Abstract
Background
Portal vein system thrombosis (PVST) is a potentially fatal complication after splenectomy with esophagogastric devascularization (SED) in cirrhotic patients with portal hypertension. However, the impact of portal vein velocity (PVV) on PVST after SED remains unclear. Therefore, this study aims to explore this issue.
Methods
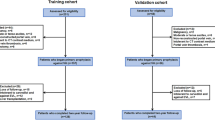
Consecutive cirrhotic patients with portal hypertension who underwent SED at Tongji Hospital between January 2010 and June 2022 were enrolled. The patients were divided into two groups based on the presence or absence of PVST, which was assessed using ultrasound or computed tomography after the operation. PVV was measured by duplex Doppler ultrasound within one week before surgery. The independent risk factors for PVST were analyzed using univariate and multivariate logistic regression analysis. A nomogram based on these variables was developed and internally validated using 1000 bootstrap resamples.
Results
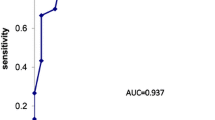
A total of 562 cirrhotic patients with portal hypertension who underwent SED were included, and PVST occurred in 185 patients (32.9%). Multivariate logistic regression analysis showed that PVV was the strongest independent risk factor for PVST. The incidence of PVST was significantly higher in patients with PVV ≤ 16.5 cm/s than in those with PVV > 16.5 cm/s (76.2% vs. 8.5%, p < 0.0001). The PVV-based nomogram was internally validated and showed good performance (optimism-corrected c-statistic = 0.907). Decision curve and clinical impact curve analyses indicated that the nomogram provided a high clinical benefit.
Conclusion
A nomogram based on PVV provided an excellent preoperative prediction of PVST after splenectomy with esophagogastric devascularization.
Graphical abstract





Similar content being viewed by others
References
Ginès P, Krag A, Abraldes JG, Solà E, Fabrellas N, Kamath PS (2021) Liver cirrhosis. Lancet 398:1359–1376. https://doi.org/10.1016/S0140-6736(21)01374-X
Lv Y, Fan D, Han G (2023) Transjugular intrahepatic portosystemic shunt for portal hypertension: 30 years experience from China. Liver Int 43:18–33. https://doi.org/10.1111/liv.15313
de Franchis R, Bosch J, Garcia-Tsao G, Reiberger T, Ripoll C, Faculty BVII (2022) Baveno VII—renewing consensus in portal hypertension. J Hepatol 76:959–974. https://doi.org/10.1016/j.jhep.2021.12.022
de Franchis R, Faculty BVI (2015) Expanding consensus in portal hypertension: Report of the Baveno VI Consensus Workshop: stratifying risk and individualizing care for portal hypertension. J Hepatol 63:743–752. https://doi.org/10.1016/j.jhep.2015.05.022
European Association for the Study of the Liver (2016) EASL Clinical Practice Guidelines: liver transplantation. J Hepatol 64:433–485. https://doi.org/10.1016/j.jhep.2015.10.006
Li Y, Fu X, Li Y, Liu P, Liu S, Pan Y (2022) Early prevention and risk factors analysis of portal vein system thrombosis after laparoscopic splenectomy and pericardial devascularization. Surg Endosc 36:8918–8926. https://doi.org/10.1007/s00464-022-09340-5
Zhe C, Jian-wei L, Jian C, Yu-dong F, Ping B, Shu-guang W, Shu-guo Z (2013) Laparoscopic versus open splenectomy and esophagogastric devascularization for bleeding varices or severe hypersplenism: a comparative study. J Gastrointest Surg 17:654–659. https://doi.org/10.1007/s11605-013-2150-4
Chen Z-L, Yao L-Q, Pu J-L, Wu H, Xu X-F, Chen T-H, Zhou Y-H, Wang H, Chen Z-Y, Sun L-Y, Diao Y-K, Zhong J-H, Lau WY, Pawlik TM, Huang D-S, Shen F, Liang Y-J, Yang T (2022) Impact of concurrent splenectomy and esophagogastric devascularization on surgical outcomes of partial hepatectomy for hepatocellular carcinoma in patients with clinically significant portal hypertension: a multicenter propensity score matching analysis. Eur J Surg Oncol 48:1078–1086. https://doi.org/10.1016/j.ejso.2021.11.118
Zhang E-L, Zhang Z-Y, Huang Z-Y (2023) Splenectomy may facilitate systemic therapy for advanced hepatocellular carcinoma with hypersplenism. Hepatobiliary Surg Nutr 12:137–139. https://doi.org/10.21037/hbsn-22-545
Ikeda M, Sekimoto M, Takiguchi S, Kubota M, Ikenaga M, Yamamoto H, Fujiwara Y, Ohue M, Yasuda T, Imamura H, Tatsuta M, Yano M, Furukawa H, Monden M (2005) High incidence of thrombosis of the portal venous system after laparoscopic splenectomy: a prospective study with contrast-enhanced CT scan. Ann Surg 241:208–216. https://doi.org/10.1097/01.sla.0000151794.28392.a6
Intagliata NM, Caldwell SH, Tripodi A (2019) Diagnosis, development, and treatment of portal vein thrombosis in patients with and without cirrhosis. Gastroenterology 156:1582-1599.e1. https://doi.org/10.1053/j.gastro.2019.01.265
Wu L-F, Bai D-S, Shi L, Jin S-J, Zhou B-H, Jiang G-Q (2022) Predictors of portal vein thrombosis after laparoscopic splenectomy and azygoportal disconnection in hepatitis B cirrhosis: a prospective study. Surg Endosc 36:4090–4098. https://doi.org/10.1007/s00464-021-08730-5
Lai W, Lu S-C, Li G-Y, Li C-Y, Wu J-S, Guo Q-L, Wang M-L, Li N (2012) Anticoagulation therapy prevents portal-splenic vein thrombosis after splenectomy with gastroesophageal devascularization. World J Gastroenterol 18:3443–3450. https://doi.org/10.3748/wjg.v18.i26.3443
Kinjo N, Kawanaka H, Akahoshi T, Tomikawa M, Yamashita N, Konishi K, Tanoue K, Shirabe K, Hashizume M, Maehara Y (2010) Risk factors for portal venous thrombosis after splenectomy in patients with cirrhosis and portal hypertension. Br J Surg 97:910–916. https://doi.org/10.1002/bjs.7002
Jiang G-Q, Bai D-S, Chen P, Xia B-L, Qian J-J, Jin S-J (2016) Predictors of portal vein system thrombosis after laparoscopic splenectomy and azygoportal disconnection: a retrospective cohort study of 75 consecutive patients with 3-months follow-up. Int J Surg 30:143–149. https://doi.org/10.1016/j.ijsu.2016.04.047
Qian Y, Li K (2017) The early prevention and treatment of PVST after laparoscopic splenectomy: a prospective cohort study of 130 patients. Int J Surg 44:147–151. https://doi.org/10.1016/j.ijsu.2017.05.072
Blann AD, Lip GY (2001) Virchow’s triad revisited: the importance of soluble coagulation factors, the endothelium, and platelets. Thromb Res 101:321–327. https://doi.org/10.1016/s0049-3848(00)00419-9
Turon F, Driever EG, Baiges A, Cerda E, García-Criado Á, Gilabert R, Bru C, Berzigotti A, Nuñez I, Orts L, Reverter JC, Magaz M, Camprecios G, Olivas P, Betancourt-Sanchez F, Perez-Campuzano V, Blasi A, Seijo S, Reverter E, Bosch J, Borràs R, Hernandez-Gea V, Lisman T, Garcia-Pagan JC (2021) Predicting portal thrombosis in cirrhosis: a prospective study of clinical, ultrasonographic and hemostatic factors. J Hepatol 75:1367–1376. https://doi.org/10.1016/j.jhep.2021.07.020
Stine JG, Wang J, Shah PM, Argo CK, Intagliata N, Uflacker A, Caldwell SH, Northup PG (2018) Decreased portal vein velocity is predictive of the development of portal vein thrombosis: a matched case–control study. Liver Int 38:94–101. https://doi.org/10.1111/liv.13500
Zocco MA, Di Stasio E, De Cristofaro R, Novi M, Ainora ME, Ponziani F, Riccardi L, Lancellotti S, Santoliquido A, Flore R, Pompili M, Rapaccini GL, Tondi P, Gasbarrini GB, Landolfi R, Gasbarrini A (2009) Thrombotic risk factors in patients with liver cirrhosis: correlation with MELD scoring system and portal vein thrombosis development. J Hepatol 51:682–689. https://doi.org/10.1016/j.jhep.2009.03.013
Tran T, Demyttenaere SV, Polyhronopoulos G, Séguin C, Artho GP, Kaneva P, Fried GM, Feldman LS (2010) Recommended timing for surveillance ultrasonography to diagnose portal splenic vein thrombosis after laparoscopic splenectomy. Surg Endosc 24:1670–1678. https://doi.org/10.1007/s00464-009-0828-1
Kramer AA, Zimmerman JE (2007) Assessing the calibration of mortality benchmarks in critical care: the Hosmer-Lemeshow test revisited. Crit Care Med 35:2052–2056. https://doi.org/10.1097/01.CCM.0000275267.64078.B0
DeLong ER, DeLong DM, Clarke-Pearson DL (1988) Comparing the areas under two or more correlated receiver operating characteristic curves: a nonparametric approach. Biometrics 44:837–845
Vickers AJ, Cronin AM, Elkin EB, Gonen M (2008) Extensions to decision curve analysis, a novel method for evaluating diagnostic tests, prediction models and molecular markers. BMC Med Inform Decis Mak 8:53. https://doi.org/10.1186/1472-6947-8-53
Senzolo M, Garcia-Tsao G, García-Pagán JC (2021) Current knowledge and management of portal vein thrombosis in cirrhosis. J Hepatol 75:442–453. https://doi.org/10.1016/j.jhep.2021.04.029
Zoli M, Iervese T, Merkel C, Bianchi G, Magalotti D, Marchesini G, Gatta A, Pisi E (1993) Prognostic significance of portal hemodynamics in patients with compensated cirrhosis. J Hepatol 17:56–61. https://doi.org/10.1016/s0168-8278(05)80521-5
Ramachandran P, Dobie R, Wilson-Kanamori JR, Dora EF, Henderson BEP, Luu NT, Portman JR, Matchett KP, Brice M, Marwick JA, Taylor RS, Efremova M, Vento-Tormo R, Carragher NO, Kendall TJ, Fallowfield JA, Harrison EM, Mole DJ, Wigmore SJ, Newsome PN, Weston CJ, Iredale JP, Tacke F, Pollard JW, Ponting CP, Marioni JC, Teichmann SA, Henderson NC (2019) Resolving the fibrotic niche of human liver cirrhosis at single-cell level. Nature 575:512–518. https://doi.org/10.1038/s41586-019-1631-3
Trautwein C, Friedman SL, Schuppan D, Pinzani M (2015) Hepatic fibrosis: concept to treatment. J Hepatol 62:S15-24. https://doi.org/10.1016/j.jhep.2015.02.039
Lemoinne S, Cadoret A, Rautou P-E, El Mourabit H, Ratziu V, Corpechot C, Rey C, Bosselut N, Barbu V, Wendum D, Feldmann G, Boulanger C, Henegar C, Housset C, Thabut D (2015) Portal myofibroblasts promote vascular remodeling underlying cirrhosis formation through the release of microparticles. Hepatology 61:1041–1055. https://doi.org/10.1002/hep.27318
Tripodi A, Primignani M, Chantarangkul V, Dell’Era A, Clerici M, de Franchis R, Colombo M, Mannucci PM (2009) An imbalance of pro- vs anti-coagulation factors in plasma from patients with cirrhosis. Gastroenterology 137:2105–2111. https://doi.org/10.1053/j.gastro.2009.08.045
Tripodi A, Mannucci PM (2011) The coagulopathy of chronic liver disease. N Engl J Med 365:147–156. https://doi.org/10.1056/NEJMra1011170
Intagliata NM, Argo CK, Stine JG, Lisman T, Caldwell SH, Violi F, Faculty of the 7th International Coagulation in Liver Disease (2018) Concepts and controversies in haemostasis and thrombosis associated with liver disease: proceedings of the 7th international coagulation in liver disease conference. Thromb Haemost 118:1491–1506. https://doi.org/10.1055/s-0038-1666861
Li J, Wu Q-Q, Zhu R-H, Lv X, Wang W-Q, Wang J-L, Liang B-Y, Huang Z-Y, Zhang E-L (2022) Machine learning predicts portal vein thrombosis after splenectomy in patients with portal hypertension: comparative analysis of three practical models. World J Gastroenterol 28:4681–4697. https://doi.org/10.3748/wjg.v28.i32.4681
Swinson B, Waters PS, Webber L, Nathanson L, Cavallucci DJ, O’Rourke N, Bryant RD (2022) Portal vein thrombosis following elective laparoscopic splenectomy: incidence and analysis of risk factors. Surg Endosc 36:3332–3339. https://doi.org/10.1007/s00464-021-08649-x
Krauth M-T, Lechner K, Neugebauer EAM, Pabinger I (2008) The postoperative splenic/portal vein thrombosis after splenectomy and its prevention—an unresolved issue. Haematologica 93:1227–1232. https://doi.org/10.3324/haematol.12682
Acknowledgements
The authors would like to thank all the medical staff involved in this study.
Funding
This work was supported by Hubei Provincial Special Grants for Scientific and Technical Innovation (2021BCA115).
Author information
Authors and Affiliations
Contributions
Study concepts: J-LW, Z-WZ; Study design: J-LW, Z-WZ, E-LZ, Z-YH; Data acquisition: J-LW; Data analysis and interpretation: J-LW, JL, W-QW; Statistical analysis: J-LW, JL, XL, R-HZ, TY; Manuscript editing: J-LW; Manuscript review: E-LZ, Z-WZ, Z-YH. All authors read and approved the final version of the manuscript.
Corresponding authors
Ethics declarations
Disclosures
Jin-lin Wang, Jian Li, Wen-qiang Wang, Xing Lv, Rong-hua Zhu, Tong Yuan, Er-lei Zhang, Zhi-wei Zhang, and Zhi-yong Huang have no conflicts of interest to disclose.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Wang, Jl., Li, J., Wang, Wq. et al. Portal vein velocity predicts portal vein system thrombosis after splenectomy with esophagogastric devascularization. Surg Endosc 38, 648–658 (2024). https://doi.org/10.1007/s00464-023-10566-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-023-10566-0