Abstract
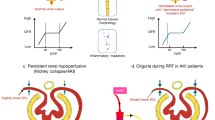
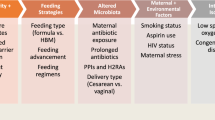
Renal impairment occurs in neonates receiving indomethacin for treatment of patent ductus arteriosus. Inhibition of cyclooxygenase within the neonatal kidney results in decreased prostaglandin synthesis and consequent reduction in renal perfusion. Indomethacin has been reported to cause short-term reduction in glomerular filtration that resolves after cessation of the drug. There is little information on the long-term effects of postnatal exposure to indomethacin. The aim of this study was to determine the incidence of renal impairment in infants treated with indomethacin in a single center, to determine whether there is evidence of renal impairment on day 30 or at discharge, and to identify risk factors for renal impairment. In a retrospective study, infants of less than 30 weeks completed gestation who received indomethacin to close the ductus arteriosus were matched with infants of the same gestation, birth weight, and severity of illness. Serum creatinine and glomerular filtration rates (GFR) were obtained prior to commencing indomethacin and on days 2, 7, and 30 following indomethacin administration. Acute renal failure was defined as an increase in creatinine of greater than 25%. Of those infants who were less than 30 weeks completed gestation, 24% had acute renal failure following indomethacin administration. There was a significant elevation in serum creatinine on day 2 and day 7 (P<0.0001, P=0.002) and a decrease in GFR on day 2 and day 7 (P<0.0001, P=0.01) following administration of indomethacin. Renal function had normalized by day 30 or discharge. The incidence of acute renal failure in neonates treated with indomethacin is clinically significant. Renal function returns to normal by day 30. Linear regression found no statistical significance for gestational age, day of indomethacin dosing, Clinical Risk Index for Babies (CRIB) score, and presence of an umbilical artery catheter to confound the effect of indomethacin on renal function.
Similar content being viewed by others
References
Toth-Heyn P, Drukker A, Guignard J-P (2000) The stressed neonatal kidney: from pathophysiology to clinical management of neonatal vasomotor nephropathy. Pediatr Nephrol 14:227–239
Emmanouilides G (1978) Persistent patency of the ductus arteriosus in premature infants: incidence, perinatal factors and natural history. In: Heymann M, Rudolph A (eds) The ductus arteriosus. The 75th Conference on Pediatric Research. Columbus, Ohio, Ross Laboratories pp 63–69
Ellison RC, Peckham GJ, Lang P, Talner NS, Lerer TJ, Lin L, Dooley KJ, Nadas AS (1983) Evaluation of the preterm infant for patent ductus arteriosus. Pediatrics 71:364–372
Hammerman C, Kaplan M (2001) Comparative tolerability of pharmacological treatments for patent ductus arteriosus. Drug Saf 24:537–551
Narayanan M, Cooper B, Weiss H, Clyman RI (2000) Prophylactic indomethacin: factors determining permanent ductus closure. J Pediatr 136:330–337
Van Overmeire B, Van deBroek H, VanLaer P, Weyler J, Vanbaesebrouck P (2001) Early versus late indomethacin treatment for patent ductus arteriosus in premature infants with respiratory distress syndrome. J Pediatr 138:205–211
Shaffer CL, Gal P, Random JL, Carlos RQ, Smith MS, Davy AM, Smith MS, Davey AM, Dimaguila MVT, Brown YL, Schall SA (2002) Effect of age and birth weight on indomethacin pharmacodynamics in neonates treated for patent ductus arteriosus. Crit Care Med 30:343–348
Pezzati M, Vargi V, Biagotti R, Bertini G, Cianciulli D, Rubatelli FF (1999) Effects of indomethacin and ibuprofen on mesenteric and renal blood flow in preterm infants with patent ductus arteriosus. J Pediatr 135:733–738
Ojala R, Ala-Houhala M, Ahonen S, Harmoinen A, Turjanmaa V, Ikonen S, Tammela O (2001) Renal follow up of premature infants with and without perinatal indomethacin exposure. Arch Dis Child Fetal Neonatal Ed 84:F28–F33
Zachello G, Bondi M, Saia OS, Largaiolli G, Vedaldi, Rubaltelli FF (1982) Simple estimate of creatinine clearance from plasma creatinine in neonates. Arch Dis Child 57:297–300
The International Neonatal Network (1993) The CRIB (clinical risk index for babies) score: a tool for assessing initial neonatal risk and comparing performance of neonatal intensive care units. Lancet 342:193–198
Edwards AD, Wyatt JS, Richardson C, Potter A, Cope M, Delpy DT, Reynolds EDR (1990) Effects of indomethacin on cerebral haemodynamics in very preterm infants. Lancet 335:1491–1495
Schmidt B, Davis P, Moddemann D, Ohlsson A, Roberts RS, Saigal S, Solimano A, Vincer M, Wright LL (2001) Long-term effects of indomethacin prophylaxis in extremely-low-birth-weight infants. N Engl J Med 344:1966–1972
Van Overmeire B, Follens I, Hartmann S, Creten WL, Van Acker KJ (1997) Treatment of patent ductus arteriosus with ibuprofen. Arch Dis Child 76:F179–184
Van Overmeire B, Smets K, Lecoutere D, Van de Broek H, Weyler J, Degroote K, Langhendries JP (2000) A comparison of ibuprofen and indomethacin for closure of patent ductus arteriosus. N Engl J Med 343:674–681
Varvarigou A, Bardin CL, Beharry K, Chemtob S, Papageorgiou A, Aranda JV (1996) Early ibuprofen administration to prevent patent ductus arteriosus in premature newborn infants. JAMA 275:539–544
Saarela T, Lanning P, Koivisto M, Paavilainen T (1999) Nephrocalcinosis in full-term infants receiving furosemide treatment for congestive heart failure: a study of the incidence and 2-year follow up. Eur J Pediatr 158:668–672
Hufnagle KG, Khan SN, Penn D, Cacciarelli A, Williams P (1982) Renal calcifications: a complication of long-term furosemide therapy in preterm infants. Pediatrics 70:360–363
Ezzedeen F, Adelman RD, Ahlfors CE (1988) Renal calcification in preterm infants: pathophysiology and long-term sequelae. J Pediatr 113:532–539
Acknowledgement
The authors express their gratitude to Deborah Davy for her excellent technical and administrative assistance.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Akima, S., Kent, A., Reynolds, G.J. et al. Indomethacin and renal impairment in neonates. Pediatr Nephrol 19, 490–493 (2004). https://doi.org/10.1007/s00467-003-1402-z
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00467-003-1402-z