessons from inherited tubulopathies. Pediatr Endocrinol Rev 2(2):203–208
Giebisch G (1998) Renal potassium transport: mechanisms and regulation. Am J Physiol 274(2):F817–F833
Satlin LM (1999) Regulation of potassium transport in the maturing kidney. Semin Nephrol 19(2):155–165
Satlin LM (2004) Developmental regulation of expression of renal potassium secretory channels. Curr Opin Nephrol Hypertens 13(4):445–450
Woda CB, Miyawaki N, Ramalakshmi S, Ramkumar M, Rojas R, Zavilowitz B, Kleyman TR, Satlin LM (2003) Ontogeny of flow-stimulated potassium secretion in rabbit cortical collecting duct: functional and molecular aspects. Am J Physiol Renal Physiol 285(4):F629–F639
Bailey MA, Cantone A, Yan, Q MacGregor GG, Leng Q, Amorim JB, Wang T, Hebert SC, Giebisch G, Malnic G (2006) Maxi-K channels contribute to urinary potassium excretion in the ROMK-deficient mouse model of Type II Bartter’s syndrome and in adaptation to a high-K diet. Kidney Int 70(1):51–59
Shuck ME, Bock JH, Benjamin CW, Tsai TD, Lee KS, Slightom JL, Bienkowski MJ (1994) Cloning and characterization of multiple forms of the human kidney ROM-K potassium channel. J Biol Chem 269(39):24261–24270
Liou HH, Zhou SS, Huang CL (1999) Regulation of ROMK1 channel by protein kinase A via a phosphatidylinositol 4,5-bisphosphate-dependent mechanism. Proc Natl Acad Sci USA 96(10):5820–5825
MacGregor GG, Xu JZ, McNicholas CM, Giebisch G, Hebert SC (1998) Partially active channels produced by PKA site mutation of the cloned renal K+ channel, ROMK2 (kir1.2). Am J Physiol 275(2):F415–F22
Schulte U, Hahn H, Konrad M, Jeck N, Derst C, Wild K, Weidemann S, Ruppersberg JP, Fakler B, Ludwig J (1999) pH gating of ROMK (K(ir)1.1) channels: control by an Arg-Lys-Arg triad disrupted in antenatal Bartter syndrome. Proc Natl Acad Sci USA 96(26):15298–15303
Acknowledgement
We acknowledge Ms. Yoshimi Nozu for her help in genetic analysis. This work was supported by grants from the Ministry of Education, Culture, Sports, Science and Technology of Japan.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Nozu, K., Fu, X.J., Kaito, H. et al. A novel mutation in KCNJ1 in a Bartter syndrome case diagnosed as pseudohypoaldosteronism. Pediatr Nephrol 22, 1219–1223 (2007). https://doi.org/10.1007/s00467-007-0468-4
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00467-007-0468-4