Abstract
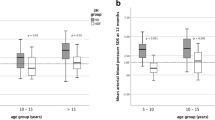
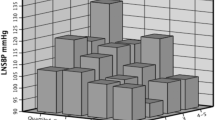
The hemolytic uremic syndrome (HUS) is the most common cause of acute renal failure (ARF) in young children. Most patients recover from the acute phase of the illness but they may develop arterial hypertension (AH) after many years, even in the absence of signs of renal impairment during short-term follow-up. In this study, we performed casual blood pressure (BP) measurement, 24-h blood pressure monitoring (ABPM), and a Bruce walking treadmill study (ET) in 24 children (aged 5–15 years, 13 males, 11 females) with a history of HUS and normal renal function during follow-up (median 5.8 years, range 1.8–12.4 years). There were 22 children (91%) with prodromal diarrhea associated with HUS and 20 (83%) underwent dialysis during the acute illness. All children had normal casual BP measurement. Of 13 children (54%) with normal ABPM, 5 patients (38%) had an abnormal BP response during the ET study. There were 4 (58%) of the 7 patients with AH by ABPM (29%) and an abnormal BP response during ET. These findings suggest that ET could be a useful means of identifying children with a history of HUS that could be at risk of future AH even if they had normal renal function, casual BP, and ABPM during long-term follow-up. These results should be confirmed with a large prospective clinical study.
Similar content being viewed by others
References
Siegler RL, Pavia AT, Cook JB (1997) Hemolytic-uremic syndrome in adolescents. Arch Pediatr Adolesc Med 151:165–169
Gianantonio CA, Vitacco M, Mendilaharzu F, Gallo GE, Sojo ET (1973) The hemolytic uremic syndrome. Nephron 11:174–192
Trompeter RS, Schwartz R, Chantler C, Dillon MJ, Haycock GB, Kay R, Barratt TM (1983) Haemolytic-uraemic syndrome: an analysis of prognostic features. Arch Dis Child 58:101–105
Loirat C, Sonsino E, Varga Moreno A, Pillion G, Mercier JC, Beaufils F, Mathieu H (1984) Hemolytic-uremic syndrome: an analysis of the natural history and prognostic features. Acta Paediatr Scand 73:505–514
Tonshoff B, Sammet A, Sanden I, Mehls O, Waldherr R, Scharer K (1994) Outcome and prognostic determinants in the haemolytic uremic syndrome of children. Nephron 68:63–70
Siegler RL, Milligan MK, Burningham TH, Christofferson RD, Chang SY, Jorde LB (1991) Long term outcome and prognostic indicators in the haemolytic-uremic syndrome. J Pediatr 118:195–200
Kmar R, Ferraris JR, Ramirez JA, Ruiz S, Salomon A, Galvez HM, Janson JJ, Galarza CR, Waisman G (2001) Ambulatory blood pressure monitoring after recovery from hemolytic uremic syndrome. Pediatr Nephrol 16:812–816
Bald M, Lettgen B, Wingen AM, Bonzel KE (1996) 24-hour blood pressure monitoring in children and adolescents after recovery from hemolytic uremic syndrome. Clin Nephrol 46:50–53
Nobuyuki M, Mikio A, Ikuharu M, Kazuhisa M, Ichiro N, Shintaro T (2000) Exercise BP response in subjects with high-normal BP. J Am Coll Cardiol 36:1626–1631
Matthews CE, Pate RR, Jackson KL, Ward DS, Macera CA, Kohl HW, Blair SN (1998) Abnormal blood pressure response to dynamic exercise and risk of future hypertension. J Clin Epidemiol 51:29–35
Benbassat J, Froom P (1986) Blood pressure response to exercise as a predictor of hypertension. Arch Intern Med 146:2053–2055
Dlin RA, Hanne N, Silverburg DS, Bar-Or O (1983) Follow up of normotensive men with exaggerated blood pressure response to exercise. Am Hearth J 106:316–320
Per Lund J (2002) Blood pressure response during exercise as a prognostic factor. J Hypertens 20:1473–1475
Update on the 1987 Second Task Force Report on High Blood Pressure in children and adolescents: a working group report from the National High Blood Pressure Education Program (1996). Pediatrics 98:649–658
Soergel M, Kirschstein M, Busch C, Danne T, Gellermann J, Holl R, Krull F, Reichert H, Reusz GS, Rascher W (1997) Oscillometric twenty-four-hour ambulatory blood pressure values in healthy children and adolescents: a multicenter trial including 1141 subjects. J Pediatr 130:178–184
Calzolari A, Ventre S, Cama G, Giordano U (1994) Exercise testing on treadmill in normal children. Int J Sports Cardiol 3:27–34
Ren J, Hakki A, Kotler MN, Iskandrian A (1985) Exercise systolic blood pressure: a powerful determinant of left ventricular mass in patients with AH. J Am Coll Cardiol 5:1224–1231
Singh JP, Larson MG, Manolio TA, O’Donnell CJ, Lauer M, Evans JC, Levy D (1999) Blood pressure response during treadmill testing as a risk factor for new-onset hypertension. Circulation 99:1831–1836
Manolino TA, Burke GL, Savage PJ, Sidney S, Gardin GM, Oberman A (1994) Exercise blood pressure response and 5-years risk of elevated blood pressure in a cohort of young adults: the CARDIA study. Am J Hypertens 7:234–241
Goble MM, Schieken RM (1994) Blood pressure response to exercise: a marker for future hypertension. Am J Hypertens 617S–620S
Mancia G, Parati G (2000) Ambulatory blood pressure monitoring and organ damage. Hypertension 36:894–900
Mitsnefes MM, Kimball TR, Daniels ST (2003) Office and ambulatory blood pressure elevation in children with chronic renal failure. Pediatr Nephrol 18:145–149
Tucker B, Fabbian F, Giles M, Thuraisngham RC, Raine AE, Baker LR (1997) Left ventricular hypertrophy and ambulatory blood pressure monitoring in chronic renal failure. Nephrol Dial Transplant 12:724–728
Gottdiener JS, Brown J, Zoltick J, Fletcher R (1990) Left ventricular hypertrophy in men with normal blood pressure: relation to abnormal blood pressure response to exercise. Ann Intern Med 112:161–166
De Simone G, Devereux RB, Roman MJ, Schlussel Y, Alderman MH, Laragh JH (1991) Echocardiographic left ventricular mass and electrolyte intake predict arterial hypertension. Ann Intern Med 114:202–209
Fagard R, Amery A (1995) Physical exercise in AH. In: Laragh JH, Brenner BM (eds) AH: pathophysiology, diagnosis and management, 2nd edn. Raven, New York, p 2669
Lingens N, Soergel M, Loirat C, Bush C, Lemmer B, Scharer K (1995) Ambulatory blood pressure monitoring in pediatric patients treated by regular hemodyalisis or peritoneal dialysis. Pediatr Nephrol 9:167–172
Morgan H, Khan I, Hashmi A, Hebert D, McCrindle BW, Balfe JW (2001) Ambulatory blood pressure monitoring after renal transplantation in children. Pediatr Nephrol 16:843–847
Sorof JM, Poffenbarger T, Portman R (2000) Abnormal 24-hour blood pressure patterns in children after renal transplantation. Am J Kidney Dis 35:681–686
Baumgart P, Walger P, Gemen S, Eiff M von, Raidt H, Rahn KH (1991) Blood pressure elevation during the night in chronic renal failure, haemodialysis and after renal transplantation. Nephron 57:293–298
O’Shea JC, Murphy MB (2000) Nocturnal blood pressure dipping: a consequence of diurnal physical activity blipping? Am J Hypertens 13:601–606
Middeke M, Schrader J (1994) Nocturnal blood pressure in normotensive subjects and those with white coat, primary, and secondary AH. BMJ 308:630–632
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
De Petris, L., Gianviti, A., Giordano, U. et al. Blood pressure in the long-term follow-up of children with hemolytic uremic syndrome. Pediatr Nephrol 19, 1241–1244 (2004). https://doi.org/10.1007/s00467-004-1582-1
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00467-004-1582-1