Abstract
Background
Currently, only a limited number of remote assistance modalities are utilized in the basic phase of robotic surgery training to facilitate the rapid acquisition of robotic surgery skills by surgeons. This study aimed to investigate the benefits of real-time remote surgical robotic skill training based on a multi-channel video recording and playback system.
Methods
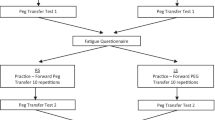
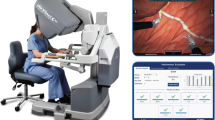
We randomly divided 40 medical students without prior expertise in the use of surgical robots into two groups to assess the performance of trainees on a robotic simulator (Mimic dV-Trainer). The remote group received remote training, while the control group received live one-on-one guidance. We compared the learning curves of the two groups based on simulator scores. Furthermore, the NASA task load index (NASA-TLX) scale was used to measure the fatigue load of the trainers.
Results
We observed no significant differences in the demographics or initial baseline skill levels between the two groups. Participants in the remote group achieved higher total scores in the Match Board 2 and Thread the Rings 1 exercises compared to the control group. In addition, trainers in the remote group reported lower subjective fatigue load than in the control group.
Conclusions
The remote approach to surgical robotics skills training based on the Remote Teaching System for Robotic Surgery (ReTeRoS) is both feasible and has the potential for large-scale training.
Graphical abstract










Similar content being viewed by others
References
Turner SR, Mormando J, Park BJ, Huang J (2020) Attitudes of robotic surgery educators and learners: challenges, advantages, tips and tricks of teaching and learning robotic surgery. J Robot Surg 14:455–461
Augestad KM, Bellika JG, Budrionis A, Chomutare T, Lindsetmo RO, Patel H, Delaney C (2013) Surgical telementoring in knowledge translation–clinical outcomes and educational benefits: a comprehensive review. Surg Innov 20:273–281
Foote JR, Valea FA (2016) Robotic surgical training: where are we? Gynecol Oncol 143:179–183
Williams TE Jr, Satiani B, Thomas A, Ellison EC (2009) The impending shortage and the estimated cost of training the future surgical workforce. Ann Surg 250:590–597
Hakamada K, Mori M (2021) The changing surgical scene: from the days of Billroth to the upcoming future of artificial intelligence and telerobotic surgery. Ann Gastroenterol Surg 5:268–269
Anvari M, Manoharan B, Barlow K (2021) From telementorship to automation. J Surg Oncol 124:246–249
Boyers LN, Schultz A, Baceviciene R, Blaney S, Marvi N, Dellavalle RP, Dunnick CA (2015) Teledermatology as an educational tool for teaching dermatology to residents and medical students. Telemed J E Health 21:312–314
Park KM, Rashidian N, Anderson C, Brian R, Calthorpe LM, Gee D, Hernandez S, Lau J, Nepomnayshy D, Patel NM, Pei K, Reddy RM, Roman SA, Scott DJ, Alseidi A (2022) Evidence-based guidelines on the use of virtual surgical education pertaining to the domains of cognition and curriculum, psychomotor skills training, and faculty development and mentorship. Ann Surg 276:e6–e15. https://doi.org/10.1097/SLA.0000000000005014
Rojas-Muñoz E, Cabrera ME, Andersen D, Popescu V, Marley S, Mullis B, Zarzaur B, Wachs J (2019) Surgical telementoring without encumbrance: a comparative study of see-through augmented reality-based approaches. Ann Surg 270:384–389
Ab K, Augestad KM (2021) Educational value of surgical telementoring. J Surg Oncol 124:231–240
Augestad KM, Han H, Paige J, Ponsky T, Schlachta CM, Dunkin B, Mellinger J (2017) Educational implications for surgical telementoring: a current review with recommendations for future practice, policy, and research. Surg Endosc 31:3836–3846
Yang K, Perez M, Hubert N, Hossu G, Perrenot C, Hubert J (2017) Effectiveness of an integrated video recording and replaying system in robotic surgical training. Ann Surg 265:521–526
Bric JD, Lumbard DC, Frelich MJ, Gould JC (2016) Current state of virtual reality simulation in robotic surgery training: a review. Surg Endosc 30:2169–2178
Lee JY, Mucksavage P, Kerbl DC, Huynh VB, Etafy M, McDougall EM (2012) Validation study of a virtual reality robotic simulator—role as an assessment tool? J Urol 187:998–1002
Yang K, Perez M, Hossu G, Hubert N, Perrenot C, Hubert J (2017) “Alarm-corrected” ergonomic armrest use could improve learning curves of novices on robotic simulator. Surg Endosc 31:100–106
Fan S, Zhang Z, Wang J, Xiong S, Dai X, Chen X, Li Z, Han G, Zhu J, Hao H, Yu W, Cui L, Shen C, Li X, Zhou L (2022) Robot-assisted radical prostatectomy using the KangDuo Surgical Robot-01 system: a prospective, single-center, single-arm clinical study. J Urol 208:119–127
Nguyen NT, Okrainec A, Anvari M, Smith B, Meireles O, Gee D, Moran-Atkin E, Baram-Clothier E, Camacho DR (2018) Sleeve gastrectomy telementoring: a SAGES multi-institutional quality improvement initiative. Surg Endosc 32:682–687
Fehervari M, Das B, Soleimani-Nouri P, Ahmad M, Fadel MG, Deputy M, Morgan C, Burke JR, Mason JD, Nott D, Spalding D (2022) Can surgical skills be taught using technological advances online? A comparative study of online and face-to-face surgical skills training. Surg Endosc 36:4631–4637
Jewer J, Parsons MH, Dunne C, Smith A, Dubrowski A (2019) Evaluation of a mobile telesimulation unit to train rural and remote practitioners on high-acuity low-occurrence procedures: pilot randomized controlled trial. J Med Internet Res 21:e14587
Kirkpatrick AW, Tien H, LaPorta AT, Lavell K, Keillor J, Wright Beatty HE, McKee JL, Brien S, Roberts DJ, Wong J, Ball CG, Beckett A (2015) The marriage of surgical simulation and telementoring for damage-control surgical training of operational first responders: a pilot study. J Trauma Acute Care Surg 79:741–747
Budrionis A, Hasvold P, Hartvigsen G, Bellika JG (2016) Assessing the impact of telestration on surgical telementoring: a randomized controlled trial. J Telemed Telecare 22:12–17
Bogen EM, Schlachta CM, Ponsky T (2019) White paper: technology for surgical telementoring-SAGES Project 6 Technology Working Group. Surg Endosc 33:684–690
Co M, Chu KM (2020) Distant surgical teaching during COVID-19—a pilot study on final year medical students. Surg Pract 24:105–109
Carter SC, Chiang A, Shah G, Kwan L, Montgomery JS, Karam A, Tarnay C, Guru KA, Hu JC (2015) Video-based peer feedback through social networking for robotic surgery simulation: a multicenter randomized controlled trial. Ann Surg 261:870–875
Tejos R, Crovari F, Achurra P, Avila R, Inzunza M, Jarry C, Martinez J, Riquelme A, Alseidi A, Varas J (2021) Video-based guided simulation without peer or expert feedback is not enough: a randomized controlled trial of simulation-based training for medical students. World J Surg 45:57–65
Bakshi SK, Ho AC, Chodosh J, Fung AT, Chan RVP, Ting DSW (2020) Training in the year of the eye: the impact of the COVID-19 pandemic on ophthalmic education. Br J Ophthalmol 104:1181–1183
Mizota T, Kurashima Y, Poudel S, Watanabe Y, Shichinohe T, Hirano S (2018) Step-by-step training in basic laparoscopic skills using two-way web conferencing software for remote coaching: a multicenter randomized controlled study. Am J Surg 216:88–92
Anvari M (2007) Remote telepresence surgery: the Canadian experience. Surg Endosc 21:537–541
Williams TP, Klimberg V, Perez A (2021) Tele-education assisted mentorship in surgery (TEAMS). J Surg Oncol 124:250–254
von Hessling A, Reyes Del Castillo T, Roos JE, Karwacki GM (2022) Technical considerations and tips for using the Tegus remote proctoring system in elective and emergency cases and in webinars. J Neurointerv Surg 14:976–978
Wang H, Sugand K, Newman S, Jones G, Cobb J, Auvinet E (2019) Are multiple views superior to a single view when teaching hip surgery? A single-blinded randomized controlled trial of technical skill acquisition. PLoS ONE 14:e0209904. https://doi.org/10.1371/journal.pone.0209904
Abdelaal AE, Avinash A, Kalia M, Hager GD, Salcudean SE (2020) A multi-camera, multi-view system for training and skill assessment for robot-assisted surgery. Int J Comput Assist Radiol Surg 15:1369–1377
Jung JJ, Jüni P, Lebovic G, Grantcharov T (2020) First-year analysis of the operating room black box study. Ann Surg 271:122–127
Mendelsohn AH, Kim C, Song J, Singh A, Le T, Abiri A, Berke GS, Geoghegan R (2020) Transoral robotic surgical proficiency via real-time tactile collision awareness system. Laryngoscope 130(Suppl 6):s1–s17
Shin DH, Dalag L, Azhar RA, Santomauro M, Satkunasivam R, Metcalfe C, Dunn M, Berger A, Djaladat H, Nguyen M, Desai MM, Aron M, Gill IS, Hung AJ (2015) A novel interface for the telementoring of robotic surgery. BJU Int 116:302–308
Acknowledgements
The authors would like to thank all the volunteers who participated in this study for their kind support.
Funding
This study was supported by Zhongnan Hospital of Wuhan University Science, Technology and Innovation Seed Fund. The title of our funded project was “Project Stereo vision-based determination and characterization of surgical robot operator trajectory” (Grant No. znpy2019003); Provincial Teaching Research Projects in Hubei Universities (dated 2022013).
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Disclosures
Lingxiao Jiang, Gaojie Chen, Lu Li, Ziyan Chen, Kun Yang, and Xinghuan Wang have no conflicts of interest or financial ties to disclose.
Ethical approval
The study was approved by the Ethics Committee of Zhongnan Hospital of Wuhan University (ID: 2023074k) and was registered at ChiCTR (ID: ChiCTR2300071027).
Informed consent
All participants were provided with detailed information about the study and signed an informed consent form in writing.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
464_2023_10443_MOESM1_ESM.tif
Supplementary file1 (TIF 267 KB) Supplementary Figure 1. The sensor emits a horizontal detection line. When the front arm blocks the detection line on the armrest, the sensor does not sound a warning tone. When the front arm is lifted off the armrest, the detection line is not blocked by the forearm. The sensor can emit a “left or right hand” warning tone, indicating that the forearm has too much range of motion
464_2023_10443_MOESM2_ESM.tif
Supplementary file2 (TIF 574 KB) Supplementary Figure 2. Through OBS, multi-channel video sources are collected and the operation is displayed to the remote end using the Tencent Meeting shared screen. All participants can interact with the voice by connecting to a Bluetooth headset
464_2023_10443_MOESM3_ESM.tif
Supplementary file3 (TIF 208 KB) Supplementary Figure 3. The effect of training order on the results of PB2: The left graph shows the results of comparing the overall score of the first three and the last three in the control group, and the right graph shows the results of comparing the overall score of the first three and the last three in the remote group
464_2023_10443_MOESM4_ESM.tif
Supplementary file4 (TIF 250 KB) Supplementary Figure 4. The effect of training order on the results of MB2: The left graph shows the results of comparing the overall score of the first three and the last three in the control group, and the right graph shows the results of comparing the overall score of the first three and the last three in the remote group
464_2023_10443_MOESM5_ESM.tif
Supplementary file5 (TIF 1609 KB) Supplementary Figure 5. (a):Trainer instruction at the remote side; (b):Route Planning; (c):Remind the angle of the clamping and release; (d):Remind the trainees to adjust their foot placement; (e): Reminded of the improper force which caused the instrument to turn red; (f):Reminder of improper needle holding position and needle feeding angle
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Jiang, L., Chen, G., Li, L. et al. Remote teaching system for robotic surgery and its validation: results of a randomized controlled study. Surg Endosc 37, 9190–9200 (2023). https://doi.org/10.1007/s00464-023-10443-w
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-023-10443-w