Abstract
Background and Aims
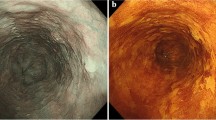
Chromoendoscopy with Lugol’s staining is used to screen for early esophageal squamous cell carcinoma (ESCC). Its efficacy is greatly limited by unstandardized defoaming preparation. This study aimed to confirm whether pre-procedure oral administration of pronase could improve the diagnostic performance of Lugol chromoendoscopy in high-risk patients being screened for early ESCC.
Methods
A total of 955 patients at-risk were prospectively recruited for screening for ESCC. Patients were randomly assigned (1:1) to groups with or without (control group) pronase administration. Endoscopic diagnosis of early ESCC was based on the presence of pink-color sign in Lugol’s unstained area, and a biopsy was routinely conducted if the Lugol’s unstained lesion was larger than 0.5 cm. The early cancer detection rate was used as the primary endpoint.
Results
Pre-procedure oral administration of pronase improved mucosal visibility during Lugol chromoendoscopy (P = 0.008). There were no differences in the number of Lugol’s unstained lesions between the 2 groups (23.27% [111/477] vs. 25.11% [120/478], P = 0.508). Meaningfully, the detection rate of ESCC (confirmed by histopathology) was significantly higher in the pronase group than in the control group (27.03% [30/111] vs. 17.50% [21/120], P = 0.041), as well as the detection rate of lesions with pink-color sign during chromoendoscopy (35.14% [39/111] vs. 13.33% [16/120], P < 0.001). The diagnostic performance of Lugol chromoendoscopy had improved with the use of pronase (area under the curve = 0.85 vs. 0.69, P = 0.019), accompanied by an increased sensitivity (86.67% vs. 47.62%, P = 0.004). There was no difference in the adverse events between the 2 groups (P = 0.793).
Conclusions
Pre-procedure oral administration of pronase significantly increased the detection rate of early ESCC and optimized the diagnostic performance of Lugol chromoendoscopy, which should be recommended during routine endoscopic screening for early ESCC in high-risk patients.
Trial registration
Pronase improves efficacy of Lugol chromoendoscopy screening on esophageal cancerous lesions (NCT02030769).



Similar content being viewed by others
Change history
22 February 2023
A Correction to this paper has been published: https://doi.org/10.1007/s00464-023-09966-z
References
Bray F, Ferlay J, Soerjomataram I, Siegel RL, Torre LA, Jemal A (2018) Global cancer statistics 2018: GLOBOCAN estimates of incidence and mortality worldwide for 36 cancers in 185 countries. CA Cancer J Clin 68:394–424
Wang SM, Katki HA, Graubard BI, Kahle LL, Chaturvedi A, Matthews CE, Freedman ND, Abnet CC (2021) Population attributable risks of subtypes of esophageal and gastric cancers in the United States. Am J Gastroenterol 116:1844–1852
Zeng H, Chen W, Zheng R, Zhang S, Ji JS, Zou X, Xia C, Sun K, Yang Z, Li H, Wang N, Han R, Liu S, Li H, Mu H, He Y, Xu Y, Fu Z, Zhou Y, Jiang J, Yang Y, Chen J, Wei K, Fan D, Wang J, Fu F, Zhao D, Song G, Chen J, Jiang C, Zhou X, Gu X, Jin F, Li Q, Li Y, Wu T, Yan C, Dong J, Hua Z, Baade P, Bray F, Jemal A, Yu XQ, He J (2018) Changing cancer survival in China during 2003–15: a pooled analysis of 17 population-based cancer registries. Lancet Glob Health 6:e555–e567
Wei WQ, Chen ZF, He YT, Feng H, Hou J, Lin DM, Li XQ, Guo CL, Li SS, Wang GQ, Dong ZW, Abnet CC, Qiao YL (2015) Long-term follow-up of a community assignment, one-time endoscopic screening study of esophageal cancer in China. J Clin Oncol 33:1951–1957
Shao Y, Yu ZL, Ji M, Wu YD, Yu YZ, Liang XM, Yu LI, Niu YL, Li P, Zhang ST (2015) Lugol chromoendoscopic screening for esophageal dysplasia/early squamous cell carcinoma in patients with esophageal symptoms in low-risk region in China. Oncol Lett 10:45–50
Mwachiro MM, Burgert SL, Lando J, Chepkwony R, Bett C, Bosire C, Abnet CC, Githanga J, Waweru W, Giffen CA, Murphy G, White RE, Topazian MD, Dawsey SM (2016) Esophageal squamous dysplasia is common in asymptomatic Kenyans: a prospective, community-based, cross-sectional study. Am J Gastroenterol 111:500–507
Li J, Xu R, Liu M, Cai H, Cao C, Liu F, Li F, Guo C, Pan Y, He Z, Ke Y (2018) Lugol chromoendoscopy detects esophageal dysplasia with low levels of sensitivity in a high-risk region of China. Clin Gastroenterol Hepatol 16:1585–1592
Yokoyama A, Hirota T, Omori T, Yokoyama T, Kawakubo H, Matsui T, Mizukami T, Mori S, Sugiura H, Maruyama K (2012) Development of squamous neoplasia in esophageal iodine-unstained lesions and the alcohol and aldehyde dehydrogenase genotypes of Japanese alcoholic men. Int J Cancer 130:2949–2960
Dubuc J, Legoux J, Winnock M, Seyrig J, Barbier J, Barrioz T, Laugier R, Boulay G, Grasset D, Sautereau D, Grigoresco D, Butel J, Scoazec J, Ponchon T, Societe Francaise d’Endoscopie D (2006) Endoscopic screening for esophageal squamous-cell carcinoma in high-risk patients: a prospective study conducted in 62 French endoscopy centers. Endoscopy 38:690–695
Shimizu Y, Omori T, Yokoyama A, Yoshida T, Hirota J, Ono Y, Yamamoto J, Kato M, Asaka M (2008) Endoscopic diagnosis of early squamous neoplasia of the esophagus with iodine staining: high-grade intra-epithelial neoplasia turns pink within a few minutes. J Gastroenterol Hepatol 23:546–550
Park CH, Yang DH, Kim JW, Kim JH, Kim JH, Min YW, Lee SH, Bae JH, Chung H, Choi KD, Park JC, Lee H, Kwak MS, Kim B, Lee HJ, Lee HS, Choi M, Park DA, Lee JY, Byeon JS, Park CG, Cho JY, Lee ST, Chun HJ (2020) Clinical practice guideline for endoscopic resection of early gastrointestinal cancer. Clin Endosc 53:142–166
Goda K, Dobashi A, Yoshimura N, Kato M, Aihara H, Sumiyama K, Toyoizumi H, Kato T, Ikegami M, Tajiri H (2015) Narrow-band imaging magnifying endoscopy versus lugol chromoendoscopy with pink-color sign assessment in the diagnosis of superficial esophageal squamous neoplasms: a randomised noninferiority trial. Gastroenterol Res Pract 2015:639462
Ishihara R, Kanzaki H, Iishi H, Nagai K, Matsui F, Yamashina T, Matsuura N, Ito T, Fujii M, Yamamoto S, Hanaoka N, Takeuchi Y, Higashino K, Uedo N, Tatsuta M, Tomita Y, Ishiguro S (2013) Pink-color sign in esophageal squamous neoplasia, and speculation regarding the underlying mechanism. World J Gastroenterol 19:4300–4308
Chen HW, Hsu HC, Hsieh TY, Yeh MK, Chang WK (2014) Pre-medication to improve esophagogastroduodenoscopic visibility: a meta-analysis and systemic review. Hepatogastroenterology 61:1642–1648
Monrroy H, Vargas JI, Glasinovic E, Candia R, Azua E, Galvez C, Rojas C, Cabrera N, Vidaurre J, Alvarez N, Gonzalez J, Espino A, Gonzalez R, Parra-Blanco A (2018) Use of N-acetylcysteine plus simethicone to improve mucosal visibility during upper GI endoscopy: a double-blind, randomized controlled trial. Gastrointest Endosc 87:986–993
Kuo CH, Sheu BS, Kao AW, Wu CH, Chuang CH (2002) A defoaming agent should be used with pronase premedication to improve visibility in upper gastrointestinal endoscopy. Endoscopy 34:531–534
Lee GJ, Park SJ, Kim SJ, Kim HH, Park MI, Moon W (2012) Effectiveness of premedication with pronase for visualization of the mucosa during endoscopy: a randomized, controlled trial. Clin Endosc 45:161–164
Chiu PWY, Uedo N, Singh R, Gotoda T, Ng EKW, Yao K, Ang TL, Ho SH, Kikuchi D, Yao F, Pittayanon R, Goda K, Lau JYW, Tajiri H, Inoue H (2019) An Asian consensus on standards of diagnostic upper endoscopy for neoplasia. Gut 68:186–197
Chen MJ, Wang HY, Chang CW, Hu KC, Hung CY, Chen CJ, Shih SC (2013) The add-on N-acetylcysteine is more effective than dimethicone alone to eliminate mucus during narrow-band imaging endoscopy: a double-blind, randomized controlled trial. Scand J Gastroenterol 48:241–245
Kim GH, Cho YK, Cha JM, Lee SY, Chung IK (2015) Effect of pronase as mucolytic agent on imaging quality of magnifying endoscopy. World J Gastroenterol 21:2483–2489
Yokoyama A, Ohmori T, Makuuchi H, Maruyama K, Okuyama K, Takahashi H, Yokoyama T, Yoshino K, Hayashida M, Ishii H (1995) Successful screening for early esophageal cancer in alcoholics using endoscopy and mucosa iodine staining. Cancer 76:928–934
Ishihara R, Yamada T, Iishi H, Kato M, Yamamoto S, Yamamoto S, Masuda E, Tatsumi K, Takeuchi Y, Higashino K, Uedo N, Tatsuta M, Ishiguro S (2009) Quantitative analysis of the color change after iodine staining for diagnosing esophageal high-grade intraepithelial neoplasia and invasive cancer. Gastrointest Endosc 69:213–218
Mori M, Adachi Y, Matsushima T, Matsuda H, Kuwano H, Sugimachi K (1993) Lugol staining pattern and histology of esophageal lesions. Am J Gastroenterol 88:701–705
Le CT (2006) A solution for the most basic optimization problem associated with an ROC curve. Stat Methods Med Res 15:571–584
Nagami Y, Tominaga K, Machida H, Nakatani M, Kameda N, Sugimori S, Okazaki H, Tanigawa T, Yamagami H, Kubo N, Shiba M, Watanabe K, Watanabe T, Iguchi H, Fujiwara Y, Ohira M, Hirakawa K, Arakawa T (2014) Usefulness of non-magnifying narrow-band imaging in screening of early esophageal squamous cell carcinoma: a prospective comparative study using propensity score matching. Am J Gastroenterol 109:845–854
Hashimoto CL, Iriya K, Baba ER, Navarro-Rodriguez T, Zerbini MC, Eisig JN, Barbuti R, Chinzon D, Moraes-Filho JP (2005) Lugol’s dye spray chromoendoscopy establishes early diagnosis of esophageal cancer in patients with primary head and neck cancer. Am J Gastroenterol 100:275–282
Inoue H, Rey JF, Lightdale C (2001) Lugol chromoendoscopy for esophageal squamous cell cancer. Endoscopy 33:75–79
Shimizu Y, Tukagoshi H, Fujita M, Hosokawa M, Kato M, Asaka M (2001) Endoscopic screening for early esophageal cancer by iodine staining in patients with other current or prior primary cancers. Gastrointest Endosc 53:1–5
Liu X, Guan CT, Xue LY, He S, Zhang YM, Zhao DL, Li Y, Liu FG, Li J, Liu YF, Ling AS, Wei WQ, Wang GQ (2018) Effect of premedication on lesion detection rate and visualization of the mucosa during upper gastrointestinal endoscopy: a multicenter large sample randomized controlled double-blind study. Surg Endosc 32:3548–3556
Shimizu Y, Tukagoshi H, Fujita M, Hosokawa M, Kato M, Asaka M (2001) Metachronous squamous cell carcinoma of the esophagus arising after endoscopic mucosal resection. Gastrointest Endosc 54:190–194
Takahashi M, Shimizu Y, Ono M, Suzuki M, Omori S, Yoshida T, Mori Y, Nakagawa M, Ono S, Nakagawa S, Mabe K, Kato M, Hatanaka K, Asaka M, Sakamoto N (2014) Endoscopic diagnosis of early neoplasia of the esophagus with narrow band imaging: correlations among background coloration and iodine staining findings. J Gastroenterol Hepatol 29:762–768
Acknowledgements
This work was supported by the National Natural Science Foundation of China (Grant No. 81572820, 81702355) and the Key Research and Development Program of Shaanxi Province (Grant No. 2023-ZDLSF-36).
Author information
Authors and Affiliations
Contributions
ZL and YH designed the study. XZ collected the data and interpreted the data. MG drafted the manuscript and performed the statistical analysis; LZ, SZ, TD and HL conducted the endoscopic examination and performed the clinical patient management; WY and JZ critically revised the manuscript; all authors were involved in the review and interpretation of data and approved the final copy.
Corresponding authors
Ethics declarations
Disclosures
Xin Zhao, Meng Guo, Shaohua Zhu, Linhui Zhang, Tao Dong, Hui Luo, Weihua Yu, Jiangyi Zhu, Xiaotong Fan, Ying Han, and Zhiguo Liu have no conflicts of interest or financial ties to disclose.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Zhao, X., Guo, M., Zhu, S. et al. Pre-procedure oral administration of pronase improves efficacy of lugol chromoendoscopy in esophageal squamous cell carcinoma screening: a prospective, double-blinded, randomized, controlled trial. Surg Endosc 37, 4421–4430 (2023). https://doi.org/10.1007/s00464-023-09902-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-023-09902-1