Abstract
Background
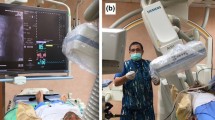
The radiofrequency identification (RFID) lung marking system is a novel technique using near-field radio-communication technology. The purpose of this study was to investigate the utility and feasibility of this system in the resection of small pulmonary nodules.
Methods
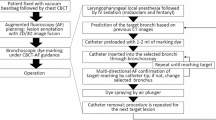
We retrospectively reviewed clinical records of 182 patients who underwent sublobar resection with the RFID marking system between March 2020 and November 2021 in six tertial hospitals in Japan. Target markings were bronchoscopically made within 3 days before surgery. The contribution of the procedure to the surgery and safety was evaluated.
Results
Target nodule average diameter and depth from the lung surface were 10.9 ± 5.4 mm and 14.6 ± 9.9 mm, respectively. Radiologically, one third of nodules appeared as pure ground-glass nodules (GGNs) on CT. The average distance from target nodule to RFID tag was 8.9 ± 7.1 mm. All surgical procedures were completed by video-assisted thoracoscopic surgery. Planned resection was achieved in all cases without any complications. The surgeons evaluated this system as helpful in 93% (necessary: 67%, useful; 26%) of cases. Nodule radiological features (p < 0.001) and type of surgery (p = 0.0013) were associated with the degree of contribution. In most cases, identification of the RFID tag was required within 1 min despite adhesion (p = 0.27).
Conclusion
The RFID lung marking system was found to be safe and effective during successful sublobar resection. Patients with pure GGNs are the best candidates for the system.



Similar content being viewed by others
Abbreviations
- CT:
-
Computed tomography
- GGN:
-
Ground-glass nodule
- GGO:
-
Ground-glass opacity
- RFID:
-
Radiofrequency identification
- VAL-MAP:
-
Virtual-assisted lung mapping
References
Tanaka N, Waseda R, Saito D, Ohsima M, Matsumoto I, Takemura H (2001) A novel fluorescent lung-marking technique using the photodynamic diagnosis endoscope system and vitamin B2. Interact Cardiovasc Thorac Surg 31:853–859
Nakajima J (2019) Advances in techniques for identifying small pulmonary nodules. Surg Today 49:311–315
Tomiyama N, Yasuhara Y, Nakajima Y, Adachi S, Arai Y, Kusumoto M, Eguchi K, Kuriyama K, Sakai F, Noguchi M, Murata K, Murayama S, Mochizuki T, Mori K, Yamada K (2006) CT-guided needle biopsy of lung lesions: a survey of severe complication based on 9783 biopsies in Japan. Eur J Radiol 59:60–64
Sato M, Kobayashi M, Kojima F, Tanaka F, Yanagiya M, Kosaka S, Fukai R, Nakajima J (2018) Effect of virtual-assisted lung mapping in acquisition of surgical margins in sublobar lung resection. J Thorac Cardiovasc Surg 156:1691–1701
Yutaka Y, Sato T, Tanaka S, Miyahara S, Yoshizawa A, Morita S, Date H (2022) Feasibility study of a novel wireless localization technique using radiofrequency identification markers for small and deeply located lung lesions. JTCVS Tech 12:185–195
Sato T, Yutaka Y, Nakamura T, Date H (2020) First clinical application of radiofrequency identification (RFID) marking system—Precise localization of a small lung nodule. JTCVS Tech 4:301–304
Ginsberg RJ, Rubinstein LV (1995) Randomized trial of lobectomy versus limited resection for T1 N0 non-small cell lung cancer. Ann Thorac Surg 60:615–623
Saji H, Okada M, Tsuboi M, Nakajima R, Suzuki K, Aokage K, Aoki T, Okami J, Yoshino I, Ito H, Okumura N, Yamaguchi M, Ikeda N, Wakabayashi M, Nakamura K, Fukuda H, Nakamura S, Mitsudomi T, Watanabe S, Asamura H, West Japan Oncology Group and Japan Clinical Oncology Group (2022) Segmentectomy versus lobectomy in small-sized peripheral non-small-cell lung cancer (JCOG0802/WJOG4607L): a multicentre, open-label, phase 3, randomised, controlled, non-inferiority trial. Lancet 399:1607–1617
Suzuki K, Watanabe S, Wakabayashi M, Saji H, Aokage K, Moriya Y, Yoshino I, Tsuboi M, Nakamura S, Nakamura K, Mitsudomi T, Asamura H, West Japan Oncology Group and Japan Clinical Oncology Group (2022) A single-arm study of sublobar resection for ground-glass opacity dominant peripheral lung cancer. J Thorac Cardiovasc Surg 163:289–301
Suzuki K, Nagai K, Ohmatsu H (1999) Video-assisted thoracoscopic surgery for small indeterminate pulmonary nodules: Indications for preoperative marking. Chest 115:563–568
Cardillo G, Regal M, Sera F, Martino M, Carbone L, Facciolo F, Martelli M (2003) Videothoracoscopic management of the solitary pulmonary nodule: a single-institution study on 429 cases. Ann Thorac Surg 75:1607–1611
Powell TI, Joanne DJ, Clifton JC, Guerra HL, Church N, English J, Evans K, Yee J, Coxson H, Mayo JR, Finley RJ (2004) Peripheral lung nodules: fluoroscopically guided video-assisted thoracoscopic resection after computed tomography-guided localization using platinum microcoils. Ann Surg 240:481–489
Lizza N, Eucher P, Haxhe JP, Wispelaere JFD, Johnson PM, Delaunois L (2001) Thoracoscopic resection of pulmonary nodules after computed tomographic-guided coil labeling. Ann Thorac Surg 71:986–988
Sancheti MS, Lee R, Ahmed SU, Pickens A, Fernandez FG, Small WC, Nour SG, Force SD (2014) Percutaneous fiducial localization for thoracoscopic wedge resection of small pulmonary nodules. Ann Thorac Surg 97:1914–1919
Hanauer M, Perentes JY, Krueger T, Ris HB, Bize P, Schmidt S, Gonzalez M (2016) Pre-operative localization of solitary pulmonary nodules with computed tomography-guided hook wire: report of 181 patients. J Cardiothorac Surg 11:1–7
Kleedehn M, Kim DH, Lee FT, Lubner MG, Robbins JB, Ziemlewicz TJ, Hinshaw JL (2016) Preoperative pulmonary nodule localization: a comparison of methylene blue and hookwire techniques. Am J Roentgenol 207:1334–1339
McConnell PI, Feola GP, Meyers RL (2002) Methylene blue-stained autologous blood for needle localization and thoracoscopic resection of deep pulmonary nodules. J Pediatr Surg 37:1729–1731
Watanabe K, Nomori H, Ohtsuka T, Kaji M, Naruke T, Suemasu K (2006) Usefulness and complications of computed tomography-guided lipiodol marking for fluoroscopy-assisted thoracoscopic resection of small pulmonary nodules: experience with 174 nodules. J Thorac Cardiovasc Surg 132:320–324
Sato M, Omasa M, Chen F, Sato T, Sonobe M, Bando T, Date H (2014) Use of virtual assisted lung mapping (VAL-MAP), a bronchoscopic multispot dye-marking technique using virtual images, for precise navigation of thoracoscopic sublobar lung resection. J Thorac Cardiovasc Surg 147:1813–1819
Park CH, Han K, Hur J, Lee SM, Lee JW, Hwang SH, Seo JS, Lee KH, Kwon W, Kim TH, Choi BW (2007) Comparative effectiveness and safety of preoperative lung localization for pulmonary nodules: a systematic review and meta-analysis. Chest 151:316–328
Lin MW, Chen JS (2016) Image-guided techniques for localizing pulmonary nodules in thoracoscopic surgery. J Thorac Dis 8:S749–S755
Asano F, Eberhardt R, Herth FJF (2014) Virtual bronchoscopic navigation for peripheral pulmonary lesions. Respiration 88:430–440
Qian K, Krimsky WS, Sarkar SA, Deng Y (2009) Efficiency of electromagnetic navigation bronchoscopy and virtual bronchoscopic navigation. Ann Thorac Surg 109:1731–1740
Xu C, Wang Y, Li L, Yuan Q, Wang Y, Hu H, Zhang X (2021) Diagnostic value of virtual bronchoscopic navigation combined with endobronchial ultrasound guided transbronchial lung biopsy for peripheral pulmonary lesions. Technol Cancer Res Treat 20:1–6
Reisenauer J, Duke JD, Kern R, Bessy SF, Edell E (2022) Combining shape-sensing robotic bronchoscopy with mobile three-dimensional imaging to verify tool-in-lesion and overcome divergence: a pilot study. Mayo Clin Proc Innov Qual Outcomes 6:177–185
Chen AC, Pastis N, Mahajan AK, Khandhar SJ, Simoff MJ, Machuzak M, Cicenia J, Gildea TR, Silvestri GA (2021) Robotic bronchoscopy for peripheral pulmonary lesions: a multicenter pilot and feasibility study (Benefit). Chest 159:845–852
Shinagawa N, Yamazaki K, Onodera Y, Asahina H, Kikuchi E, Asano F, Miyasaka K, Nishimura M (2007) Factors related to diagnostic sensitivity using an ultrathin bronchoscope under CT guidance. Chest 131:549–553
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Disclosures
Drs. Yojiro Yutaka, Hiroshi Date and Toshihiko Sato have a financial relationship with HOGY Medical Co Ltd. Drs. So Miyahara, Ryuichi Waseda, Yuichirou Ueda, Jun Suzuki, Hiroyuki Oizumi, Masashi Goto, Tatsuo Nakagawa, Fumitsugu Kojima, Masaru Takenaka and Fumihiro Tanaka have no conflicts of interest or financial ties to disclose.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Supplementary file2 (MPG 39192 kb)—This video demonstrates the sequence of the process of the RFID tag placement and surgery.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Miyahara, S., Waseda, R., Ueda, Y. et al. Evaluation of the radiofrequency identification lung marking system: a multicenter study in Japan. Surg Endosc 37, 3619–3626 (2023). https://doi.org/10.1007/s00464-022-09858-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-022-09858-8