Abstract
Background
Although perioperative hypothermia is a well-known consequence of general anesthesia, it has been hypothesized that laparoscopic surgery exacerbates hypothermia to a greater extent than open surgery. The aim of this study was to demonstrate that laparoscopic surgery does not represent an increased risk for hypothermia.
Methods
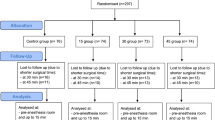
A case-controlled retrospective study was conducted on 45 patients, 25 undergoing laparoscopic chole-cystectomy and 20 undergoing parathyroid surgery under endotracheal general anesthesia. Data were collected regarding age, sex, weight, height, American Society of Anesthesiologists (ASA) status, length of surgery, and anesthesia. In addition, we analyzed the type of intraoperative intravenous fluids, anesthetics and perioperative drugs, and temperature, blood pressure, and heart rate recordings during anesthesia.
Results
There was no significant difference between the two groups with respect to age, sex, body mass index (BMI), ASA status, type or amount of intravenous fluids infused, length of anesthesia or surgery, changes in mean blood pressure, or heart rate. Core body temperatures in both groups decreased significantly over time (p < 0.001). However, the core body temperature changes at all measurement points and the rate of temperature drop were similar in both laparoscopic and parathyroidectomy groups (p > 0.05). There was no difference between the groups in terms of maximum drop in temperature (lowest temperature recorded vs baseline temperature) (1.1 ∓ 0.7 vs 1.0 ∓ 0.7°C, p > 0.05).
Conclusion
This study demonstrates that patients who undergo laparoscopic and open procedures of similar duration under endotracheal general anesthesia have similar profiles in terms of perioperative hypothermia.
Similar content being viewed by others
References
Bessell JR, Karatassas A, Patterson JR, Jamieson GG, Maddern GJ (1995) Hypothermia induced by laparoscopic insufflation: a randomized study in a pig model. Surg Endosc 9: 791–796
Carli F, Emergy PW, Freemantle CAJ (1989) Effect of perioperative normothermia on postoperative protein metabolism in elderly patients undergoing hip arthroplasty. Br J Anaesth 63: 276–282
Castillo V, Gutierrez-Crespo A, Luis-Navaro JC (1996) Body temperature variations during laparoscopic cholecystectomies [in Spanish]. Rev Esp Anesthesiol Reanim 43: 201–203
Colboc O, Protais P, Costentin J (1982) Histamine-induced rise in core temperature of chloral-anesthetized rats: mediation by H2-receptors located in the preopticus area of hypothalamus. Neuropharmocology 21: 45–50
Forstot RM (1995) The etiology and management of inadvertent peri-operative hypothermia. J Clin Anesth 7: 657–674
Frank SM, Beattie C, Christopherson R, Norris EJ, Perler BA, Williams GM, Gottlieb SO (1993) Unintentional hypothermia is associated with postoperative myocardial ischemia. Anesthesiology 78: 468–476
Frank SM, Shir Y, Raja NS, Fleischer LA, Beattie C (1994) Core hypothermia and skin-surface temperature gradients: epidural versus general anesthesia and the effects of age. Anesthesiology 80: 502–508
Heier T. Caldwell JE, Sessler DI, Miller RD (1991) Mild intraoperative hypothermia increases duration of action spontaneous recovery of vecuronium blockade during nitrous oxide-isoflurane anesthesia in humans. Anesthesiology 74: 815–819
Hirose M, Hara Y, Matsusaki MP (1995) Remedication with famotidine augments core hypothermia during general anesthesia. Anesthesiology 83: 1179–1183
Huntington TR, LeMaster CB (1997) Laparoscopic hypothermia: heat loss from insufflation of gas flow. Surg Laparosc Endosc 7: 153–155
Lomax P, Green MD (1981) Histaminergic neurons in the hypothalamic thermoregulatory pathways. FASEB J 40: 2741–2745
Lopez M, Sessler DI, Walter K, Emerick T, Ozaki M (1994) Rate and gender dependence of the sweating, vasoconstriction, and shivering thresholds in humans. Anesthesiology 80: 780–788
Luck AJ, Moyes D, Maddern GJ, Hewett PJ (1999) Core temperature changes during open and laparoscopic colorectal surgery. Surg Endosc 13: 480–483 DOI: 10.1007/s004649901017
Makinen T (1997) Comparison of body temperature changes during laparoscopic and open cholecystectomy. Acta Anaesthesiol Scand 41: 736–740
Mansvelt B, Arnould P, Bertrand C, Roden AN (1995) Utilization of gas humidifier in the course of celioscopics. Acta Chir Belg 95: 100–102
Matsukawa T, Sessler DI, Sessler AM, Schroeder M, Ozaki M, Kurz A, Cheng C (1995) Heat flow and distribution during induction of general anesthesia. Anesthesiology 82: 662–673
Monagle J. Bradfield S. Nottle P (1993) Carbon dioxide, temperature and laparoscopic cholecystectomy. Aust N Z J Surg 63: 186–189
Moore SS, Green CR, Wang FL, Pandit SK, Hurd WW (1997) The role of irrigation in the development of hypothermia during laparoscopic surgery. Am J Obstet Gynecol 176: 598–602
Morris RH (1971) Influence of ambient temperature on patient temperature during intraabdominal surgery. Ann Surg 173: 230–233
Mouton WG, Bessell JR, Millard SH, Baxter PS, Maddern GJ (1999) A randomized controlled trial assessing the benefit of humidified insufflation gas during laparoscopic surgery. Surg Endosc 13: 106–108 DOI: 10.1007/s004649900915
Ott DE (1991) Correction of laparoscopic insufflation hypothermia. J Laparoendosc Surg 1: 183–186
Ott DE (1991) Laparoscopic hypothermia. J Laparoendosc Surg 1: 127–131
Rose DK, Cohen MM, Soutter DI (1992) Laparoscopic cholecystectomy: the anesthetist’s point of view. Can J Anaesth 39: 809–815
Sanabria JR, Clavien PA, Strasberg SM (1993) Laparoscopic versus open cholecystectomy: a matched study. Can J Surg 36: 330–336
Sessler DI (1997) Perioperative thermoregulation and heat balance. Ann N Y Acad Sci 813: 757–777
Sessler DI, Olofson CI, Rubinstein EH (1988) The thermoregulatory threshold in humans during nitrous oxide-fentanyl anesthesia. Anesthesiology 69: 357–364
Taylor KM, Snyder SH (1972) Dynamics of the regulation of histamine levels in mouse brain. J Neurochem 19: 341–354
Valeri CR, Feingold H. Cassidy G, Ragno G, Khuri S, Altschule MD (1987)Hypothermia-induced reversible platelet dysfunction. Ann Surg 205: 175–181
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Berber, E., String, A., Garland, A. et al. Intraoperative thermal regulation in patients undergoing laparoscopic vs open surgical procedures. Surg Endosc 15, 281–285 (2001). https://doi.org/10.1007/s004640000330
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1007/s004640000330