Abstract
Background
Gastric cancer is associated with significant mortality worldwide. Radical gastrectomy with lymphadenectomy is considered the only curative option. Traditionally, these operations are associated with significant morbidity. Laparoscopic gastrectomy (LG) and more recently robotic gastrectomy (RG) techniques have been developed to potentially decrease the perioperative morbidity. We sought to compare oncologic outcomes with laparoscopic and robotic techniques for gastrectomy.
Methods
Utilizing the National Cancer Database we identified patients who underwent gastrectomy for adenocarcinoma. Patients were stratified by open, robotic or laparoscopic surgical technique. Open gastrectomy patients were excluded.
Results
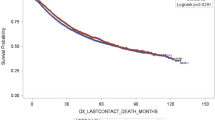
We identified 1,301 patients who underwent RG and 4,892 LG with median ages of 65 (20–90) and 66 (18–90) respectively, p = 0.02. The mean number of positive lymph nodes were higher in the LG 2.2 ± 4.4 vs RG 1.9 ± 3.8, p = 0.01. The R0 resections were higher in the RG at 94.5% vs 91.9% in LG, p = 0.001. Conversions to open were 7.1% in the RG and 16% in the LG group, p < 0.001. The median length of hospitalization was 8 (6–11) in both groups. There was no difference in the 30-day readmission (p = 0.65), 30-day mortality (p = 0.85) and 90-day mortality (p = 0.34) between groups. The median and overall 5-year survival was 71.3 mo and 56% in the RG and 66.1 mo and 52% in the LG, p = 0.03. Multivariate analysis revealed that age, Charlson-Deyo comorbidity scores, location of gastric cancer, histology grade, pathologic T-stage, pathologic N-stage, surgical margins, and facility volume were all predictors of survival.
Conclusions
Robotic and laparoscopic techniques are both acceptable approaches to gastrectomy. However, conversions to open are higher and R0 resections rates are lower in the laparoscopic group. Additionally, a survival benefit is demonstrated in those undergoing robotic gastrectomy.
Graphical abstract




Similar content being viewed by others
References
Siegel RL, Miller KD, Fuchs HE, Jemal A (2022) Cancer statistics, 2022. CA Cancer J Clin 72:7–33
Huang C, Liu H, Hu Y, Sun Y, Su X, Cao H et al (2022) Laparoscopic vs open distal gastrectomy for locally advanced gastric cancer: five-year outcomes from the CLASS-01 randomized clinical trial. JAMA Surg 157:9–17
Liu F, Huang C, Xu Z, Su X, Zhao G, Ye J et al (2020) Morbidity and mortality of laparoscopic vs open total gastrectomy for clinical stage i gastric cancer: the CLASS02 multicenter randomized clinical trial. JAMA Oncol 6:1590–1597
Kostakis ID, Alexandrou A, Armeni E, Damaskos C, Kouraklis G, Diamantis T et al (2017) Comparison between minimally invasive and open gastrectomy for gastric cancer in Europe: a systematic review and meta-analysis. Scand J Surg 106:3–20
Katai H, Mizusawa J, Katayama H, Morita S, Yamada T, Bando E et al (2020) Survival outcomes after laparoscopy-assisted distal gastrectomy versus open distal gastrectomy with nodal dissection for clinical stage IA or IB gastric cancer (JCOG0912): a multicentre, non-inferiority, phase 3 randomised controlled trial. Lancet Gastroenterol Hepatol 5:142–151
Hyung W, Yang H, Park Y, Lee H, An J, Kim W et al (2020) Long-Term outcomes of laparoscopic distal gastrectomy for locally advanced gastric cancer: the KLASS-02-RCT randomized clinical TRIAL. J Clin Oncol 38:3304–3313
Etoh T, Ohyama T, Sakuramoto S, Tsuji T, Lee S, Yoshida K et al (2023) Five-year survival outcomes of laparoscopy-assisted vs open distal gastrectomy for advanced gastric cancer: the JLSSG0901 randomized clinical trial. JAMA Surg 158:445–454
Li ZY, Zhou YB, Li TY, Li JP, Zhou ZW, She JJ et al (2021) Robotic gastrectomy versus laparoscopic gastrectomy for gastric cancer: a multicenter cohort study of 5402 Patients in China. Ann Surg. https://doi.org/10.1097/SLA.0000000000005046
Ojima T, Nakamura M, Hayata K, Kitadani J, Katsuda M, Takeuchi A et al (2021) Short-term outcomes of robotic gastrectomy vs laparoscopic gastrectomy for patients with gastric cancer: a randomized clinical trial. JAMA Surg 156:954–963
Zheng-Yan L, Yong-Liang Z, Feng Q, Yan S, Pei-Wu Y (2021) Morbidity and short-term surgical outcomes of robotic versus laparoscopic distal gastrectomy for gastric cancer: a large cohort study. Surg Endosc 35:3572–3583
Hikage M, Fujiya K, Kamiya S, Tanizawa Y, Bando E, Notsu A et al (2021) Robotic gastrectomy compared with laparoscopic gastrectomy for clinical stage I/II gastric cancer patients: a propensity score-matched analysis. World J Surg 45:1483–1494
Yue F, Geng X (2017) Impact of conversion during laparoscopic gastrectomy on outcomes of patients with gastric cancer. J BUON 22:926–931
Hu Y, Huang C, Sun Y, Su X, Cao H, Hu J et al (2016) Morbidity and mortality of laparoscopic versus open D2 distal gastrectomy for advanced gastric cancer: a randomized controlled trial. J Clin Oncol 34:1350–1357
Xie FN, Chen J, Li ZY, Bai B, Song D, Xu S et al (2021) Impact of laparoscopic converted to open gastrectomy on short- and long-term outcomes of patients with locally advanced gastric cancer: a propensity score-matched analysis. J Gastrointest Surg 25:2484–2494
Stiekema J, Trip AK, Jansen EP, Boot H, Cats A, Ponz OB et al (2014) The prognostic significance of an R1 resection in gastric cancer patients treated with adjuvant chemoradiotherapy. Ann Surg Oncol 21:1107–1114
Postlewait LM, Squires MH, Kooby DA, Poultsides GA, Weber SM, Bloomston M et al (2015) The importance of the proximal resection margin distance for proximal gastric adenocarcinoma: A multi-institutional study of the US Gastric Cancer Collaborative. J Surg Oncol 112:203–207
Cordero-García E, Ramos-Esquivel A, Alpízar-Alpízar W (2018) Predictors of overall survival after surgery in gastric cancer patients from a Latin-American country. J Gastrointest Oncol 9:64–72
Choi M, Ishizawa S, Kraemer D, Sasson A, Feinberg E (2022) Perioperative chemotherapy versus adjuvant chemotherapy strategies in resectable gastric and gastroesophageal cancer: A Markov decision analysis. Eur J Surg Oncol 48:403–410
Cats A, Jansen EPM, van Grieken NCT, Sikorska K, Lind P, Nordsmark M et al (2018) Chemotherapy versus chemoradiotherapy after surgery and preoperative chemotherapy for resectable gastric cancer (CRITICS): an international, open-label, randomised phase 3 trial. Lancet Oncol 19:616–628
Kim S, Lim DH, Lee J, Kang WK, MacDonald JS, Park CH et al (2005) An observational study suggesting clinical benefit for adjuvant postoperative chemoradiation in a population of over 500 cases after gastric resection with D2 nodal dissection for adenocarcinoma of the stomach. Int J Radiat Oncol Biol Phys 63:1279–1285
Bang YJ, Kim YW, Yang HK, Chung HC, Park YK, Lee KH et al (2012) Adjuvant capecitabine and oxaliplatin for gastric cancer after D2 gastrectomy (CLASSIC): a phase 3 open-label, randomised controlled trial. Lancet 379:315–321
Lu J, Zheng CH, Xu BB, Xie JW, Wang JB, Lin JX et al (2021) Assessment of robotic versus laparoscopic distal gastrectomy for gastric cancer: a randomized controlled trial. Ann Surg 273:858–867
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Disclosure
Caitlin Takahashi, Jamie Glasser, Cassie Schuster, Jamie Huston, Ravi Shridhar and Kenneth Meredith have no conflicts of interest or financial ties to disclose.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Takahashi, C., Glasser, J., Schuster, C. et al. Comparative outcomes of laparoscopic and robotic approaches to gastrectomy: a National Cancer Database study. Surg Endosc 37, 7530–7537 (2023). https://doi.org/10.1007/s00464-023-10204-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-023-10204-9