Abstract
Background
Preoperative optimization cut-offs are frequently utilized to determine eligibility for elective ventral hernia repair. Our objective was to assess the relationship between gender, race, and socioeconomic status and preoperative optimization goals.
Methods
We queried our institutional database for adults with ventral hernia diagnoses between 2016 and 2021. Demographics, comorbidities, laboratory, and operative data were collected and analyzed. The following cut-offs were used to determine eligibility for elective repair: body mass index (BMI) < 40 kg/m2, no active smoking, and glycated hemoglobin (HbA1c) < 8%. Socioeconomic status was assessed using the Distressed Communities Index.
Results
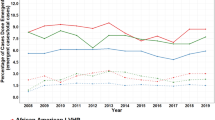
A total of 5638 patients were included [Whites = 4321 (77%), Blacks = 794 (14%), Hispanics = 318 (6%), and other/unknown 205 (4%)]. Median age was 61 years and 50% were male. Most common hernia types were umbilical (36%) and incisional (20%). 10% had BMI > 40 kg/m2, 9% were active smokers and 4% had HbA1c > 8%. 21% of all patients did not meet the preoperative optimization cut-offs at time of diagnosis and those were less likely to undergo hernia repair during the study timeframe compared to those who did (OR 0.50; 95% CI [0.42–0.60]). There was a higher proportion of females (21%) and Blacks (22%) with BMI > 40 kg/m2 compared to males (11%) and other races (11–15%), p = 0.002. As the level of socioeconomic distress increased, there was a corresponding increase in the proportion of patients who did not meet preoperative optimization cut-offs from 16% in prosperous communities to 25% in distressed communities (p < 0.0001).
Conclusion
Nearly 1 of 5 patients with ventral hernias is affected by commonly used arbitrary preoperative optimization cut-offs. These cut-offs disproportionately impact females, Black patients and those with higher socioeconomic distress. These disparities need to be considered when planning preoperative optimization protocols and resource allocation to ensure equitable access to elective ventral hernia repair.
Graphical abstract



Similar content being viewed by others
References
Liang MK, Holihan JL, Itani K, Alawadi ZM, Gonzalez JRF, Askenasy EP, Ballecer C, Chong HS, Goldblatt MI, Greenberg JA, Harvin JA, Keith JN, Martindale RG, Orenstein S, Richmond B, Roth JS, Szotek P, Towfigh S, Tsuda S, Vaziri K, Berger DH (2017) Ventral hernia management: expert consensus guided by systematic review. Ann Surg 265:80–89. https://doi.org/10.1097/SLA.0000000000001701
Grove TN, Kontovounisios C, Montgomery A, Heniford BT, Windsor ACJ, Warren OJ (2021) Perioperative optimization in complex abdominal wall hernias: Delphi consensus statement. BJS Open 5:zrab082. https://doi.org/10.1093/bjsopen/zrab082
Arroyo-Johnson C, Mincey KD (2016) Obesity epidemiology trends by race/ethnicity, gender, and education: National Health Interview Survey, 1997–2012. Gastroenterol Clin North Am 45:571–579. https://doi.org/10.1016/j.gtc.2016.07.012
Syamlal G, Mazurek JM, Dube SR (2014) Gender differences in smoking among U.S. working adults. Am J Prev Med 47:467–475. https://doi.org/10.1016/j.amepre.2014.06.013
Wong RJ, Chou C, Ahmed A (2014) Long term trends and racial/ethnic disparities in the prevalence of obesity. J Community Health 39:1150–1160. https://doi.org/10.1007/s10900-014-9870-6
Hiscock R, Bauld L, Amos A, Fidler JA, Munafò M (2012) Socioeconomic status and smoking: a review. Ann N Y Acad Sci 1248:107–123. https://doi.org/10.1111/j.1749-6632.2011.06202.x
Beckles GL, Chou C-F (2016) Disparities in the prevalence of diagnosed diabetes—United States, 1999–2002 and 2011–2014. MMWR Morb Mortal Wkly Rep 65:1265–1269. https://doi.org/10.15585/mmwr.mm6545a4
Mehaffey JH, Hawkins RB, Charles EJ, Turrentine FE, Hallowell PT, Friel C, Jones RS, Tracci MC (2020) Socioeconomic “Distressed Communities Index” improves surgical risk-adjustment. Ann Surg 271:470–474. https://doi.org/10.1097/SLA.0000000000002997
Carmichael H, Moore A, Steward L, Velopulos CG (2020) Disparities in emergency versus elective surgery: comparing measures of neighborhood social vulnerability. J Surg Res 256:397–403. https://doi.org/10.1016/j.jss.2020.07.002
Delaney LD, Howard R, Palazzolo K, Ehlers AP, Smith S, Englesbe M, Dimick JB, Telem DA (2021) Outcomes of a presurgical optimization program for elective hernia repairs among high-risk patients. JAMA Netw Open 4:e2130016. https://doi.org/10.1001/jamanetworkopen.2021.30016
Delaney LD, Kattapuram M, Haidar JA, Chen AS, Quiroga G, Telem DA, Howard R (2021) The impact of surgeon adherence to preoperative optimization of hernia repairs. J Surg Res 264:8–15. https://doi.org/10.1016/j.jss.2021.01.044
Howard R, Ehlers A, Delaney L, Solano Q, Shen M, Englesbe M, Dimick J, Telem D (2022) Sex disparities in the treatment and outcomes of ventral and incisional hernia repair. Surg Endosc. https://doi.org/10.1007/s00464-022-09475-5
Best MJ, McFarland EG, Thakkar SC, Srikumaran U (2021) Racial disparities in the use of surgical procedures in the US. JAMA Surg 156:274–281. https://doi.org/10.1001/jamasurg.2020.6257
Hoffman RD, Danos DM, Lau FH (2021) National health disparities in incisional hernia repair outcomes: an analysis of the Healthcare Cost and Utilization Project National Inpatient Sample (HCUP-NIS) 2012–2014. Surgery 169:1393–1399. https://doi.org/10.1016/j.surg.2020.11.028
Katzen M, Sacco J, Ku D, Scarola G, Colavita P, Augenstein V, Heniford BT (2022) Impact of race and ethnicity on rates of emergent ventral hernia repair (VHR): has anything changed? Surg Endosc. https://doi.org/10.1007/s00464-022-09732-7
Docimo S, Spaniolas K, Yang J, Talamini MA, Pryor AD (2020) Health care disparity exists among those undergoing emergent hernia repairs in New York State. Hernia J Hernias Abdom Wall Surg. https://doi.org/10.1007/s10029-020-02244-0
Renshaw SM, Olson MA, Poulose BK, Collins CE (2022) Community distress as a predictor of early hernia recurrence for older adults undergoing ventral hernia repair (VHR). Surg Endosc. https://doi.org/10.1007/s00464-022-09587-y
Tracy BM, Finnegan TM, Smith RN, Senkowski CK (2021) Random forest modeling using socioeconomic distress predicts hernia repair approach. Surg Endosc 35:3890–3895. https://doi.org/10.1007/s00464-020-07860-6
Cox TC, Blair LJ, Huntington CR, Colavita PD, Prasad T, Lincourt AE, Heniford BT, Augenstein VA (2016) The cost of preventable comorbidities on wound complications in open ventral hernia repair. J Surg Res 206:214–222. https://doi.org/10.1016/j.jss.2016.08.009
Owei L, Swendiman RA, Kelz RR, Dempsey DT, Dumon KR (2017) Impact of body mass index on open ventral hernia repair: a retrospective review. Surgery 162:1320–1329. https://doi.org/10.1016/j.surg.2017.07.025
Tastaldi L, Krpata DM, Prabhu AS, Petro CC, Rosenblatt S, Haskins IN, Olson MA, Stewart TG, Rosen MJ, Greenberg JA (2019) The effect of increasing body mass index on wound complications in open ventral hernia repair with mesh. Am J Surg 218:560–566. https://doi.org/10.1016/j.amjsurg.2019.01.022
Sorensen LT, Friis E, Jorgensen T, Vennits B, Andersen BR, Rasmussen GI, Kjaergaard J (2002) Smoking is a risk factor for recurrence of groin hernia. World J Surg 26:397–400. https://doi.org/10.1007/s00268-001-0238-6
Goodenough CJ, Liang MK, Nguyen MT, Nguyen DH, Holihan JL, Alawadi ZM, Roth JS, Wray CJ, Ko TC, Kao LS (2015) Preoperative glycosylated hemoglobin and postoperative glucose together predict major complications after abdominal surgery. J Am Coll Surg 221:854–861.e1. https://doi.org/10.1016/j.jamcollsurg.2015.07.013
Won EJ, Lehman EB, Geletzke AK, Tangel MR, Matsushima K, Brunke-Reese D, Pichardo-Lowden AR, Pauli EM, Soybel DI (2015) Association of postoperative hyperglycemia with outcomes among patients with complex ventral hernia repair. JAMA Surg 150:433–440. https://doi.org/10.1001/jamasurg.2014.3160
Maspero M, Bertoglio CL, Morini L, Alampi B, Mazzola M, Girardi V, Zironda A, Barone G, Magistro C, Ferrari G (2022) Laparoscopic ventral hernia repair in patients with obesity: should we be scared of body mass index? Surg Endosc 36:2032–2041. https://doi.org/10.1007/s00464-021-08489-9
Addo A, Lu R, Broda A, George P, Huerta N, Park A, Zahiri HR, Belyansky I (2021) Impact of Body Mass Index (BMI) on perioperative outcomes following minimally invasive retromuscular abdominal wall reconstruction: a comparative analysis. Surg Endosc 35:5796–5802. https://doi.org/10.1007/s00464-020-08069-3
Petro CC, Haskins IN, Tastaldi L, Tu C, Krpata DM, Rosen MJ, Prabhu AS (2019) Does active smoking really matter before ventral hernia repair? An AHSQC analysis. Surgery 165:406–411. https://doi.org/10.1016/j.surg.2018.07.039
Al-Mansour MR, Vargas M, Olson MA, Gupta A, Read TE, Algarra NN (2022) S-144 lack of association between glycated hemoglobin and adverse outcomes in diabetic patients undergoing ventral hernia repair: an ACHQC study. Surg Endosc. https://doi.org/10.1007/s00464-022-09479-1
James TJ, Hawley L, Ding L, Alicuben ET, Samakar K (2021) Impact of a Body Mass Index threshold on abdominal wall hernia repair at a safety-net hospital. Am Surg. https://doi.org/10.1177/00031348211047504
Acknowledgements
We acknowledge the University of Florida Integrated Data Repository (IDR) and the UF Health Office of the Chief Data Officer for providing the analytic data set for this project. Additionally, the research reported in this publication was supported by the National Center for Advancing Translational Sciences of the National Institutes of Health under the University of Florida Clinical and Translational Science Award UL1TR001427. The content of this publication, presentation, and/or proposal is solely the responsibility of the authors and does not necessarily represent the official views of the National Institutes of Health.
Funding
No funding was received for this project.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Disclosures
Mazen R. Al-Mansour received speaker fees from Medtronic Inc., educational support from Intuitive Surgical and general payments from W. L. Gore & Associates, Inc. Khal-Hentz Gabriel and Dan Neal have no conflicts of interest or financial ties to disclose.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Al-Mansour, M.R., Gabriel, KH. & Neal, D. Gender, racial, and socioeconomic disparity of preoperative optimization goals in ventral hernia repair. Surg Endosc 37, 9399–9405 (2023). https://doi.org/10.1007/s00464-023-10365-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-023-10365-7