Abstract
Introduction
Different techniques have been proposed for reoperation after failed anti-reflux surgery. However, there is no consensus on which should be preferred. We aim to report and compare the outcomes of different revisional techniques for failed anti-reflux surgery.
Methods
We performed a retrospective analysis of patients who underwent redo fundoplication (RF) or Roux-en-Y gastric bypass (RYGB) conversion after a failed fundoplication at our institution between 2016 and 2021. The primary outcome was long-term presence of reflux or dysphagia following revisional surgery. Secondary outcomes included 30-day perioperative complications as well as long-term use of anti-reflux medication and radiographic recurrence of hiatal hernia (HH).
Results
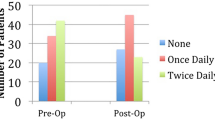
A total of 165 (median age 63 years, 73.9% female) patients were included. RF was performed in 120 (73 Toupet and 47 Nissen), RYGB in 38, and 7 patients had fundoplication takedown alone. The RYGB group had a significantly higher BMI, and more prior revisional surgeries compared to the other groups. Median operative time and length of stay were longer for RYGB. Twenty (12.1%) patients experienced postoperative complications, with the highest incidence in the RYGB group. Reflux and dysphagia improved significantly for the whole cohort, with the greatest improvement noted with reflux in the RYGB group (89.5% with preoperative reflux vs. 10.5% with postoperative reflux, p = < .001). On multivariable regression we found that prior re-operative surgery was associated with persistent reflux and dysphagia, whereas RYGB conversion was protective against reflux.
Conclusion
Conversion to RYGB may offer superior resolution of reflux than RF, especially for obese patients.

Similar content being viewed by others
References
El-Serag HB, Sweet S, Winchester CC, Dent J (2014) Update on the epidemiology of gastro-oesophageal reflux disease: a systematic review. Gut 63(6):871–880
Hampel H, Abraham NS, El-Serag HB (2005) Meta-analysis: obesity and the risk for gastroesophageal reflux disease and its complications. Ann Intern Med 143(3):199–211
Schlottmann F, Herbella FA, Allaix ME, Rebecchi F, Patti MG (2017) Surgical treatment of gastroesophageal reflux disease. World J Surg 41(7):1685–1690
Antiporda M, Jackson C, Smith CD, Thomas M, Elli EF, Bowers SP (2019) Strategies for surgical remediation of the multi-fundoplication failure patient. Surg Endosc 33(5):1474–1481
Grant AM, Boachie C, Cotton SC, Faria R, Bojke L, Epstein DM et al (2013) Clinical and economic evaluation of laparoscopic surgery compared with medical management for gastro-oesophageal reflux disease: 5-year follow-up of multicentre randomised trial (the REFLUX trial). Health Technol Assess 17(22):1–167
Dallemagne B, Weerts J, Markiewicz S, Dewandre JM, Wahlen C, Monami B et al (2006) Clinical results of laparoscopic fundoplication at ten years after surgery. Surg Endosc 20(1):159–165
Obeid NR, Altieri MS, Yang J, Park J, Price K, Bates A et al (2018) Patterns of reoperation after failed fundoplication: an analysis of 9462 patients. Surg Endosc 32(1):345–350
Patti MG, Allaix ME, Fisichella PM (2015) Analysis of the causes of failed antireflux surgery and the principles of treatment: a review. JAMA Surg 150(6):585–590
Maret-Ouda J, Wahlin K, El-Serag HB, Lagergren J (2017) Association between laparoscopic antireflux surgery and recurrence of gastroesophageal reflux. JAMA 318(10):939–946
del Campo SEM, Mansfield SA, Suzo AJ, Hazey JW, Perry KA (2017) Laparoscopic redo fundoplication improves disease-specific and global quality of life following failed laparoscopic or open fundoplication. Surg Endosc 31(11):4649–4655
Coakley KM, Groene SA, Colavita PD, Prasad T, Stefanidis D, Lincourt AE et al (2018) Roux-En-Y gastric bypass following failed fundoplication. Surg Endosc 32(8):3517–3524
Mittal SK, Légner A, Tsuboi K, Juhasz A, Bathla L, Lee TH (2013) Roux-en-Y reconstruction is superior to redo fundoplication in a subset of patients with failed antireflux surgery. Surg Endosc 27(3):927–935
Al Hashmi AW, Pineton de Chambrun G, Souche R, Bertrand M, De Blasi V, Jacques E et al (2019) A retrospective multicenter analysis on redo-laparoscopic anti-reflux surgery: conservative or conversion fundoplication. Surg Endosc 33(1):243–51
Altieri MS, Pryor AD (2015) Gastroesophageal reflux disease after bariatric procedures. Surg Clin North Am 95(3):579–591
Felsenreich DM, Langer FB, Bichler C, Eilenberg M, Jedamzik J, Kristo I et al (2020) Roux-en-Y gastric bypass as a treatment for barrett’s esophagus after sleeve gastrectomy. Obes Surg 30(4):1273–1279
Pallati PK, Shaligram A, Shostrom VK, Oleynikov D, McBride CL, Goede MR (2014) Improvement in gastroesophageal reflux disease symptoms after various bariatric procedures: review of the bariatric outcomes longitudinal database. Surg Obes Relat Dis 10(3):502–507
Shao JM, Elhage SA, Prasad T, Gersin K, Augenstein VA, Colavita PD et al (2021) Best reoperative strategy for failed fundoplication: redo fundoplication or conversion to Roux-en-Y gastric diversion? Surg Endosc 35(7):3865–3873
Giulini L, Razia D, Mittal SK (2022) Redo fundoplication and early Roux-en-Y diversion for failed fundoplication: a 3-year single-center experience. Surg Endosc 36(5):3094–3099
Furnée EJB, Draaisma WA, Broeders IAMJ, Gooszen HG (2009) Surgical reintervention after failed antireflux surgery: a systematic review of the literature. J Gastrointest Surg 13(8):1539–1549
Armijo PR, Pokala B, Misfeldt M, Pagkratis S, Oleynikov D (2019) Predictors of Hiatal hernia recurrence after laparoscopic anti-reflux surgery with Hiatal Hernia repair: a prospective database analysis. J Gastrointest Surg 23(4):696–701
Lidor AO, Kawaji Q, Stem M, Fleming RM, Schweitzer MA, Steele KE et al (2013) Defining recurrence after paraesophageal hernia repair: correlating symptoms and radiographic findings. Surgery 154(2):171–178
Funding
No funding was received for this study.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Disclosures
Drs. Rocio Castillo-Larios, Naga Swati Gunturu, Jorge Cornejo, Spencer W. Trooboff, Abhishek Ramgir Giri, Steven P. Bowers and Enrique F. Elli have no conflicts of interest or financial ties to disclose.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Castillo-Larios, R., Gunturu, N.S., Cornejo, J. et al. Redo fundoplication vs. Roux-en-Y gastric bypass conversion for failed anti-reflux surgery: which is better?. Surg Endosc 37, 6429–6437 (2023). https://doi.org/10.1007/s00464-023-10074-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-023-10074-1