Abstract
Background
Research on the utilization of robotic surgical approaches in the management of inflammatory bowel disease (IBD) is limited. The aims of this study were to identify temporal trends in robotic utilization and compare the safety of a robotic to laparoscopic operative approach in patients with IBD.
Methods
Patients who underwent minimally invasive surgery (MIS) for IBD were identified using the American College of Surgeons National Surgical Quality Improvement Program (ACS-NSQIP) database (2013–2021). Temporal trends of robotic utilization were assessed from 2013 to 2021. Primary (30-day overall and serious morbidity) and secondary (unplanned conversion to open) outcomes were assessed between 2019 and 2021, when robotic utilization was highest. Multivariable logistic regression was performed.
Results
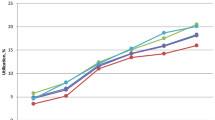
The use of a robotic approach for colectomies and proctectomies increased significantly between 2013 and 2021 (p < 0.001), regardless of disease type. A total of 6016 patients underwent MIS for IBD between 2019 and 2021. 2234 (37%) patients had surgery for UC [robotic 430 (19.3%), lap 1804 (80%)] and 3782 (63%) had surgery for CD [robotic 500 (13.2%), lap 3282 (86.8%)]. For patients with UC, there was no difference in rates of overall morbidity (22.6% vs. 20.7%, p = 0.39), serious morbidity (11.4% vs. 12.3%, p = 0.60) or conversion to open (1.5% vs. 2.1%, p = 0.38) between the laparoscopic and robotic approaches, respectively. There was no difference in overall morbidity between the two groups in patients with CD (lap 14.0% vs robotic 16.4%, p = 0.15), however the robotic group exhibited higher rates of serious morbidity (7.3% vs. 11.2%, p < 0.01), shorter LOS (3 vs. 4 days, p < 0.001) and lower rates of conversion to an open procedure (3.8% vs. 1.6%, p = 0.02). Adjusted analysis showed similar results.
Conclusion
The use of the robotic platform in the surgical management of IBD is increasing and is not associated with an increase in 30-day overall morbidity compared to a laparoscopic approach.



Similar content being viewed by others
References
Ng SC, Shi HY, Hamidi N, Underwood FE, Tang W, Benchimol EI, Panaccione R, Ghosh S, Wu JCY, Chan FKL, Sung JJY, Kaplan GG (2017) Worldwide incidence and prevalence of inflammatory bowel disease in the 21st century: a systematic review of population-based studies. Lancet Lond Engl 390:2769–2778
Windsor JW, Kaplan GG (2019) Evolving epidemiology of IBD. Curr Gastroenterol Rep 21:40
Dahlhamer JM, Zammitti EP, Ward BW, Wheaton AG, Croft JB (2016) Prevalence of inflammatory bowel disease among adults aged ≥18 years—United States, 2015. MMWR Morb Mortal Wkly Rep 65:1166–1169
GBD 2017 Inflammatory Bowel Disease Collaborators (2020) The global, regional, and national burden of inflammatory bowel disease in 195 countries and territories, 1990–2017: a systematic analysis for the Global Burden of Disease Study 2017. Lancet Gastroenterol. Hepatol. 5:17–30
Turner D, Ricciuto A, Lewis A, D’Amico F, Dhaliwal J, Griffiths AM, Bettenworth D, Sandborn WJ, Sands BE, Reinisch W, Schölmerich J, Bemelman W, Danese S, Mary JY, Rubin D, Colombel J-F, Peyrin-Biroulet L, Dotan I, Abreu MT, Dignass A, International Organization for the Study of IBD (2021) STRIDE-II: an update on the selecting therapeutic targets in inflammatory bowel disease (STRIDE) initiative of the international organization for the study of IBD (IOIBD): determining therapeutic goals for treat-to-target strategies in IBD. Gastroenterology 160:1570–1583
Kotze PG, Holubar SD, Lipman JM, Spinelli A (2021) Training for minimally invasive surgery for IBD: a current need. Clin Colon Rectal Surg 34:172–180
Crippa J, Carvello M, Kotze PG, Spinelli A (2021) Robotic surgery in inflammatory bowel disease. Curr Drug Targets 22:112–116
Hansraj N, Kavic SM (2015) Surgery for Crohn’s disease: an emerging surgical specialty. Inflamm Bowel Dis 21:E28-29
Abd El Aziz MA, Grass F, Behm KT, D’Angelo A-L, Mathis KL, Dozois EJ, Larson DW (2022) Trends and consequences of surgical conversion in the United States. Surg Endosc 36:82–90
Miller AT, Berian JR, Rubin M, Hurst RD, Fichera A, Umanskiy K (2012) Robotic-assisted proctectomy for inflammatory bowel disease: a case-matched comparison of laparoscopic and robotic technique. J Gastrointest Surg 16:587–594
Rencuzogullari A, Gorgun E, Costedio M, Aytac E, Kessler H, Abbas MA, Remzi FH (2016) Case-matched comparison of robotic versus laparoscopic proctectomy for inflammatory bowel disease. Surg Laparosc Endosc Percutan Tech 26:e37-40
Huerta S, Meier J, Emuakhagbon V-S, Favela J, Argo M, Polanco PM, Augustine MM, Pham T (2021) A comparative analysis of outcomes of open, laparoscopic, and robotic elective (procto-) colectomies for benign and malignant disease. J Robot Surg 15:53–62
Flynn J, Larach JT, Kong JCH, Waters PS, Warrier SK, Heriot A (2021) The learning curve in robotic colorectal surgery compared with laparoscopic colorectal surgery: a systematic review. Colorectal Dis Off J Assoc Coloproctol G B Irel 23:2806–2820
American College of Surgeons (ACS) (n.d.) ACS NSQIP participant use data file. https://www.facs.org/quality-programs/data-and-registries/acs-nsqip/participant-use-data-file/. Accessed 13 Jan 2023
American College of Surgeons (ACS) (n.d.) About ACS NSQIP. https://www.facs.org/quality-programs/data-and-registries/acs-nsqip/about-acs-nsqip/. Accessed 13 Jan 2023
Shinall MC, Arya S, Youk A, Varley P, Shah R, Massarweh NN, Shireman PK, Johanning JM, Brown AJ, Christie NA, Crist L, Curtin CM, Drolet BC, Dhupar R, Griffin J, Ibinson JW, Johnson JT, Kinney S, LaGrange C, Langerman A, Loyd GE, Mady LJ, Mott MP, Patri M, Siebler JC, Stimson CJ, Thorell WE, Vincent SA, Hall DE (2020) Association of preoperative patient frailty and operative stress with postoperative mortality. JAMA Surg 155:e194620
Yan Q, Kim J, Hall DE, Shinall MC Jr, Reitz KM, Stitzenberg KB, Kao LS, George EL, Youk A, Wang CP, Silverstein JC, Bernstam EV, Shireman PK (2023) Association of frailty and the expanded operative stress score with preoperative acute serious conditions, complications, and mortality in males compared to females: a retrospective observational study. Ann Surg 277(2):e294–e304
Dindo D, Demartines N, Clavien P-A (2004) Classification of surgical complications: a new proposal with evaluation in a cohort of 6336 patients and results of a survey. Ann Surg 240:205–213
Gaglani T, Davis CH, Bailey HR, Cusick MV (2019) Trends and outcomes for minimally invasive surgery for inflammatory bowel disease. J Surg Res 235:303–307
Ramji KM, Cleghorn MC, Josse JM, MacNeill A, O’Brien C, Urbach D, Quereshy FA (2016) Comparison of clinical and economic outcomes between robotic, laparoscopic, and open rectal cancer surgery: early experience at a tertiary care center. Surg Endosc 30:1337–1343
Baek S-J, Kim S-H, Cho J-S, Shin J-W, Kim J (2012) Robotic versus conventional laparoscopic surgery for rectal cancer: a cost analysis from a single institute in Korea. World J Surg 36:2722–2729
Flynn J, Larach JT, Kong JCH, Warrier SK, Heriot A (2021) Robotic versus laparoscopic ileal pouch-anal anastomosis (IPAA): a systematic review and meta-analysis. Int J Colorectal Dis 36:1345–1356
Shrestha B (2016) Minimally invasive surgery for inflammatory bowel disease: current perspectives. World J Gastrointest Pharmacol Ther 7:214–216
Acknowledgements
The authors would like to acknowledge the role of the Johns Hopkins Surgery Center for Outcomes (JSCOR) for supporting this study.
Funding
Shannon N. Radomski received financial support from National Cancer Institute (NCI) Grant 5T32CA126607-12. Mr. Edwin Lewis provided generous support of Dr. Efron’s Department of Surgery Research Fund. The Nicholl Family Foundation provided generous support of the Johns Hopkins Division of Colorectal Surgery Research Fund.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Disclosures
Vincent J. Obias formerly served as a consultant for Intuitive Surgical, Inc. Shannon N Radomski, Miloslawa Stem, Michael Consul, Jay Rammohan Maturi, Haniee Chung, Susan Gearhart and Ada Graham have no relevant financial or non-financial interests to disclose.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Radomski, S.N., Stem, M., Consul, M. et al. National trends and feasibility of a robotic surgical approach in the management of patients with inflammatory bowel disease. Surg Endosc 37, 7849–7858 (2023). https://doi.org/10.1007/s00464-023-10333-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-023-10333-1