Abstract
Background
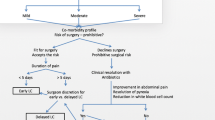
Early laparoscopic cholecystectomy (ELC) for acute cholecystitis (AC) poses multiple challenges. The Tokyo Guidelines 2018 (TG18) eliminated the time limit (< 72 h) and expanded the surgical indication to severe AC. This study aimed to evaluate the clinical outcomes of ELC for AC following the TG18 in a single high-volume center.
Methods
From 2019 to 2021, we managed all AC patients with a TG18 flowchart and prospectively enrolled those who underwent ELC within 7 days of symptom onset. The primary outcome was overall morbidity, with a comparison between mild (Grade I) and moderate/severe (Grade II/III) AC.
Results
During the study period, 201 patients underwent ELC was for Grade I (56.2%), II (40.3%), and III (3.5%) ACs. Mean age was 69 ± 15.2 years and time to surgery from symptom onset was 0 (12.9%), 1–3 (66.7%), and 4–7 days (20.4%). Mean operative time and blood loss were 118.9 ± 42.7 min and 57.8 ± 99.4 mL, respectively. The critical view of safety (CVS) was achieved in 76.1% of patients, and bailout procedures were performed in 21.4%. There were no open conversions or bile duct injuries. Major morbidities (Clavien–Dindo classification ≥ IIIa) were observed in 5.5% of cases and mortality in 0.5%. Comparing Grades II/III to Grade I, operative time was longer (112.3 vs. 127.3 min, p = 0.014), blood loss was higher (40.3 vs. 80.1 mL, p = 0.005), the CVS rate was lower (83.2 vs. 67.0%, p = 0.012), and the major morbidity rate was higher (1.8 vs. 10.2%, p = 0.012). In the subgroup analysis of Grade II/III, there were no significant differences in major morbidities (p = 0.288) between the two groups (0–3 vs. 4–7 days).
Conclusion
ELC for AC following TG18 is feasible with low morbidity rates. However, ELC for Grade II/III ACs remains challenging, and surgeons must carefully assess intraoperative difficulties and surgical risks before proceeding.


Similar content being viewed by others
References
Indar AA, Beckingham IJ (2002) Acute cholecystitis. BMJ 325:639–643
Gallaher JR, Charles A (2022) Acute cholecystitis: a review. JAMA 327:965–975
Lo CM, Liu CL, Fan ST, Lai EC, Wong J (1998) Prospective randomized study of early versus delayed laparoscopic cholecystectomy for acute cholecystitis. Ann Surg 227:461–467
Kolla SB, Aggarwal S, Kumar A, Kumar R, Chumber S, Parshad R, Seenu V (2004) Early versus delayed laparoscopic cholecystectomy for acute cholecystitis: a prospective randomized trial. Surg Endosc 18:1323–1327
Gutt CN, Encke J, Köninger J, Harnoss JC, Weigand K, Kipfmüller K, Schunter O, Götze T, Golling MT, Menges M, Klar E, Feilhauer K, Zoller WG, Ridwelski K, Ackmann S, Baron A, Schön MR, Seitz HK, Daniel D, Stremmel W, Büchler MW (2013) Acute cholecystitis: early versus delayed cholecystectomy, a multicenter randomized trial (ACDC study, NCT00447304). Ann Surg 258:385–393
Yokoe M, Hata J, Takada T, Strasberg SM, Asbun HJ, Wakabayashi G, Kozaka K, Endo I, Deziel DJ, Miura F, Okamoto K, Hwang TL, Huang WS, Ker CG, Chen MF, Han HS, Yoon YS, Choi IS, Yoon DS, Noguchi Y, Shikata S, Ukai T, Higuchi R, Gabata T, Mori Y, Iwashita Y, Hibi T, Jagannath P, Jonas E, Liau KH, Dervenis C, Gouma DJ, Cherqui D, Belli G, Garden OJ, Giménez ME, de Santibañes E, Suzuki K, Umezawa A, Supe AN, Pitt HA, Singh H, Chan ACW, Lau WY, Teoh AYB, Honda G, Sugioka A, Asai K, Gomi H, Itoi T, Kiriyama S, Yoshida M, Mayumi T, Matsumura N, Tokumura H, Kitano S, Hirata K, Inui K, Sumiyama Y, Yamamoto M (2018) Tokyo Guidelines 2018: diagnostic criteria and severity grading of acute cholecystitis (with videos). J Hepatobiliary Pancreat Sci 25:41–54
Okamoto K, Suzuki K, Takada T, Strasberg SM, Asbun HJ, Endo I, Iwashita Y, Hibi T, Pitt HA, Umezawa A, Asai K, Han HS, Hwang TL, Mori Y, Yoon YS, Huang WS, Belli G, Dervenis C, Yokoe M, Kiriyama S, Itoi T, Jagannath P, Garden OJ, Miura F, Nakamura M, Horiguchi A, Wakabayashi G, Cherqui D, de Santibañes E, Shikata S, Noguchi Y, Ukai T, Higuchi R, Wada K, Honda G, Supe AN, Yoshida M, Mayumi T, Gouma DJ, Deziel DJ, Liau KH, Chen MF, Shibao K, Liu KH, Su CH, Chan ACW, Yoon DS, Choi IS, Jonas E, Chen XP, Fan ST, Ker CG, Giménez ME, Kitano S, Inomata M, Hirata K, Inui K, Sumiyama Y, Yamamoto M (2018) Tokyo Guidelines 2018: flowchart for the management of acute cholecystitis. J Hepatobiliary Pancreat Sci 25:55–72
Wakabayashi G, Iwashita Y, Hibi T, Takada T, Strasberg SM, Asbun HJ, Endo I, Umezawa A, Asai K, Suzuki K, Mori Y, Okamoto K, Pitt HA, Han HS, Hwang TL, Yoon YS, Yoon DS, Choi IS, Huang WS, Giménez ME, Garden OJ, Gouma DJ, Belli G, Dervenis C, Jagannath P, Chan ACW, Lau WY, Liu KH, Su CH, Misawa T, Nakamura M, Horiguchi A, Tagaya N, Fujioka S, Higuchi R, Shikata S, Noguchi Y, Ukai T, Yokoe M, Cherqui D, Honda G, Sugioka A, de Santibañes E, Supe AN, Tokumura H, Kimura T, Yoshida M, Mayumi T, Kitano S, Inomata M, Hirata K, Sumiyama Y, Inui K, Yamamoto M (2018) Tokyo Guidelines 2018: surgical management of acute cholecystitis: safe steps in laparoscopic cholecystectomy for acute cholecystitis (with videos). J Hepatobiliary Pancreat Sci 25:73–86
Roulin D, Saadi A, Di Mare L, Demartines N, Halkic N (2016) Early versus delayed cholecystectomy for acute cholecystitis, are the 72 hours still the rule?: a randomized trial. Ann Surg 264:717–722
Amirthalingam V, Low JK, Woon W, Shelat V (2017) Tokyo Guidelines 2013 may be too restrictive and patients with moderate and severe acute cholecystitis can be managed by early cholecystectomy too. Surg Endosc 31:2892–2900
Altieri MS, Brunt LM, Yang J, Zhu C, Talamini MA, Pryor AD (2020) Early cholecystectomy (< 72 h) is associated with lower rate of complications and bile duct injury: a study of 109,862 cholecystectomies in the state of New York. Surg Endosc 34:3051–3056
Devas N, Guenthart A, Nie L, Joshi I, Yang J, Morris-Stiff G, Pryor A (2022) Timing is everything: outcomes of 30,259 delayed cholecystectomies in New York State. Surg Endosc 36:9390–9397
Onishi I, Kayahara M, Yamaguchi T, Yamaguchi Y, Morita A, Sato N, Kurosaka Y, Takegawa S (2022) Surgeons have hesitated early cholecystectomy because of cardiovascular comorbidities during adoption of guidelines. Sci Rep 12:502
Charlson ME, Pompei P, Ales KL, MacKenzie CR (1987) A new method of classifying prognostic comorbidity in longitudinal studies: development and validation. J Chronic Dis 40:373–383
American Society of Anesthesiologists (2014) ASA physical status classification system. https://www.asahq.org/resources/clinical-information/asa-physical-status-classification-system/. Accessed 15 Oct 2014
Strasberg SM, Brunt LM (2010) Rationale and use of the critical view of safety in laparoscopic cholecystectomy. J Am Coll Surg 211:132–138
Strasberg SM (2019) A three-step conceptual roadmap for avoiding bile duct injury in laparoscopic cholecystectomy: an invited perspective review. J Hepatobiliary Pancreat Sci 26:123–127
Mishima K, Wakabayashi G (2021) Tokyo Guidelines and their limits. In: Di Carlo I (ed) Difficult acute cholecystitis. Springer, Cham, pp 47–52. https://doi.org/10.1007/978-3-030-62102-5_5
Bekki T, Abe T, Amano H, Hanada K, Kobayashi T, Noriyuki T, Ohdan H, Nakahara M (2021) Validation of the Tokyo guideline 2018 treatment proposal for acute cholecystitis from a single-center retrospective analysis. Asian J Endosc Surg 14:14–20
Bundgaard NS, Bohm A, Hansted AK, Skovsen AP (2021) Early laparoscopic cholecystectomy for acute cholecystitis is safe regardless of timing. Langenbecks Arch Surg 406:2367–2373
Sabour AF, Matsushima K, Love BE, Alicuben ET, Schellenberg MA, Inaba K, Demetriades D (2020) Nationwide trends in the use of subtotal cholecystectomy for acute cholecystitis. Surgery 167:569–574
Braschi C, Tung C, Tang A, Delgado C, Uribe L, Senekjian L, Keeley JA (2022) Early outcomes of subtotal vs total cholecystectomy for acute cholecystitis. JAMA Surg 157:1062–1064
Kohga A, Suzuki K, Okumura T, Yamashita K, Isogaki J, Kawabe A, Kimura T (2020) Risk factors for postoperative bile leak in patients who underwent subtotal cholecystectomy. Surg Endosc 34:5092–5097
Koo JGA, Chan YH, Shelat VG (2021) Laparoscopic subtotal cholecystectomy: comparison of reconstituting and fenestrating techniques. Surg Endosc 35:1014–1024
Loh AYH, Chean CS, Durkin D, Bhatt A, Athwal TS (2022) Short and long term outcomes of laparoscopic fenestrating or reconstituting subtotal cholecystectomy versus laparoscopic total cholecystectomy in the management of acute cholecystitis. HPB 24:691–699
Nassar A, Elshahat I, Forsyth K, Shaikh S, Ghazanfar M (2022) Outcome of early cholecystectomy compared to percutaneous drainage of gallbladder and delayed cholecystectomy for patients with acute cholecystitis: systematic review and meta-analysis. HPB (Oxford) 24:1622–1633
Acknowledgements
The authors would like to thank Sarah Mitchel and Guy Temporal for their assistance in proofreading the article.
Funding
The authors declare that they have no financial ties or any other types of support to disclose.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Disclosures
This research was approved by the Ethics Committee of Ageo Central General Hospital, Saitam, Japan. Kohei Mishima, Yoshiki Fujiyama, Taiga Wakabayash, Kazuharu Igarash, Takahiro Ozaki, Masayuki Honda, Shozo Mori, Naotake Funamizu, Atsuko Tsutsui, Nobuhiko Okamoto, Jacques Marescaux, and Go Wakabayashi have no conflicts of interest or financial ties to disclose.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Mishima, K., Fujiyama, Y., Wakabayashi, T. et al. Early laparoscopic cholecystectomy for acute cholecystitis following the Tokyo Guidelines 2018: a prospective single-center study of 201 consecutive cases. Surg Endosc 37, 6051–6061 (2023). https://doi.org/10.1007/s00464-023-10094-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-023-10094-x