Abstract
Background
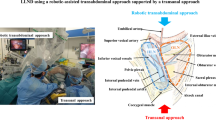
An optimal surgical approach to lateral lymph node dissection (LLND) remains controversial. With the recent popularity of transanal total mesorectal excision, a two-team procedure combining the transabdominal and transanal approaches was established as a novel approach to LLND. This study aimed to clarify the safety and feasibility of two-team LLND (2team-LLND) and compare its short-term outcomes with those of conventional transabdominal LLND (Conv-LLND).
Methods
Between April 2013 and March 2020, 463 patients diagnosed with primary locally advanced rectal cancer underwent a transanal total mesorectal excision; among them, 93 patients who underwent bilateral prophylactic LLND were included in this single-center, retrospective study. Among these patients, 50 and 43 patients underwent Conv-LLND (the Conv-LLND group) and 2team-LLND (the 2team-LLND group), respectively. The short-term outcomes, including the operation time, blood loss volume, number of complications, and number of harvested lymph nodes, were compared between the two groups.
Results
The intraoperative and postoperative complications in the 2team-LLND group were equivalent to those in the Conv-LLND group; furthermore, the incidence of postoperative urinary retention in the 2team-LLND group was acceptably low (9%). Compared with the Conv-LLND group, the 2team-LLND group had a significantly shorter operation time (P = 0.003), lower median blood loss (P = 0.02), and higher number of harvested lateral lymph nodes (P = 0.0005).
Conclusion
The intraoperative and postoperative complications of 2team-LLND were comparable with those of Conv-LLND. Thus, 2team-LLND was safe and feasible for advanced lower rectal cancer. Moreover, it was superior to Conv-LLND in terms of the operation time, blood loss volume, and number of harvested lateral lymph nodes. Therefore, it can be a promising LLND approach.




Similar content being viewed by others
References
Watanabe T, Muro K, Ajioka Y, Hashiguchi Y, Ito Y, Saito Y, Hamaguchi T, Ishida H, Ishiguro M, Ishihara S, Kanemitsu Y, Kawano H, Kinugasa Y, Kokudo N, Murofushi K, Nakajima T, Oka S, Sakai Y, Tsuji A, Uehara K, Ueno H, Yamazaki K, Yoshida M, Yoshino T, Boku N, Fujimori T, Itabashi M, Koinuma N, Morita T, Nishimura G, Sakata Y, Shimada Y, Takahashi K, Tanaka S, Tsuruta O, Yamaguchi T, Yamaguchi N, Tanaka T, Kotake K, Sugihara K (2018) Japanese society for cancer of the colon and rectum (JSCCR) guidelines 2016 for the treatment of colorectal cancer. Int J Clin Oncol 23:1–34
Kobayashi H, Mochizuki H, Kato T, Mori T, Kameoka S, Shirouzu K, Sugihara K (2009) Outcomes of surgery alone for lower rectal cancer with and without pelvic sidewall dissection. Dis Colon Rectum 52:567–576
Glynne-Jones R, Wyrwicz L, Tiret E, Brown G, Rödel C, Cervantes A, Arnold D (2017) Rectal cancer: ESMO clinical practice guidelines for diagnosis, treatment and follow-up. Ann Oncol 28:iv22–iv40
Fujita S, Mizusawa J, Kanemitsu Y, Ito M, Kinugasa Y, Komori K, Ohue M, Ota M, Akazai Y, Shiozawa M, Yamaguchi T, Bandou H, Katsumata K, Murata K, Akagi Y, Takiguchi N, Saida Y, Nakamura K, Fukuda H, Akasu T, Moriya Y (2017) Mesorectal excision with or without lateral lymph node dissection for clinical stage II/III lower rectal cancer (JCOG0212): a multicenter, randomized controlled, noninferiority trial. Ann Surg 266:201–207
Hashiguchi Y, Muro K, Saito Y, Ito Y, Ajioka Y, Hamaguchi T, Hasegawa K, Hotta K, Ishida H, Ishiguro M, Ishihara S, Kanemitsu Y, Kinugasa Y, Murofushi K, Nakajima TE, Oka S, Tanaka T, Taniguchi H, Tsuji A, Uehara K, Ueno H, Yamanaka T, Yamazaki K, Yoshida M, Yoshino T, Itabashi M, Sakamaki K, Sano K, Shimada Y, Tanaka S, Uetake H, Yamaguchi S, Yamaguchi N, Kobayashi H, Matsuda K, Kotake K, Sugihara K (2020) Japanese society for cancer of the colon and rectum (JSCCR) guidelines 2019 for the treatment of colorectal cancer. Int J Clin Oncol 25:1–42
Kyo K, Sameshima S, Takahashi M, Furugori T, Sawada T (2006) Impact of autonomic nerve preservation and lateral node dissection on male urogenital function after total mesorectal excision for lower rectal cancer. World J Surg 30:1014–1019
Kim MJ, Hur BY, Lee ES, Park B, Joo J, Kim MJ, Park SC, Baek JY, Chang HJ, Kim DY, Oh JH (2018) Prediction of lateral pelvic lymph node metastasis in patients with locally advanced rectal cancer with preoperative chemoradiotherapy: focus on MR imaging findings. PLoS ONE 12:13
Agger E, Åkerlund V, Ekberg O, Jörgren F, Lydrup ML, Buchwald P (2021) Management, treatment and prognostic significance of lateral lymph node metastases in rectal cancer-a regional cohort study. Int J Colorectal Dis 36:2707–2714
Ogura A, Konishi T, Cunningham C, Garcia-Aguilar J, Iversen H, Toda S, Lee IK, Lee HX, Uehara K, Lee P, Putter H, van de Velde CJH, Beets GL, Rutten HJT, Kusters M, Aalbers AGJ, Aiba T, Akiyoshi T, Beets-Tan RGH, Betts M, Blazic IM, Brown KG, Campbell N, Choi MH, Gollub MJ, Hanaoka Y, Kim MK, Meershoek-Klein-Kranenbarg E, Kuroyanagi H, Maas M, Martling A, Moore J, Nieuwenhuijzen GA, Oh SN, Roodbeen S, Sammour T, Schaap D, Solomon MJ, Thomas M, Tomizawa K, van der Sande ME, Suzuki C, van der Valk MJM, Wells T, Won DD (2019) Neoadjuvant (chemo) radiotherapy with total mesorectal excision only is not sufficient to prevent lateral local recurrence in enlarged nodes: results of the multicenter lateral node study of patients with low cT3/4 rectal cancer. J Clin Oncol 37:33–43
Malakorn S, Yang Y, Bednarski BK, Kaur H, You YN, Holliday EB, Dasari A, Skibber JM, Rodriguez-Bigas MA, Chang GJ (2019) Who should get lateral pelvic lymph node dissection after neoadjuvant chemoradiation. Dis Colon Rectum 62:1158–1166
Ahmadi N, Brown KGM, Lee P, Quinn M, Austin KKS, Solomon MJ (2020) Is neoadjuvant chemoradiotherapy sufficient in patients with advanced rectal malignancy and positive extra-mesorectal lateral lymph nodes. Colorectal Dis 22:689–693
Song SH, Choi GS, Kim HJ, Park JS, Park SY, Lee SM, Choi JA, Seok HA (2021) Long-term clinical outcomes of total mesorectal excision and selective lateral pelvic lymph node dissection for advanced low rectal cancer: a comparative study of a robotic versus laparoscopic approach. Tech Coloproctol 25:413–423
Du R, Zhou J, Li D, Zhang Q, Liu J, Ma C, Wang L, Wang D (2021) Postoperative morbidity and mortality after mesorectal excision with laparoscopic versus conventional open lateral lymph node dissection for advanced rectal cancer: a meta-analysis. Asian J Surg 44:26–35
Yamaguchi T, Kinugasa Y, Shiomi A, Kagawa H, Yamakawa Y, Furutani A, Manabe S, Yamaoka Y, Hino H (2018) Oncological outcomes of robotic-assisted laparoscopic versus open lateral lymph node dissection for locally advanced low rectal cancer. Surg Endosc 32:4498–4505
Sylla P, Rattner DW, Delgado S, Lacy AM (2010) Notes transanal rectal cancer resection using transanal endoscopic microsurgery and laparoscopic assistance. Surg Endosc 24:1205–1210
Persiani R, Biondi A, Pennestri F, Fico V, De Simone V, Tirelli F, Santullo F, Ugo D (2018) Transanal total mesorectal excision vs laparoscopic total mesorectal excision in the treatment of low and middle rectal cancer: a propensity score matching analysis. Dis Colon Rectum 61:809–816
Penna M, Hompes R, Arnold S, Wynn G, Austin R, Warusavitarne J, Moran B, Hanna BG, Mortensen JN, Tekkis PP (2017) Transanal total mesorectal excision: international registry results of the first 720 cases. Ann Surg 266:111–117
Perdawood SK, Al Khefagie GA (2016) Transanal vs laparoscopic total mesorectal excision for rectal cancer: initial experience from Denmark. Colorectal Dis 18:51–58
Zeng ZW, Zhang XW, Chen JJ, Huang L, Luo SL, Kang L (2019) Transanal lateral lymph node dissection surgery for 5 cases of mid-low rectal cancer. Zhonghua Wei Chang Wai Ke Za Zhi 22:781–785
Ishii M, Nitta T, Kataoka J, Iida R, Ueda Y, Senpuku S, Matsutani A, Yamamoto M, Ishibashi T, Okuda J (2022) A case report of the transanal lateral lymph node dissection with a combined abdominal assisted approach for the lower rectal cancer. Ann Med Surg (Lond) 73:103173
Matsuda T, Yamashita K, Hasegawa H, Urakawa N, Kanaji S, Oshikiri T, Nakamura T, Kakeji Y (2021) Two-team lateral pelvic lymph node dissection assisted by the transanal approach. Dis Colon Rectum 64:e719–e724
Kusters M, Slater A, Muirhead R, Hompes R, Guy RJ, Jones OM, George BD, Lindsey I, Mortensen NJ (2017) What to do with lateral nodal disease in low locally advanced rectal cancer? a call for further reflection and research. Dis Colon Rectum 60:577–585
Ogura A, Konishi T, Cunningham C, Garcia-Aguilar J, Iversen H, Toda S, Lee IK, Lee HX, Uehara K, Lee P, Putter H, van de Velde CJH, Beets GL, Rutten HJT, Kusters M, Lateral Node Study Consortium Lateral Node Study Consortium (2019) Neoadjuvant (chemo) radiotherapy with total mesorectal excision only is not sufficient to prevent lateral local recurrence in enlarged nodes: results of the multicenter lateral node study of patients with low cT3/4 rectal cancer. J Clin Oncol 37:33–43
Gröne J, Loch FN, Taupitz M, Schmidt C, Kreis ME (2018) Accuracy of various lymph node staging criteria in rectal cancer with magnetic resonance imaging. J Gastrointest Surg 22:146–153
Watanabe J, Ishibe A, Suwa Y, Suwa H, Ota M, Kunisaki C, Endo I (2020) Autonomic nerve-preserving lymph node dissection for lateral pelvic lymph node metastasis of the pelvic floor using the transanal approach. Dis Colon Rectum 63:113–114
Fujita S, Akasu T, Mizusawa J, Saito N, Kinugasa Y, Kanemitsu Y, Ohue M, Fujii S, Shiozawa M, Yamaguchi T, Moriya Y, Nakamura K, Katayama H, Takashima A, Kaba H, Nakano A, Fukuda H (2012) Postoperative morbidity and mortality after mesorectal excision with and without lateral lymph node dissection for clinical stage II or stage III lower rectal cancer (JCOG0212): results from a multicentre, randomised controlled, non-inferiority trial. Lancet Oncol 13:616–621
Dindo D, Demartines N, Clavien PA (2004) Classification of surgical complications: a new proposal with evaluation in a cohort of 6336 patients and results of a survey. Ann Surg 240:205–213
Yamaguchi T, Kinugasa Y, Shiomi A, Tomioka H, Kagawa H (2016) Robotic-assisted laparoscopic versus open lateral lymph node dissection for advanced lower rectal cancer. Surg Endosc 30:721–728
Kim HJ, Choi GS, Park JS, Park SY, Yang CS, Lee HJ (2018) The impact of robotic surgery on quality of life, urinary and sexual function following total mesorectal excision for rectal cancer: a propensity score-matched analysis with laparoscopic surgery. Colorectal Dis 20:O103–O113
Kanao H, Fujiwara K, Ebisawa K, Hada T, Ota Y, Andou M (2014) Various types of total laparoscopic nerve-sparing radical hysterectomies and their effects on bladder function. J Gynecol Oncol 25:198–205
Oshio H, Oshima Y, Yunome G, Yano M, Okazaki S, Ashitomi Y, Musha H, Kamio Y, Motoi F (2022) Potential urinary function benefits of initial robotic surgery for rectal cancer in the introductory phase. J Robot Surg 16:159–168
Chang GJ, Rodriguez-Bigas MA, Skibber JM, Moyer VA (2007) Lymph node evaluation and survival after curative resection of colon cancer: systematic review. J Natl Cancer Inst 99:433–441
Akiyoshi T, Watanabe T, Miyata S, Kotake K, Muto T, Sugihara K (2012) Results of a Japanese nationwide multi-institutional study on lateral pelvic lymph node metastasis in low rectal cancer: is it regional or distant disease? Ann Surg 255:1129–1134
Dumont F, Barreteau T, Simon G, Loaec C (2022) Laparoscopic extraperitoneal approach to bilateral pelvic lymph node dissection in low rectal cancer: technique with video and 3D modeling. Ann Surg Oncol 29:109–111
Shiraishi T, Sasaki T, Tsukada Y, Ikeda K, Nishizawa Y, Ito M (2021) Radiologic factors and areas of local recurrence in locally advanced lower rectal cancer after lateral pelvic lymph node dissection. Dis Colon Rectum 64:1479–1487
Ouyang M, Liao T, Lu Y, Deng L, Luo Z, Wu J, Ju Y, Yao X (2019) Laparoscopic versus open surgery in lateral lymph node dissection for advanced rectal cancer: a meta-analysis. Gastroenterol Res Pract 2019:7689082
Watanabe J, Ishibe A, Suwa Y, Ozawa M, Nakagawa K, Suwa H, Ota M, Kunisaki C, Endo I (2021) Short- and long-term outcomes of laparoscopic versus open lateral lymph node dissection for locally advanced middle/lower rectal cancer using a propensity score-matched analysis. Surg Endosc 35:4427–4435
Di Candido F, Carvello M, Keller DS, Vanni E, Maroli A, Montroni I, Hompes R, Sacchi M, Montorsi M, Spinelli A (2021) A comparative cost analysis of transanal and laparoscopic total mesorectal excision for rectal cancer. Updates Surg 73:85–91
Acknowledgements
None.
Funding
This research received no funding from any specific public, commercial, or non-profit agencies.
Author information
Authors and Affiliations
Contributions
SN made substantial contributions to the study’s conception and design, acquisition of data, and analysis and interpretation of the collected data. DK drafted the manuscript and revised it critically for important intellectual content. KI, HH, KT, YT, and YN were involved in the discussions about this study. MI gave the final approval of the manuscript to be published. All authors have read and approved the final manuscript.
Corresponding author
Ethics declarations
Disclosures
Drs. Satoshi Narihiro, Daichi Kitaguchi, Koji Ikeda, Hiro Hasegawa, Koichi Teramura, Yuichiro Tsukada, Yuji Nishizawa and Masaaki Ito have no conflicts of interest or financial ties to disclose.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Narihiro, S., Kitaguchi, D., Ikeda, K. et al. Two-team lateral lymph node dissection assisted by the transanal approach for locally advanced lower rectal cancer: comparison with the conventional transabdominal approach. Surg Endosc 37, 5256–5264 (2023). https://doi.org/10.1007/s00464-023-10012-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-023-10012-1